Female Reproductive Physiology* - Fertility Society · Female Reproductive Physiology* Fetus at 7.5...
Transcript of Female Reproductive Physiology* - Fertility Society · Female Reproductive Physiology* Fetus at 7.5...

Dr Anne Clark, MPS, MBChB, FRCOG, FRANZCOG, CREI
Medical Director, Fertility First
Sydney, Australia
Female Reproductive Physiology*
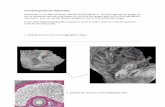
Fetus at 7.5 weeks – germ cells already developing in fetal ovaries
*The science that deals with the
functioning of living organisms
or their parts’

1 in 6 couples have
a fertility problem
Infertility is a W.H.O.
medical condition,
it is not a choice!!

Normal Time to Conceive
Couples are usually advised to seek advice after 12 months of unprotected intercourse.
But sooner if known fertility issues exist, such as anovulation, sperm problems or age >35 years for either partner.
100%
80%
60%
40%
20%
0%
40%
20%
14%
11%
0 - 3 3 - 6 6 - 9 9 - 12
Cumulative
Pregnancy Rate (%)
Months or cycles of
treatment

Fertility Parameters: Even a mild reduction in fertility parameters,
particularly in combination, can reduce the
chance of pregnancy each month
Number of
mild factors
0
1
2
3
Typical
monthly chance
20%
5%
1%
0.2%
Estimated time
to a pregnancy
4 months
2 years
7 years
40 years

3. Ovulated oocyte
to be fertilized in
the fallopian tube
2. Sufficient normal sperm to
swim through cervical mucous into
the fallopian tube
4. Receptive Uterine lining -
endometrium
1. As oocyte
matures the
follicle grows

A lot goes on inside an ovarian follicle to make that happen ……
Fertility & Sterility Cover; July 2009, Vol. 92, No.1.
•to produce a mature
egg that can result in a
pregnancy
•to assist the sperm to
reach the egg
•to prepare and support
the lining of the uterus
to allow an embryo to
hatch out and implant
•continue to support the
pregnancy until it is
independent at 8 to 9
weeks gestation

A lot goes on inside an ovarian follicle to make that happen ……
Fertility & Sterility Cover; July 2009, Vol. 92, No.1.
Achieves this by
.Process of oogenesis to
produce female gametes
•Secretion of hormones
from the cells lining the
follicular walls

Maternal Age and Oocyte Numbers A woman has the most eggs she’ll ever have when her mother is
6 months pregnant

Folliculogenesis and Oocyte Development
At birth a woman’s oocytes
are halted at first meiosis
division with a diploid (46)
number of chromosomes for
up to 50 years – primary
oocyte

Folliculogenesis and Oocyte Development The development of a primordial follicle containing an oocyte to a
preovulatory follicle takes in excess of 120 days.
After puberty, if an oocyte
develops in a menstrual
cycle completion of first
meiosis I results in a
secondary oocyte (GV or MI)
with a haploid (23) number
of chromosomes and the
first polar body.

Follicle Stimulating
Hormone (FSH) and
Lutienising Hormone
(LH) production in an
orderly fashion in
the brain is key to
the development of
a mature oocyte and
endometrium that
can result in a
pregnancy.

Connection between the Brain and the
Female Reproductive System
A feedback system of hormones secreted by the ovary,
hypothalamus and pituitary

FSH and LH only act in the final weeks of the development of a mature oocyte Initiation of follicular growth is continuous and occurs independently of gonadotrophic stimulation. It cannot be slowed or increased by medical means in normal circumstances. But in IVF want all the recruited oocytes to have a chance to mature.
McGee and Hsueh (2000)

Oocyte Development
Meiosis II is completed at
fertilisation and a second
polar body created
- Metaphase II oocyte –
The LH surge is critical
for this phase - HCG or
equivalent used in ART cycles

Thecal Cells – make androgens
Antral Follicle
Granulosa Cells – convert the
androgens to oestrogen
Cumulus Cells
Egg - Oocyte

Science • Granulosa cells are the only
cells in the female body known
to possess FSH receptors
• Antral formation requires stimulation by FSH starting when follicles reach about 0.25mm in diameter
• The pre-ovulatory surge of
gonadotropins (FSH and LH) is
essential to induce the
resumption of chromosomal
meiosis and final maturation of
the egg
antrim

• LH receptors are present in
theca cells and granulosa
cells in the ovary.
• In response to LH, thecal
tissues are stimulated to
produce androgens that
are then converted,
through FSH-induced
aromatisation to
oestrogens in the granulosa
cells.
• Therefore, ovarian
steroidogenesis is LH-
dependent to a significant
degree i.e. granulosa cells
are dependent on
androgens from the theca
to make oestrogen.
antrim
Science

‘Two cell, two gonadotrophin’ theory
Only FSH is required
for follicular growth
but some LH is
essential to achieve
adequate follicular
steroidogenesis and
develop the capacity
of the follicle to
ovulate and luteinise
when exposed to hCG
• Inhibin B secreted by
granulosa cells in response to
FSH, directly suppresses
pituitary secretion.
• Activin originating in both
pituitary and granulosa,
augments FSH secretion and
action.

The ‘LH window’ concept
That there is a threshold and a
ceiling for ideal LH levels to
maximise normal oocyte development
during the follicular phase.
The threshold has to change once the
oocyte is mature to ensure normal
oocyte maturation and ovulation.

LH Surge >20IU/l required for Ovulation
OVU
LATIO
N
LH E2
14-24 hours
10-12 hours
• The LH surge initiates the continuation of meiosis in the oocyte, luteinisation of the granulosa and synthesis of progesterone and prostaglandins within the follicle
• Progesterone enhances the activity of proteolytic enzymes responsible, together with prostaglandins, for digestion and rupture of the follicular wall.
• The progesterone-influenced midcycle rise in FSH frees the oocyte from follicular attachments and ensures sufficient LH receptors are present to allow an adequate luteal phase.
• If progesterone appears too early then premature luteinisation occurs, adversely affecting oocyte and pregnancy potential

In an IVF cycle need to first prevent ovulation before the eggs are collected with down regulation but ensure they have completed their maturation with a trigger injection
Progesterone (ng/ml)
Estrogen
Progesterone
LH
FSH
100 100
0 0
0 14 28
Ovulation
Follicular Phase Luteal Phase
FSH (mlU/ml) LH (mlU/ml)
500 20
0 0
Estrogen (ng/ml)

Endocrine Testing
Egg growth – oestrogen
Timing Ovulation – LH
Luteal phase and/or
ovulation - progesterone

Assessing a Woman’s Fertility
Potential: The Holy Grail Ultrasound assessment of antral follicle
count – normal number is 6 to 12
Ultrasound can only detect the number of oocytes
that have developed an antral follicle. It cannot
detect the total number of eggs available.

Assessing a Woman’s Fertility Potential:
Anti Mullerian Hormone (AMH)
Text goes here ….. As anti-mullerian hormone is
secreted by granulosa cells
in theory, the more eggs,
the more follicles so the
more AMH
Antral
Follicle

The primary physiological function of AMH in the ovary is inhibition
follicle recruitment into the antral follicle pool, so a woman’s egg
number lasts until her normal time of menopause.
AMH also reduces the sensitivity of growing follicles to FSH.
Assessing a Woman’s Fertility Potential:
Anti Mullerian Hormone (AMH)

From 2005, measurement of serum levels of anti-Müllerian hormone
emerged as a potential way of assessing ‘ovarian reserve’.
The higher the AMH, the more eggs a woman was believed to have in
reserve and therefore the better her fertility potential and also her
response to fertility treatments.
Anti-Müllerian Hormone (AMH)
Testing in Women

The levels are not reproducible. There is up to a 48%
significant variability of AMH results when the same woman
was tested.
Being on the oral contraceptive pill lowers AMH levels.
So sample variability in AMH results should be taken into
account when advising patients on their future fertility.
Most importantly, the test does not reflect egg quality or the
ability to conceive!
AMH could stand for “Anxiety Making Hormone”
Rustamov et al, Eshre, July 2012 108 women who had 2 or more AMH measurements within a median time gap of 3 months
However there are problems in relying on
AMH testing alone to advise a woman on
her reproductive potential.

AMH is Not a Useful Predictor of
Live Birth?
Extremely low levels of AMH do not mean a
woman cannot get pregnant naturally or on
treatment and therefore deserves the same
workup as any other fertility patient.

Effect of Maternal Age on Live Birth Rates
after IVF Using a Woman’s Own Oocytes
40
Live Births (percentage)
35
30
25
20
15
10
5
0
23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46
Woman’s Age (years)
There are significant factors besides the woman’s age and
ovarian reserve that contribute to reducing fertility potential,
that can be corrected.

Vitamin D
100
90
80
70
60
50
40
30
20
10
0
Percent
conceived
0 1 2 3 4 5 6
Sufficiency
At risk of inadequacy
or deficiency
Adjusted for age, race, BMI category, alcohol consumption, smoking
status and physical activity score. At risk of inadequacy or deficiency
is defined as serum 25(OH)D <50nmol/L; sufficiency is defined as
serum 25(OH)D >50nmol/L. Fung. Vitamin D and Fertility. Fertil Steril 2017.
Months from baseline
Women’s time to conception for
pregnancy by serum 25(OH)D status

Vitamin D Deficiency and Latitude:
Vitamin D deficiency
during pregnancy is
associated with an
increased risk of
multiple sclerosis,
asthma, schizophrenia
and autoimmune
diseases when the
child reaches
adulthood
Lucas et al., 2008 26x higher risk of developing multiple sclerosis if born in
Tasmania, 10x higher risk if born in Victoria cf if born in
Queensland

Serum and follicular fluid levels of Vitamin D
are highly correlated.
Vitamin D is from sunlight, fish, dairy and
sun exposed mushrooms.
As well as reducing fertility for men and
women, Vitamin D deficiency increases the
risk of miscarriage and pregnancy
complications, including stillbirth.
Ozkan et al Vit D and Reproductive Success Fert Steril 2010
Lowest Highest
Clinical Pregnancy (%)
IVF Pregnancy Rates and Vitamin D Levels
Lifestyle Factors Known to Improve Pregnancy Rates – Adequate Vitamin D levels

Nutrition: Mushrooms and Vitamin D
Similar to humans, mushrooms produce
Vitamin D naturally following exposure to
sunlight or a sunlamp.
All mushrooms contain vitamin D, but
growers have the ability to
increase levels by exposing mushrooms to
ultraviolet light.
Three to four Vitamin D mushrooms are
sufficient to supply daily needs.
http://www.fungi.com/blog/items/place-mushrooms-in-
sunlight-to-get-your-vitamin-d.html

Iodine: Adjusted Probability for Not Becoming Pregnant
0
0.25
0.55
0.75
1.0
0 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15
Time to Pregnancy in Menstrual Cycles
Percent Remaining Non-Pregnant
Iodine to Creatinine Ratio <50mg/g
50 mg/g <= Iodine to Creatinine Ratio < 100 mg/g
Iodine to Creatinine Ratio >= 100mg/g
Women who are iodine deficient are 46% less likely to get pregnant over each menstrual cycle compared to women who have sufficient iodine
Mills et al, Hum Reproduction, March 2018

Maternal Age:
Fertility and Miscarriage Rates
Miscarriage
Fertility
20-24 25-29 30-34 35-39 40-44 >45
500
450
400
350
300
250
200
150
100
50
0
100
90
80
70
60
50
40
30
20
10
0
Fertility Rate (per 100 women)
Miscarriage Rate (percentage)
Maternal Age (Years)
As a woman’s age
increases her fertility
decreases and her risk
of miscarriage
increases.

Fertility is a couple
issue, NOT a
woman’s issue.
They both have a
biological clock
A woman is only half the baby… ‘It takes two to tango’

An egg and sperm contribute an equal amount of genetic material to a pregnancy. The placenta is largely dependent on the expression of genes from the paternal chromosomes.
Miozzo and Simoni, 2002, Biol. Neonate; 81:217-228

Normal: >15 million per ml; >40% motile – 32% progressive;
>4% normal forms
Not all sperm are created equal!

0
20
15
10
5
25
Time to Pregnancy (months)
Time to Conception for a 25 year old Woman vs. Male Partner’s Age
<25 >40 35-40 30-35 25-30
Male Partner’s Age (Years) Hassan et al, F&S 2003, 2006
2x longer
4x longer

Dunson et al, Hum Reprod 2002:
Impact of a Man’s Age on the Chance of
Natural Conception plus Importance of
Timing Intercourse
Pregnancy
Probability
Halved
Likelihood of conception following IVF is halved for women 38 to 40
years if their partner is aged 40 years or older.
Rochebrochard et al, Fertil Steril; 85:5 May 2006, 2017

How to maximise fertility potential? Choose a younger partner
Check for and treat if
required increased sperm
DNA damage if the man is
over 35 years of age
Collette Dinnigan, pregnant naturally aged 46, and her husband, Bradley Cocks, aged 36

Paternal Age
20-29 yrs
30-34 yrs
35-39 yrs
40-64 yrs
Maternal Age
20-29 yrs 30-34 yrs 35-44 yrs
Standard Risk Zone
Standard Risk Zone
Standard Risk Zone
Standard
Risk Zone
High
Risk Zone
High
Risk Zone
High
Risk Zone
High
Risk Zone
Highest
Risk Zone
SRZ
HRZ
HjRZ
1.00 (Reference)
2.87 (1.86-4.45)
5.65 (3.20-9.98)
A man’s age, as well as a woman’s,
impacts on the risk of a miscarriage
de la Rochebrochard and Thonneau, 2002

Incidence of Downs’ Syndrome Related
to Paternal Age as well as Maternal Age
Maternal age uncorrected
for paternal age
Maternal age corrected
for paternal age
<24 25-29 30-34 35-39 40>
Maternal Age (years)
700
600
500
400
300
200
100
0
Rate per
100,000 births
Harry Fisch, Grace Hyun et al, Journal of Urology; Vol.169, 2275-2278, 2003

So what else can women do to maximise antral follicle count and fertility potential?
Know their family’s reproductive
history e.g. endometriosis, earlier
menopause and seek early
intervention if concerned
Don’t smoke
Use the pill for contraception
Minimise ovarian surgery that
reduces ovarian reserve

Maximising Fertility – Stop Smoking!
Women who smoke will have their
menopause 1 to 3 years earlier.
Up to 13% of infertility is attributable
to cigarette smoking, more than tubal
disease
Cigarette smoking increases the risk of
an ectopic pregnancy by 3-4x, more
than chlamydia
Miscarriage is 3-4x more likely.
Women who smoke ~ 20 cigarettes a day
expose their bodies to the radiation
equivalent of one chest X-ray a day!!
ASRM Practice Committee, Smoking and Infertility, Fertil Steril;
Nov 2006

Protects against ovarian cysts, endometriosis, PID
and premature ovarian failure
Prevention of Diminished Ovarian Reserve
Take the oral contraceptive pill

Maximising Fertility Potential – Marry!
Percentage without children
Age Range (average of first child is 30 Years*)
*Australian Bureau of Statistics 2011
A woman who is partnered but not married is 2 to 3 times
less likely to have children.
0
10
20
30
40
50
60
70
80
20-24 25-29 30-34 35-39 40-44
Married Defacto Partner
Average
age 1st child
women
Average
age 1st child
men

• Understanding the menstrual cycle is key to understanding how to assess and treat a woman’s fertility issues.
• Fertility is a couple issue, NOT just a woman’s issue
• Just as care needs to be taken to not give women unrealistic fertility expectations, it is just as important to assess each woman individually and not be unnecessarily negative.
• A woman should never be advised
she is unable to have a child or
treatment on the basis of an AMH
level alone.
To Conclude:
Fertilised egg in fallopian tube

Questions and Feedback
?
? ?
?
? ?
? ? ? ?
?
?
?
? ?
?
?
? ? ?
?
?
? ?
?
?
? ?
?