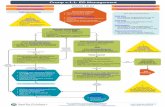
Dr. S. Benson GPSTI. Infections URTI Croup Epiglottitis Whooping Cough Bronchiolitis Pneumonia TB.
-
Upload
delphia-lawrence -
Category
Documents
-
view
220 -
download
1
Transcript of Dr. S. Benson GPSTI. Infections URTI Croup Epiglottitis Whooping Cough Bronchiolitis Pneumonia TB.
URTI Coryza – Usually rhinovirus, coronavirus,
RSVPharyngitis – viral or Group A beta-
haemolytic strepTonsillitis – Group A beta-haemolytic strep
and EBVAcute Otitis Media – viruses, pneumococcus,
strep, haemophilus, moraxella catarrhalisSinusitis – viral or bacterial
URTIChildren often present with:
Sore throatFever (inc febrile convulsions)Blocked NoseNasal DischargeEaracheWheeze
URTIThorough examination is neededExclude serious infectionsAddress feeding and hydrationConsider possible bacterial causes for:
Otitis Media (discharge, ruptured drum, red and bulge)
Tonsillitis (exudative with pus)
Mainstay of treatment is paracetamol and ibuprofen
URTIAntibiotics – to prescribe or not to prescribe?Recommend if tonsilitis or acute OM
Tonsilitis – Give Penecillin V (avoid amoxicillin as maybe caused by EBV – rash)
Acute OM – Coamoxiclav is a suitable choice
Take throat swabs before treatmentMost URTI are viral
CroupViral laryngotracheobronchitisMucosal inflammation of respiratory tractUsually caused by RSV, parainfluenza and
influenzaUsually children are 6 months to 6 years oldPresents as stridor and difficulty breathing
CroupCan be managed at home if mildGive humidified airGive steroids (reduces severity and duration
of croup) oral prednisolone (2mg/kg) for 3 days nebulised budesonide (2mg stat)
Nebulised adrenaline provides transient relief
If severe or desaturating will need admission
Acute EpiglottitisLife threatening swelling of the epiglottisCan cause septicaemiaCaused by haemophilus influenza type BMostly in children 1-6yo
DO NOT examine the throatKeep the child calm
Acute EpiglottitisManagement is in ITUET intubation often required7-10 days of 3rd gen cephalosporinRifampicin prophylaxis for close contacts
Croup vs EpiglottitisCroup Epiglottitis
Time Course Days Hours
Prodrome Coryza None
Cough Barking None
Feeding Can drink None
Mouth Closed Drooling
Toxic No Yes
Fever <38.5 >38.5
Stridor Rasping Soft
Voice Hoarse Weak / Silent
Whooping CoughCaused by bordatella pertussisThree stages of illness
Catarrhal (1-2 weeks) – fever, cough, coryzaParoxysmal (2-6 weeks) – barking coughConvalescent (2-4 weeks) – lesser symptoms
which resolveThe barking cough has a characteristic
paroxysmal nature with an inspiratory whoop
Whooping CoughInvestigations:
Eyes – Subconjunctival haemorrhages are indicated
CXRFBC – Leucocytosis and lymphocytosisNasal swab for pertussis
As part of the work up, we need to ensure this is not pneumonia.
Treatment is with erythromycin / clarythromycinThese have limited effect on cough
Whooping CoughAdmission required if:
ApnoeasCyanosisParoxysmsRisk of seizures
Patients should isolated for 5 daysImmunize close contacts under the age of 7
Only 90% effective and wanes as child agesProphylactic antibiotics to close contacts
BronchiolitisMost commonly due to RSVAlso can be caused by influenza,
parainfluenza, adenovirus, rhinovirus and C and M Pneumoniae
Causes problems by:Invading nasal and pharyngeal epitheliumSpreading to lower airwaysIncreasing mucus production, desquamation
and obstruction
Net effect is hyperinflation and atelectasis
BronchiolitisHistory
Winter monthsCoryzal illnessDry coughWorsening SOBWheezeFeeding problemsApnoeic episodes
BronchiolitisExamination findings
Cyanosis or pallorDry coughTachypnoeaSubcostal and intercostal recessionChest hyperinflationProlonged expirationRespiratory pausesWheeze Crackles
BronchiolitisTreatment mainly supportiveKeep oxygen saturations above 92%If tachypnoeic when feeding consider NG tubeBronchodilators (salbutamol, atrovent,
adrenaline)Mechanical ventilation if severeReserve antivirals for immunodeficient patientsProphylaxis is available for preterm or babies
with chronic lung problems
PneumoniaLower respiratory tract infectionMostly bacterialCommon pathogens shown below
Age PathogenNeonate Group B strep
E. ColiKlebsiellaListeria
Infants Strep pneumoniaeChlamydia
School age Strep pneumoniaeStaph aureusGroup A strepBordatellaMycoplasma pneumoniae
PneumoniaSymptoms and Signs
High tempProductive coughTachypnoea (>50)GruntingRecessionCyanosisLethargyFocal signs / bronchial breathing
PneumoniaInvestigations
NPAFBCMicrobiologyCXR (not of mild and uncomplicated)Pleural fluid if effusion may be indicated
PneumoniaFollow local guidelines for treatmentRecommended treatments are
Amoxicillin CoamoxiclavCefuroxime
Antipyretics can also be helpfulIV fluidsOxygen as requiredPhysiotherapy is not all that helpful in children