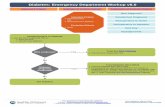
How to navigate through a diabetes emergency
Click here to load reader
-
Upload
stephen-mabry -
Category
Health & Medicine
-
view
174 -
download
4
description
Transcript of How to navigate through a diabetes emergency

How to navigate through a diabetes emergency April 26, 2014
1
How to navigate through a diabetes emergency:
Correct the Blood glucose
Chase down the Cause
Consider what you learned High BG, ketones and sick days 2 key concepts: fluids and insulin What ketones tell you Fluid management Insulin adjustments

How to navigate through a diabetes emergency April 26, 2014
2
Other considerations: nutrition, activity, frequency of monitoring, preventing hypo (mini glucagon rescue) Practice examples
Time
Blood glucose
Ketones
What to do ?
7 AM
450
Large
9 AM
380
Large
12 N
350
Moderate
2 PM
260
Moderate
4 PM
346
Small
6 PM
230
Moderate
9 PM
180
Moderate
When would you call the diabetes team?
Yes No, not yet
Situation
Gave 3 extra doses and child no better (still sleepy and won’t drink) Gave 2 extra doses, child drinking and eating well, ketones coming down Fever, won’t drink Breathing hard, looks sick Sore throat, blood glucose high but no ketones BG high, no ketones, gave usual AM dose, now child won't eat Child vomited twice, BG normal, small ketones, due for supper dose

How to navigate through a diabetes emergency April 26, 2014
3
Mini Dose Glucagon Rescue for hypoglycemia during illness
Consult your diabetes team about the use of this treatment! When to use:
• BG less than 80 AND • Stomach illness with nausea or vomiting
DO NOT USE Mini dose glucagon AS A TREATMENT FOR SEVERE HYPOGLYCEMIA. Use the full dose of glucagon. Mini dose glucagon Dosing:
Age Initial Dose (glucagon drawn with an insulin syringe)
2 years and younger 2 units (20 mcg) 2 to 15 years old 1 unit (10 mcg) for year of age 15 and older 15 units (150 mcg) What to expect:
• BG may rise 60-90 mg/dl and last about one hour. • If the BG does not rise sufficiently within 20-30 minutes the glucagon
dose can be doubled and given again. • These doses may be given every 1-2 hours as needed. • Mixed glucagon can be stored in the refrigerator and used for up to
24 hours. Any unused glucagon should be discarded after 24 hours.
Reference
Haymond, M. ,& Schreiner, B. (2001). Mini-dose glucagon rescue for hypoglycemia in children with Type 1 diabetes. Diabetes Care. 24(4): 643-645.

How to navigate through a diabetes emergency April 26, 2014
4
Finding patterns in the chaos: Putting blood sugar data to work to predict and prevent problems What
• What are your BG goals? When
• When are BG levels out of target? Why
• Why are the BG levels out of target? How
• How will you bring the BG levels back into target? References Chase, Peter. (2006). Understanding Diabetes, 11th Edition Chase, Peter. (2007). Understanding Insulin Pumps & Continuous Glucose Monitors Available to read at: http://www.ucdenver.edu/academics/colleges/medicalschool/centers/BarbaraDavis/OnlineBooks/Pages/default.aspx

How to navigate through a diabetes emergency April 26, 2014
5
Brk Lu Su Brk
AA BB CC DD EE FF
Brk Lu Su Brk
AA BB CC DD EE FF
Brk Lu Su Brk
AA BB CC DD EE FF
WHEN?
INTERPRETING BLOOD GLUCOSE VALUES
Time Frame
Blood glucose
Dose affected
1-2 hours after Breakfast
Breakfast Bolus
4-5 hours after Breakfast
Basal
1-2 hours after Lunch
Lunch Bolus
4-5 hours after Lunch
Basal or May indicate need for snack bolus
1-2 hours after Supper
Supper Bolus
Overnight: 9-12 MN MN-3 AM 3AM-7 AM
Basal rate: 30 mg/dl difference from one time frame to another may indicate need to adjust rate (Some need an overnight rate twice the daytime rate)

How to navigate through a diabetes emergency April 26, 2014
6
WHY? INSULIN • Amount: What are current doses?
• Timing: When is the insulin given in relation to the meal? • Freshness: How old is the vial or pen of insulin being used? • How is insulin stored? • Is it the correct type of insulin? • Is the total daily amount reasonable? • How does the insulin seem to work for this child? • Who gives the dose — if child, is he or she supervised? • Is it possible that doses have been missed? How often? • Have doses recently changed? What was the effect?
SITES • Are sites lumpy? • What is current rotation pattern? • What angle is used for injection? • What length needle is used? Is injection going too shallow? • Does insulin leak from site after injection?
CHILD GROWTH
• How old is child? Going through growth spurt? • (Girls) Is menarche/menses affecting BG? • (Girls) Is it possible the teen is pregnant? (Episodes of unexplained hypoglycemia may occur in 1st trimester.)
HYPO-
GLYCEMIA • What time of day? What are common symptoms? • What is BG during symptoms? What is BG following episode? • How is hypoglycemia treated? Is it overtreated? • Nausea • Nightmares; restless sleep • Chronic headache; headache in morning when wakes up
KETONES • Are ketones only in am. — and clear later in day without extra insulin? • Are there ketones at other times? • How quickly do the ketones clear and by what means?
EXERCISE • What type/duration/time? If child, when is PE? • Is child experiencing post exercise hypoglycemia?
DIET • Adherence with meal plan? What types of snacks? • How close is meal time to testing time? LIFE
ISSUES • Is there family/work/school stress? • Could there be an eating disorder? • Has there been unexplained weight gain or loss?
CHECKING • What type of meter is used? Any recent meter problems? • When was it last calibrated or controlled? • If child, is he or she supervised? • What are BG results at "odd" times (after meals, night, etc.) • What is the recent A1c result?