Effects of surgical repair of congenital diaphragmatic hernia on cerebral hemodynamics evaluated by...
-
Upload
andrea-dotta -
Category
Documents
-
view
215 -
download
1
Transcript of Effects of surgical repair of congenital diaphragmatic hernia on cerebral hemodynamics evaluated by...
Journal of Pediatric Surgery (2005) 40, 1748–1752
www.elsevier.com/locate/jpedsurg
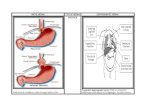
Effects of surgical repair of congenital diaphragmatic
hernia on cerebral hemodynamics evaluated by
near-infrared spectroscopy
Andrea Dotta*, Jole Rechichi, Francesca Campi, Annabella Braguglia,Sabrina Palamides, Irma Capolupo, Simona Lozzi, Alessandro Trucchi,Carlo Corchia, Pietro Bagolan, Marcello Orzalesi
Department of Medical and Surgical Neonatology–Bambino Gesu Children’s Hospital, 00165 Rome, Italy
0022-3468/$ – see front matter D 2005
doi:10.1016/j.jpedsurg.2005.07.001
T Corresponding author. Neonatal In
00165 Rome, Italy. Tel.: +39066859242
E-mail addresses: [email protected]
Index words:Congenital diaphragmatic
hernia;
Near-infrared
spectroscopy;
Newborn
Abstract
Background: Cardiorespiratory stabilization is recommended before surgical repair of congenital
diaphragmatic hernia (CDH) because surgery may induce a transitory deterioration of chest compliance
and gas exchange. It is not known if surgical intervention can affect cerebral circulation and oxygenation.
Aim: The aim of the study was to assess noninvasively, by near-infrared spectroscopy, the possible
changes in cerebral hemodynamics and oxygenation associated with surgical repair of CDH.
Subjects: Twenty-five newborns with severe CDH (birth weight, 3057F 354 g; gestational age, 37.8F
1.8 weeks; male/female newborns, 15/10; left/right CDH, 19/6) were sedated, paralyzed, and
mechanically ventilated by conventional gentle ventilation and surgically corrected at a median age
of 2.7 days (min-max, 2-14 days) after cardiorespiratory stabilization.
Methods: Heart rate (HR [beats per minute]), preductal transcutaneous oxygen saturation (tcSao2 [%]),
carbon dioxide tension (tcPco2 [Torr]), and mean arterial blood pressure (mm Hg) were continuously
monitored. Inspired fractional oxygen concentration (Fio2) was adjusted to maintain a preductal tcSao2
of greater than 80%, whereas the ventilator’s settings were kept unchanged throughout the surgical
procedure. Cerebral hemodynamics was assessed by near-infrared spectroscopy (NIRO 300,
Hamamatsu Photonics, Japan), recording continuously and noninvasively the relative changes in
concentration of oxygenated (DO2Hb [lmol/L]), deoxygenated (DHHb [lmol/L]), and total (DtHb
[lmol/L]) hemoglobin; the tissue oxygenation index (TOI [%]) was also calculated (TOI = O2Hb/O2Hb
+ HHb). Total hemoglobin concentration is considered to be representative of cerebral blood volume.
Arterial blood gases were also measured at the beginning (T1) and at the end of surgery (T2). For all
measurements, results at T1 and at T2, as well as the differences between T1 and T2, have been
expressed as means or medians and SDs or 95% confidence intervals or ranges. The differences
between T1 and T2 were considered statistically significant for a P value of less than .05 by the Student
t test for paired values.
Results: At T1, mean tcSao2%was 94.1 % (SD, 4.6) with a Fio2 of 0.25 (SD, 0.1); at T2, to obtain similar
values of tcSao2 (93.4%; SD, 4.4), it was necessary to increase the Fio2 to 0.37 (SD, 0.14; P b .001).
Elsevier Inc. All rights reserved.
tensive Care Unit, Department of Medical and Surgical Neonatology, bBambino GesuQ Children’s Hospital–IRCCS
7; fax: +39066875540.
t, [email protected] (A. Dotta).
,
Cerebral hemodynamics in congenital diaphragmatic hernia 1749
Mean HR at T1 was 149.5 beats per minute (SD, 9.1) and increased significantly (P b .05) at T2 (165.2
beats per minute; SD, 14.2). Mean arterial blood pressure was 54.7 mm Hg (SD, 7.7) at T1 and did not
change appreciably at T2 (55.6 mm Hg; SD, 8.1). Moreover, tcPco2 did not change significantly
during the procedure (mean tcPco2 = 49.9 Torr [SD, 12.8] at T1 and 57.3 mm Hg [SD, 17.9] at T2).
O2Hb and tHb decreased (P b .001 and b.005) and HHb increased (P b .05) significantly during the
surgical procedure (mean D [SD]: DO2Hb= ÿ10.9 lmol/L [9.7], DtHb = ÿ7.5 lmol/L [11.7], and
DHHb = ÿ3.5 lmol/L [6.8]). Mean TOI was 70% at T1 (normal values N60%) and decreased
significantly at T2 (mean DTOI = ÿ6.1% [SD, 10.6]). In all infants, the greatest changes occurred when
the viscera were positioned into the abdomen.
Conclusions: Notwithstanding the initial cardiorespiratory stabilization, surgical repair of CDH was
associated with a rise in HR and oxygen requirement and a drop in cerebral tHb and O2Hb, suggesting a
reduction in cerebral blood volume and oxygenation. These events were probably due to the combined
effects of an increase in right to left shunting (as indicated by the increased oxygen requirement) and a
decrease in venous return (possibly due to compression of the inferior vena cava by the viscera positioned
into the abdomen). These preliminary results reinforce the importance of achieving a good
cardiorespiratory stability before undertaking surgical correction of CDH to minimize the possible
interference of the procedure with cerebral circulation and oxygenation.
D 2005 Elsevier Inc. All rights reserved.
Congenital diaphragmatic hernia (CDH) is still associ-
ated with a high mortality rate, ranging widely from 25% to
as much as 74% in different centers [1,2]. Among the
various strategies explored in the treatment of CDH, a
delayed approach to surgical repair, after a period of
cardiorespiratory stabilization and gentle ventilation, with
permissive hypercapnia, has been associated with lower
mortality rates [1,3]. Until 20 years ago, CDH was
considered a surgical emergency. In 1986, Cartlidge et al
[4] reported a marked improvement in survival in CDH
newborns who had been stabilized for 4 to 16 hours before
surgery when compared with a historical control group
(from 13% to 54%). Two years later, Langer et al [5]
showed similar mortality rates in CDH patients operated at
a mean age of 4 hours (42%) or at 24 hours (50%). In the
same years, Sakai et al [6] described a significant
deterioration in pulmonary compliance in the immediate
postoperative period in infants with CDH. Following these
studies, the need for immediate surgical intervention in
infants with CDH was reconsidered. In 1998, a report by
the Congenital Diaphragmatic Hernia Study Group, de-
scribing the surgical management of CDH in various
institutions in North America, Europe, and Australia,
highlighted that only 38% of surgical repairs were
performed within 24 hours, whereas in the majority of
cases surgery, surgical repairs was delayed [7]. More
recently, Boloker et al [8] treated 120 infants with high-
risk CDH using permissive hypercapnia/spontaneous respi-
ration/elective repair, with an excellent survival rate and
minimal pulmonary morbidity at discharge. In 2004,
Rozmiarek et al [9] concluded that the most important
negative factors influencing survival in CDH are associated
cardiac defects, renal failure, and initial blood gases and not
the timing of surgery.
Ventilatory strategies used to guarantee adequate gas
exchange in infants with CDH have changed in the last
decades as the understanding of neonatal pathophysiology
improved, showing that a significant cause of mortality
was iatrogenic injury of the hypoplastic lung. In 1981,
Drummond et al [10] showed that alkalosis and hypocapnia
could reverse ductal shunting; as a result, hyperventilation
became a popular ventilatory strategy for CDH in the
following years. More recently, based on the work of Wung
et al [11] and Langham et al [12], it has been recommended
to avoid high peak inspiratory pressures (PIPs) and lung
overdistension. However, the optimal mode of ventilation
for patients with CDH is still unclear. At present, a
permissive hypercapnia strategy is used in most of centers;
moreover, strategies designed to limit lung overdistension
and excessive inspiratory pressures (gentle ventilation) are
considered to be the most adequate modes of ventilation in
CDH [2].
The search for the best ventilatory and surgical strategies
for the management of patients with CDH has focused
mainly on the cardiorespiratory system, and little is known
concerning the effects of surgical repair on cerebral
hemodynamics. Surgery could affect cerebral circulation
in 2 ways: through changes in arterial carbon dioxide
tension (Paco2), which is considered a potent regulator of
the cerebral circulation [13], and through modifications in
arterial blood pressure and systemic venous return, second-
ary to compression of the inferior vena cava by the herniated
viscera repositioned into the abdomen.
Among the different techniques available for studying
cerebral hemodynamics and oxygenation, near-infrared
spectroscopy (NIRS), first introduced by Jobsis [14] in
1977, has gained rapid clinical acceptance because it is
noninvasive, well tolerated by the patient, and relatively
easy to apply at the bedside [15,16]. NIRS takes advantage
of the fact that near-infrared light, generated by a laser
beam, can penetrate up to 6 to 8 cm through the skull into
the neonatal brain. The light beam spreads diffusely into the
Table 1 Major characteristics of the 25 CDH infants studied
Gender (male/female) 15/10
Gestational age, wk (mean F SD) 37.8 F 1.8
Birth weight, g (mean F SD) 3057 F 354
Prenatal diagnosis (n) 21
Side of hernia (left/right) 19/6
Age at surgery, d (mean [median] F SD) 3.5 [2.7] F 2.5
A. Dotta et al.1750
brain; it is partially absorbed by various chromophores
(including oxygenated [O2Hb] and deoxygenated (HHb)
hemoglobin and cytochrome oxidase), and it can be detected
by an appropriate sensor (optode) and conducted to a
photomultiplier. The 2 hemoglobins have different absor-
bance characteristics, depending on their oxygenation state,
and by appropriate elaboration of the light signal at different
wavelengths, it is possible to detect the relative changes in
their concentration. This method not only gives valuable
information on the oxygenation state of the brain, but, by
measuring changes of the total hemoglobin concentration
(tHb = O2Hb + HHb), it provides an estimate of
modifications of the cerebral blood volume (CBV) [15-17].
In our department, infants undergoing surgical correction
of CDH, during the past 3 years, were treated by a standard
protocol and were systematically studied by NIRS. The aim
of this study was to analyze the possible changes in cerebral
hemodynamics and oxygenation during surgical correction
of CDH.
1. Subjects and methods
1.1. Subjects
Only infants with isolated high-risk CDH and without
associated malformations were included in this study. All
infants were managed according to a standard protocol,
based on gentle ventilation and delayed surgery, after
cardiorespiratory stabilization, which has been described
previously [3].
1.2. Neonatal stabilization
In prenatally diagnosed cases, cesarean delivery was
scheduled as close to term as possible. The neonate was
immediately intubated at birth, and gentle conventional
ventilation (PIP V25 cm H2O) (Babylog 8000 plus, Draeger,
Lubeck, Germany; or Stephanie, Ginevri, Rome, Italy) was
Table 2 Cardiorespiratory variables at the beginning (T1) and at the
T1 T2
HR (beats/min) 149.5 F 9.1 165
Sao2 (%) 94.1. F 4.6 93
Fio2 0.25 F 0.05 0.3
MABP (mm Hg) 54.7 F 7.7 55
Values are expressed as means F SD or 95% CI.a Significance of difference: P b .001.
started trying to maintain Paco2 between 40 and 60 Torr, pH
greater than 7.25, and preductal transcutaneous oxygen
saturation (tcSao2) greater than 70% in the first 2 hours of
life and between 75% and 90% in the following hours. When
PIP greater than 25 cm H2O was necessary, we shifted to
high-frequency oscillatory ventilation (3100A, Sensor Med-
ics, Viasys, Conshohocken, PA or Stephanie, Ginevri).
Inhaled nitric oxide was started only if pulmonary hyperten-
sion was present as demonstrated by right to left shunting
through the ductus arteriosus and/or tricuspid insufficiency.
Sedation and paralysis were provided with fentanyl
(2 lg/kg per hour) and pancuronium (0.l mg/kg per hour),
and surgical repair was delayed until cardiovascular and
respiratory stability had been maintained for at least 48 con-
secutive hours, without pulmonary hypertension and with
closed or very small and hemodynamically insignificant
ductus arteriosus.
1.3. Surgical intervention
The surgical procedure was performed in the neonatal
intensive care unit using an abdominal subcostal approach,
without leaving a chest tube. A diaphragmatic patch was
positioned when indicated. The ventilatory settings were
kept unchanged throughout the surgical procedure, whereas
the inspired fractional oxygen concentration (Fio2) was
adjusted, to maintain a preductal tcSao2 greater than 80%.
1.4. Cardiorespiratory monitoring
Heart rate (HR [beats per minute]), preductal tcSao2,
transcutaneous carbon dioxide tension (tcPco2 [Torr]), and
mean arterial blood pressure (MABP [mm Hg]) were
monitored and recorded continuously throughout the surgi-
cal procedure.
1.5. Cerebral monitoring
Cerebral hemodynamics and oxygenation were studied
by NIRS using a NIRO 300 monitor (Hamamatsu
Photonics Inc, Hamamatsu, Japan), consisting of an emitter
and a receiver optode of near-infrared light with an
interoptode distance of 50 mm. The light emitter carries 4
laser diodes operating at 775, 810, 847, and 919 nm, and
the detector optode has 3 photodiodes, mounted in parallel
with increasing distances, permitting the calculation of the
tissue oxygenation index (TOI) [18,19]. The optodes were
placed in a holder on the forehead and held in place by a
end (T2) of surgical repair
DT2-T1 95% CI
.2 F 14.2 15.7a 10.3-21.1
.4 F 4.4 ÿ0.7 ÿ3.1 to 1.6
7 F 0.14 0.12a 0.07-0.17
.6 F 8.1 0.9 ÿ2.7 to 4.6
Table 3 Changes in cerebral hemodynamics and oxygenation
measured by NIRS before (T1) and after (T2) surgical repair
DT2-T1 95% CI P
TOI(%) ÿ6.05 F 10.6 ÿ10.9 to ÿ1.2 b.05
O2Hb (lmol/L) ÿ10.90 F 9.7 ÿ14.0 to ÿ6.9 b.001
tHb (lmol/L) ÿ7.53 F 11.7 ÿ12.4 to ÿ2.7 b.005
HHb (lmol/L) 3.50. F 6.8 0.7-6.3 b.05
Values are expressed as mean differences between T2 and T1 with SD
and 95% CI.
Cerebral hemodynamics in congenital diaphragmatic hernia 1751
self-adhesive sticker and a headband, avoiding the temporal
muscles and the sagittal sinus; interference from ambient
light was prevented by shielding the optodes [19]. This
system allows the continuous detection of relative changes
in the cerebral concentration of tHb, O2Hb, and HHb,
(in micromoles per liter) as well as the calculation of the
TOI (TOI% = O2Hb/O2Hb + HHb) [17,20].
1.6. Data analysis
Baseline values of each variable were recorded immedi-
ately before surgery and were compared with the values
measured at the end of the surgical procedure. The 2 sets of
data were compared using the Student t test for paired
values, and the differences were considered statistically
significant for P values less than .05. Data have been
expressed as means or medians and SD or 95% confidence
intervals (95% CIs) and range where appropriate.
2. Results
2.1. Subjects
Twenty-five consecutive patients with isolated CDH
were studied: mean birth weight, 3057 F 353 g; mean
gestational age, 37.8 F 1.8; male/female newborns, 15/10;
prenatal diagnosis, 21/25; left/right side, 19/6 (Table 1).
Twenty-four infants survived to discharge.
2.2. Surgical intervention
Surgical intervention was performed at a mean age of
3.5 days (median, 2.7; range, 2-14) (Table 1). Mean duration
of the surgical procedure was 109.9 F 69.0 minutes. In
12 cases, a Dacron (Dacron Bard De Bakey, Tempe, AZ)
diaphragmatic patch was positioned. The subcostal laparot-
omy was primarily closed in all cases.
2.3. Cardiorespiratory variables
At the beginning of surgery (T1), the HR was 149.5 F
9.1 beats per minute; the tcSao2 was 94.1%F 4.6%, with an
Fio2 of 0.25 F 0.05; tcPaco2 was 49.9 F 12.8 Torr, and
MABP was 54.7F 7.7 mm Hg. At the end of surgery (T2), to
obtain similar values of tcSao2 (93.4% F 4.4%), it was
necessary to increase the Fio2 to 0.37 F 0.14 (P b .001);
HR increased significantly to 165.2 F 14.2 beats per
minute (P b .001) at T2, whereas tcPaco2 and MABP did
not change significantly (57.3 F 17.9 Torr and 55.6 F
8.1 mm Hg, respectively) (Table 2).
2.4. Cerebral monitoring
TOI, O2Hb, and tHb decreased, whereas HHb increased
significantly during surgery: DTOI = ÿ6.0% F 10.6%
(95% CI, ÿ10.9 to ÿ1.2; P b .05), DO2Hb = ÿ10.9 F
9.7 lmol/L (95%CI,ÿ14.0 toÿ6.9;P b.05),DtHb =ÿ7.5F
11.7 lmol/L (95% CI, ÿ12.4 to ÿ2.7; P b 0.001),
DHH = +3.5 F 6.8 lmol/L (95% CI, 0.71/6.3; P b .005)
(Table 3).
3. Discussion
The present study indicates that infants with isolated
severe CDH, treated with a delayed surgery and gentle
ventilation strategy, experience a moderate but statistically
significant reduction in CBV and cerebral oxygenation
during the surgical procedure.
Despite the adjustment in Fio2, to maintain a preductal
tcSao2 greater than 85%, there was a reduction in cerebral
TOI and oxygenated hemoglobin and an increase in cerebral
deoxygenated hemoglobin during the surgical procedure.
Total hemoglobin, which is an indirect index of CBV, also
decreased significantly during surgery. In particular, in all
infants, the most important modifications in cerebral
hemodynamics were observed when the herniated viscera
were repositioned into the abdomen.
The reasons for these changes are not completely clear.
One possible factor affecting cerebral circulation is Paco2
[13]: hypocapnia induces a vasoconstricting response,
whereas hypercapnia is followed by cerebral vasodilation
[21]. Our infants were mechanically ventilated since birth
with the aim to maintain their Paco2 between 40 and
60 Torr. Moreover, during surgery, the ventilatory settings
were maintained constant, trying to avoid sudden changes in
transmural pulmonary pressure and arterial blood gases.
Furthermore, the Paco2 was continuously recorded by
transcutaneous monitoring and also by arterial blood gas
analysis at the beginning and at the end of surgery, showing
only a modest and insignificant rise. Therefore, it is unlikely
that the observed changes in cerebral hemodynamics were
caused by modifications of the Paco2.
Since the most significant changes were observed during
the repositioning of the herniated viscera into the abdomen, it
is more likely that this maneuver might have interfered with
cerebral perfusion, through a compression of the inferior
vena cava and a reduction of the cardiac venous return. This
possibility is also supported by the significant increase in
HR, which could represent a compensatory phenomenon
aimed at avoiding a fall in perfusion pressure. Since the mean
arterial blood pressure did not change appreciably after
surgery, it is also possible that there was a redistribution of
the cardiac output. These factors, along with the well-known
A. Dotta et al.1752
reduced autoregulation of cerebral blood flow, typical of the
neonatal period, could have led to a decrease in cerebral
perfusion. Considering that these infants underwent surgical
correction after at least 48 hours of cardiorespiratory
stabilization, it appears that the even delayed surgery cannot
avoid moderate changes in cerebral hemodynamics in infants
with CDH. Therefore, it is reasonable to speculate that such
changes could be more marked in the presence of cardiore-
spiratory instability, particularly in preterm infants who are
less capable of autoregulating their cerebral perfusion.
The technique that we used can only measure relative
changes in cerebral circulation and oxygenation and does not
provide absolute values; furthermore, normal standards for
newborn infants are not yet available. Therefore, further and
perhaps more sophisticated studies, including appropriate
controls, are needed to clarify the clinical significance and the
possible long-term consequences of such changes in cerebral
hemodynamics. In any case, it is clear that the cerebral
circulation of infants with severe CDH seems to be
particularly sensitive to invasive maneuvers and that the
introduction of innovative therapeutic strategies for CDH
should include the evaluation of cerebral hemodynamics.
References
[1] Ivascu FA, Hirschl RB. New approaches to managing congenital
diaphragmatic hernia. Semin Perinatol 2004;28(3):185 -98.
[2] Doyle NM, Lally KP. The CDH study group and advances in the
clinical care of the patient with congenital diaphragmatic hernia.
Semin Perinatol 2004;28(3):174-84.
[3] Bagolan P, Casaccia G, Crescenzi F, et al. Impact of a current
treatment protocol on outcome of high-risk congenital diaphragmatic
hernia. J Pediatr Surg 2004;39:313 -8.
[4] Cartlidge PH, Mann NP, Kapila L. Preoperative stabilization in
congenital diaphragmatic hernia. Arch Dis Child 1986;61:1226-8.
[5] Langer JC, Filler RM, Bohn DJ, et al. Timing of surgery for
congenital diaphragmatic hernia: is emergency operation necessary?
J Pediatr Surg 1988;23:731 -4.
[6] Sakai H, Tamura M, Hosokawa Y, et al. Effect of surgical repair on
respiratory mechanics in congenital diaphragmatic hernia. J Pediatr
1987;111:432-8.
[7] Clark RH, Harding WD, Hirschl RB, et al. Current surgical
management of congenital diaphragmatic hernia: a report from the
Congenital Diaphragmatic Hernia Study Group. J Pediatr Surg 1998;
33:1004-9.
[8] Boloker J, Batemen DA, Wung JT, et al. Congenital diaphragmatic
hernia in 120 infants treated consecutively with permissive hypercap-
nia/ spontaneous respiration/elective repair. J Pediatr Surg 2002;37:
357 -66.
[9] Rozmiarek AJ, Qureshi FG, Cassidy L, et al. Factors influencing
survival in newborns with congenital diaphragmatic hernia: the
relative role of timing of surgery. J Pediatr Surg 2004;39:821 -4.
[10] Drummond WH, Gregory GA, Heymann MA, et al. The independent
effects of hyperventilation, tolazoline, and dopamine on infants with
persistent pulmonary hypertension. J Pediatr 1981;98:603 -11.
[11] Wung JT, Sahni R, Moffitt ST, et al. Congenital diaphragmatic hernia:
survival treated with very delayed surgery, spontaneous respiration,
and no chest tube. J Pediatr Surg 1995;30:406 -9.
[12] Langham MR, Kays DW, Beierle EA, et al. Twenty years of progress
in congenital diaphragmatic hernia at the University of Florida. Am
Surg 2003;69:45 -52.
[13] van Bel F, van de Bor M, Baan J, et al. The influence of abnormal
blood gases on cerebral blood flow velocity in the preterm newborn.
Neuropediatrics 1988;19:27-32.
[14] Jobsis FF. Non invasive, infrared monitoring of cerebral and
myocardial oxygen sufficiency and circulatory parameters. Science
1977;198:1264-74.
[15] Adcock LM, Wafelman LS, Hegmier S, et al. Neonatal intensive care
applications of near-infrared spectroscopy. Clin Perinatol 1999;26(4):
893-902.
[16] Naulaers G, Morren G, Van Huffel S, et al. Cerebral tissue
oxygenation index in very premature infants. Arch Dis Child Fetal
Neonatal Ed 2002;87:F189-92.
[17] Weiss M, Schulz G, Fasnacht M, et al. Transcutaneously measured
near-infrared spectroscopic liver tissue oxygenation does not correlate
with hepatic venous oxygenation in children. Can J Anaesth
2002;49(8):824-9.
[18] Schulz G, Keller E, Haensse D, et al. Slow blood sampling from an
umbilical artery catheter prevents a decrease in cerebral oxygenation
in preterm newborn. Pediatrics 2003;111(1):e73-6.
[19] Suzuki S, Takasaki S, Osaki T, et al. A tissue oxygenation monitor
using NIR spatially resolved spectroscopy. Proc SPIE 1999;3597:
582-92.
[20] Valipour A, McGown AD, Makker H, et al. Some factors affecting
cerebral tissue saturation during obstructive sleep apnoea. Eur Respir J
2002;20:444 -50.
[21] Pryds O. Control of cerebral circulation in the high-risk neonate. Ann
Neurol 1991;30:321.