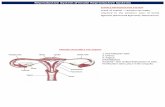
Female Reproductive System I
-
Upload
namibian-students-in-moscow -
Category
Health & Medicine
-
view
301 -
download
4
Transcript of Female Reproductive System I
Ovary (female sex gland, female gonad)
Functions- female gamete production – ovogenesis
- female sex hormone secretion
⇓ estrogens
progesterone
Ovary is almond-shaped organ
is enclosed by the tunica albuginea is covered with the germinal epithelium
⇓
Ovary is subdivided into the cortex and medulla
Cortex
⇓- developing ovarian follicles
- atretic follicles and atretic bodies
- corpus luteum and corpus albicans
Medulla
⇓- loose connective tissue
- blood vessels and lymphatics
- nerves
Ovogenesis is a process of the ovum development
Includes 3 stages- stage of proliferation
- stage of growth
- stage of maturation
Ovogenesis stage of proliferation
is represented by oogonia (2n, 2c) proliferating by mitotic divisions
⇑oogonia in the embryonic ovary
Oogonium proliferation occurs only in the fetal period
oogonia are converted to the primary oocytes before birth
⇔
Ovogenesis stage of growth
is represented by primary oocytes (2n, 4c) is subdivided into
- small growth
- large growth
Small growth begins in the embryogenesis
primary oocytes enter the prophase
of the first meiotic division prophase does not complete until puberty oocytes remain in suspended prophase
called the dictyotene for several years
Large growth begins at puberty
lasts for two weeks until before ovulation
oocytes considerably enlarge in size
⇓
from 30µm to 150 µm
oocytes synthesize and accumulate
⇓ - organelles
- cortical granules
- yolk granules
⇒
0vogenesis stage of maturation includes meiosis
primary oocyte (2n, 4c)⇓
1st meiotic division
⇓
secondary oocyte (n, 2c)⇓
2nd meiotic division
⇓ ootida (n, c)
First meiotic division completes before ovulation
second meiotic division
⇓
- begins at ovulation
- is arrested at metaphase
- is completed in fertilization
Female meiotic division is unequal
only one cell receives almost all the cytoplasm polar bodies receive minimal cytoplasm and are nonfunctional cells
Ovarian follicle
is the oocyte surrounded by envelopes provides the microenvironment for developing oocyte
Folliculogenesis
Includes stages
⇓- primordial follicle
- primary follicle
- secondary follicle
- tertiary follicle
Primordial follicle
Consists of
- primary oocyte in the small growth
- a single layer of flat follicular cells
Primordial follicle primary oocyte
is arrested in the meiotic dictyotene
measures about 30 µm in diameter
Primordial follicles predominate in the ovary
are located in the cortex periphery just beneath the tunica albuginea
⇒
Primary follicle
Consists of
- primary oocyte
- zona pellucida
- a single layer of cuboidal follicular cells
Zona pellucida
is homogeneous acidophilic gel-like layer consists of glycosaminoglycans and glycoproteins is secreted by oocyte and follicular cells
⇔
Secondary (growing) follicle
Consists of
- primary oocyte in the large growth
- zona pellucida
- several layers of follicular cells
- connective tissue theca folliculi
⇔
Membrana granulosa or stratum granulosum
is stratified follicular epithelium follicular cells are identified as the granulosa cells
Stratum granulosum results from cell proliferation
estrogens stimulate granulosa cell proliferation ⇒
Follicular fluid or liquor folliculi
appears when the stratum granulosum reaches
a thickness of 6 to 12-cell layers is secreted by the granulosa cells
FSH stimulates fluid secretion
Granulosa cell endocrine function
Granulosa cells
- convert androgens to estrogens under
FSH stimulation
- release estrogens to fluid and blood
Theca folliculi
Is subdivided into
- theca interna – loose connective tissue
- theca externa – more dense connective tissue
Theca interna
Contains
- rich network of small vessels
- theca cells
⇔
⇑theca cells arise from mesenchyme
Theca cells are typically steroid-producing cells
Are rich in
- sER
- Golgi apparatus
- vesicular mitochondria
- lipid droplets
⇒
LH stimulates cell activity
Theca cells produce androgens under LH stimulation
Androgens
are transported to the stratum granulosum Granulosa cells
- convert androgens into estrogens
- release estrogens into the fluid and blood
⇑
⇑
Growing follicles are estrogen-producing structures
Estrogen blood level ⇒- increases as the follicles grow
- attains the maximal size before ovulation
Hormonal regulation of ovarian follicle endocrine function
LH stimulates the theca cells
- to produce androgens FSH stimulates the granulosa cells
- to convert androgens to estrogens
- to release estrogens into the blood
Estrogens through feed-back loop
- inhibit FSH release
- activate LH production
Tertiary follicle (mature follicle or Graafian vesicle)
represents the final stage of folliculogenesis is preovulatory follicle measures 10 mm and more in diameter extends through the full cortex thickness bulges on the ovarian surface
Tertiary follicle oocyte
reaches its final size – about 150 µm in diameter resumes the first meiotic division becomes secondary oocyte
Tertiary follicle oocyte is acentrically positioned
on the cumulus oophorus
is surrounded by envelopes
- zona pellucida
- corona radiata
cumulus oophorus ⇑
Tertiary follicle envelopes
Stratum granulosum
- becomes thin
- forms the cumulus oophorus Antrum
- increases in size Theca folliculi
- is more prominent
Ovulation
is the release of the secondary oocyte
with zona pellucida and corona radiata
from the Graafian follicle ⇒
occurs on the 14th day of the large growth
Ovulating oocyte
begins the second meiotic division progresses only to the metaphase division is arrested at the metaphase II
secondary oocyte at the metaphase II
leaves the ovary in ovulation ⇒
Stigma formation Stigma ruptures, forming a small gap in
- germinal epithelium
- ovarian capsule
- wall of the Graafian follicle
⇓secondary oocyte with envelopes leaves the ovary
Ovulation mechanisms
follicular fluid increases in volume and pressure proteolytic enzymes
- lyse the stigma and follicular wall
- separate the oocyte-cumulus complex theca externa myofibroblasts contract
the oocyte leaves the ovary ⇒
Ovulation is hormonal-mediated process
is induced by the gonadotropin maximal
blood concentration ⇒⇓
LH peak (surge) – 12 hours before ovulation
FSH peak (surge) – 36 hours before ovulation
Ovulated oocyte enters the oviduct
Oviduct infundibulum fimbriae cover the ovarian surface direct the oocyte into the oviduct prevent it to enter the peritoneal cavity
Bleeding from the capillaries into the follicular lumen
leads to the corpus hemorrhagicum formation with a central clot connective tissue invades the former follicular cavity
⇔
Corpus luteum formation – luteinization
Stages of vascularization and proliferation glandular metamorphosis secretion involution
Stage of vascularization and proliferation
granulosa basement membrane is destroyed capillaries enter the stratum granulosum and form a rich vascular network granulosa cells and theca cells proliferate
Stage of glandular metamorphosis
granulosa cells and theca-cells differentiate and become the lutein cells increase in size and accumulate
- sER- mitochondria with vesicular cristae- Golgi apparatus- lipid droplets- pigment lipochrome
lipochrome imparts to lutein cells a yellow appearance in fresh preparation
Granulosa lutein cells
are derived from the granulosa cells are pale and large – 30 µm in diameter are centrally located
⇔
Theca lutein cells
are derived from the theca-cells are darker and smaller – 15 µm in diameter are peripherally located
⇔
Stage of secretion
Corpus luteum secretes progesterone
⇓- prepares female organs (the endometrium, mammary glands) for pregnancy
- inhibits ovarian follicle development
secretion is regulated by LTH (prolactin)
Corpus luteum types
Corpus luteum of pregnancy develops if fertilization and implantation occur attains a size of 2 to 3 cm exists about 6 months
Corpus luteum of menstruation develops if fertilization do not occur is small in size exists about 12 days
Stage of involution occurs after pregnancy or menstruation
lutein cells die by apoptosis cell remnants are phagocytosed by macrophages connective tissue corpus albicans is formed
⇔
Atresia is a process of ovarian follicle degeneration
primordial and primary follicles degenerate and disappear,
leaving no trace of their existence
Stratum granulosum changes appear in the first place
granulosa is infiltrated by neutrophils and macrophages granulosa cells are sloughed into the antrum connective tissue and blood vessels invade
the granulosa and antrum
Oocyte degeneration occurs for the second time
oocyte undergoes apoptosis zona pellucida becomes folded and is broken down their remnants are phagocytozed by macrophages
Theca-cells proliferate and differentiate
become the atretic body cells produce steroid hormones, mainly estrogens
⇔
⇑atretic body contains rich capillary network
Glassy membrane is a characteristic feature of the atretic bodies
is the former granulosa basal membrane separates from follicular cells increases in thickness and becomes folded
the glassy membrane in an atretic follicle ⇒