Hypertension by Dr. Mohib Ali
-
Upload
mohib-ali -
Category
Health & Medicine
-
view
107 -
download
2
Transcript of Hypertension by Dr. Mohib Ali

HYPERTENSION
Dr. Mohib AliJanuary 06, 2015

Definition
• Hypertension is defined as a systolic blood pressure (SBP) of 140
mm Hg or more, or a diastolic blood pressure (DBP) of 90 mm Hg or
more on repeated measurement, or taking antihypertensive
medication.

HTN Classification
Blood Pressure Classification
SBP mmHg DBP mmHg
Normal <120 And <80
Pre-Hypertension 120-139 Or 80-89
Stage 1 Hypertension 140-159 Or 90-99
Stage 2 Hypertension -/> 160 Or -/> 100

• Isolated increase in the systolic BP with diastolic BP<90 mm Hg
Class Systolic BP Diastolic BP
Grade 1 140-159 <90
Grade 2 >/- 160 <90

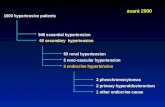
• 90-95% Essential HTN
• 05-10% Secondary

Essential Hypertension
• Multifactorial Aetiology.
– Genetic factors
– Fetal factors
• Environmental factors
– Obesity
– Alcohol intake
– Sodium intake
– Stress
– Smoking
• Insulin resistance
– (Metabolic syndrome)
The majority (80–90%) of patients with hypertension have primary
elevation of blood pressure, i.e. essential hypertension of unknown
cause.

Secondary Hypertension
• Identifiable cause
• Suspected in ;
– Early onset
– First episode over age 50 years
– Those previously well controlled become refractory to treatment

Secondary causes of Hypertension
Endocrine Adrenal Renal Cardiovascular Drugs
• Cushing's syndrome
• Acromegaly
• Thyroid disease
• Hyperparathyroid disease
• Conn's syndrome
• Adrenal hyperplasia
• Phaeochromocytoma
• Diabetic nephropathy
• Chronic glomerulonephritis
• Adult polycystic disease
• Chronic tubulointerstitial nephritis
• Renovasculardisease
• Aortic coarctation
• NSAIDs• Oral
contraceptives• Steroids• Carbenoxalone• Liquorice• Sympathomim
etics• Vasopressin• Monoamine
oxidase inhibitors (with tyramine)

• A 71-year-old woman is reviewed in the clinic. Her blood pressure is
146/ 94 mmHg. This is confirmed on a second reading. what is the
most appropriate next-step?
a) Ask her to come back in 6 months for a blood pressure check
b) Arrange 3 blood pressure checks with the practice nurse over the
next 2 weeks with medical review following
c) Arrange ambulatory blood pressure monitoring
d) Reassure her this is acceptable for her age
e) Start treatment with a calcium channel blocker

Diagnosis Of Hypertension

Investigation of all patients
• Urinalysis for blood, protein and glucose
• Blood urea, electrolytes and creatinine
– Hypokalaemic alkalosis may indicate primary
hyperaldosteronism but is usually due to diuretic therapy
• Blood glucose
• Serum total and HDL cholesterol
• 12-lead ECG (left ventricular hypertrophy, coronary artery disease)

Investigation of selected patients
• Chest X-ray: to detect cardiomegaly, heart failure, coarctation of the
aorta
• Ambulatory BP recording: to assess borderline or ‘white coat’
hypertension
• Echocardiogram: to detect or quantify left ventricular hypertrophy
• Renal ultrasound: to detect possible renal disease
• Renal angiography: to detect or confirm presence of renal artery
stenosis
• Urinary catecholamines: to detect possible phaeochromocytoma
• Urinary cortisol and dexamethasone suppression test: to detect
possible Cushing’s syndrome
• Plasma renin activity and aldosterone: to detect possible primary
aldosteronism

Diagnosis Of HTN
• NICE now recommend ambulatory blood pressure monitoring to aid
diagnosis
• The 2012 NICE guidelines recognize that in the past there was
overtreatment of 'white coat' hypertension. The use of ambulatory
blood pressure monitoring (ABPM) aims to reduce this.
– When ABPM is used, at least two measurements per hour
should be taken during person’s waking hours.
– Use the average value of at least 14 measurements taken during
person’s waking hours to confirm diagnosis of hypertension.

Diagnosis of Hypertension
• If clinic blood pressure is >140/90, offer AMBULATORY BLOOD
PRESSURE MONITORING to confirm diagnosis.
– When ABPM is used, at least two measurements per hour
should be taken during person’s waking hours.
– Use the average value of at least 14 measurements taken during
person’s waking hours to confirm diagnosis of hypertension.

The Oscar 2 monitor.
The ambulatory blood pressure
monitor

Another option is Home Blood Pressure Monitoring
(HBPM). When this is used:
For each blood pressure recording, two consecutive
measurements are taken, at least 1 minute apart and with person
seated,
Blood pressure is recorded twice daily, in morning and evening,
Blood pressure recording continues for at least 4 days, ideally for
7 days.
Measurements on first day are discarded
Average of remaining measurements are used to confirm
diagnosis

• ABPM/HBPM
– <135/85 mmHg = Normal
– >135/85 mmHg = Stage 1 Hypertension
– >150/95 mmHg = Stage 2 Hypertension
• Based on a study examining relationships between clinic BPMs and
ABPM measurements;
– 135/85 ABPM is equivalent to 140/90 clinic BPMs ,
– and 150/95 ABPM is equivalent to 160/100 clinic

NICE Guidelines for Management
Of Hypertension

Importance of lowering blood pressure
• Lowering blood pressure can significantly decrease risk of CV
disease.
– 61 prospective observational trials, nearly 1 million people, age
bands from 40 to 89
– Examined relationship between blood pressure level and 12,000
strokes, 34,000 heart disease events over an average of 13.2
years follow-up
– Reductions in systolic of 20mmHg and diastolic 10mmHg was
associated with reductions in death from stroke and ischemic
heart disease of about one half (~50%)

Importance of lowering blood pressure
• A similar analysis of 9 observational studies looking at relationship
between BP level and strokes/coronary events found:
– Reductions in diastolic BP of 5, 7.5, and 10 mmHg was
associated with reductions in stroke of 34%, 46%, and 56%, and
coronary heart disease of 21%, 29%, and 37%, respectively

Cardiovascular risk assessment
• Important to determine presence of CV disease or high CV risk
states (diabetes or CKD).
• Risk models have been developed for doctors to assess likelihood
of patients developing cardiovascular disease. (10 year risk).
• Factors involved in risk assessment include:
– Gender, age, diabetic status, smoking status, total cholesterol,
HDL cholesterol, and blood pressure.
• Allows for identification of patients under greatest overall risk and
treatment of modifiable risk factors.

Target Organ Damage
• Another important objective in assessing people with suspected
hypertension is ;
– To document presence or absence of target organ damage.
– Examples include:
• Left ventricular hypertrophy, hypertensive retinopathy, and
increased albumin:creatinine ratio (kidney damage)

Target Organ Damage in HTN
AtherosclerosisAneurysmsAortic dissections
Pulmonary oedemaMyocardial infarctionLeft ventricular hypertrophy
HaematuriaUraemiaProteinemia
Haemorrhage / infarctionSeizuresVascular dementia
HaemorrhagesExudatesA-V nippingPapilloedema

Hypertensive retinopathy(Keith-Wagener classification)
• Grade 1– tortuosity of the retinal arteries with increased reflectiveness (silver wiring)
• Grade 2– grade 1 plus the appearance of arteriovenous nipping produced when
thickened retinal arteries pass over the retinal veins
• Grade 3– grade 2 plus flame-shaped haemorrhages and soft (‘cotton wool’) exudates
actually due to small infarcts
• Grade 4– grade 3 plus papilloedema (blurring of the margins of the optic disc)
• Grades 3 and 4 are diagnostic of malignant hypertension.

Grade 4 hypertensive retinopathy
showing swollen optic disc, retinal
haemorrhages
and multiple cotton wool spots
(infarcts)
Central retinal vein thrombosis
showing swollen optic disc and
widespread fundal haemorrhage,
commonly associated with systemic
hypertension

Lifestyle Modifications
• Dietary modifications and exercise
– Low calorie diets have modest effect on BP in overweight
individuals (avg. 5-6 mm Hg).
– Aerobic exercise (brisk walking, jogging, or cycling) for 30-60
min., 3-5 times/week, had small effect on BP (2-3 mm Hg).
• Relaxation therapies
– These activities (stress management, meditation, cognitive
therapy, muscle relaxation) reduce by average of 3-4 mm Hg.

Lifestyle Modifications
• Limit alcohol consumption
– Excessive alcohol consumption is associated with raised blood
pressure, poorer CV and hepatic health.
– Reducing alcohol can lower BP 3-4 mm Hg.
• Limiting excessive consumption of coffee/caffeine (small
benefit).
• Limit dietary sodium intake
– < 6 g/day, modest reduction of 2-3 mm Hg.
• Encourage smoking cessation (reduce risk of
CV/pulmonary disease).

Criteria for starting Antihypertensive drug treatment
• Offer step 1 treatment to people aged under 80 with stage 1
hypertension and one or more of:
• target organ damage
• established cardiovascular disease
• renal disease
• diabetes mellitus
• 10-year cardiovascular risk equivalent to 20% or more.
• Offer step 1 treatment to people of any age with stage 2
hypertension.
• People with newly diagnosed hypertension and a 10-year
cardiovascular disease risk of 20% or higher are offered statin
therapy.

• For people aged under 40 years with stage 1 hypertension and no
evidence of target organ damage, CV disease, renal disease or
diabetes, consider specialist evaluation of secondary causes of
hypertension and more detailed assessment of potential target
organ damage.

Step 1 Treatment
• Patients > 55 years CALCIUM CHANNEL BLOCKER
– Offer to people aged over 55 years and to black people of
African or Caribbean family origin of any age.
– If CCB is not suitable (i.e. edema, intolerance, evidence of heart
failure or risk of heart failure), offer a thiazide-like diuretic over
conventional thiazide diuretics
• Chlorthalidone 12.5-25 mg daily; indapamide 1.5-2.5 mg
once daily
– Calcium Channel Blockers examples—amlodipine, nifedipine,
felodipine, verapamil, diltiazem.

Step 1 Treatment
• Patients < 55 years ACE INHIBITOR or ARB
– Offer people aged under 55 years an ACE inhibitor or a low-cost
ARB.
– If ACE inhibitor is prescribed and is not tolerated (i.e. because of
cough), offer a low-cost ARB.
– ACE inhibitor examples—benazepril , captopril , enalapril ,
fosinopril, lisinopril , quinapril (Accupril), ramipril
– ARB examples—candesartan , irbesartan, losartan, olmesartan,
telmisartan, valsartan

Step 2 Treatment
• ACE inhibitor/ARB + Calcium Channel Blocker
• Offer a CCB in combination with either an ACEI or an ARB.
• If a CCB is not suitable, for example because of oedema or intolerance, or if there is evidence of heart failure or a high risk of heart failure, offer a thiazide-like diuretic.
• For black people of African or Caribbean family origin, consider an ARB in preference to an ACE inhibitor, in combination with a CCB.
• Before considering step 3 treatment, review medication to ensure step 2 treatment is at optimal or best tolerated doses.

Step 3 Treatment
• ACEI/ARB + CCB + Thiazide-like diuretic
– Based on the recommendations and analyses performed in the
first two steps.
– Thiazide diuretic examples: chlorthalidone , indapamide ,
hydrochlorothiazide , metolazone.

Recommendations for Step 4
• Addition of low-dose Spironolactone
– Considered when potassium level is < 4.5 mmol/L
• Potassium, sodium, creatinine : checked 2 weeks after
initiation and periodically thereafter.
• Higher-dose thiazide-like diuretic treatment
– Considered when potassium level is > 4.5 mmol/L
• Other options for add-on therapy: alpha blockers or beta blockers

Blood Pressure Goals
• People aged < 80 years with treated hypertension: <140/90 (home:
135/85)
• People aged > 80 years with treated hypertension: <150/90 (home:
145/85)
• For diabetics it s <140/80 mmHg
• For people with “white coat effect”—difference of 20/10 mmHg
between clinic and average daily reading—consider adjunct
ambulatory or home BP measurement to monitor BP.

All people with Hypertension
Lifestyle Interventions
Criteria for starting Antihypertensive
drug treatment
Antihypertensive drug treatment
Review annually

Antihypertensive drug treatment
People starting antihypertensive drug
treatment
General principles
Blood pressure targets
Patient education & adherence to drug
treatment
Person under age 55
Person aged over 55 or
black person of African or
caribbean family origin of
any age

Person under age 55
Person aged over 55 or black
person of African or caribbean
family origin of any age
Step 1
ACE inhibitor or low cost
Angiotensin 2 receptor blocker
Step 1
Calcium channel blocker
Step 2
ACEI or ARB + CCB
Step 3
ACEI or ARB + CCB + Thiazide-like diuretic
Step 4 Resistant hypertension
ACEI or ARB + CCB + TLDU + consider
further diuretic or alpha-blocker or beta-
blocker
Consider seeking expert advice
Monitor drug treatment
Review annually

The Eighth Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of
High Blood Pressure (JNC 8) in adults was published in December 2013.

Adults aged > 18 yrs with HTN
Implement lifestyle interventions
(continue throughout management)
Set BP goal & initiate BP lowering medication based on
age, diabetes & CKD
Age > 60 yrs Age < 60 yrs
All ages DM
present, no
CKD
All ages CKD
present with or
without DM
No DM or CKD DM or CKD present
BP goal
SBP <
150mmHg
DBP < 90mmHg
BP goal
SBP <
140mmHg
DBP < 90 mmHg
BP goal
SBP <
140mmHg
DBP < 90mmHg
BP goal
SBP
<140mmHg
DBP < 90mmHg
Initiate thiazide type
DIU or ACEI or ARB or
CCB, alone or in
combination
Initiate thiazide type DIU
or CCB, alone or in
combination
Initiate ACEI or ARB,
alone or in combination
with other drug class
Non Black Black All races

Select a drug treatment titration strategya) Maximize 1st medication before adding second or
b) Add 2nd medication before reaching max. dose of 1st medication orc) Start with 2 medication classes separately or as fixed dose combination
Reinforce medication & lifestyle adherence
For strategies A & B, add & titrate thiazide type DIU or ACEI or ARB
or CCB (use medication class not previously selected & avoid
combined use of ACEI & ARB)
Reinforce medication & lifestyle adherence
Add and titrate thiazide type DIU or ACEI or ARB or CCB (use
medication class not previously selected & avoid combined use of
ACEI & ARB)
Reinforce medication & lifestyle adherence
Add additional medication (e.g. B-blocker, aldosterone antagonist, or
others) and/or refer to physician with expertise in Hypertension
management
At goal BP ?
At goal BP ?
At goal BP ?
At goal BP ?
Continue
current
treatment
&
monitoring
yes
no
yes
yes
yes
no
no
no

Lifestyle modifications
• JNC 8 recommendations to lower BP and decrease cardiovascular
disease risk include the following, with greater results achieved
when 2 or more lifestyle modifications are combined :
• Weight loss (range of approximate systolic BP reduction [SBP],
5-20 mm Hg per 10 kg)
• Limit alcohol intake to no more than 1 oz (30 mL) of ethanol per
day for men or 0.5 oz (15 mL) of ethanol per day for women and
people of lighter weight (range of approximate SBP reduction, 2-
4 mm Hg)
• Reduce sodium intake to no more than 100 mmol/day (2.4 g
sodium or 6 g sodium chloride; range of approximate SBP
reduction, 2-8 mm Hg)

Lifestyle modifications
• Maintain adequate intake of dietary potassium (approximately 90
mmol/day)
• Maintain adequate intake of dietary calcium and magnesium for
general health
• Stop smoking and reduce intake of dietary saturated fat and
cholesterol for overall cardiovascular health
• Engage in aerobic exercise at least 30 minutes daily for most days
(range of approximate SBP reduction, 4-9 mm Hg)

Pharmacologic therapy
• If lifestyle modifications are insufficient to achieve the goal BP, there
are several drug options for treating and managing hypertension.
• Compelling indications may include high-risk conditions such as heart
failure, ischemic heart disease, chronic kidney disease, and recurrent
stroke, or those conditions commonly associated with hypertension,
including diabetes and high coronary disease risk.

Pharmacologic therapy
• Drug intolerability or contraindications may also be factors.
• An angiotensin-converting enzyme (ACE) inhibitor, angiotensin
receptor blocker (ARB), calcium channel blocker (CCB), and beta-
blocker are all acceptable alternative agents in such compelling
cases.

GUIDELINES FOR SELECTING INITIAL DRUG
TREATMENT OF HYPERTENSION
Class of Drug Compelling
Indications
Possible
Indications
Compelling
Contraindi-
cations
Possible
Contraindi-
cations
Diuretics Heart failure
Elderly
patients
Systolic
hypertension
Diabetes Gout Dyslipidemia
β-Blockers Angina
After M.I
Tachyarrhythmi
as
Heart failure
Pregnancy
Asthma and
COPD
Heart block
Dyslipidemia
Athletes and
physically
active patients
Peripheral
vascular
disease

GUIDELINES FOR SELECTING INITIAL DRUG
TREATMENT OF HYPERTENSION
ACE inhibitors Heart failure
Left ventricular
dysfunction
After M.I
Diabetic
nephropathy
Chronic renal
parenchymal
disease
Pregnancy
Hyperkalemia
Bilateral renal
artery stenosis
Angiotensin
receptor
blockers
ACEI
Intolerance
Heart failure
Diabetic
nephropathy
Chronic renal
parenchymal
disease
Pregnancy
Hyperkalemia
Bilateral renal
artery stenosis
Calcium
channel
blocker
Angina
Elderly
patients
Systolic
hypertension
Peripheral
vascular
disease
Heart block Congestive
heart failure


Resistant Hypertension
• Resistant hypertension is defined as the failure to reach
blood pressure control in patients who are adherent to full
doses of an appropriate three-drug regimen (including a
diuretic).

CAUSES OF RESISTANT HYPERTENSION
• Improper BP measurement
• Volume overload & pseudotolerance
– Excess sodium intake
– Volume retention from kidney disease
– Inadequate diuretic therapy
• Associated conditions– Obesity
– Excess alcohol intake
• Identifiable causes of HTN
• Drug-induced or other causes– Nonadherence
– Inadequate doses
– Inappropriate combinations
– NSAIDS ; COX 2 Inhibitors, cocaine, amphetamines, other illicit drugs
– Sympathomimetics(decongestants, anoretics)
– Oral contraceptives
– Adrenal steroids
– Cyclosporine & tacrolimus
– Ertythropoietn
– Licorice (including some chewing tobacco)
– Selected over the counter dietary supplements & medicines (eg, ephedra, ma huang, bitter orange)

Hypertensive Urgencies
• Hypertensive urgencies are situations in which blood pressure must
be reduced within a few hours.
• These include patients with asymptomatic severe hypertension
(systolic blood pressure > 220 mm Hg or diastolic pressure > 125
mm Hg that persists after a period of observation) and those with
optic disk edema, progressive target organ complications, and
severe perioperative hypertension.

Hypertensive Emergencies
• Hypertensive emergencies require substantial reduction of
blood pressure within 1 hour to avoid the risk of serious
morbidity or death.
• Emergencies include ;
– Hypertensive encephalopathy (headache, irritability,
confusion, and altered mental status due to cerebrovascular
spasm)
– Hypertensive nephropathy ( hematuria, proteinuria,and
progressive kidney dysfunction due to arteriolar necrosis and
intimal hyperplasia of the interlobular arteries ),
– Intracranial hemorrhage, aortic dissection, preeclampsia,
eclampsia, pulmonary edema, unstable angina, or
myocardial infarction.




Malignant Hypertension
Malignant hypertension is by historical definition
characterized by encephalopathy or nephropathy with
accompanying papilledema.

Management of hypertension in
pregnancy
• There are three types of hypertension seen in pregnant women:
i. Chronic or pre-existing hypertension
ii. Gestational hypertension
iii. Pre-eclampsia and eclampsia.

• During the normal pregnancy there is a reduction in blood pressure
due to a fall in systemic vascular resistance which is maximal by
weeks 22–24.
• Patients with pre-existing hypertension should discontinue ACE
inhibitors and ARBs which are associated with abnormalities of the
developing fetal renal system.
• The first-line therapy during pregnancy is methyldopa which has no
adverse effects on the fetus although sedating side-effects may limit
up-titration.
• Second-line agents include nifedipine and labetalol.
• The target blood pressure should be <150/100 mmHg.

• Gestational hypertension is a blood pressure of >140/90 mmHg in
the 2nd trimester in a previously normotensive woman.
• These patients should have twice-weekly BP measurements and
urine tested for protein as there is an increased risk of developing
pre-eclampsia
• Patients with moderate hypertension (159–150/109–100 mmHg)
should commence oral labetalol and have blood tests performed
(electrolytes, blood count, liver function tests) and those with severe
hypertension (≥160/110 mmHg) should be admitted to hospital.

• Pre-eclampsia is a multi-system disorder that occurs after 20 weeks’
gestation consisting of:
• Hypertension
• Oedema
• Proteinuria (>0.3 g/24 hours).
• These patients should be admitted and treated for hypertension with
regular BP measurements (4 times daily) and blood tests 2–3/week.
• Patients who progress to eclampsia (convulsions) and/or HELLP
(haemolysis, elevated liver enzymes, low platelet count) syndrome
should be admitted to a critical care unit and may require intravenous
hydralazine, labetalol, and magnesium sulphate (for convulsions) and
prompt delivery.

• Taking at least 30 minutes of regular physical exercise is expected to
have what effect on systolic blood pressure ?
a) An increase of 4-7mmHg
b) No effect expected
c) A reduction of 1-2mmHg
d) A reduction of 4-9mmHg

• What is the target blood pressure for a patient with type 2 diabetes
(assuming no co-morbidities) ?
a) Less than 120/75mmHg
b) Less than 130/80mmHg
c) Less than 140/80mmHg
d) Less than 150/90mmHg

• Which ONE of the following treatments should be used first-line for a
73 year old patient with primary hypertension?
a) Atenolol
b) Indapamide
c) Amlodipine
d) Ramipril

THANK YOU