Endocrine emergencies in adolescents G. Chiumello, M.P.Guarneri
description
Transcript of Endocrine emergencies in adolescents G. Chiumello, M.P.Guarneri

Endocrine emergencies in adolescentsEndocrine emergencies in adolescents G. Chiumello, M.P.GuarneriG. Chiumello, M.P.Guarneri
Paediatric Department, Endocrine UnitVita –Salute San Raffaele University, Milan, ITALY


16561656 children (age 0-15 yrs) affected by diabetes type 1
• DKA 19 %, severe DKA 4%
• DKA 30 %, severe DKA 8 % less 2 yrs
Diabetes Care 2010

M.S. 14 yrs3rd year of junior high school poor school performanceslarge familydisadvantaged socio-economic conditions
•Diabetes (onset 6 years of age) poor glycometabolic control
respiratory distressprogressive worsening of general conditions
with state of consciousness alteration

EMERGENCY ROOM:
- pH 6,97 pCO2 17 HCO3 3,9 BEB -26,4- glycemia 714 mg/dL- Na+ 126mmol/L, K+ 5,7 mmol/L, creatinine 1,46 mg/dL
Intensive Care Unit
discontinuous insulin therapy during last 10-15
days and probably interruption of treatment in the last 24-48 hours

I PERIOD: volume expansion / shock treatment (1-2 hours):
10-20 ml/Kg saline solution 0,9%
II PERIOD: fluid replacement and maintenance (6 hours):
Saline solution 0,9% + 40 mEq/L K+ (50% KCl + 50% KPO4)
III PERIOD: fluid replacement and maintenance (16-24 hours):
Saline solution 0,45% + 40 mEq/L K+
TREATMENT

• Gradual glycemia reduction
AFTER THE FIRST PERIOD
• e.v insulin (0,1 U/Kg/h) until DKA resolution then switch to subcutaneous insulin therapy

A.M. 18 yrs diabetes 13 yrs duration HbA1c> 10% poor glycometabolic control
good social conditions optimal level of family care
During a relative’s acute illness, she voluntarily suspended the administration of insulin for 48 hours
EMERGENCY ROOM: loss of consciousness

Serious DKA with oligoanuria and hyperkalemia. Admitted to intensive care unit
Psychological support
Persistence of poor glycometabolic control and onset of eating disorders.
Found lifeless in bed dead in bed syndrome






J.P.B. 17 yrsdiabetes 13 yrs duration poor glycometabolic control with frequent asymptomatic
hypoglycemiaHbA1c> 9%
arrived in Italy 1 year ago from Moroccounsatisfactory familiar and personal compliance
After insulin injection, eveningwith friends, loss of consciousness with generalized convulsions glycemia 22 mg/dl
The following year, during another serious hypoglycemia, involved in a traffic accident.



HyperthyroidismHyperthyroidism
Incidence 1:100.000/yr
0.1:100.000/yr (early childhood)
3:100.000/yr (adolescence)
initial symptoms can be mild: nervousness and anxiety, irritability, emotional lability, fatigue, palpitations, tremors, insomnia, profuse sweating. Often drop in school performance
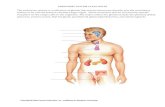
variable thyroid size, usually symmetrical increase with tense consistence
ophthalmic abnormalities less severe than in adults, with staring eyes, puffiness around the eyes, increased tear formation, irritation and unusual sensitivity to light. True exophthalmos is quite unusual



METHIMAZOLE / PROPYLTHIOURACIL (not available in Italy)
METHIMAZOLE PROPYLTHIOURACIL
Mechanism of action inhibition TPOinhibition TPO +
inhibition peripheral conversion T4/T3
Serum Half-lifeFreq. administration
4-6 hours every 12-24 hours
75 min. every 8 ore
Attack dose 0.5-1 mg/kgMax dose 30 mg/die
5-10 mg/kg
Time to normalization of thyroid function 4-6 weeks 4-6 weeks
SYMPTOMATIC THERAPY beta-blocker during the first 2 weeks of therapy children propranololadults atenolol

Thyrotoxic crisis

CausesCauses
surgery
status epilecticus
diabetes ketoacidosis
burns
sepsis
thyroxine overdose is not a cause of thyrotoxic crisis


METHIMAZOLO/PROPYLTHIOURACIL ev: block of thyroid hormones synthesis
LUGOL’S IODINE: oral or nasogastric administration inibition of FT4 / FT3 conversion
CORTISONICS: useful for their collateral inhibition of peripheral conversion of T4 to T3.
Dexamethasone: 8-10mg/die in 3 administrations Hydrocortisone: 100-300mg/die in 3 administrations
BETA-BLOCKERS: if signs of marked adrenergic activity (psychosis, extreme agitation, hyperexcitability) PROPRANOLOL:
0.1 mg/kg (up to 2mg) in 5-10 min ev 2 mg/kg/die every 4-6 hours (max 6mg/kg/die)



Acute adrenal insufficiency DEFECTS OF ADRENAL STEROIDOGENESIS
- congenital adrenal insufficiency- 21OHD- other enzyme defects
ADDISON D.
- autoimmune disease- genetic defects- adrenal hemorrhage- adrenoleukodystrophy
SECONDARY ADDISON D.
Panhypopituitarism

P.G. 17 yrs ICS
Holidays in Egypt with friends
Fails to inform friends about his underlying disease
Acute gastroenteritis with severe evolution and fever
Admitted after 36 hours of symptoms in intensive care unit

loss of consciousness,
severe hypotension
dyselectrolitemia
Parents, alerted by friends, informed local doctorsabout son’s disease (ICS)
Diagnosis:Acute adrenal insufficiency in ICS
Adequate therapy


Replacement therapy:
Glucocorticoid (hydrocortisone) Mineralcorticoid (deoxycorticosterone)
Absolute need of:
good therapeutic compliance therapeutic management

Causes: Infections Surgery Severe stress Accidents and injuries Strenuous physical activity Therapeutic non-compliance
Clinical features: Anorexia Nausea Vomiting Abdominal pain Hypotension Dyselectrolitemia Hypoglycemia Fever Lethargy Shock
Acute adrenal crisis

GLUCOSALINE SOLUTIONGLUCOSALINE SOLUTION Glucose solution 5% with NaCl (10-5mEq/kg/die)Glucose solution 5% with NaCl (10-5mEq/kg/die) 120-150 ml/kg/die, half in first three hours120-150 ml/kg/die, half in first three hours
GLUCOCORTICOIDGLUCOCORTICOIDFlebocortid endovenous 2-3 mg/kg (bolus)Flebocortid endovenous 2-3 mg/kg (bolus)then 5mg/kg in three hours then 5mg/kg in three hours then 10mg/kg/diethen 10mg/kg/die
MINERALCORTICOIDMINERALCORTICOIDDeoxycorticosterone acetate i.m. 3 mg/dieDeoxycorticosterone acetate i.m. 3 mg/die





• Prevalence in children: 0.005-0.007 per 100,000 (M:F = 9:10)
• 32,8 % of pancreatic tumors
• Unusual before 10 years (1.2%). Average age at diagnosis>40 years
• More aggressive in children
• Survival rate at 15 years: 50%
PANCREATIC NEUROENDOCRINE TUMORSIN PEDIATRIC AGE
J. Pediatric Surgery 2008

87% accidentally found
Sugical choice:distal pancreatectomy /
DCP

CLINICAL PRESENTATION
• Accidental ultrasound/radiologic diagnosis (lesions < 1 cm)
• Clinical syndromes related to endocrine mediators peptides production (sometimes accidentally discovered at blood tests)
Tumor Secreting Peptides Symptomatology
-Insulinoma (5-10%) Insulin, PP, VIP Hypoglycemia signs and symptoms -Glucagonoma (10%) Glucagone, PP Erythema
Calcitonin HyperglycemiaGloss/stomatitis
-Gastrinoma (25-40%) Gastrin, VIP, PP Zollinger Ellison Neurotensina Syndome
-VIPoma (5%) VIP Verner Morrison Syndrome
-Silent functional endocrine tumor (20%)
MAIN PANCREATIC NET AND ASSOCIATION TO MEN1

CLINICAL PRESENTATION
GLUCAGONOMA•necrolytic migrant erythema (70%)•hyperglycemia (83%)•glossitis and stomatitis (34%)•weight loss (66%)•thromboembolic disease (30%) •occasionally, but not always present, nausea and vomiting
ZOLLINGER ELLISON SYNDROME• Multiple peptic ulcers prone to perforation•Diarrhea•Identification of tumor•Weight loss
VERNER MORRISON SYNDROME•Pancreatic cholera: non continues diarrhea, even while fasting, with faecal volume over 700 ml/die• Electrolytic alterations(ipokaliemia, acloridia)• Dyspepsia (inhibition of acid and peptic secretion )
Specific symptoms not always present: catch down growth, weight loss. Possible accidental diagnosis.
Confounding clinical features for multiple hormons.

DIAGNOSTIC PROBLEMS
• multiple hormonal involvement
• MIXED TUMOR: neuroendocrine and neoplastic exocrine tumors
• possible changes in tumor secretion (spontaneous or treatment-induced)

A.O. 9 yrs
Catch down growth
GH: Clonidine 29.3 ng/ml, GRF + Arginine > 35 ng/ml IGF1 50-90° p.le
•TSH 6.6 mcu/ml; FT4 1.08 ng/dl. •Thyroid Ultrasound: image suggestive of chronic mild diffuse thyroiditis. •Bone age = statural age Hypothalamic-pituitary RM: normal
Persistence velocity rate ≈ - 2SDS
• TSH: 9.36…6.28; FT4: 1.45…1.12 • Eutirox 1,4 mcg/kg/die TSH normalization
• urinary cortisol 24h: 122...125…240 mcg/24h. (v.n. 25 – 75), ACTH: normal (34.4 pg/ml)
Hypercortisolism Hypothesis: dexamethasone suppression test at low doses: adequate inhibition of cortisol and ACTH
T

Hypercortisolism Hypothesis?
Suppression test at low doses (Dexamethasone 0,5 mg x 4/die for 2 days)
Cortisol 3 mcg/dl (v.n. < 1,4) Cushing syndrome admission to our Department
Absence of circadian rhythmCortisol 12 p.m. (242…162 ng/ml v.n. <44)Urinary and salivary cortisol:
Dexamethasone Test: appropriate cortisol and ACTH inhibition
FUNCTIONAL HYPERCORTICISM
Abdomen ultrasound: adenoma 5x4x4,5 cm (pancreatic tale)
TAC e RM: NEUROENDOCRINE TUMOR Markers: Glucagon +++ Glucagonoma
Laparotomic partial pancreatectomy