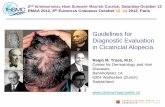
Fungal infection in hair
-
Upload
vishal-kulkarni -
Category
Health & Medicine
-
view
1.098 -
download
1
Transcript of Fungal infection in hair

Fungal Infection in HairDr Vishal Kulkarni
MBBS MD (Microbiology)

IntroductionHair is one of the defining characters
of humans. Fungi that causes infection of hair
- Trichosporon spp.- Piedra Hortae- Dermatophytes.

Piedra-• Superficial infection of hair shaft.• Often asymptomatic• Piedra (spanish)- stone• Two types-• White piedra (Trichosporon spp.)• Black piedra ( Piedra hortae)

White PiedraCaused by yeast-like fungal species of
genus Trichosporon.Present as branched hyphae & arthrospores
both within and around hair shaft.Trichomycosis nodularis OR
Trichosporonosis nodosa.Systemic infection- Trichosporonosis.Was first described by Biegel in 1865.

Mycology- Family- CryptococcaceaeClass- Basidiomycetes.
White piedra 1.Head- Trichosporon ovoides2.Pubis- Trichosporon inkin

Epidemology- Inhabits in soil & human skin. Has also been described in horses,
monkeys, dogs etc. Affects temperate & tropical areas
including Eastern Europe, Asia, South America.
More common in Black people. Incidence varies according to hair styling
fashion, social customs, hygienic conditions, humidity.


Pathogenesis & Pathology- Infection starts just beneath cuticle
following damage. Organism may grow inward & through shaft
to form nodular swellings spaced irregularly along the axis.
Hair weakened at these point hence easily breaks.
Growth occurs as collarette around hair shaft & consist of mycelia that rapidly fragment into arthrospores.


Clinical features- Soft, white, grayish or light brown
nodules on hair shaft. Seen mainly on distal portion of facial &
axillary hair, beard, moustache, pubic hair
Pruritis, pain, inflammation. Hair can be easily breaks. Mass can be
easily detached from shaft. Infection may accompanied by bacteria
like corynebacterium.

Nodules of white piedra

Differential diagnosis-- Trichomycosis axillaris- Phthiriasis pubis- Pediculosis capitis.- Geotrichum spp. infection.

Lab diagnosis- Do not fluoresce on Wood’s Lamp
examination. On microscopy- fungus is seen like concretion
that are composed of hyphae & rectangular arthrospores within & around hair. (KOH & LPCB)
Culture is done on SDA with chloramphenicol. Moist yeast like cream colored colonies.
Assimilation of glucose, maltose, sucrose, galactose & lactose.
Breaks down urea.


Black PiedraIs also nodular type of infection caused by
Piedra hortae.Also called as ‘tinea nodosa’.Mycology-
- Exists in a perfect state during colonisation.- Family- Piedraiaceae- Order- Dothideales- Class- Pyrenomycetes.- Phylum- Ascomycota.

Epidemology- Found in tropical countries in warm &
humid climates. Central & South America, Southeast Asia in
population where hair care is done with oily substances.
Exists in soil. Affects humans & animals.

Pathogenesis and pathology- Infection starts under cuticle of hair shaft
with stone hard, black nodule. Fungal mass enlarge & grow outside the
hair & completely envelop the shaft. Mature nodule in periphery composed of
aligned hyphal strands Fungus destroys cuticular layers, cortex
leads to destruction of hair shaft & breakage of hair.


Clinical features- Formation of discrete, gritty, hard, brown
black nodules firmly attached to hair shaft.
Affect mainly hair of scalp. Moustache, beard & pubic hair may be
affected. Itching usually absent.

Lab Diagnosis- Crushed brittle nodules on KOH mount. Dark colored thick walled septate
hyphae. Culture on SDA with chloramphenicol,
glycerine & cycloheximide. Slow growing, adherent, coal black,
cerebriform colonies. LCB mount shows dark walled septate
hyphae with chlymydospores. Microculture technique using DTM


Treatment & prophylaxis- Ideal T/t for both piedra is shaving off hair
in affected part. May not feasible in women. Oral azols × 3-4 weeks with topical
antifungals × 3-4 months Topical azols, ciclopirox olamine,
chlorhexidine solution, amphotericin B lotion etc.
Terbinafine 250mg/day × 6 wks for Black piedra.
Good personal hygiene.

Dermatophytes causing Hair infectionAre most common types of cutaneous
fungal infections in humans affecting skin, hair & nail.
Also known by terms like ‘tinea’ OR ‘ringworm’.
Trichophyton Skin, Hair & Nails
Microsporum Skin & Hair
Epidermophyton Skin & Nails

Hair infections caused by dermatophytes- Tinea capitis Favus Kerion Tinea barbae

Tinea capitis- Infection of shaft of scalp hair & present
as Inflammatory Noninflammatory Infected hairs appears dull & grey. Base of hair shaft & follicle are involved. Breakage of hair at follicular orifice which
creates patches of alopecia with ring formation.
Clinical types

Kerion-- Caused by T. verrucosum & T.
mentagrophytes- Severely painful inflammatory reaction
producing raised, boggy mass on scalp- Follicles discharging pus, sinus formation at
multiple points- Thick crusting with matting of adjuscent
hairs.- ‘Kerion celsi’

Favus (Tinea Favosa) Caused by T. schoenleinii Form cup like crusts around infected follicles. Fungal growth within hair is minimal which remains intact. Patchy alopecia, scarring.
Black-dot Caused by T. tonsurans & T. violaceum Endothrix like invasion. Breakage of hair near surface results in
blackdot appearance.

Ectothrix infections• The arthrospores
appear as mosaic sheath around hair or on surface of hair shaft.
• Cuticle remains intact.
Endothrix infection• Hyphae form
arthrospores within the hair shaft
• Cuticle usually get destroyed.
Ectothrix Endothrix T.mentagrophytes T.schoenleinii
M.canis T.tonsuransM.gypseum T.violaceumM.audouinii T.Soudanense
T.verrucosumT.Rubrum


Tinea barbae Caused by T.verrucosum,
T.mentagrophyte, M.canis Ringworm infection of beard &
moustache areas Also called as ‘Barber’s itch’. Erythematous patches on face, scaling Fragile & lusterless hair.

Diagnosis- Clinical examinationHistory- age, occupation, hobbies, living
conditions, onset, duration & progress.Lab diagnosis-
Microscopy Isolation of fungus in cultureSerological tests

Direct examination-KOH wet mount simple & reliableBasal root portion of hair is taken by plucking &
not by clippingFungus is seen as branching hyaline mycelia with
arthrospore production

Wood lamp examination-
Principle Flurescence produced mainly by microsporum &
rarely by trichophyton spp.
Microorganisms Fluorescence colorM.Audouinii Bright greenM.Canis Bright greenM.ferrogineum Blue greenM.gypseum Dull yellowT.schoenleinii Dull yellowMalessezia furfur Golden yellowCoeynebacterium minutissimum
Coral red

Fungal culture-SDA with cycloheximide incubated at 3 temp.
i.e. 25˚C, 30 ˚C & 37 ˚C.Colony morphology & LCB microscopy DTM – dermatophytes turns medium into red
color.DIM- to avoide false positive results given by
DTMSpecies Colony morphology LCB mount
Trichophyton spp.
Powdery, velvety, waxy with pigment
Macroconidia- sparse, pensil shaped with blunt endMicroconidia-abundunt
Microsporum Cottony, velvety, powdery with white to brown pigment
Macroconidia- abundunt, spindle shaped, rough.Microconidia- scanty

ImmunodiagnosisSkin test with dermatophytic Ag ‘trichphytin’.Serological tests- immunodiffusionPCR fingerprinting
Animal pathogenicity- To study the nature of the lesion & immunity
produced by organisms.

Treatment & prophylaxis- Topical antifungals Oral griseofulvin 10mg/kg (for nail & scalp) Or single dose 2gm in adults. Micronised prepatrations. Resistance Itraconazole, fluconazole & terbinafine therapy
for 12 weeks ‘Live spore vaccine’, killed cell vaccine &
soluble cytoplasmic extract for T. mentagrophyte.
Good personal hygiene.

Thank you…