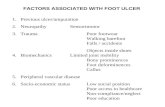
Diabetic Foot Kuliah
Transcript of Diabetic Foot Kuliah

Diabetic FootDiabetic Foot
SURGERY DEPARTMENTSURGERY DEPARTMENTFACULTY OF MEDICINEFACULTY OF MEDICINE
YARSI UNIVERSITYYARSI UNIVERSITYJAKARTAJAKARTA

Introduction
EpidemiologyPathophysiologyClassification Treatment

EpidemiologyDM largest cause of neuropathy in N.A.1 million DM patients in CanadaHalf don’t knowFoot ulcerations is most common cause of hospital admissions for DiabeticsExpensive to treat, may lead to amputation and need for chronic institutionalized care

Epidemiology$34,700/year (home care and social services) in amputeeAfter amputation 30% lose other limb in 3 yearsAfter amputation 2/3rds die in five yearsType II can be worse15% of diabetic will develop a foot ulcer

Pathophysiology
Vascular disease?Neuropathy
SensoryMotor autonomic

Vascular Disease30 times more prevalent in diabeticsDiabetics get arthrosclerosis obliterans or “lead pipe arteries”Calcification of the mediaOften increased blood flow with lack of elastic properties of the arteriolesNot considered to be a primary cause of foot ulcers

Peripheral Artery Disease
Prevalence (ABI < 0.9):Prevalence (ABI < 0.9):10%-20% in type 2 diabetes at diagnosis10%-20% in type 2 diabetes at diagnosis30% in diabetics 30% in diabetics age 50 years age 50 years40%-60% in diabetics with foot ulcer40%-60% in diabetics with foot ulcer
Complications:Complications:ClaudicationClaudicationAssociated coronary and cerebral vascular Associated coronary and cerebral vascular diseasediseaseDelayed ulcer healingDelayed ulcer healing
DiabetDiabet Med.Med. 2005;22:1310 2005;22:1310DiabetesDiabetes Care.Care. 2003;26:3333 2003;26:3333

NeuropathyChanges in the vasonervorum with resulting ischemia ? cause
Increased sorbitol in feeding vessels block flow and causes nerve ischemiaIntraneural acculmulation of advanced products of glycosylation
Abnormalities of all three neurologic systems contribute to ulceration

Sensory NeuropathyLoss of protective sensationStarts distally and migrates proximally in “stocking” distributionLarge fibre loss – light touch and proprioceptionSmall fibre loss – pain and temperatureUsually a combination of the two

Sensory Neuropathy
Two mechanisms of UlcerationUnacceptable stress few times
rock in shoe, glass, burn
Acceptable or moderate stress repeatedly
Improper shoe waredeformity

Motor Neuropathy
Mostly affects forefoot ulcerationIntrinsic muscle wasting – claw toesEquinous contracture

Autonomic NeuropathyRegulates sweating and perfusion to the limbLoss of autonomic control inhibits thermoregulatory function and sweatingResult is dry, scaly and stiff skin that is prone to cracking and allows a portal of entry for bacteria

Autonomic Neuropathy

Gangguan NeuropatiGangguan Neuropati
Paralisis Paralisis Perubahan faal muskuloskeletal kakiPerubahan faal muskuloskeletal kakiPerubahan anatomiPerubahan anatomiTitik tekan di telapak kaki lainTitik tekan di telapak kaki lain
Mati rasaMati rasaCedera tak disadariCedera tak disadariTekanan pada luka tak dihindariTekanan pada luka tak dihindari
Gangguan faal saraf otonomGangguan faal saraf otonomPerfusi kulit kurangPerfusi kulit kurangPintas arteri vena kulit terbukaPintas arteri vena kulit terbuka

Sensory Joint Motor Autonomic PADNeuropathy Mobility Neuropathy Neuropathy
Protective Muscle atrophy and Sweating Ischemia sensation 2° foot deformities 2° dry skin
Foot pressure Foot pressure Fissure HealingMinor trauma esp. over recognition bony prominences
Callus Pre-ulcer ULCER Infection AMPUTATION Minor Trauma: Interdigital Maceration Mechanical (Moisture, Fungus) Chemical Thermal
PATHOGENESIS OF DIABETIC FOOT ULCER AND AMPUTATION
©2006. American College of Physicians. All Rights Reserved.

Nerve damage Poor blood supply
Injury
Infection
Amputation
Ulcer
Pathway to diabetic foot problems

Causal Pathways for Causal Pathways for Foot UlcersFoot Ulcers
NeuropathyNeuropathy
DeformityDeformity
ULCERULCER
% Causal Pathways% Causal Pathways
Neuropathy: Neuropathy: 78% 78%
Minor trauma:Minor trauma: 79%79%
Deformity:Deformity: 63%63%
Behavioral Behavioral ? ?
DiabetesDiabetes Care.Care. 1999; 22:157 1999; 22:157
Poor self-foot carePoor self-foot care
Minor TraumaMinor Trauma
- Mechanical (shoes)- Mechanical (shoes)
- Thermal- Thermal
- Chemical- Chemical

PENYEBABPENYEBAB
AngiopatiAngiopatiPerdarahan jaringan marginalPerdarahan jaringan marginal
NeuropatiNeuropatiParalisis otot kakiParalisis otot kakiRasa matiRasa matiGangguan saraf otonomGangguan saraf otonom
TraumaTrauma

Motor Neuropathy and Foot Deformities
Hammer toesHammer toes
Claw toesClaw toes
Prominent metatarsal headsProminent metatarsal heads
Hallux valgusHallux valgus
Collapsed plantar archCollapsed plantar arch

Hammer Toes
Claw Toes
© 2002 American Diabetes AssociationFrom The Uncomplicated Guide to Diabetes ComplicationsReprinted with permission from The American Diabetes Association


© 2002 American Diabetes AssociationFrom The Uncomplicated Guide to Diabetes ComplicationsReprinted with permission from The American Diabetes Association
Hallux Valgus

Boulton, et al. Guidelines for Diagnosis of Outpatient Management of Diabetic Peripheral Neuropathy. Diabetic Medicine 1998, 15:508-512

Pre-ulcer Cutaneous Pathology
Persistent erythema after shoe Persistent erythema after shoe removalremoval
CallusCallus
Callus with subcutaneous Callus with subcutaneous hemorrhagehemorrhage
FissureFissure
Interdigital maceration, fungal Interdigital maceration, fungal infectioninfection
Nail pathologyNail pathology

AJM Boulton, H Connor, PR Cavanagh, The Foot in Diabetes, 2002
Pre-ulcer

Sukar sembuh karena:Sukar sembuh karena:
Trauma terus menerusTrauma terus menerus
Tekanan abnormalTekanan abnormal
Lingkungan diabetes subur untuk Lingkungan diabetes subur untuk berkembangnya kuman patogenberkembangnya kuman patogen
Perfusi jaringan kulit kurang baikPerfusi jaringan kulit kurang baik
Kurang mendapat nutrienKurang mendapat nutrien

Monofilament TestingTest characteristics:Test characteristics:
Negative predictive value = 90%-98%Negative predictive value = 90%-98%
Positive predictive value = 18%-36%Positive predictive value = 18%-36%
Prospective observational study:Prospective observational study:80% of ulcers and 100% of amputations 80% of ulcers and 100% of amputations occur in insensate feetoccur in insensate feet
Superior predictive value vs. other test Superior predictive value vs. other test modalitiesmodalities
J Fam Pract. 2000;49:S30Diabetes Care. 1992;15:1386

Using the MonofilamentDemonstrate on forearm or handDemonstrate on forearm or hand
Place monofilament perpendicular Place monofilament perpendicular to test siteto test site
Bow into C-shape for 1 secondBow into C-shape for 1 second
Test 4 sites/foot Test 4 sites/foot
Heel testing does Heel testing does notnot predict ulcer predict ulcer
Avoid calluses, scars, Avoid calluses, scars, and ulcersand ulcers

Monofilament Testing Tips
Insensate at 1 site = insensate feetInsensate at 1 site = insensate feet
Falsely insensate with edema, cold Falsely insensate with edema, cold feetfeet
Test annually when sensation Test annually when sensation normalnormal
Use monofilament Use monofilament < 100 times day < 100 times day
Replace if bentReplace if bent
Replace every 3 monthsReplace every 3 months





Vibration TestingBiothesiometerBiothesiometer
Best predictor of foot ulcer riskBest predictor of foot ulcer risk
128-Hz tuning fork at halluces128-Hz tuning fork at hallucesEquivalent to 10-g monofilamentEquivalent to 10-g monofilamentNewly recommended by ADANewly recommended by ADA
DiabetesDiabetes Care.Care. 2006;29(Suppl 1):S25 2006;29(Suppl 1):S25DiabetesDiabetes ResRes ClinClin PractPract. 2005;70:8. 2005;70:8

Diagnosis Angiopati Diagnosis Angiopati DiabetesDiabetes
Gambaran klinisGambaran klinisDerajat kelainan kakiDerajat kelainan kaki
Tipe angiopatiTipe angiopatiMakroangiopatiMakroangiopatiMikroangiopatiMikroangiopati
Sifat ObstruksiSifat ObstruksiAkutAkutKronik Kronik
Status pembuluh darahStatus pembuluh darahPulsasi denyut nadiPulsasi denyut nadiDoppler Doppler

BASIC FOOT CARE CONCEPTS
Daily foot inspectionMay require mirror, magnification, or caregiverEducate patient to recognize/report ASAP:
Persistent erythemaEnlarging callusPre-ulcer (callus with hemorrhage)
©2006. American College of Physicians. All Rights Reserved.

BASIC FOOT CARE CONCEPTS
Commitment to self-care:Wash/dry daily
Avoid hot water; dry thoroughly between toes
Lubricate daily (not between toes)Debride callus/corn to reduce plantar pressure 25%
Avoid sharp instruments, corn plasters
No self-cutting of nails if:Neuropathy, PAD, poor vision
©2006. American College of Physicians. All Rights Reserved.

BASIC FOOT CARE CONCEPTS
Protective behaviors:Avoid temperature extremesNo walking barefoot/stocking-footedAppropriate exercise if sensory neuropathy
Bicycle/swim > walking/treadmill
Inspect shoes for foreign objectsOptimal footwear at all times
©2006. American College of Physicians. All Rights Reserved.

Basic Footwear Education
AvoidAvoid::Pointed Pointed toestoesSlip-onsSlip-onsOpen toesOpen toesHigh heelsHigh heelsPlasticPlasticBlack colorBlack colorToo smallToo small
FavorFavor::
Broad-round toesBroad-round toes
Adjustable (laces, Adjustable (laces, buckles, Velcro)buckles, Velcro)
Athletic shoes, walking Athletic shoes, walking shoesshoes
Leather, canvasLeather, canvas
White/light colorsWhite/light colors
½” between longest ½” between longest toe and end of shoetoe and end of shoe
Diabetes Self-Management. 2005;22:33

©2006. American College of Physicians. All Rights Reserved.

Patient Evaluation
MedicalVascular OrthopedicIdentification of “Foot at Risk”
? Our job

Patient EvaluationSemmes-Weinstein Monofilament Aesthesiometer
5.07 (10g) seems to be threshold
90% of ulcer patients can’t feel it
Only helpful as a screening tool

Patient Evaluation
Medical Optimized glucose controlDecreases by 50% chance of foot problems

Patient EvaluationVascular
Assessment of peripheral pulses of paramount importanceIf any concern, vascular assessment
ABI (n>0.45)Sclerotic vessels
Toe pressures (n>40-50mmHg)TcO2 >30 mmHg
Expensive but helpful in amp. level

Patient Evaluation
OrthopedicUlcerationDeformity and prominencesContractures

Patient Evaluation
X-rayLead pipe arteriesBony destruction (Charcot or osteomyelitis)Gas, F.B.’s

Patient Evaluation

Patient EvaluationNuclear medicine
OverusedCombination Bone scan and Indium scan can be helpful in questionable cases (i.e. Normal X-rays)Gallium scan useless in these patientsBest screen – indium – and if Positive – bone scan to differentiate between bone and soft tissue infection

Patient Evaluation
CT can be helpful in visualizing bony anatomy for abscess, extent of diseaseMRI has a role instead of nuclear medicine scans in uncertain cases of osteomyelitis

Derajat Kelainan Kaki Derajat Kelainan Kaki Diabetik (WAGNER)Diabetik (WAGNER)
DerajatDerajat SifatSifat
LukaLuka AbsesAbses SelulitisSelulitis OsteoOsteomielitismielitis
GangGanggrengren
00 -- -- -- -- --
II SuperfisialSuperfisial -- -- -- --
IIII sampai sampai tendo/tendo/tulangtulang
-- -- -- --
IIIIII DalamDalam ++++ +/-+/- +/-+/- --
IVIV DalamDalam +/-+/- +/-+/- +/-+/- JariJari
VV GanggrenGanggren Seluruh Seluruh kakikaki

Ulcer ClassificationWagner’s Classification0 – Intact skin (impending ulcer)1 – superficial2 – deep to tendon bone or ligament3- osteomyelitis4 – gangrene of toes or forefoot5 – gangrene of entire foot

ClassificationType 2 or 3

ClassificationType 4

Treatment
Patient educationAmbulationShoe wareSkin and nail careAvoiding injury
Hot waterF.B’s

Treatment
Wagner 0-2Total contact castDistributes pressure and allows patients to continue ambulationPrinciples of application
Changes, Padding, removal
Antibiotics if infected

Treatment

Treatment
Wagner 0-2Surgical if deformity present that will reulcerate
Correct deformityexostectomy

Treatment
Wagner 3Excision of infected boneWound allowed to granulateGrafting (skin or bone) not generally effective

Treatment
Wagner 4-5Amputation
Level ?

Treatment
After ulcer healedOrthopedic shoes with accommodative (custom made insert)Education to prevent recurrence

Charcot FootMore dramatic – less common 1%Severe non-infective bony collapse with secondary ulcerationTwo theories
NeurotraumaticNeurovascular

Charcot FootNeurotraumatic
Decreased sensation + repetitive trauma = joint and bone collapse
NeurovascularIncreased blood flow → increased osteoclast activity → osteopenia → Bony collapseGlycolization of ligaments → brittle and fail →
Joint collapse

Classification
Eichenholtz1 – acute inflammatory process
Often mistaken for infection
2 – coalescing phase3 - consolidation

Classification
LocationForefoot, midfoot (most common) , hindfoot
Atrophic or hypertrophic Radiographic findingLittle treatment implication


Case 1

Case 1

Case 1

Case 2

Case 2

Case 3

Case 3

Case 4

Case 4

Indications for Amputation
Uncontrollable infection or sepsisInability to obtain a plantar grade, dry foot that can tolerate weight bearingNon-ambulatory patientDecision not always straightforward

Low RiskAnnual comprehensive foot Annual comprehensive foot examinationexamination
Questionnaire completed by patient Questionnaire completed by patient
ExaminationExamination
Self-management and footwear Self-management and footwear educationeducation
Brief counselingBrief counseling
Written handoutWritten handout
JAMA. 2005;293:217

High RiskAnnual comprehensive foot examAnnual comprehensive foot exam
Inspect feet every office visitInspect feet every office visit
Podiatry care as neededPodiatry care as needed
Intensive patient educationIntensive patient education
Detect/manage barriers to foot Detect/manage barriers to foot carecare
Therapeutic footwear, as neededTherapeutic footwear, as needed

Therapeutic Footwear Goals
Protect feetProtect feetReduce plantar pressure, shock, and Reduce plantar pressure, shock, and shear shear Accommodate, stabilize, support Accommodate, stabilize, support deformitiesdeformitiesSuitable for occupation, home, leisureSuitable for occupation, home, leisure
DiabetesDiabetes Care.Care. 2004;27:1832 2004;27:1832DiabDiab MetabMetab ResRes RevRev. 2004;20(Suppl1):S51. 2004;20(Suppl1):S51

Therapeutic Footwear Components
Padded socks Padded socks (e.g., CoolMax, (e.g., CoolMax, Duraspun, others)Duraspun, others)
Shoe inserts/insoles Shoe inserts/insoles (closed-cell (closed-cell foam, viscoelastic)foam, viscoelastic)
Therapeutic shoesTherapeutic shoes

Therapeutic Footwear Efficacy
Decreases plantar pressure 50%-Decreases plantar pressure 50%-70%70%Uncertain reduction in ulcer rateUncertain reduction in ulcer rate
DiabetesDiabetes CareCare. 2004;27:1774. 2004;27:1774

ConclusionDiabetic foot ulcer is commonDiabetic foot ulcer is common
Foot ulcers have devastating Foot ulcers have devastating consequencesconsequences
Screening is simpleScreening is simple
Screening and team care reduce Screening and team care reduce diabetic foot ulcers and diabetic foot ulcers and amputationsamputations

Conclusion
Multi-disciplinary approach neededGoing to be an increasing problemHigh morbidity and costSolution is probably in preventionMost feet can be spared…at least for a while



















©2006. American College of Physicians. All Rights Reserved.



Thank You