GEMC- Oral and Dental Emergencies: The Patient with a Sore Throat- Resident Training
-
Upload
openmichigan -
Category
Education
-
view
106 -
download
0
description
Transcript of GEMC- Oral and Dental Emergencies: The Patient with a Sore Throat- Resident Training

Project: Ghana Emergency Medicine Collaborative
Document Title: Oral and Dental Emergencies: The Patient With A Sore
Throat
Author(s): Joe Lex, MD, FAAEM, FACEP (Temple University) 2013
License: Unless otherwise noted, this material is made available under the
terms of the Creative Commons Attribution Share Alike-3.0 License:
http://creativecommons.org/licenses/by-sa/3.0/
We have reviewed this material in accordance with U.S. Copyright Law and have tried to maximize your
ability to use, share, and adapt it. These lectures have been modified in the process of making a publicly
shareable version. The citation key on the following slide provides information about how you may share and
adapt this material.
Copyright holders of content included in this material should contact [email protected] with any
questions, corrections, or clarification regarding the use of content.
For more information about how to cite these materials visit http://open.umich.edu/privacy-and-terms-use.
Any medical information in this material is intended to inform and educate and is not a tool for self-diagnosis
or a replacement for medical evaluation, advice, diagnosis or treatment by a healthcare professional. Please
speak to your physician if you have questions about your medical condition.
Viewer discretion is advised: Some medical content is graphic and may not be suitable for all viewers.
1

Attribution Key
for more information see: http://open.umich.edu/wiki/AttributionPolicy
Use + Share + Adapt
Make Your Own Assessment
Creative Commons – Attribution License
Creative Commons – Attribution Share Alike License
Creative Commons – Attribution Noncommercial License
Creative Commons – Attribution Noncommercial Share Alike License
GNU – Free Documentation License
Creative Commons – Zero Waiver
Public Domain – Ineligible: Works that are ineligible for copyright protection in the U.S. (17 USC § 102(b)) *laws in
your jurisdiction may differ
Public Domain – Expired: Works that are no longer protected due to an expired copyright term.
Public Domain – Government: Works that are produced by the U.S. Government. (17 USC § 105)
Public Domain – Self Dedicated: Works that a copyright holder has dedicated to the public domain.
Fair Use: Use of works that is determined to be Fair consistent with the U.S. Copyright Act. (17 USC § 107) *laws in your
jurisdiction may differ
Our determination DOES NOT mean that all uses of this 3rd-party content are Fair Uses and we DO NOT guarantee that
your use of the content is Fair.
To use this content you should do your own independent analysis to determine whether or not your use will be Fair.
{ Content the copyright holder, author, or law permits you to use, share and adapt. }
{ Content Open.Michigan believes can be used, shared, and adapted because it is ineligible for copyright. }
{ Content Open.Michigan has used under a Fair Use determination. }
2

Oral and Dental Emergencies
The Patient with a Sore Throat
Joe Lex, MD, FACEP, FAAEM
Associate Professor, Department of
Emergency Medicine
Temple University School of Medicine
Philadelphia, PA

Objectives
1. Understand that teething does
not cause fever
2. Define, recognize, and treat
pericoronitis, periapical abscess,
and alveolar osteitis
3. Describe treatment for ANUG
4. State three ways to treat bleeding
gums

Objectives
5. Identify and differentiate among
these mouth lesions: aphthous,
HSV, herpangina, perlèche
6. Describe the demographics of
GABHS
7. Memorize the Centor criteria
8. Know the rationale behind using
antibiotics to treat a sore throat

Teeth
David Shankbone, Wikimedia Commons

How Many Teeth?
32 permanent
• 8 incisors
• 4 canines
(cuspids)
• 8 premolars
(bicuspids)
• 12 molars
(tricuspids)
20 primary or
deciduous
• 8 incisors
• 4 canines
• 8 molars

How to Name the Teeth
Gray’s Anatomy, Wikimedia Commons

Source Undetermined

Source Undetermined

Definitions
• Interproximal: the surfaces
between two adjacent teeth
• Mesial: interproximal surface
facing toward midline
• Distal: interproximal surface facing
away from midline
• Occlusal: chewing surface

Definitions
• Labial: toward the lips, specific to
anterior teeth
• Buccal: toward the cheek, specific
to posterior teeth
• Palatal: toward the palate, specific
to maxillary teeth
• Lingual: toward the tongue,
specific to mandibular teeth

Definitions
• Apical: toward the tip of the root of
the tooth
• Radicular: associated with the
root, especially the apical region
• Coronal: toward the crown of the
tooth
• Incisal: toward the biting edge of
incisors

Basic Anatomy
• Dentin surrounds pulp, which is
neurovascular supply
• Crown: enamel on dentin, visible
portion of tooth
• Root: cementum on dentin,
extends into the alveolar bone

Sam Fentress, Wikimedia
Commons

Basic Anatomy
• Periodontium = attachment
apparatus
• Periodontal ligament = collagen
fibers that extend from alveolar
bone to root of tooth
• Gingivitis and periodontal disease
destroy peridontium tooth
mobility and loss

Basic Anatomy
• Gingiva = keratinized stratified squamous epithelium
– Free gingiva: 2- to 3- mm-deep gingival sulcus in disease-free state
– Attached gingiva: adheres to alveolar bone and extends to oral vestibule, floor of mouth
• Nonkeratinized alveolar mucosa covers cheeks, lips, floor of mouth

Teething
Daniel Schwen, Wikimedia Commons Vmg13, Wikimedia Commons

About ye seveth moneth, sometime more,
sometime lesse, after ye byrth, it is natural
for a child to breed teeth, in which time
many one is sore vexed with sondry
diseases and pains, as swelling of ye
gummes and jaws, unquiet crying fevers,
cramps, palsies, fluxes, reumes and other
infirmities, specially when it is long or ye
teeth come forth, for the sooner they appear
the better and the more ease it is to the childe.
Thomas Phayre – 1530
The Boke of Children, London

Death by Teething!!
• Common “Cause of Death” in
Middle Ages
• Usually weaned at same time
• Frequently lance erupting tooth
• Malnutrition from watered-down
milk
• Typhus from infected milk

Teething
• No data support association of
teething, fever, and diarrhea
• Possible mild dehydration from
excessive salivary production or
decreased intake
• Must seek other source
for fever, diarrhea

Pain from Wisdom Teeth
• Erupting third molars
• Pericoronitis: inflammation of
gingival tissue overlying occlusal
surface of erupting tooth
(operculum)
• Masseter irritation trismus
• Rx irrigate debris, antibiotic,
analgesia, dental referral

Pericoronitis
Coronation Dental Specialty Group, Wikimedia Commons

Dental Caries
• Loss of tooth enamel integrity due
to exposure to acidic metabolic
byproducts of plaque bacteria
• Early: sensitive to cold or sweet
• Later: direct communication with
dental pulp “pulpitis”
• Irreversible pulpitis: protracted
pain

Dental Caries
Dozenist, Wikimedia Commons

Antibiotics for Toothache??
• Undifferentiated dental pain
without overt infection
• Penicillin vs. placebo
• Evaluation at enrollment, again at
5- to 7-day follow-up
• Outcome measure: overt dental
infection at follow-up
Acad Emerg Med. 2004 Dec;11(12):1268-71.

Antibiotics for Toothache??
• 13 / 134 patients (9%) developed
infection
– 6/64 (9%) in penicillin group
– 7/70 (10%) in placebo group
• No significant difference in
baseline characteristics,
compliance, VAS pain scores
Acad Emerg Med. 2004 Dec;11(12):1268-71.

Antibiotics for Toothache??
• CONCLUSIONS: “These data
support the hypothesis that
penicillin is neither necessary nor
beneficial in the treatment of
undifferentiated dental pain in the
absence of overt infection.”
Acad Emerg Med. 2004 Dec;11(12):1268-71.

Periapical Abscess
• Most common source of severe
odontogenic pain: periapical
• Most common lesion: periapical
granuloma = periradicular
periodontitis, results from pulpitis
• X-ray widened periodontal
ligament space (radiolucent stripe)

Widened periodontal
ligament space
Source Undetermined

Periapical lucency Source Undetermined

Periapical abscess Source Undetermined

Periapical Abscess
• Exquisite pain with percussion
• Suppurative periodontitis = parulis
• X-rays rarely indicated
• Rx antibiotic (penicillin still best),
analgesia, referral
• Definitive treatment: extraction or
root canal

Parulis = Fistula = Gum Boil
Source Undetermined

Postextraction Pain
• Periosteitis: 24 to 48 hours,
common, easily treated
• Alveolar osteitis = dry socket:
second or third post-op day
exquisite oral pain due to bone
exposed to oral environment

Dry Socket
• Up to 35% after impacted 3rd molar removal
• X-ray for retained root tip
• Irrigate socket with sterile saline
• Pack socket with gauze soaked in oil of cloves or eugenol
• Relief is immediate
• Antibiotic if severe

Dry Socket
Source Undetermined

Infraorbital Nerve Block
Source Undetermined

Infraorbital Nerve Block
Source Undetermined

Infraorbital Nerve Block
Source Undeternined

Mental Nerve Block
Source Undetermined

Mental Nerve Block
Source Undetermined

Mental Nerve Block
Source Undetermined

Palatal Nerve Block
Source Undetermined

Palatal Nerve Block
Source Undetermined

Palatal Nerve Block
Adapted from: Alan, Flickr

Inferior Alveolar Nerve Block
Gray’s Anatomy, Wikimedia Commons

Inferior Alveolar Nerve Block
Source Undetermined

Inferior Alveolar Nerve Block
Adapted from: Lusb, Wikimedia Commons

Inferior Alveolar Nerve Block
Source Undetermined

Inferior Alveolar Nerve Block
Mikael Häggström, Wikipedia

Frenum Diastema
i.e., gap-toothed
Bryon Viechnicki, Wikimedia
Commons

Tetracycline Staining
Source Undetermined

Periodontal Disease
• Gingivitis: accumulation of plaque
along gum margins
• Causes: bad hygiene, hormonal
variations (puberty, pregnancy),
medications (phenytoin), etc.
• Sulcus deepens pockets
periodontitis mineralization
bone loss tooth loss

Periodontal Disease
Source Undetermined

Periodontal Disease
Source Undetermined

ANUG
• Acute Necrotizing Ulcerative
Gingivitis = Vincent ´s disease =
trench mouth
• Diagnostic triad: pain + ulcerated
or “punched out” interdental
papillae + gingival bleeding
• Etiology unclear, but opportunistic
• Anaerobes always present

ANUG
• Invades otherwise healthy tissue
• Treatment:
– Identify, treat predisposing factors
– Chlorhexidine oral rinses twice daily
– Debridement and scaling by dentist
– Metronidazole 250 mg tid
– Supportive therapy: soft diet rich in
protein and vitamins

ANUG
Source Undetermined

ANUG
Source Undetermined

Gingival Hyperplasia
• Associated with many commonly
used medications
• 50% of patients on chronic
phenytoin
• Also calcium channel blockers
(especially nifedipine) and
cyclosporine.
• Treatment: fastidious oral hygiene

Gingival Hyperplasia
Lesion, Wikimedia Commons

Bleeding Gums
• Hemorrhage after scaling easily
controlled with peroxide mouth
rinses or direct gingival pressure
• Clotting factor deficiencies,
leukemia, and end- stage liver
disease may first present as
spontaneous gingival hemorrhage
• Treatment: based on cause

Bleeding Gums
Source Undetermined

Bleeding Gums
Source Undetermined

Post-Extraction Bleeding
Usually a dislodged clot
1. Firm pressure usually adequate:
folded 2 × 2 gauze pad placed over
extraction site, then firm pressure by
clenching teeth for 20 minutes
2. Tea bag: tannic acid is hemostatic
3. Gel-Foam, Avitene, or Instat sutured
snugly into socket
4. Infiltrate lidocaine with epinephrine

Pyogenic Granuloma
• “Pregnancy tumor”
• Benign proliferation of connective
tissue, primarily on gingiva
• Not pyogenic, not a granuloma
• Usually recurs if removed during
pregnancy
• If not regressed 2 to 3 months
postpartum, definitive removal

Pyogenic Granuloma
Source Undetermined

Pyogenic Granuloma
Kuebi, Wikimedia Commons

Before We Leave the Gums…
Intentional pain
And the taste of gums bleeding
Prevent toothlessness
Morsels sit between my teeth
Minty, waxy nylon thread
Saves my smile
Two Flossing Haiku

Oral Candidiasis
• Present in 60% of healthy adults
• Opportunistic pathogen: many risk
factors
• Adherent white plaque
• Perioral = angular cheilitis
• Rx topical oral (nystatin) or
systemic (fluconazole) antifungal
agent

Oral Candidiasis
James Heilman, MD, Wikimedia Commons

Oral Candidiasis
Centers for Disease Control and Prevention, Wikimedia Commons

Angular Cheilitis = Perlèche
• Breakdown at labial commissures
• Candida albicans implicated
• Radiation therapy
• HIV
• Dietary deficiencies
• Antifungal with steroid may help

Angular Cheilitis = Perlèche
James Heilman, MD, Wikimedia Commons

Angular Cheilitis = Perlèche
Lesion, Wikimedia Commons

Angular Cheilitis = Perlèche
Source Undetermined

Aphthous Stomatitis
• Canker sores: common
• Probable cell-mediated response
• Nonkeratinized epithelium
• Superficial painful ulcers
• Resolve in 10 – 14 days
• Rx topical steroid: betamethasone syrup or 0.01% dexamethasone elixir mouth rinse

Aphthous Stomatitis
Noorus, Wikimedia Commons

HSV = Cold Sores
• Type 1 most common
• Gingivostomatitis: painful
ulcerations on mucosal surfaces
• Fever, lymphadenitis common
• Prodrome: tingling 1 – 2 days
before outbreak
• Rx palliative: antivirals started
during prodrome severity

HSV = Cold Sores
Centers for Disease Control and Prevention, Wikimedia
Commons
WarXboT, Wikimedia Commons

Herpangina
• Coxsackieviruses
• Summer and autumn
• Sudden high fever, sore throat,
headache, malaise then vesicles
• Soft palate, uvula, posterior
pharynx, tonsillar pillars
• Buccal mucosa, tongue, gums
spared

Herpangina
• Lasts 7 to 10 days
• Distinguished from herpetic
gingivostomatitis by lack of gingival
involvement
United Kingdom Royal Navy,
Wikimedia Commons

Herpangina
Shawn C, Wikimedia Commons
Aphilosophicalmind, Wikimedia Commons

Hand, Foot, and Mouth
• Coxsackievirus
• Vesicles on tongue, gums, soft palate, buccal mucosa
• Rupture painful, shallow ulcers with red halo
• Lateral & dorsal fingers & toes
• Fever day or two, rash 5 to 8 days
• Treatment: palliative

Hand, Foot, and Mouth
MidgleyDJ, Wikimedia Commons
James Heilman, MD, Wikimedia Commons
Ngufra, Wikimedia Commons

Lichen Planus
• Chronic cutaneous
vesiculoerosive disease
• T- lymphocytes on basal cell layer
• Scattered white papules
interconnected with white lines
(Wickham’s striae)
• Symptomatic: topical steroids

Lichen Planus
Source Undetermined

Cheek Chewing
Source Undetermined

Aspirin Burn (ASAcid!)
Source Undetermined

Aspirin Burn (ASAcid!)
Source Undetermined

Torus Palatinus
• Hard, firm isolated mass on hard
palate.
• May be several centimeters
• Appears in adulthood
• Don’t confuse with neoplasm
• May interfere with dentures

Torus Palatinus
Dozenist, Wikimedia Commons

Torus Mandibularis
Source Undetermined

Denture Stomatitis
Source Undetermined Source Undetermined

Nicotine Stomatitis
Source Undetermined

Uvulitis
• Quincke’s disease
• Patient complains “something
hanging down my throat”
• Bacteria, virus, angioedema
• Treatment symptomatic: antibiotic,
antihistamine, nebulized steroid or
epinephrine

Uvular Angioedema
Source Undetermined

Ludwig’s Angina
• Cellulitis of submandibular and
lingual spaces
• Potentially life threatening.
• Rapidly spreading cellulitis
• Brawny induration of suprahyoid
region and elevation of tongue

Ludwig’s Angina
• Epiglottis can be involved
• Airway compromise is immediate
concern
• Treatment: high- dose penicillin
and metronidazole or cefoxitin,
immediate oral and maxillofacial
consultation

Ludwig’s Angina
Stevenfruitsmaak, Wikimedia Commons

Ludwig’s Angina
Source Undetermined

Geographic Tongue
• Erythema migrans = geographic
tongue = benign migratory
glossitis
• Multiple, well-demarcated zones
of erythema due to atrophy of
filiform papillae
• Usually asymptomatic
• Reassurance sufficient

Geographic Tongue
Bin im Garten, Wikimedia Commons

Geographic Tongue
Martanopue, Wikimedia Commons

Fissured Tongue
Kozlovsk, Wikimedia Commons

Scrotal Tongue
Source Undetermined

Median Rhomboid Glossitis
• Believed to be developmental
defect of the dorsal surface of the
tongue
• 1 x 2 cm ovoid erythematous area
just anterior to circumvallate
papillae
• Devoid of papillae, asymptomatic
• No treatment necessary

Median Rhomboid Glossitis
Klaus D. Peter, Wikimedia Commons

Black Hairy Tongue
• Discoloration of elongated filiform
papillae
• Can grow up to 18 mm
• Usually asymptomatic
• Treatment: frequent tongue
brushing, avoid tobacco, strong
mouthwashes, antibiotics
• Resolution usually spontaneous

White Hairy Tongue
Source Undetermined Source Undetermined

Black Hairy Tongue
Source Undetermined
Source Undetermined

Pepto-Bismol® Tongue
• Bismuth + sulfur (in saliva) =
bismuth sulfide = black tongue
(and sometimes black stool)
• Harmless, self limited
Source Undetermined

Strawberry Tongue
• Associated with erythrogenic
toxin-producing Streptococcus
pyogenes or Kawasaki disease
• Prominent red spots on white-
coated background.
• Treatment: antibiotics directed at
group A streptococci

Strawberry Tongue
Source Undetermined

Strawberry Tongue
Source Undetermined

Leukoplakia (Precancerous)
Source Undetermined

Leukoplakia (Precancerous)
Source Undetermined

Frenulum
Jean-Rene Vauzelle, Wikimedia Commons Zabbed, Wikimedia Commons

Salivary Glands
BruceBlaus, Wikimedia Commons

Salivary Glands
• Parotid and submandibular
• Parotid (Stenson) duct opens
opposite upper second molar
• Submandibular ducts open into
mouth at either side of frenulum
• Multiple sublingual ducts open into
sublingual fold or submandibular
duct

Viral Parotiditis
• Mumps: paramyxovirus
• Incubation period: 12 to 21 days.
• Infective from 3 days prior to 7
days after salivary gland swelling
• Repeat episodes possible
• Others: influenza, enteroviruses,
cytomegalovirus, human
immunodeficiency virus (HIV).

Viral Parotiditis
• Swelling bilateral ~70%
• May be surrounding edema
• No discharge from Stenson duct
• Benign in kids
• 25% of men suffer orchitis
• Diagnosis: clinical
• Treatment: supportive

Viral Parotiditis
Source Undetermined

Viral Parotiditis
Source Undetermined

Suppurative Parotiditis
• Debilitated, dehydrated patients
• Tender, red, swollen parotid
• Bilateral in ~25%
• Fever and trismus common
• Pus from Stenson duct
• Staphylococcus aureus mixed with anaerobes.
• Diagnosis is clinical

Suppurative Parotiditis
Source Undetermined

Sialolithiasis
• Any age, peak from 30 to 60
• >80% are submandibular
• Mostly calcium phosphate
• Pain, swelling, tenderness
• Similar to parotitis, ductal
obstructive symptoms (pain and
swelling) exacerbated by meals

Sialolithiasis
• Diagnosis clinical; extraoral x-rays
~50% sensitive
• Therapy initiated on clinical
findings: analgesics, massage,
and sialogogues, like lemon drops

Sialolithiasis
Source Undetermined Source Undetermined

Ranula – “little frog”
• Sublingual mucocele
• Benign, usually asymptomatic
• No special treatment

Ranula
Ph0t0happy, Wikimedia Commons Klaus D. Peter, Wikimedia Commons

Piercings
Tommy T, Wikimedia Commons Sara Marx, Wikimedia Commons
Doct Blake, Wikimedia Commons

The Patient with a Sore Throat
U.S. Navy, Wikimedia Commons
ParentingPatch, Wikimedia Commons

Sore Throat
• Dysphagia = difficulty
swallowing
• Odynophagia = painful
swallowing
• Pharyngitis = infection or
irritation of pharynx

Pharyngitis
• Rare under 1 year
• Uncommon under 2 years
• Peak incidence: 4 to 7 years
• Higher incidence in winter
• Viruses, bacteria, fungi, parasites
• Most common causes: rhinovirus
and adenovirus

Principles of appropriate antibiotic
use for acute pharyngitis in adults
•Large majority of adults with acute
pharyngitis have self-limited illness
•Antibiotic treatment benefits only
patients with GABHS infection
•Adults with sore throat: “Strep
throat” prevalence 5 –15%
Cooper et al. Ann Emerg Med. June 2001;37:711-719

• Offer all appropriate analgesics,
antipyretics, other supportive care
• Clinically screen adults with
pharyngitis for Centor criteria
• Do not test or treat patients with
zero or one; they are unlikely to
have GABHS
Cooper et al. Ann Emerg Med. June 2001;37:711-719
Principles of appropriate antibiotic
use for acute pharyngitis in adults

Centor Score
1. history of fever
2. tonsillar exudates
3. no cough
4. anterior cervical lymphadenitis
Score 0-1 = <5% GABHS
Score 2-3 = 5 – 30% GABHS
Score 4 = 30 – 60% GABHS
Cooper et al. Ann Emerg Med. June 2001;37:711-719

Centor
Points
Pretest probability of GABHS (%)
5 10 15 20 25 40 50
0 1 2 2 3 5 10 14
1 2 3 5 7 9 17 23
2 4 8 12 16 20 33 43
3 10 19 27 34 41 58 68
4 25 41 53 61 68 81 86
Post-test probability of GABHS

Principles of appropriate antibiotic
use for acute pharyngitis in adults
1. Rapid antigen if 2, 3, or 4
criteria; antibiotic only if test + 2. Rapid antigen if 2 or 3 criteria;
antibiotic if test + or 4 criteria
3. Antibiotic if 3 or 4 criteria; no
rapid antigen testing
Cooper et al. Ann Emerg Med. June 2001;37:711-719

• Throat culture not recommended
for routine primary evaluation of
adult with sore throat or to confirm
negative rapid antigen
• Preferred antibiotic for GABHS
pharyngitis: penicillin or
erythromycin if penicillin-allergic
Cooper et al. Ann Emerg Med. June 2001;37:711-719
Principles of appropriate antibiotic
use for acute pharyngitis in adults

“We Prevent Rheumatic Disease”
• 1/3000 untreated GABHS leads to
acute rheumatic fever
• 1000 kids / 20% prevalence = 200
• Strep screen 80% sensitive, 95%
specific
• Treat 160, send cultures on other
840 TP = 160 FP = 40
TN = 760 FN = 40

“We Prevent Rheumatic Disease”
• Prevalence now 40/840 ~5%
• Culture 95% sensitive, 95%
specific
• NNT = 798/38 = 21 cultures to find
one positive
• 3000 x 21 = 63,000 prevent one
case ARF
• NNH = 15
TP = 38 FP = 2
TN = 798 FN = 2

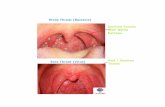
Pharyngitis – GABHS
James Heilman, MD, Wikimedia Commons

Pharyngitis – GABHS
Source Undetermined

Pharyngitis – GABHS
Real exudates Source Undetermined

Epiglottitis
• Potentially life-threatening - rapid,
unpredictable airway obstruction
• Epiglottis plus aryepiglottic folds
and pre-epiglottic and paraglottic
loose connective tissue
• Traditional: children 2 – 8 years
• Contemporary: adults increasing

Epiglottitis
• Most common: Haemophilus
influenzae type b (Hib)
• 1- to 2-day prodrome resembles
benign URI
• Exam: apprehensive, drooling,
difficulty lying flat, stridor, tongue
protruding
• Fever initially absent in 30 – 50%

Epiglottitis
• Movement of upper trachea or
thyroid cartilage painful
• Diagnosis by history, examination,
radiographs, and laryngoscopy
• Use extreme care – unpredictable
sudden airway obstruction

Epiglottitis
• Lateral soft tissue neck x-ray:
vallecula obliterated, aryepiglottic,
prevertebral and retropharyngeal
soft tissues swollen, hypopharynx
ballooned
• Find hyoid bone to find epiglottis
• Epiglottis: large, thumb-shaped

Epiglottitis
• >1/3 moderate cases initially
misdiagnosed
• Immediate otolaryngologic consult
• Never leave patient unattended
• Initial treatment: IV hydration,
oxygen, monitor, IV antibiotics.
• Be prepared for difficult intubation

Epiglottitis
藤澤孝志, Wikimedia Commons

Epiglottitis
Insert tube here
Source Undetermined

Epiglottitis
Epiglottitis
Normal epiglottis
Source Undetermined

Epiglottitis
Source Undetermined

Epiglottitis
Source Undetermined

Mononucleosis
• Classic: fever, lymphadenopathy,
exudative pharyngitis, atypical
lymphocytosis, splenomegaly
• Severe sore throat is common
complaint
• Physical: severe bilateral
exudative tonsillitis / pharyngitis –
“wet white leather”

Mononucleosis
• Treatment: supportive
• Ampicillin rash (transient EBV-
induced antibodies against drug)
• Acyclovir has in vitro effects on
EBV replication, but in vivo clinical
studies have failed to show any
clinically significant effect

Mononucleosis
Source Undetermined

Mononucleosis
Note petechiae!
Wet white leather
Source Undetermined

Mononucleosis
Cervical adenopathy
James Heilman, MD, Wikimedia Commons

Mononucleosis
Atypical lymphocytes
Ed Uthman, MD, Wikimedia Commons

PTA
• Peritonsillar abscess = quinsy:
most common deep-space
infection of head and neck
• Young adults
• Predominant bugs: Streptococcus
pyogenes, peptostreptococcus,
bacteroides, Staphylococcus
aureus

PTA
• Symptoms: fever, malaise, “hot-
potato voice,” odynophagia,
dysphagia, otalgia
• Signs: tonsil hypertrophy, swollen
deviated uvula, inferior and medial
displacement of infected tonsil,
tender cervical nodes, drooling,
bad breath, trismus

PTA
• Diagnostic gold standard:
aspiration of pus through needle
• Majority treated with outpatient
needle aspiration, antibiotics, pain
medication
• High-dose penicillin is drug of
choice

PTA
• Anesthetize mucosa using
lidocaine with epinephrine
• Insert 18-gauge needle medially
and superiorly within abscess
cavity no more than 1 cm (use
needle guard)
• Carotid artery lies laterally and
inferiorly

PTA
Large but
normal tonsils
Scurik 19, Wikimedia Commons

PTA
“Kissing” tonsils
Source Undetermined

PTA
Deviated uvula
Source Undetermined

PTA
Source Undetermined

Post-Tonsillectomy Bleed
• Classically 5 – 10 days postop
• Management: ensure airway,
control bleeding, consult ENT
• Direct pressure to tonsillar bed
• Silver nitrate, electric cautery,
oxidized cellulose, thrombin
packs, gauze moistened with
lidocaine / epinephrine

Tonsillitis – GABHS
Pbeck, Wikimedia Commons

Tonsillectomy
~3 Days
Post-op
James Heilman, MD, Wikimedia Commons

Diphtheria
Adherent exudate
Frederick Magee Rossiter,
Wikimedia Commons
Source Undetermined

Steroids for Sore Throat?
Pain improve in 24 hours (VAS)
• 1.8 ± 0.8 w/ dexamethasone
• 1.2 ± 0.9 w/ placebo (P<.05)
Time to onset of pain relief
• 6.3 ± 5.3 hrs w/ dexamethasone
• 12.4 ± 8 .5 hrs w/ placebo
(P<.01)
O'Brien et al. Ann Emerg Med 1993;22(2):212-5

Steroids for Sore Throat?
CONCLUSION: In patients with
severe, acute exudative pharyngitis,
single-injection dexamethasone
compared with placebo resulted in
statistically and clinically significant
more rapid onset and greater
degree of pain relief
O'Brien et al. Ann Emerg Med 1993;22(2):212-5

Steroids for Sore Throat?
12 and 24 hour pain relief (VAS)
• IM dexamethasone 4.2 ± 2.3
• Oral dexamethasone 3.8 ± 2.3
• Placebo 2.1 ± 2.0
Onset of pain relief average 4 hours
earlier in IM dexamethasone
group
Wei JL, et al. Laryngoscope 2002;112(1):87-93

Steroids for Sore Throat?
CONCLUSIONS: Patients treated
with IM or oral dexamethasone had
significant relief of pain (relative to
baseline) compared with patients
given placebo.
Wei JL, et al. Laryngoscope 2002;112(1):87-93

Steroids for Sore Throat?
35 IM steroid plus oral placebo
35 IM placebo plus oral steroid
No difference in pain scores at 24
(p=0.13) or 48 hours (p=0.82)
No difference in hours to relief of
pain (p=0.06)
Marvez-Valls EG, et al. Acad Emerg Med 2002;9:9-14