FETAL MEMBRANES Placenta Nutrition - 3. lékařská fakulta · PDF fileFetal...
Transcript of FETAL MEMBRANES Placenta Nutrition - 3. lékařská fakulta · PDF fileFetal...

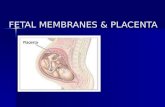
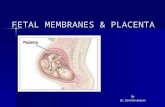
FETAL MEMBRANESPlacentaNutrition
2011

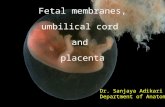
Fetal membranes
Chorion Amnion Yolk sac Allantois They develop from zygote, however they
are not involved in embryo formation except for small part of yolk sac, that participate on gut formation

Amnion Amnionic fluid Amnioblasts,
interstitial fluid form endometrium
Embryo (before skin keratinization) – transudation from body
Umbilical cord Respiratory system,
urine
10th week – 30ml 20th week – 350ml 37th week - 700-
1000ml

Function of amniotic fluid It allows symetric growth Protects from infection Facilitates normal development of lung Protects from adhesion Protects from injury Keeps stabile temperature Alows free movement Takes place in homeostasis (electrolytes)

Failures of amnionic fluid volume
Oligohydramnion – less than 400ml - rupture of fetal membranes, renal agenesis – (Potter syndrome) - pulmonary hypoplasia, pes equinovarus, face dysmorfy
Polyhydramnion – more than 2000 ml – malformed CNS, esofageal atresia, twins, idiopatic

Yolk sac Transfer and metabolism of nutrients – as
liver Development of blood cells and vessels
-vitelline vascular system Participation on formation of primitive
gut Primordial gamets in endoderm of yolk
sac during 3rd week

Allantois Development form hindgut – evagination
into embryonic stalk - only transient Vessels – umbilical arteries and veins for
placenta supply Intraembryonic part – urachus, urinary
bladder ( ligamentum umbilicale medianum)

Placenta Fetal organ providing nutrition and many
other functions: Function:
− Metabolism (synthesis, for example glycogen)− Transport of gases and nutrients− Excretion of waste products− Production of hormones (hCG)

Embryo nutrition Nutrients supply in yolk sac (AA, lipids) Histiotrophe – secret from glandular cells
in fallopian tube, uterus, digestion of endometrium
Haematotrophe – maternal blood Organ that provide nutrition of embryo in
mammals - chorion/placenta

Placenta - structure Fetal part – chorion – chorionic plate and
chorionic villi Maternal part – endometrium – pars
functionalis – decidua basalis

Decidua Zona functionalis that is changing during
pregnancy Decidua basalis Decidua capsularis Decidua parietalis
Progesteron – cell in stroma (fibroblasts) are changed in decidual cells (content of glycogen and lipids)+ changes in vascular supply = decidual reaction

Implantation

Implantation During implantation embryo invades in
zona functionalis of endometrium Trophoblast diferentiates into
syncytiotrophoblast and cytotrophoblast Extraembryonic mesoderm adds to
cytotrophoblast
= CHORION


Development of chorionic villi Primary: Syncytiotrophoblast and
cytotrophoblast Secondary: Syncytiotrophoblast,
cytotrophoblast and extraembryonic mesoderm
Tertiary: Vessels occur in mesoderm Terctiary villi are all from 3rd week of
development

Placenta development Chorion laeve Chorion frondosum Decidua capsularis get thiner, later
disappears, chorion laeve is on the surface, it unites with decidua parietalis and obliterates uterine cavity ( week 22 -24)

Intervillous space It develops from lacunae in sytiotrophoblast
It is divided by placental septa
Maternal blood – spiral arteries in decidua basalis – uteroplacental vessels
It wash up villi – it is drained into placental veins. Fetal and maternal blood do not mix !!!
Hemocytoblasts (stem cells) may cross from embryonic to maternal blood and stay there for relatively long time (several years) -chimera

Placental circulation Umbilical arteries
-deoxygenated blood from embryonic body
Chorionic arteries branching in chorionic plate
Capillary network in chorionic villi

Placental membrana Interface between maternal and fetal
blood• Syncytiotrophoblast
• Cytotrophoblast• Connective tissue
• Endothelium of fetal capillary
After week 12 cytotrophoblast gradually disappears, vessels come near to surface and get in contact with syncytiotrophoblast

3rd trimester Nuclei of
syncytiotrophoblast form aggregations – syncytial knots that may set free
Formation of fibrinoid – it reduces placental transfer

Syncytiotrophoblast – microvilli, SER, RER, GC, mito – active synthesis
Cytotrophoblast – undifferentiated cells – mitoses
Basal membrane Continuous
endothelium

Feto-maternal junction Different genotype – necessity to supress
imunity: Maternal and fetal tissue are separted by the
cells that do not have typical superficial antigens. Hormonal changes (progesteron, glucocorticods)
– Blood - Syncytiotrophoblast
– Connective tissue – Cytotrophoblastic shell Stem - anchoring villi attach chorion to the
decidua basalis – inside cytotrophoblastic plug

Placenta Placental shape – discoid (olliformis) +
haemochorial Placental septa – rests of decidua basalis.
They separate placenta from maternal side in lobes - cotyledons
Cotyledons – contain 2 and more anchoring villi
Diameter – 15 -20 cm, thickness 2-3 cm, weight 500 to 600 g


Placental transfer Difusion Facilitated difusion Active transport Pinocytosis Other types of transfer:
Damage of placetal barrier – blood cellas Own activity – Treponema pallidum Damage due to infection - toxoplasmosa

Transfer Many substances from maternal blood
may transfer placental barrier including drugs
Nutrients – glucose, AK, fatty acids, water, vitamines, electrolytes
Hormones – only steroid unconjugates Maternal antibodies, transferin+ iron

Syntesis hCG – human chorionic gonadotropin hCS – human chorionic somato-
mammotropin/placental lactogen hCT human chorionic thyrotropin hCACTH human chorionic corticotropin Progesteron and estrogens

Placental abnormalities Atypical implatation: Placenta previa Placenta accreta Placenta percreta Placenta membranacea Placenta accessoria Atypical attachment of umbilical cord--
marginal, velamentous

Development of mbilical cord Connective stalk with umbilical arteries
and veins and allantois Ductus omphaloentericus connecting gut
with yolk sac Extraembryonic coelom Umbilicus

Developmentof umbilical cord• Length 50 cm