Escott Stump - Fetal Origins of Adult Chronic...
Transcript of Escott Stump - Fetal Origins of Adult Chronic...

9/13/2018
1
Fetal Origins of Adult Chronic DiseaseSylvia Escott‐Stump, MA, RDN, LDN, FAND
Objectives
• Participants will be able to
– Identify 3 chronic disorders that are affected by maternal nutrition/malnutrition
– Describe 2 measures for consideration by dietitians working in maternal‐child health
– Identify additional areas of research that are needed
Epigenetics
• Epigenetics explains how a stable genome is influenced to be expressed
– Genes are upregulated or downregulated without changes to genetic sequence
• Changes to the phenotype results!
• Changes reset fetal homeostatic set points by changes in metabolism, hormone production, hormone sensitivity, or organ development.
• Remain with the genome through the child’s life
• Millar and Dean, 2012

9/13/2018
2
JOURNAL OF THEAMERICAN DIETETICASSOCIATION
Genetic Variation
Nutrigen
etics
Nutrigen
omics
Food/NutrientNutrient AbsorptionNutrient UtilizationFood/Nutrient ToleranceNutrient Requirement
Genome Evolution/SelectionGenome Mutation RateIn‐utero Genome ViabilityGenome Programming Gene Expression
Nutrient‐genome interactions.
Managing Genome‐Diet Interactions (Stover and Caudil, 2008)
Risk Phenotype
ObesityHypertensionInsulin Resistance
Early Nutrition Experiences
MalnutritionSub‐optimal‐nutrientEnvironments
Adult Onset Disease
Cardiovascular DiseaseDiabetesMetabolic Syndrome
“Program”“Imprint”
Genetic and Epigenetic Contributions to Health
(Stover and Caudil 2008)
Single Nucleotide Polymorphisms (SNPs) and Diet
• One of the underlying mechanisms for metabolic individuality is genetic variation.
– SNPs in genes of metabolic pathways can create metabolic inefficiencies that alter the dietary requirement for, and responses to, nutrients.
– For example: in adults, SNPs determine whether people develop fatty liver, liver damage and muscle damage when eating diets low in choline (Zeisel et al, 2012.)

9/13/2018
3
One‐CarbonMetabolism
ATP/ADPNADP+/NADPHFolateVitamin B6
Vitamin B12
RiboflavinZincIronAmino AcidsCarbohydrates
DNA Synthesis‐ Deoxyribonucleotides
Chromatin Structure‐ DNA Methylation‐Histone Methylation
Nutrition/Metabolism Genome
Folate‐mediated one‐carbon metabolism is a conduit between the cellular628 nutrient environment and genome synthesis and methylation.
Genetic and Epigenetic Contributions to Health:
Managing Genome‐Diet Interactions (Stover and Caudil, 2008)
ATP = Adenosine Triphosphate
ADP = Adenosine Diphosphate
NADP+ = Nicotinamide adenine dinucleotide phosphate
NADPH = Reduced form of NADP+
DNA =Deoxyribonucleic acid
DNA Methylation Changes
• While in utero, environmental factors influence the DNA methylation profile at birth
• Exposure to smoking leads to DNA methylation change in the aryl hydrocarbon receptor repressor (AHRR) gene in blood; hypomethylation of AHRR occurs
• Novakovic et al, 2014
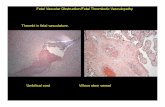
Placental Dysfunction
• Placental dysfunction underlies common and serious pregnancy complications such as fetal growth‐restriction (FGR), pre‐eclampsia, pre‐term birth and pregnancy loss.
– The origins of placental dysfunction arise after the first trimester
• Leeuwerke M et al, 2016

9/13/2018
4
Placenta as Regulator
• The placenta: important regulator of the intrauterine environment that links maternal and fetal nervous systems.
– Placental epigenetic signatures have been associated with neurodevelopment of newborns
• Quantified through the NICU Network Neurobehavioral Scales (NNNS).
– Associations have been observed for DNA methylation of genes involved in cortisol (NR3C1, HSD11B), serotonin (HTR2A), and metabolic (LEP) pathways.
• Brain epigenetic marks have been involved in idiopathic neurodevelopmental disorders, including Autism Spectrum Disorders (ASD)
• Lesseur et al, 2014
Fetal origins of adult disease (FOAD) from LBW
Dr. David Barker
(1938‐2013)
Malnutrition in Fetal Period
• Fetal malnutrition induces a nature of thrift in fetuses• Higher chance of developing non‐communicable diseases, such as obesity and
diabetes, if they grow up in the current well‐fed society.
• Similarly, mental stress during the neonatal period can alter the epigenetic expression status of neuronal genes in neonates. Moreover, such environmental, stress‐induced, epigenetic changes are transmitted to the next generation via an acquired epigenetic status in sperm.
• The advantage of epigenetic modifications over changes in genetic sequences is their potential reversibility; thus, epigenetic alterations are potentially reversed with gene expression.
• Kubota et al, 2015

9/13/2018
5
Developmental Origins of Health and Disease (DOHaD)
• Fetal over‐nutrition and undernutrition: long‐lasting effects on neuroendocrine control systems, energy homeostasis, and metabolism
• Sensitive time windows during early development:
– Environmental cues can program persistent epigenetic modifications
• Dutch famine birth cohort
• Fetal overnutrition (exposure to maternal obesity or high blood sugars) ‐‐ 10‐20% of pregnancies.
• Epigenetic changes: predispose the offspring to develop metabolic disease and transmit the adverse environmental exposure to the next generation.
– El Hajj N et al., 2014
DOHaD
• Early exposures to threat or adverse conditions have lifelong consequences
• The maternal endocrine 'fight or flight' system is a source of programming information for the human fetus to detect threats and adjust their developmental trajectory for survival.
• Fetal exposures to intrauterine conditions including elevated stress hormones increase the risk for a spectrum of health outcomes depending on the timing of exposure, the timetable of organogenesis and the developmental milestones assessed.
• Fetal exposures to biological markers of adversity have significant and largely negative consequences for fetal, infant and child emotional and cognitive regulation and reduced volume in specific brain structures.
– Sandman and Davis, 2012
14
Inter‐Individual Variations
DOHaD hypothesis: supported by a large number of direct animal studies and a smaller number of compelling observational studies in humans
• Little direct evidence exists in humans
• Epigenetic variation should be apparent in a tissue relevant to the disease of interest prior to phenotypic onset in order to avoid confounding and the potential for reverse causation.
• The functional relevance of specific epigenetic change must be demonstrated.
“Only large longitudinal life‐course studies commencing prior to birth, with extensive environmental exposure data and biospecimens, can provide direct evidence in support of a role of epigenetic processes as drivers of the DOHaDin humans.” (Saffery, 2014)

9/13/2018
6
Paradigm
• Environmental stressors:
– a variety of environmental and occupational hazards
– deficiency and oversupply of nutrients and energy
• Grandjean et al, 2015
OBESITYMore than just Overnutrition
Global Obesity and Metabolic Disease
• The generally accepted cause of obesity is overconsumption of calorie‐dense food and diminished physical activity (the “calories in‐calories out” model).
– Emerging evidence: environmental factors can predispose exposed individuals to gain weight, irrespective of diet and exercise.
Environmental obesogenmodel:
• chemical exposure during critical stages in development can influence subsequent adipogenesis, lipid balance and obesity.
• some obesogens elicit transgenerational effects on a variety of health endpoints
Janesick et al, 2014

9/13/2018
7
Endocrine Disrupting Chemicals (EDCs)
• Obesogenic EDCs may inappropriately stimulate adipogenesis and fat storage, influence metabolism and energy balance, and increase susceptibility to obesity.
• Tributyltin, brominated diphenyl ether 47, and polycyclic aromatic hydrocarbons alter methylation of peroxisome proliferator‐activated receptor‐γ (PPARγ) ‐‐the master regulator of adipogenesis, or its target genes.
• Advances in epigenomics:
• potential epigenetic markers for obesity that can be detected at birth
• basis to determine the effects of developmental exposure to obesogenic EDCs in humans.
• important to monitor low‐level early‐life environmental exposures
Birnbaum and Miller, 2015
Stel and Legler, 2015
PPARy (Ahmadian et al, 2013)
Double Burden of DiseaseUndernutrition and Overnutrition

9/13/2018
8
Double Burden of Disease
Undernutrition • Stunting, wasting, infectious
diseases
Overweight and Obesity• Non‐Communicable Disease
(NCD): risk more with lifestyle changes and urbanization
Social and environmental factors such as parental migration, financial situation of the household, child‐rearing knowledge and practices of the primary caregivers
Prominent in Sub‐Saharan Africa, Asia (rural China, India)
Feng et al, 2015
Maternal and Child Malnutrition• Child malnutrition in low‐income and middle‐income countries
encompasses both undernutrition and a growing problem with overweight and obesity
– Prevalence of stunting of linear growth of children younger than 5 years has decreased during the past two decades
• Higher in south Asia and sub‐Saharan Africa
– Deficiencies of vitamin A and zinc result in deaths
– Deficiencies of iodine and iron, with stunting, can contribute to children not reaching their developmental potential.
– Undernutrition (including fetal growth restriction, stunting, wasting, and deficiencies of vitamin A and zinc, and suboptimum breastfeeding) causes 3.1 million child deaths annually…45% of all child deaths in 2011 (Black et al, 2013)
Maternal and Child Malnutrition
• Maternal undernutrition contributes to fetal growth restriction, which increases the risk of neonatal deaths and, for survivors, of stunting by 2 years of age.
• Suboptimum breastfeeding results in an increased risk for mortality in the first 2 years of life.

9/13/2018
9
Cardiovascular, Liver, Lung, Renal, Reproductive ChangesThe impact of perinatal insults
Perinatal Insults and Cardiovascular Disease
• The cardiovascular, renal and metabolic diseases during adult life that occur as a consequence of several insults during fetal and postnatal periods are secondary to multiple structural and functional changes (Tomat and Salazar, 2014)
• Maternal obesity is a risk factor for the development of cardiovascular diseases in the child later ‐‐ an exaggerated leptin surge (Samuelsson et al, 2014)
Perinatal Insults, Hypertension and Renal Changes
• Maternal undernutrition, maternal glucocorticoids, placental insufficiency, and maternal sodium overload can program changes in renal Na(+) excretion leading to hypertension
– Fetal exposure to an adverse maternal environment may reduce GFR by decreasing the surface area of the glomerular capillaries
• Paixao and Alexander, 2013

9/13/2018
10
Lactation and Insulin Resistance
• Both early weaning and overfeeding by more milk intake may lead to insulin resistance in later life.
– Maternal stress, obesity, hyperglycemia, and even smoking during lactation might also cause reduced insulin sensitivity in the offspring
– Breast milk may be the “agent,” transferring altered levels of hormones, insulin, or fatty acid contents from maternal circulation to neonate (Jiang et al, 2013.)
Perinatal Insults and Nonalcoholic Fatty Liver Disease (NAFLD)
• Most common liver disease globally
– Altered early life nutrition is now associated with an increased risk for the development of NAFLD
Li et al, 2015
Perinatal Insults and Lung Disease
• Perinatal insults:
– Intrauterine growth restriction, preterm birth, maternal exposure to toxins, or dietary deficiencies produce deviations in the epigenome of lung cells
– Final stages of lung development
– DNA methylation, histone modifications, and microRNA changes are all observed in various forms of lung disease
• Joss‐Moore et al, 2015

9/13/2018
11
Perinatal Insults on the Female Reproductive System
• Reproductive maturation and function
– primordial follicle pool is established early in life
– insults cause decline in ovarian follicular reserve, changes in ovulation rates, and altered age at onset of puberty
– protein malnutrition especially a concern
Chan et al, 2015
Diabetes (T2DM)T2DM – worldwide a problem – 2.8% ‐ 4.4%
India the country with the highest prevalence
Islet Cells
• Islets are the most plastic during the early life course; hence programming during fetal and lactational life is most potent.
– High fat exposure (through acute hyperglycemia) during weaning initiates beta cell programming and dysfunction
Cerf, 2015

9/13/2018
12
Type 2 Diabetes Mellitus (T2DM)
• Multifactorial disease: genetic, epigenetic, and environmental factors.
• Maternal factors during pregnancy may increase the risk of diabetes in offspring in later life:– malnutrition, hyperglycemia, obesity, behavior (smoking, drinking, and junk
food diet), hormone administration, and stress
• In neonates: – catch‐up growth, fatty acid exposure during lactation, glucocorticoids
administration, and stress have all been found to increase the risk of insulin resistance or T2DM
– unfavorable socioeconomic situation, famine or obesity also increase susceptibility to T2DM in adults.
Heindel et al 2015; Jiang X et al, 2013; Mennitti et al, 2015
High Fat Programming during PG/BFThe maternal nutritional condition and fatty acid intake during pregnancy and/or lactation are critical for programming:
The maternal body accumulates fat; in late pregnancy, the lipolytic activity in the maternal adipose tissue is increased
Fetal exposure to trans fatty acids appears to promote early deleterious effects in the offspring's health
Maternal intake of saturated fatty acids seems to trigger alterations in the liver and adipose tissue function associated with insulin resistance and diabetes
PUFAs (particularly arachidonic acid, EPA and DHA) play an important and beneficial physiologic role in the offspring who receive these fatty acids during critical periods of development.
Mennitti et al, 2015
Protein Insufficiency during Pregnancy
• The effect of low protein diet during pregnancy on postnatal β cells (Jiang et al, 2013.)
– increased oxidative stress, fibrosis
– defective mitochondriogenesis, mitochondria dysfunction
– increased cell differentiation instead of proliferation

9/13/2018
13
Neurological ConditionsThe brain is a high risk organ
Stress and the Fetal Brain
Stress During Pregnancy
• Psychobiological markers of stress during pregnancy, especially early in gestation, result in:
– delayed fetal maturation
– disrupted emotional regulation
– impaired cognitive performance during infancy
– decreased brain volume in areas associated with learning and memory in 6‐ to 8‐year‐old children
The Fetal Brain
• During gestation, the fetal brain develops dramatically as structures and connections form, providing the foundation for all future development. The fetal environment plays a critical role in these early neural processes, for better or for worse.
• Exposure to maternal stress can sometimes have deleterious effects on the fetus, depending on the cause, timing, duration, and intensity of stress.
Stress and the Brain (Buss et al 2012)
39

9/13/2018
14
Prenatal Inflammation
• Known risk factor for long term neurobehavioral disorders including cerebral palsy, schizophrenia, and autism
– Immune response and adverse neurobehavioral outcomes occur in the exposed fetus.
– The immune system in the placenta is activated, inducing a fetal immune response and subsequent brain injury.
– Changes in the fetal brain lead to changes in gene expression patterns into the neonatal period.
– Subclinical intrauterine inflammation can lead to fetal brain injury, mechanistically associated with long term adverse outcomes for exposed offspring.
Elovitz et al, 2011
Maternal Obesity and High‐Fat Diet
• Increased obesity and increased vulnerability to mood disorders
• Programming of brain and behavior by perinatal diet is propagated by inflammatory mechanisms‐‐ interleukin [IL]‐6 and 11‐1β
Bolton and Bilbo, 2014
Sasaki et al, 2013
CancerGenes + Environment

9/13/2018
15
Cancer
Tumor cell plasticity ‐ Intrinsic factors govern cell functioning
More, larger and longer studies are needed (Brock et al, 2015)
Non‐communicable diseases (NCDs) and maternal health are closely linked. NCDs such as diabetes, obesity and hypertension have a significant adverse impact on maternal health and pregnancy outcomes, and future generations.
The cycle of vulnerability to NCDs is repeated with increasing risk accumulation in subsequent generations. (Kapur, 2015)
Effects and ActionsInterventions
Effects of Nutritional Insults

9/13/2018
16
What is the Time to Intervene?
First 1000 Days Project
• Issues:
– Low birthweight – high risk for DM and hypertension later
– Breastfeeding –exclusive for at least 6 months
– Stunting – 20% begins in the womb if mom is malnourished
– Acute Malnutrition –wasting leads to stunted growth, cognitive deficits and NCDs in adulthood
– Anemia – diminished energy and health in women and their children
– Obesity – childhood obesity contributes to diabetes and hypertension
http//thousanddays.org/
First 1000 Days Principles• The nutritional health of women and children, particularly during the 1,000 day window
between pregnancy and age two, is a policy and funding priority.
• The world’s mothers and future mothers are valued, healthy and well‐nourished.
• More babies are exclusively breastfed from birth to six months and are continuing to breastfeed for at least one year.
• Women are empowered and supported to breastfeed and make choices about how to nourish their children in a way that is free from predatory marketing and commercial influence.
• Women and young children eat a healthy and diverse diet of nutritious foods. This requires a shift in food and agriculture policies, food systems and environments and social norms so that healthy foods are available, affordable and desired.
• Women and children have access to quality health care, clean water and sanitation, and social support systems.
• Life‐saving treatment for acute malnutrition reaches those who need it the most.
• There is greater collaboration to bring an end to malnutrition in all its forms.

9/13/2018
17
Public Health Measures
• Coexistence of stunting, overweight or obesity, and anemia at the national, household calls for policies and programs to prevent these conditions
• Educate the public, especially young women
• Evaluate nutrient requirements on a regular basis
Increasing Intake
UL
Ris
k o
f in
ad
equ
ac
y
Risk o
f excess
0.5 0.5
EAR
AI
RDA
Increasing Intake
UL
Ris
k o
f in
ad
equ
ac
y
Risk o
f excess
0.5 0.5
EAR
AI
RDA
Possible genomic criteria for setting the EAR and UL
- Uracil in DNA-Mutation rate-Protein profiles- Genome methylation- Gene expression profiles
Possible genomic criteria for establishing dietary requirements.
Genetic and Epigenetic
Contributions to Health (Stover and Caudil, 2008)
EAR = Estimated Average Requirement;
UL = Tolerable Upper Intake Levels
RDA = Recommended Dietary Allowances
DNA = Deoxyribonucleic Acid
Our Goals
Promote Maternal and Child Health Strategies• Promote health literacy in the public
Reduce Infant Malnutrition
• Provide high‐quality complementary foods
• Promote well‐balanced dietary patterns

9/13/2018
18
What Can We Do?
• Promote preconceptual care to modify a woman’s medical, behavioral and social risks through interventions
• Diagnose and treat NCDs to reduce their impact during pregnancy
– Give ample time to treat hypertension, diabetes, obesity, systemic lupus erythematosus, thyroid disease, anemia, epilepsy, asthma, and cardiac disease
– Manage these conditions carefully during pregnancy to prevent long‐term consequences for mother, child, and future generations
• Hadar et al, 2015
Future Research Considerations
• Sample size
• Potentially confounding factors
• Tissue heterogeneity
• Reverse causation
• The role of genetics in modulating epigenetic profiles
– Januar et al 2015
Let’s NOT Be Too Late….

9/13/2018
19
ReferencesAhmadian M et al. PPARγ signaling and metabolism: the good, the bad and the future. Nat Med. 19:557‐66, 2013.
Birnbaum LS, Miller MF. Prenatal Programming and Toxicity (PPTOX) Introduction. Endocrinology. 156:3405‐7, 2015.
Black et al. Maternal and child undernutrition and overweight in low‐income and middle‐income countries. Lancet. 382:427‐51, 2013.
Bolton JL, Bilbo SD. Developmental programming of brain and behavior by perinatal diet: focus on inflammatory mechanisms. Dialogues Clin Neurosci. 16:307‐20, 2014.
Brock A et al. Control of cancer formation by intrinsic genetic noise and microenvironmental cues. Nat Rev Cancer. 15:499‐509, 2015.
Buss C et al. The Role of Stress in Brain Development: The Gestational Environment's Long‐Term Effects on the Brain. Cerebrum. 2012:4, 2012.
Cerf ME. High fat programming of beta cell compensation, exhaustion, death and dysfunction. Pediatr Diabetes. 16:71‐8, 2015.
Chan KA et al. Early‐life nutritional effects on the female reproductive system. J Endocrinol. 224:45‐62, 2015.
El Hajj N et al. Epigenetics and life‐long consequences of an adverse nutritional and diabetic intrauterine environment. Reproduction. 148:111‐20, 2014.
Elovitz MA et al. Intrauterine inflammation, insufficient to induce parturition, still evokes fetal and neonatal brain injury. Int J Dev Neurosci. 29:663‐71, 2011.
Feng A et al. Developmental Origins of Health and Disease (DOHaD): Implications for health and nutritional issues among rural children in China. Biosci Trends. 9:82‐7, 2015.
ReferencesGrandjean P et al. Life‐Long Implications of Developmental Exposure to Environmental Stressors: New Perspectives. Endocrinology. 156:3408‐15, 2015.
Hadar E et al. The preconceptional period as an opportunity for prediction and prevention of noncommunicable disease. Best Pract Res Clin Obstet Gynaecol. 29:54‐62, 2015.
Hanson MA, Gluckman PD. Early developmental conditioning of later health and disease: physiology or pathophysiology? Physiol Rev. 94:1027‐76, 2014.
Heindel JJ et al. Developmental Origins of Health and Disease: Integrating Environmental Influences. Endocrinology.156:3416‐21, 2015.
Janesick AS et al. Transgenerational inheritance of prenatal obesogen exposure. Mol Cell Endocrinol. 398:31‐5, 2014.
Januar V et al. Epigenetic regulation of human placental function and pregnancy outcome: considerations for causal inference. Am J Obstet Gynecol. 213:182‐96S, 2015.
Jiang X et al. Early life factors and type 2 diabetes mellitus. J Diabetes Res. 2013:485082, 2013.
Joss‐Moore LA et al. Epigenetic contributions to the developmental origins of adult lung disease. Biochem Cell Biol. 93:119‐27, 2015 .
ReferencesKapur A. Links between maternal health and NCDs. Best Pract Res Clin Obstet Gynaecol. 29:32‐42, 2015.
Kubota T et al. Understanding the epigenetics of neurodevelopmental disorders and DOHaD. J Dev Orig Health Dis. 6:96‐104, 2015.
Lesseur C et al. Epigenetic Regulation of Infant Neurobehavioral Outcomes. Med Epigenet. 2:71‐79, 2014.
Leeuwerke M et al. DNA Methylation and Expression Patterns of Selected Genes in First‐Trimester Placental Tissue from Pregnancies with Small‐for‐Gestational‐Age Infants at Birth. Biol Reprod. 94:37, 2016.
Li M et al. Developmental Programming of Nonalcoholic Fatty Liver Disease: The Effect of Early Life Nutrition on Susceptibility and Disease Severity in Later Life. Biomed Res Int. 2015:437107, 2015.
Mennitti LV et al. Type of fatty acids in maternal diets during pregnancy and/or lactation and metabolic consequences of the offspring. J Nutr Biochem. 26:99‐111, 2015.
Millar K, Dean HJ. Developmental origins of type 2 diabetes in aboriginal youth in Canada: it is more than diet and exercise. J Nutr Metab. 2012:127452, 2012.
Novakovic B et al. Postnatal stability, tissue, and time specific effects of AHRR methylation change in response to maternal smoking in pregnancy. Epigenetics. 9:377‐86, 2014.

9/13/2018
20
ReferencesPaixaoAD, Alexander BT. How the kidney is impacted by the perinatal maternal environment to develop hypertension. BiolReprod. 89:144, 2013.
Saffery R. Epigenetic change as the major mediator of fetal programming in humans: Are we there yet? Ann Nutr Metab. 64:203‐7, 2014.
Samuelsson A et al. New perspectives on the origin of hypertension; the role of the hypothalamic melanocortin system. ExpPhysiol. 99:1110‐5, 2014.
Sandman CA, Davis EP. Neurobehavioral risk is associated with gestational exposure to stress hormones. Expert Rev Endocrinol Metab. 7:445‐459, 2012.
Sasaki A et al. Perinatal high fat diet alters glucocorticoid signaling and anxiety behavior in adulthood. Neuroscience. 240:1‐12, 2013.
Stel J, Legler J. The Role of Epigenetics in the Latent Effects of Early Life Exposure to Obesogenic Endocrine Disrupting Chemicals. Endocrinology. 156:3466‐72, 2015.
Stover PJ, Caudil MA. Genetic and epigenetic contributions to human nutrition and health: managing genome‐diet interactions. J Am Diet Assoc. 108:1480‐7, 2008.
Tomat AL, Salazar FJ. Mechanisms involved in developmental programming of hypertension and renal diseases. Gender differences. HormMol Biol Clin Investig. 18:63‐77, 2014.
Zeisel S. Diet‐gene interactions underlie metabolic individuality and influence brain development: implications for clinical practice derived from studies on choline metabolism. Ann NutrMetab. 60S:19‐25, 2012.