Endocarditis & Endovascular Infections Tricuspid valve Medic.med.uth.tmc.edu Vegetation Thomas Hawn,...
Transcript of Endocarditis & Endovascular Infections Tricuspid valve Medic.med.uth.tmc.edu Vegetation Thomas Hawn,...

Endocarditis & Endovascular Infections
Tricuspid valve
Medic.med.uth.tmc.edu
Vegetation
Thomas Hawn, July 2011

Case 1
45 yo female S/P MVAARDS in the ICU x 15 d with new onset fever.
PEIJ central line along with 2 peripheral ivs.
Question:
How do you diagnose a CVC infection?

Central Venous Catheter Infections
Diagnostic Recommendations
If CVC infection is suspected,
1. Draw 2 sets of bld cxs (one percutaneously)
2. Check paired quantitative or qualitative with time to positivity monitoring
3. If catheter is removed, send tip for culture.
Criteria for positivity:
>15 CFU by semi-quantitative method (roll-plate)
>100 CFU by quantitative method (sonication)

Central Venous Catheter Infections
Case:Blood culture grow Staphylococcus aureus in 2 out of 2 sets (4 bottles).
Catheter 100 CFU/ml + in 14hVein 15 CFU/ml + in 18h
Question:What is your management recommendation?Should the line be removed?Duration of Rx?Should a TTE or TEE be obtained?

Central Venous Catheter Infections
Sens SpecPaired quantitative 79 94 Siegman-Igra, meta-analysis (cath:vein ratio>3-10:1)
Unpaired quantitative 78 96 Siegman-Igra, meta-analysis (CFU/ml>15-100)
Differential time to positivity 89 100 Gaur et al, n=33 (time>120 minutes)
96 100 Blot et al (1998), n=64, (time > 120 minutes)
94 91 Blot et al (1999), n=28, (time > 120 minutes)
Criteria for positivity
Paired quantitative: catheter:vein cfu ratio >3
Unpaired quantitative: catheter cx >100 cfu/ml
Differential time: >120 minutes

Uncomplicated CVC Bacteremia
1) No septic emboli
2) Negative surveillance cultures 2-4 d after starting therapy
3) Removable focus of infection
4) Not immunocompromised
5) Rapid clinical resolutions of sxs within 72h of starting abx and removing focus of infection
6) No indwelling prosthetic devices or underlying heart disease

Should the line be removed in S. aureus bacteremia?
S. aureus bacteremia, n=244
Management recommended: remove focus of infection, check surveillance cultures, TEE, start therapy (decide duration based on whether endocarditis present)
Cure rate:
Recommendations followed: 79.5%
Recommendations not followed: 64.4%
Foreign body removed: 83.7%
Foreign body not removed: 43.5%
Fowler et al (1998) CID 27: 478-86

Case 250 yo F in ICU with fever
Bld Culture:Tunneled line: +Candida in 2/2 bottlesPeripheral: No growth
Questions1. Can you treat through the line?2. What anti-fungal treatment do you start?3. When do you change Rx after species known?4. When do you get MICs for fluconazole?

Candidemia in non-neutropenic host
1. Initial Rx: Fluconazole 800 mg load, then 400 mg qdayOR Echinocandin qday (A-I)
Echinocandin preferred if higher illness severity or recent azole exposure (A-III)
2. Remove catheter (A-II)3. Search for metastatic foci4. Rx duration: 2 wks if uncomplicated (A-III)
Pappas et al (2009) CID 48: 503-35 IDSA Candida 2009 Guidelines

Rx Success associated with Catheter Removal
RDBPCT, n=595 candidemic pts
Treatment SuccessCatheter removed 77.9%Catheter not removed 63.2%
P=0.001
Pappas et al (2007) CID 45: 883-93
Micafungin versus Caspofungin for Treatmentof Candidemia and Other Forms of InvasiveCandidiasis
But, also some controversial & contradictory data:Nucci et al CID 51: 295-303 (2010), Horn et al Eur J Clin Micro Infection 29: 223-29 (2010), Kuse et al Lancet 369: 1519-1527 (2007)

Anidulafungin non-inferior to fluconazole, But, … possibly more efficacious
Reboliet al (2007) NEJM 356: 2472

Drug choice & need to check sensitivitiesC. albicans: sensis not routine, based on risksC. glabrata: echinocandin preferred (B-III) or check fluc
sensiC. krusei: no flucC. parapsilosis: fluc preferred (B-III)
IDSA Candida 2009 Guidelines

Short Term CVC Management
Mermel et al CID 2009 IDSA Catheter Rx Recs

Long Term CVC Management
Mermel et al CID 2009 IDSA Catheter Rx Recs

Case 340 yo M with mitral valve prolapse.Dentist plans to place orthodontic brackets.
50 yo F with a history of endocarditis will undergo cystoscopy
What do you recommend for IE prophylaxis?

What is the highest risk of bacteremia exposure?
Tooth extraction Dental Exam Mucoperiosteal surgeryDaily lifeFlossingBrushing teethChewingNT tube
Cumulative exposure measures CFU per minute per ml per year of bacteria
Risk(Relative to tooth extraction)
1 222 5,5551,693,556 365,000 702,556 136,778 166
2007 guidelines: Emphasize that daily activities incur highest risk, rather than procedures.

Lockhart et al Circulation 117: 3118 (2008)

What are risk factors for IE? IE incidence#/100,000 person years
General population 4.9Prior endocarditis Rheumatic heart disease Congenital heart disease: overall VSD with medical Rx VSD with surgical Rx Aortic stenosis Pulmonic stenosis Prosthetic valve MVP with murmur MVP without murmer
Steckelberg & Wilson 1999
740440
120220 60180 20308-383 52 4.6

2007 AHA GuidelinesCardiac Conditions with recommended prophylaxis:1. Prosthetic cardiac valve2. Previous IE 3. Congenital Heart Disease: A. Unrepaired cyanotic CHD, including palliative shunts & conduits B. Completely repaired CHD with prosthetic material or device, during
the first 6 months after the procedure C. Repaired CHD with residual defects at the site or adjacent to the
site of a prosthetic patch or device4. Cardiac transplant recipients who develop cardiac valvulopathy
Compared to 1997: Simplified list with emphasis on risk of adverse outcome from IE rather than risk of acquisition.
(no longer recommended for MVP or RHD)

2007 AHA GuidelinesProcedures for which endocarditis is recommended for
the above categories of patients:1. All dental procedures that involve manipulation of gingival
tissue or the periapical region of teeth or perforation of the oral mucosa.
2. Respiratory tract or infected skin/soft tissue procedures3. NOT recommended for GU or GI procedures solely to
prevent IE
Compared to 1997: Simplified list of which procedures qualify (no GU/GI, criteria for dental procedure straightforward)

Cases 4 & 5HPI: 14 yo M2 m h/o of fever, HA, myalgias. RLQ pain led to appendectomy w/ necrotizing lymphadenitis.
Left calf pain resolved with Abx. After Abx, fever returned Then, R wrist swollen & tender R thigh pain developed.
PE: T 39.3, P 108, BP 128/35II/VI systolic murmursplinter hemorrhages in 3 nails petechial rash on legs
Labs: Bld Cx 6/6 bottles Viridans strep
45 yo M h/o ESLD, HCV, EtOH Fever x 3d. Also with SOB and abdominal pain.
PE: Tm 38.5GingivitisCV III/VI SEM over LUSB, ?splinter hemorrhages 2 nails
Labs: Bld Cx: 1/6 bottles with Viridans strep

Questions:
• What is your DDx?
• How many modified Duke criteria does this patient have?
• How useful are the modified Duke criteria?
• What work-up is needed?

DDx of EndocarditisA. associated with neoplasms: atrial myxoma, marantic (adenoCa), carcinoid
B. associated with autoimmune: rheumatic heart disease, SLE (Libman-Sacks endocarditis), anti-phospholipid syndrome, polyarteritis nodosa, Behcet’s disease
C. Postvalvular operation: thrombus, sutures
D. Other: eosinophilic heart disease, ruptured mitral chordae, myxomatous degeneration

Modified Duke Clinical CriteriaDefinite IE
Pathological criteria:Microorganisms: demonstrated by culture or histology in a vegetation, in a vegetation that has embolized, or in an intracardiac abscess, orPathologic lesions: vegetation or intracardiac abscess present, confirmed by histology showing active endocarditis.
Clinical criteria2 major criteria, or1 major and 3 minor criteria5 minor criteria

Modified Duke Clinical CriteriaPossible IE1 major and 1 minor3 minor
RejectedFirm alternate diagnosis for manifestations of endocarditisResolution of manifestations of endocarditis with antibiotic therapy for ≤ 4 days, orNo pathological evidence of IE at surgery or autopsy, after antibiotic therapy for ≤ 4 days.

Major Criteria1. Positive blood culture for IE
A. Typical microorganism consistent with IE from 2 separate blood cultures as noted below:viridans streptococci, Streptococcus bovis, HACEK group, Staphylococcus aureus, or community-acquired enterococci, in the absence of a primary focus
B. Microorganisms consistent with IE from persistently positive blood cultures as defined as (i) ≥2 positive cultures of blood samples drawn >12 hours apart(ii) all of 3 or a majority of ≥4 separate cultures of blood (with the first and last samples drawn ≥1 hour apart)iii. Coxiella: + Bld cx or anti-phase I Ab titer>1:800

Bacteremia & IE Likelihood
Pathogen IE:non IE RatioS. mutansS. bovis S. sanguis S. mitior E. faecalis S. anginosus Grp G Streptococcus Grp B Streptococcus Grp A Streptococcus
14.2 : 1 5.9 : 1 3.0 : 1 1.8 : 1 1.0 : 1.2 1.0 : 2.6 1.0 : 2.9 1.0 : 7.4 1.0 : 32.0

Major Criteria2. Evidence of endocardial involvement
A. Positive echocardiogram for IE defined as
(i) oscillating intracardiac mass on valve or supporting structures, in the path of regurgitant jets, or on implanted material in the absence of an alternative anatomic explanation, or(ii) abscess, or(iii) new partial dehiscence of prosthetic valve, or
B. New valvular regurgitation (worsening or changing or pre-existing murmur not sufficient)

Minor Criteria1. Predisposition: predisposing heart condition or intravenous drug use2. Fever: temperature ≥ 38.0 C3. Vascular phenomena: major arterial emboli, septic pulmonary infarcts, mycotic aneurysm, intracranial hemorrhage, conjunctival hemorrhage, and Janeway lesions4. Immunologic phenomena: glomerulonephritis, Osler’s nodes, Roth spots, and rheumatoid factor5. Microbiological evidence: positive blood culture but does not meet a major criteria as noted above or serologic evidence of active infection with organism consistent with IE (excludes single positive cultures for coagulase-negative Staphylococci and organisms that do not cause endocarditis).

Clinical Manifestations
Splinter hemorrhages
Osler’s nodes
Janeway’s lesions
Conjunctival hemorrhages
Mylonakis, NEJM, 2001

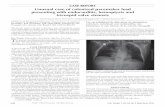
Clinical Manifestations
Septic pulmonary emboli
www.vh.org

Case 6Pt w/ endocarditis w/u has 1 major & 1
minor Duke’s Criteria
• How hard do you search for more criteria?• When do you recommend a brain MRI?• When do you recommend a TEE?• Should all pts with CVC-associated S. aureus
bacteremia get a TEE?

Role of Transesophageal ECHO in diagnosing IE
1. Prosthetic valves
2. Suspected complication
(such as perivalvular abscess)
3. Those in “Possible Endocarditis” category
4. ? Negative TTE & S. aureus bacteremia

Should all patients with S. aureus bacteremia have a TEE?
Arguing in favor:1) Increased sensitivity leads to more diagnoses & better Rx
TTE sensitivity=32%
TEE sensitivity=100%
2) ? Cost effective (save costs of lengthy treatment)
Arguing against:3) TEE more labour intensive
4) Small vegetations may be adequately treated with short course treatment.

Clinical Manifestations: ComplicationsMycotic aneurysm
www.pharmacology2000.com

Duval et al Ann Int Med 152: 497 (2010)
High rate of lesions in neurologically asymptomatic cases

Does it change management?

Assessment of Duke CriteriaSensitivity: 80% for definite IE
100% for definite + possible IE
Negative predictive value >98% for rejected category
Adopted modifications from Li et al (2000)a. S. aureus bacteremia should be a major criteria regardless of the source (community or nosocomial)b. Eliminate the ECHO minor criteria since TEE’s are more widely used nowc. Add Coxiella to list of major criteria (a single positive blood culture or antiphase I IgG antibody titer > 1:800).d. To increase specificity, change the category “possible IE” to cases with 1 major and 1 minor criteria or 3 minor criteria.

Case 730 yo M with h/o IDU with feverDiagnosed with MV IE 2° MRSAStarted on vancomycin/gentamicin
Daily cultures positive x 8 d
Questions:Should a vancomycin MIC be obtained?Should vancomycin troughs be obtained?Should a different drug be used?Does this patient need cardiac surgery?

Fowler et al NEJM 2006
Randomized trialInclusion: positive SA blood cxRandomize to: daptomcyin (n=124)vs. standard therapy ( b-lactam or vancomycin/gentamicin 1 mg/kg x 4d)
Results:Overall success ITT: daptomycin 42.7%
standard Rx: 39.3%Conclusion: Daptomycin is non-inferior to standard Rx
Median duration of bacteremia:Dapto Std Rx P
MRSA 8d 9d 0.28MSSA 4d 3d 0.25

Vancomycin Dose & MICs
Are high MICs associated with poor outcomes? YESProspective observational study (Soriano et al CID 2008)Inclusion: MRSA bacteremia, n=414
If vancomycin MIC = 2OR for mortality: 6.39 (1.68-24.3)
IDSA Guideline for complicated MRSA infection: Goal vanc trough is 15-20 ucg/ml (Rybak et al CID 2009)
Target AUC/MIC Ratios Difficult to achieve with MRSAMonte Carlo Simulations of Different Dosing (Patel et al CID 2011)
Trough of 15-20 Trough of 10-15

NOHidayat et al Arch Int Med 2008
Prospective cohort studyInclusion: MRSA sputum, blood, woundMeasure vancomycin MICCompare high (≥2) vs low (<2) MICCompare achievement of trough goal target of 15 ucg/ml
Do high vanc troughs help? YESKullar et al CID 2011Retrospective study, n=320MRSA bacteremia

Cidal vs PK/PD AdverseStatic Effects
Vancomycin C +/- Problem Renal
Daptomycin C Not for lung Myopathy
Linezolid S OK BM
Ceftaroline C OK OK
TMP-SMX C OK Renal, BM
Is Anything Better than VancFor MRSA? Unknown

Case 8: Rx ?s3. 65 yo female with 4 weeks of fever, myalgias, nausea and decreased appetitie. ECHO: MV vegetation with severe MR.
4. 30 year old male with h/o IVDU and dental caries with fever for 1 day after recent injection. ECHO: AV vegetation with severe AI.
Question:What empiric treatment do you recommend before the results of blood cultures are known?What antibiotics do you recommend for viridans strep? Who can be treated for 2 wks?

Empiric Antibiotic SelectionEmpiric Therapy for IEMain goal is to treat acute IE, most often caused by S. aureus
Acute IE:Vancomycin +/- gentamicin
Subacute IE: more difficult and less important to Rx empirically.Vancomycin + ceftriaxone covers many of the important organisms.

AHA: Rx of Viridans Strep IE
Viridans streptococci & S. bovis, PCN susceptible (MIC ≤0.12 mg/ml)
i. PCN G 12-18 mU iv/day x 4 wks,
ii. ceftriaxone 2g iv or im qd x 4 wks,
iii. PCN G 12-18 mU iv qd + x 2 wks, gentamicin 1 mg/kg iv q8h
iv. vancomycin 1g iv bid x 4 wks (for b-lactam allergic pts)

AHA: Rx of Viridans Strep IE
Viridans streptococci & S. bovis,relatively resistant to PCN (MIC > 0.12 mg/ml & < 0.5 mg/ml)
i. PCN G 24 mU iv/day x 4 wks + gentamicin 3 mg/kg iv qd x 2 wks
ii. Ceftriaxone 2g iv qd x 4 wks + gentamicin 3 mg/kg iv qd x 2 wks
iii. vancomycin 1g iv bid x 4 wks (for b-lactam allergic pts)

AHA: Rx of Enterococcus, Abiotrophia, & Grunulicatella IE
i. PCN G 18-30 mU iv/day x 4-6 wks + gentamicin 1 mg/kg iv q8h x 4-6 wks
ii. ampicillin 12 g/day iv x 4-6 wks + gentamicin 1 mg/kg iv q8h x 4-6 wks
iii. vancomycin 1g iv bid x 6 wks + gentamicin 1 mg/kg iv q8h x 6 wks
(for b-lactam allergic pts)

AHA: Rx of HACEK IE
i. ceftriaxone 2g iv/im qd x 4 wks (or other 3rd or 4th gen. cephalosporin)
ii. Ampicillin-sulbactam 12g iv/day x 4 wks iii. Ciprofloxacin 500 mg po bid or 400 mg iv bid
x 4 wks(less experience with quinolones & HACEK)

Case 916 yo male with a 1 week history of fever to 103 F. Developed confusion, blurrred vision and abdominal pain. Head CT showed hypodense lesions bilaterally in the parietal lobe, abdominal CT showed a 2 cm splenic infarct, and an ophthalmologic exam showed bilateral emboli.
4 out of 4 cultures grew MRSA. ECHO showed mild MR and a vegetation on the anterior leaflet.
Does this patient need cardiac surgery?

Indications for Cardiac Surgery
Valvular dysfunction -Acute aortic or mitral insufficiency with signs of
ventricular failure -Heart failure unresponsive to medical therapy -Valve perforation or rupture
Perivalvular extension -Valvular dehiscence, rupture, or fistula -New heart block -Large abscess, or extension of abscess despite
appropriate antimicrobial therapy.

Indications for Cardiac Surgery
Vegetation
Persistent vegetation after systemic embolization: -Anterior mitral leaflet vegetation, particularly >1 cm-One or more embolic events during the 1st 2 wks of therapy -2 or more embolic events during or after antimicrobial therapy
Increase in vegetation size after 4 weeks of antimicrobial therapy

Complications from IE1. Embolization: Difficult to predict who will embolize
emboli with: AV & MV anterior leaflet, S. aureus, Candida, HACEK, & Abiotrophia organisms,? Size > 1 cm
2. CHF: Poor prognosis with medical Rx aloneDelaying surgery until decompensation will mortality
3. Extracranial Mycotic AneurysmsSurgical intervention advised
4. Intracranial Mycotic AneurysmsDebates @ merits of screening & surgery. Very little data to guide decision.

Case 10CC: fever and rash
HPI: 45 year old male from St. Paul Island in Alaska
R thumb stung by the barb of a yellow-fin Irish Lord fish. Pain, swelling, and erythema of the thumb x 2d, spread to R arm. Prescribed TMP-SMX for cellulitis. Erythema progressed After 1 week, annular, flat, erythematous macules developed on all extremities.Pt developed fever, chills, sweats, nausea, vomiting, and myalgias over the next month.

Culture Negative EndocarditisExposure Common pathogens Diagnostic methodsBirds C. psittaci Complement fixation, ELISAEtOHism, Bartonella quintana “Fastidious” organism bld cx, homeless subCx to chocolate agarAnimals Coxiella burnetti CFA titers to phase I & II Ags
Brucella species “Fastidious” organism bld cx Serology
Nosocomial, Fungiimmuosuppression
STD, Neisseria gonorrhea Bld cx. Commercial systems sexually active may inhibit Neisseria.Epidemic Legionella Special culture for fastidious
pneumophilia organisms, urinary Ag

Culture Negative EndocarditisHoupikian & Raoult Medicine 84: 162-173 (2005)n=348 subjects, France 1983-2001blood culture negative IE
Pathogen N (%)C. burnetti 167 (48)Bartonella 99 (28)Rare fastidious 5 (1) Tropheryma whipplei Abiotrophia elegans Mycoplasma hominis Legionella pneumophilaNo etiology: on abx 58 (16.7)
not on abx 15 (4.3)

GuidelinesBaddour et al Infective Endocarditis: Treatment, Diagnosis, & Management. Circulation 111: e394-433 (2005).
Mermel et al Guidelines for the Management of Intravascular Catheter-Related Infections. CID 49: 1-45 (2009).
Pappas et al Guidelines for the management of Candidiasis CID 48: 503-35 (2009).
Wilson et al Prevention of Infective Endocarditis. Circulation 115: (2007).