Dual Plating of Humeral Shaft Fractures: Orthogonal Plates Biomechanically Outperform Side-by-Side...
Transcript of Dual Plating of Humeral Shaft Fractures: Orthogonal Plates Biomechanically Outperform Side-by-Side...

BASIC RESEARCH
Dual Plating of Humeral Shaft Fractures: Orthogonal PlatesBiomechanically Outperform Side-by-Side Plates
Victor Kosmopoulos PhD, Arvind D. Nana MD, MBA
Received: 26 June 2013 / Accepted: 5 November 2013
� The Association of Bone and Joint Surgeons1 2013
Abstract
Background Single large-fragment plate constructs cur-
rently are the norm for internal fixation of middiaphyseal
humerus fractures. In cases where humeral size is limited,
however, dual small-fragment locking plate constructs may
serve as an alternative. The mechanical effects of different
possible plate configurations around the humeral diaphysis
may be important, but to our knowledge, have yet to be
investigated.
Questions/purposes We used finite element analysis to
compare the simulated mechanical performance of five
different dual small-fragment locking plate construct con-
figurations for humeral middiaphyseal fracture fixation in
terms of (1) stiffness, (2) stress shielding of bone, (3) hardware
stresses, and (4) interfragmentary strain.
Methods Middiaphyseal humeral fracture fixation was
simulated using the finite element method. Three 90� and
two side-by-side seven-hole and nine-hole small-fragment
dual locking plate configurations were tested in compres-
sion, torsion, and combined loading. The configurations
chosen are based on implantation using either a posterior or
anterolateral approach.
Results All three of the 90� configurations were more
effective in restoring the intact compressive and torsional
stiffness as compared with the side-by-side configurations,
resulted in less stress shielding and stressed hardware, and
showed interfragmentary strains between 5% to 10% in
torsion and combined loading.
Conclusions The nine-hole plate anterior and seven-hole
plate lateral (90� apart) configuration provided the best
fixation. Our findings show the mechanical importance
of plate placement with relation to loading in dual-plate
fracture-fixation constructs.
Clinical Relevance The results presented provide novel
biomechanical information for the orthopaedic surgeon
considering different treatment options for middiaphyseal
humeral fractures.
Introduction
Locking plates for fracture fixation offer biologic and
mechanical advantages and therefore have increased in
popularity. Locking the screws to the plate allows the plate
to sit at a distance offset from the underlying bone surface
providing a biologic advantage for bone fracture healing by
preserving the periosteal blood supply underlying the plate
[12, 13, 26, 31]. Mechanically this provides stability without
Each author certifies that he or she, or a member of his or her
immediate family, has no funding or commercial associations
(eg, consultancies, stock ownership, equity interest, patent/licensing
arrangements, etc) that might pose a conflict of interest in connection
with the submitted article.
All ICMJE Conflict of Interest Forms for authors and Clinical
Orthopaedics and Related Research editors and board members
are on file with the publication and can be viewed on request.
Clinical Orthopaedics and Related Research neither advocates nor
endorses the use of any treatment, drug, or device. Readers are
encouraged to always seek additional information, including FDA-
approval status, of any drug or device prior to clinical use.
This work was performed at the University of North Texas Health
Science Center, Fort Worth, TX, USA.
V. Kosmopoulos (&), A. D. Nana
Bone and Joint Research Center, Department of Orthopaedic
Surgery, University of North Texas Health Science Center,
3500 Camp Bowie Boulevard (CBH 407), Fort Worth,
TX 76107, USA
e-mail: [email protected]
A. D. Nana
Department of Orthopaedic Surgery, John Peter Smith Hospital,
Fort Worth, TX, USA
123
Clin Orthop Relat Res
DOI 10.1007/s11999-013-3379-7
Clinical Orthopaedicsand Related Research®
A Publication of The Association of Bone and Joint Surgeons®

the need for the plate to match the curvature of the bone
surface and without the need to compress and maintain
friction between the plate and bone surface [4, 7, 31].
Currently, the majority of diaphyseal humeral fractures
are treated nonoperatively. In the subset treated opera-
tively, one large-fragment plate construct is considered the
norm for internal fixation. The smaller size of the humerus
in some patients, however, limits the diaphyseal shaft
length and/or diameter available for fixation, and therefore
makes using a large-fragment plate difficult. Difficulties
that arise include the number of screws that can be placed,
a resulting bulky fixation with undesirable stress shielding
[19], and having to precontour the large-fragment plate to
match the diverging anatomy of the humeral metaphysis.
Recent literature suggests that dual small-fragment
plating constructs may be mechanically superior to one
large-fragment plate construct [32] and may have a role in
the fixation of certain fracture patterns. Furthermore, small-
fragment plates for humeral shaft fracture fixation have
shown promising clinical results [18]. Questions remain,
however, regarding how plate placement on the diaphysis
affects the mechanical performance of the dual-plate con-
struct, necessitating further research. Plates typically are
implanted using either a posterior or anterolateral
approach. The posterior approach allows for direct obser-
vation of the fracture and posterior and lateral plate
placement but requires the nerve to be dissected out
because it is in the middle of the operative field. In con-
trast, the anterolateral approach avoids direct observation
of the nerve and allows for anterior and lateral plate
placement.
We used a finite element (FE) method, a computational
simulation approach, to compare the mechanical perfor-
mance of five different dual small-fragment locking plate
constructs for humeral shaft fracture fixation under three
different loading regimens. The five dual-plate placement
configurations chosen are based on implantation using the
aforementioned surgical approaches. Using the different
constructs and the three loading regimens (eccentric com-
pression, torsion, and combined) in a FE humerus fracture
model, we aimed to determine the best plate configuration by
assessing (1) stiffness, (2) bone stress shielding, (3) hardware
stress, and (4) interfragmentary strain.
Materials and Methods
Six (one intact and five fixation) FE models were created
and analyzed using COMSOL Multiphysics1 (Version 4.3;
COMSOL, Inc, Burlington, MA, USA). The intact humeral
cortical bone diaphysis was idealized as a hollow cylinder
with a constant cross section. Dimensions were based on
reported mean values from an MRI study of 20 volunteers
with an average age of 37 years [16]. The length of the
tested portion of the diaphysis was set to 237 mm and the
diameters of the canal and outer bone cortex were 12.1 mm
and 19.3 mm, respectively [16]. Cortical bone was modeled
as an orthotropic material characterized by nine independent
technical constants (E1 = 12.0, E2 = 13.4, E3 = 20.0 GPa; G12
= 4.53, G23 = 6.23, G13 = 5.61 GPa; m12 = 0.376; m23 = 0.235,
m13 = 0.222) [2, 3] with density set to 1817 kg/m3 [22].
To study a worst-case scenario such as an unstable
comminuted fracture, a 1-cm transverse fracture gap was
created at the middiaphysis of the intact model (simulat-
ing an Orthopaedic Trauma Association 12.C.2 fracture)
[1, 5, 6, 18, 19, 23, 30, 32]. Fracture fixation was per-
formed using five different seven-hole and nine-hole small-
fragment (3.5 mm) locking-plate configurations as follows:
(1) nine-hole plate anterior and seven-hole plate lateral, 90�apart (Fig. 1A); (2) nine-hole plate lateral and seven-hole
plate anterior, 90� apart (Fig. 1B); (3) nine-hole plate
anterolateral and seven-hole plate posterolateral, 90� apart
(Fig. 1C); (4) nine-hole plate anterolateral and seven-hole
plate posterolateral, side by side 65� apart (Fig. 1D); and
(5) nine-hole plate posterolateral and seven-hole plate
posteromedial, side by side 65� apart (Fig. 1E). The plates
in all of the aforementioned models were centered to the
fracture gap and locked at a 1-mm offset distance from the
outer cortical bone cortex [1, 5, 25]. The plates are fixed
using a total of eight bicortical locking screws [18, 25, 31]
sequentially alternating between the two plates (four
screws/plate) resulting in all the models having the same
number of fixation points and equal working lengths. Such
a staggered placement of the hardware has been suggested
to reduce the risk of plate fracture [17]. Bicortical screws
were chosen to stabilize the screw-bone interface [6, 7].
The generic locking plates and screws were modeled using
stainless steel material properties (E = 193.0 GPa; m = 0.3;
q = 8000 kg/m3) [24]. Geometric properties of the seven-
hole and nine-hole small-fragment locking plates and
screws are similar to FDA-approved commercial hardware
(Table 1).
Three different loading conditions were applied to test
the fixation constructs [8, 11]: (1) eccentric compression;
(2) torsion; and (3) combined eccentric compression and
torsion (Fig. 2). The eccentric load was inferiorly directed
and applied in 20-N increments to a maximum of 100 N a
distance 40 mm posteromedial to the central longitudinal
humeral axis at a rotation of 23.3� from the frontal plane
[10]. This off-center eccentric loading produces combined
bending and compressive loads on the humeral diaphysis.
Torsion was applied in 1.0-Nm increments from 0.5 Nm to
a maximum of 4.5 Nm along the central longitudinal axis
of the humerus. Combined loading included simultaneous
application of the eccentric compressive and torsional
loads (eg, first load step = 20 N compression and 0.5 Nm
Kosmopoulos and Nana Clinical Orthopaedics and Related Research1
123

torsion; last load step = 100 N compression and 4.5 Nm
torsion).
All outcomes, other than stiffness, are reported at the
maximum loads simulated. The extrinsic compressive stiff-
ness for each simulation was calculated as the slope of the
applied compressive load to deformation curve. An analo-
gous rotational stiffness was calculated as the slope of the
applied torsional load to the resulting rotational deformation.
Stiffness of each of the fixation constructs was compared
with the intact humerus stiffness for each respective load-
ing regimen with positive percentile differences denoting
increases and negative percentile differences denoting
decreases in stiffness. Von Mises stress distributions were
computed for the bone, screws, and plates. Average bone
stress analysis results for each of the fixation constructs were
compared with the intact humerus model. In this manner,
negative percentile changes denote decreased bone tissue
stresses as compared with the intact humerus (indicative of
bone stress shielding after fixation). To characterize the load-
sharing performance of the construct for the screws, two
additional measures were calculated. The first measure,
denoted as the maximum-minimum range, is calculated as
the difference in mean stress between the highest and lowest
stressed screws. The second, the screw-to-screw fluctuation,
is calculated as the difference in mean stress between adja-
cent screws. Lower values in these measures represent better
load-sharing characteristics among the screws. Finally, the
interfragmentary strain was characterized by dividing the
interfragmentary motion by the fracture gap size. The
interfragmentary motion for each construct was calculated
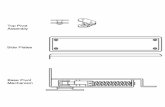
Fig. 1A–E The (A) nine-hole plate anterior and seven-hole plate
lateral, 90� apart (Model A); (B) nine-hole plate lateral and seven-
hole plate anterior, 90� apart (Model B); (C) nine-hole plate
anterolateral and seven-hole plate posterolateral, 90� apart (Model
C); (D) nine-hole plate anterolateral and seven-hole plate posterolat-
eral, side by side 65� apart (Model D); and (E) nine-hole plate
posterolateral and seven-hole plate posteromedial, side by side 65�apart (Model E) fixation construct configurations are shown. The
humeral diaphysis is light gray and the plates and screws are dark
gray. Lateral and anterior directions are oriented to the left and
bottom, respectively.
Table 1. Geometric properties of the small-fragment plates and
screws used in Models A to E
Description Length
(mm)
Width
(mm)
Hole
spacing
(mm)
Number
of holes
3.5-mm small-
fragment
9-hole plate
140 11 14.5 9
3.5-mm small-
fragment
7-hole plate
111 11 14.5 7
Core
length
(mm)
Core
diameter
(mm)
Head
height
(mm)
Head
diameter
(mm)
Locking screw 22 2.7 3.2 6.8
Fig. 2A–C The nine-hole plate anterior and seven-hole plate lateral,
90� configuration (Model A) is used to illustrate the simulated (A)
eccentric compression, (B) torsion, and (C) combined loading
conditions. The force (F) was applied in 20-N increments to a
maximum of 100 N. Torsion was applied in 1-Nm increments from 0.5
Nm to a maximum of 4.5 Nm. The superior (Sup) and inferior (Inf)
cross-sectional bone surfaces used to calculate the interfragmentary
strain also are shown.
Dual Plate Configurations
123

by adding the maximum three-dimensional displacement of
the cross-sectional bone surface superior and cross-sectional
bone surface inferior to the fracture (Fig. 2).
Results
All three of the 90� configurations (Models A through C)
were nearly equally effective in restoring the intact com-
pressive stiffness showing less than a 2% difference in
compression and combined loading, respectively (Fig. 3A).
As a result of geometric equivalency in torsion, Models A
through C behaved equally as did Models D and E. Models
A through C were more effective however, in restoring the
intact torsional stiffness (Fig. 3B). Model E, with the plates
placed side by side posteriorly, was the only construct to
exceed the intact compressive stiffness.
All of the fixation models resulted in some degree of
stress shielding by redistributing the load and consequently
reducing the average stress on the humerus (Fig. 4). The
side-by-side configuration from Model D showed the least
stress shielding in compression, whereas Models A through
C, with the 90� configuration, were better in torsion and
combined loading.
The fixation plates in Models A through C were, on
average, less stressed in torsion and combined loading than
the plates from the side-by-side constructs (Models D and
E). Model E however, with the posteriorly placed plates,
was significantly more effective in reducing plate stresses
in compression (Fig. 5). The highest stress concentrations
were located near and around the unused screw holes for
each plate and at the neck of the screws just below the
plates for all the constructs studied (Fig. 6). Generally, as
evidenced by the lower mean screw stresses, Models A
through C were better at reducing screw stress in torsion
and combined loading than the side-by-side plate con-
structs (Models D and E) (Table 2). Using the screw-to-
screw fluctuation and maximum-minimum range measures
however, Model E showed the best load-sharing charac-
teristics between screws in combined loading.
The 90� configurations tested in Models B and C
resulted in the highest (9.4%) and lowest (7.4%) inter-
fragmentary strains in combined loading, respectively
(Fig. 7). In torsion, the 90� constructs (Models A through
C) resulted in lower interfragmentary strains than the side-
by-side constructs (Models D and E). Models D and E
however, showed the highest (5.0%) and lowest (4.4%)
strain at the fracture site in compression, respectively.
Fig. 3A–B The relative stiffness of each of the tested constructs as a
percentage of (A) the intact compressive (317 N/mm) and com-
bined compressive (293 N/mm) stiffness, and (B) the intact torsional
(5 Nm/degree) and combined torsional (5 Nm/degree) stiffness are
shown. Positive percentile differences denote increases and negative
percentile differences denote decreases as compared with the intact
stiffness.
Fig. 4 The percentages of change in mean von Mises bone stress as
compared with the intact humeral stress in compression (3.4 MPa),
torsion (5.4 MPa), and combined loading (6.7 MPa) are shown. The
results are shown for each of the five construct configurations tested
(Models A through E) in maximum compression (100 N), torsion
(4.5 Nm), and combined (100 N, 4.5 Nm) loading. In torsion, as a
result of geometric equivalency, results are identical among Models A
to C and between Models D and E.
Kosmopoulos and Nana Clinical Orthopaedics and Related Research1
123

Discussion
The smaller size of the humerus in some patients may limit
application of the more commonly used large-fragment
plate constructs. In such cases, large-fragment plates may
limit the number of screws that can be inserted (ie, less
holes/unit length), and lead to increased stress shielding
from the greater mismatch in load transfer between bone
and plate [19, 32]. Dual small-fragment plate constructs
may offer a promising alternative. Dual 3.5-mm locking
plates offer advantages over one large fragment plate
including: (1) the 3.5 mm plate is more easily contoured;
(2) the 3.5 mm plate width easily accommodates small
bone diameters; and (3) dual 3.5 mm plates require a
smaller incision and working length compared with one
large fragment plate. The biomechanical benefits related to
different placement configurations of the two plates,
however, remain unanswered. Using FE modeling, we
compared the performance of five different small-fragment
dual-plate configurations for fixation of middiaphyseal
humeral fractures by evaluating (1) stiffness, (2) bone
stress shielding, (3) hardware stresses, and (4) interfrag-
mentary strain.
Limitations
The results presented are based on the specific plates and
screws modeled and may not be representative for other
plates and screws. Nevertheless, the tested plates and
screws were sized to be similar to what currently is com-
mercially available. Additionally, the use of FE modeling
offers the advantage of studying bone stress shielding as an
Fig. 5 The mean von Mises plate stress comparisons among each of
the five construct configurations tested (Models A through E) in
maximum compression (100 N), torsion (4.5 Nm), and combined
(100 N, 4.5 Nm) loading are shown. In torsion, as a result of
geometric equivalency, the results are identical among Models A
through C and between Models D and E.
Fig. 6A–B The von Mises hardware stress distributions at the
maximum combined load simulated (4.5 Nm torsion, 100 N
compression) for the best-performing configuration with the (A)
nine-hole plate anterior and seven-hole plate lateral, 90� apart (Model
A); and worst-performing configuration with the (B) nine-hole plate
anterolateral and seven-hole plate posterolateral, side by side 65�apart (Model D). Increasing element stress magnitudes are illustrated
from red to blue in the color bar legend and scaled to a maximum of
300 MPa to allow for direct visual comparison.
Table 2. Mean screw stress, fluctuation, maximum-minimum range,
and locations for the highest stressed screws*
Loading Model
A B C D E
Compression
Mean (MPa) 9.5 9.6 9.6 11.6 6.7
Screw-to-screw (MPa) 1.5 1.6 1.6 2.5 2.5
Maximum-minimum (MPa) 5.4 5.5 5.4 8.8 4.4
Screw locations with highest stress 3, 6 4, 5 4, 5 4, 5 2, 7
Torsion�
Mean (MPa) 37.4 37.4 37.4 42.7 42.7
Screw-to-screw (MPa) 6.3 6.3 6.3 7.9 7.9
Maximum-minimum (MPa) 22.1 22.1 22.1 27.9 27.9
Screw locations with highest stress 4, 5 4, 5 4, 5 4, 5 4, 5
Combined
Mean (MPa) 38.9 38.9 38.9 44.7 43.8
Screw-to-screw (MPa) 8.9 8.4 8.3 10.5 7.8
Maximum-minimum (MPa) 30.4 30.2 30.2 37.5 27.7
Screw locations with highest stress 4, 6 3, 5 4, 6 4, 6 4, 5
* Details in Materials and Methods; �because of geometric equiva-
lency in torsion, the measures for Models A through C and for Models
D and E were equal.
Dual Plate Configurations
123

outcome measure. Similar to an experimental cadaveric
study, the computational simulations presented do not
evaluate the in vivo bone remodeling response expected
after internal fixation. Clinically, the mechanics of fixation
are expected to change with stress shielding (eg, bone
resorption) or bone fracture healing, especially with union
of the fracture gap. Fatigue, like with remodeling, is
another time-related response that was not simulated in this
study. Although fatigue microdamage and crack propaga-
tion would provide additional valuable information, it also
would add to the complexity of this numerical study and
outcome variables considered [14]. Screw fixation, for
example, was fixed in the models presented. Clinically,
after cyclic loading, the behavior at the screw-bone inter-
face may weaken [9]. Even with these limitations,
however, the comparisons as presented provide worthwhile
and novel information for the orthopaedic surgeon con-
sidering different treatment options. The stress results from
the study, for example, detail the changes in load transfer
for the bone and each part of the construct otherwise
difficult to measure clinically and experimentally.
Construct stiffness is of high importance. It governs the
performance of the fixation system as indicated, for exam-
ple using the other interrelated outcomes measures reported
(bone stress shielding, hardware stress, and interfragmentary
strain). Excessive stiffness of the fixation construct reduces
stress and strain on the bone and may lead to bone resorption
[13, 28] and in time screw loosening and construct failure
[4, 7, 15, 25]. However, excessive reductions in stiffness may
lead to increasing screw and plate stress and early fatigue
failure of the construct [7, 25, 26]. Stiffness resulting from
the compressive loading simulations of the humerus may be
especially important during crutch weightbearing [18, 19].
Moreover, torsional loading also is of interest in the analysis
of humeral fracture fixation constructs because it has been
reported as a predominant loading mode and possible cause
for nonunion of humeral fractures [7, 8, 29, 30]. In com-
pression and torsion, and consequently combined loading,
the 90� configurations (Models A through C) were found to
outperform the side-by-side constructs in stiffness recovery
as compared with the intact humerus. In our simulations, the
stiffness was relatively insensitive to exchanging the seven-
hole and nine-hole plates, as is done between Models A and
B, or rotating the 90� configuration, as is done between
Models A and C. In contrast, the side-by-side posterior
placement of the plates (Model E), closer to the site of
compressive load application, reduced bending loads on the
plates and increased the construct stiffness beyond that of the
intact humerus.
Ideally, when loaded, the fixation construct design
should be balanced by reducing bone stress shielding yet
maintaining adequate fixation. Model E, with the highest
compressive stiffness, also had the highest levels of aver-
age stress shielding for all three of the loading conditions
tested. Relative to each other however, all the model
configurations tested resulted in less than a 5% difference
in stress shielding. Although in compression and combined
loading the tested configurations resulted in an approxi-
mately 40% to 45% reduction in bone tissue stress, this was
not the case in torsion. The configurations were less
effective in shielding bone shear stress. As recommended
in the literature [1, 5, 25], all of the locking plates modeled
were offset 1 mm from the cortex avoiding undue stress
shielding and contact below the plate. This advantage with
locked plates has been suggested to prevent local bone
necrosis [20].
The stability of the fixation system is influenced by
hardware factors including the number of screws, type of
screws (ie, bicortical, unicortical), working length, plate
offset from the bone cortex, and placement of the hardware
[1, 5–7, 18, 25, 31]. Other than plate placement, these
aforementioned hardware variables were controlled in this
study based on recommendations from the literature. Four
screws per fragment were used based on findings that
additional screws did not show a significant increase in
torsional stiffness [25]. In gauging performance, a goal of
the fixation system should be to reduce and more evenly
distribute the applied stress among the hardware compo-
nents of the construct [27]. This in turn will help limit
stress risers and extend the fatigue life and strength of the
system. O’Toole et al. [18], comparing single-plate locking
and nonlocking 3.5-mm small-fragment constructs for
humeral shaft fixation, reported both constructs withstood
strenuous fatigue and axially failed above anticipated
physiologic loads. Results from all of the dual-plate
Fig. 7 The results for percent interfragmentary strain for the five
construct configurations tested (Models A through E) are shown. The
results are reported at the maximum compressive (100 N), torsional
(4.5 Nm), and combined (100 N, 4.5 Nm) loads. In torsion, as a result
of geometric equivalency, the results are identical among Models A
through C and between Models D and E.
Kosmopoulos and Nana Clinical Orthopaedics and Related Research1
123

locking constructs compared in our study show the
highest stress concentrations occurring at the neck of the
screws just below the screw head and plate. These mod-
eling results confirm clinical findings suggesting this may
be the most likely location for hardware failure [27, 29].
This is especially true for the highest stressed screws
which varied in location based on plate configuration and
type of loading. In compression, Models A and E gener-
ally outperformed the other constructs by more evenly
distributing the applied load among the two plates, with
the larger nine-hole plates sustaining a slightly greater
portion of the stress. As evidenced by the lower mean
screw stress, screw-to-screw fluctuations, and maximum-
minimum ranges, these models also outperformed the
other constructs with respect to load sharing between
screws. However, the highest stressed screws in Model A
were located adjacent to the fracture on the nine-hole
plate. In contrast, the highest stressed screws in Model E
were at the far ends of the seven-hole plate. This is
indicative of the greater bending loads on Model A and
the greater axial loads on Model E. Thus, understanding
how the plate will be loaded based on its placement is
important to reduce hardware stress and improve the load-
sharing characteristics of the construct. This may help
prolong and/or prevent screw failure.
Fixation with locked plate constructs aims to minimize
motion while tolerating an increased fracture gap [4]. Some
motion at the fracture site is favored to promote secondary
bone healing [4, 21, 27]. Secondary bone healing has been
reported to occur when interfragmentary strain is kept
between 2% to 10% [4]. Although biologic responses were
not addressed in our study, all of the tested configurations
did satisfy this interfragmentary strain criteria for all the
loading regimens simulated. Strain at the fracture site was
highest (exceeding 7%) for all the models when combined
loading was applied.
Based on the simulations performed and relative
comparison between outcomes from this study, the 90�configuration with a nine-hole plate placed anteriorly and
a seven-hole plate placed laterally (Model A) was found
to mechanically outperform the side-by-side constructs
and slightly outperform the other 90� configurations
studied. As loading of the humerus in vivo is likely a
combination of compression and torsion, this configura-
tion was one of the most effective in restoring the intact
stiffness and reducing bone stress shielding and hardware
stress while meeting the suggested interfragmentary strain
criteria. Future studies are needed comparing large-frag-
ment plates, nonlocking small-fragment plates, and nail
fixation to the proposed dual small-fragment constructs to
help establish optimal fixation for middiaphyseal humeral
fractures. Although further clinical studies are needed
to confirm our main findings, the mechanical findings
presented using dual 3.5-mm small-fragment locking
plate configurations are promising.
Acknowledgments We thank the University of North Texas Health
Science Center for providing the computational resources needed to
complete this study.
References
1. Ahmad M, Nanda R, Bajwa AS, Candal-Couto J, Green S, Hui
AC. Biomechanical testing of the locking compression plate:
when does the distance between bone and implant significantly
reduce construct stability? Injury. 2007;38:358–364.
2. Ashman RB, Cowin SC, Van Buskirk WC, Rice JC. A continuous
wave technique for the measurement of the elastic properties of
cortical bone. J Biomech. 1984;17:349–361.
3. Cowin SC, Van Buskirk WC. Thermodynamic restrictions on the
elastic constants of bone. J Biomech. 1986;19:85–87.
4. Egol KA, Kubiak EN, Fulkerson E, Kummer FJ, Koval KJ.
Biomechanics of locked plates and screws. J Orthop Trauma.
2004;18:488–493.
5. Fitzpatrick DC, Doornink J, Madey SM, Bottlang M. Relative
stability of conventional and locked plating fixation in a model of
the osteoporotic femoral diaphysis. Clin Biomech (Bristol, Avon).
2009;24:203–209.
6. Fulkerson E, Egol KA, Kubiak EN, Liporace F, Kummer FJ,
Koval KJ. Fixation of diaphyseal fractures with a segmental
defect: a biomechanical comparison of locked and conventional
plating techniques. J Trauma. 2006;60:830–835.
7. Gautier E, Sommer C. Guidelines for the clinical application of
the LCP. Injury. 2003;34(suppl 2):B63–76.
8. Hak DJ, Althausen P, Hazelwood SJ. Locked plate fixation of
osteoporotic humeral shaft fractures: are two locking screws per
segment enough? J Orthop Trauma. 2010;24:207–211.
9. Hepp P, Josten C. Biology and biomechanics in osteosynthesis of
proximal humerus fractures. Eur J Trauma Emerg Surg. 2007;33:
337–344.
10. Hertel R, Knothe U, Ballmer FT. Geometry of the proximal
humerus and implications for prosthetic design. J Shoulder Elbow
Surg. 2002;11:331–338.
11. Jazrawi LM, Bai B, Simon JA, Kummer FJ, Birdzell LT, Koval
KJ. A biomechanical comparison of Schuhli nuts or cement
augmented screws for plating of humeral fractures. Clin Orthop
Relat Res. 2000;377:235–240.
12. Klaue K, Fengels I, Perren SM. Long-term effects of plate
osteosynthesis: comparison of four different plates. Injury. 2000;
31(suppl 2):S-B51–62.
13. Kolodziej P, Lee FS, Patel A, Kassab SS, Shen KL, Yang KH,
Mast JW. Biomechanical evaluation of the schuhli nut. Clin
Orthop Relat Res. 1998;347:79–85.
14. Kosmopoulos V, Schizas C, Keller TS. Modeling the onset and
propagation of trabecular bone microdamage during low-cycle
fatigue. J Biomech. 2008;41:515–522.
15. Lill H, Hepp P, Korner J, Kassi JP, Verheyden AP, Josten C, Duda
GN. Proximal humeral fractures: how stiff should an implant be? A
comparative mechanical study with new implants in human speci-
mens. Arch Orthop Trauma Surg. 2003;123:74–81.
16. Murdoch AH, Mathias KJ, Smith FW. Measurement of the bony
anatomy of the humerus using magnetic resonance imaging. Proc
Inst Mech Eng H. 2002;216:31–35.
17. Nichols SJ, Landon GC, Tullos HS. Arthrodesis with dual plates
after failed total knee arthroplasty. J Bone Joint Surg Am. 1991;
73:1020–1024.
Dual Plate Configurations
123

18. O’Toole RV, Andersen RC, Vesnovsky O, Alexander M,
Topoleski LD, Nascone JW, Sciadini MF, Turen C, Eglseder WA
Jr. Are locking screws advantageous with plate fixation of
humeral shaft fractures? A biomechanical analysis of synthetic
and cadaveric bone. J Orthop Trauma. 2008;22:709–715.
19. Patel R, Neu CP, Curtiss S, Fyhrie DP, Yoo B. Crutch weight-
bearing on comminuted humeral shaft fractures: a biomechanical
comparison of large versus small fragment fixation for humeral
shaft fractures. J Orthop Trauma. 2011;25:300–305.
20. Perren SM, Cordey J, Rahn BA, Gautier E, Schneider E. Early
temporary porosis of bone induced by internal fixation implants: a
reaction to necrosis, not to stress protection? Clin Orthop Relat
Res. 1988;232:139–151.
21. Perren SM. Evolution of the internal fixation of long bone frac-
tures: the scientific basis of biological internal fixation: choosing
a new balance between stability and biology. J Bone Joint Surg
Br. 2002;84:1093–1110.
22. Rho JY, Ashman RB, Turner CH. Young’s modulus of trabecular
and cortical bone material: ultrasonic and microtensile measure-
ments. J Biomech. 1993;26:111–119.
23. Rubel IF, Kloen P, Campbell D, Schwartz M, Liew A, Myers E,
Helfet DL. Open reduction and internal fixation of humeral
nonunions: a biomechanical and clinical study. J Bone Joint Surg
Am. 2002;84:1315–1322.
24. Shah S, Kim SY, Dubov A, Schemitsch EH, Bougherara H, Zdero
R. The biomechanics of plate fixation of periprosthetic femoral
fractures near the tip of a total hip implant: cables, screws, or
both? Proc Inst Mech Eng H. 2011;225:845–856.
25. Stoffel K, Dieter U, Stachowiak G, Gachter A, Kuster MS.
Biomechanical testing of the LCP: how can stability in locked
internal fixators be controlled? Injury. 2003;34(suppl 2):B11–
B19.
26. Stoffel K, Klaue K, Perren SM. Functional load of plates in
fracture fixation in vivo and its correlate in bone healing. Injury.
2000;31(suppl 2):37–86.
27. Strauss EJ, Schwarzkopf R, Kummer F, Egol KA. The current
status of locked plating: the good, the bad, and the ugly. J Orthop
Trauma. 2008;22:479–486.
28. Sumner DR, Galante JO. Determinants of stress shielding: design
versus materials versus interface. Clin Orthop Relat Res. 1992;
274:202–212.
29. Tan SL, Balogh ZJ. Indications and limitations of locked plating.
Injury. 2009;40:683–691.
30. Verbruggen JP, Sternstein W, Blum J, Rommens PM, Stapert JW.
Compression-locked nailing of the humerus: a mechanical ana-
lysis. Acta Orthop. 2007;78:143–150.
31. Wagner M. General principles for the clinical use of the LCP.
Injury. 2003;34(suppl 2):B31–42.
32. Watts A, Weinhold P, Kesler W, Dahners L. A biomechanical
comparison of short segment long bone fracture fixation tech-
niques: single large fragment plate versus 2 small fragment
plates. J Orthop Trauma. 2012;26:528–532.
Kosmopoulos and Nana Clinical Orthopaedics and Related Research1
123