Cysteine-Rich61(CCN1)EnhancesChemotactic … · (T2tumor; Fig. 2B) patterns of Cyr61 and...
Transcript of Cysteine-Rich61(CCN1)EnhancesChemotactic … · (T2tumor; Fig. 2B) patterns of Cyr61 and...

Cysteine-Rich 61 (CCN1) Enhances ChemotacticMigration, Transendothelial Cell Migration, andIntravasation by Concomitantly Up-RegulatingChemokine Receptor 1 and 2
Been-Ren Lin,1 Cheng-Chi Chang,2 Li-Ro Chen,2 Ming-Hsun Wu,1 Ming-Yang Wang,1
I-Hsin Kuo,2 Chia-Yu Chu,2 King-Jen Chang,1,3 Po-Huang Lee,1 Wei-Jao Chen,1
Min-Liang Kuo,2,3 and Ming-Tsan Lin1,4
1Department of Surgery, 2Laboratory of Molecular and Cellular Toxicology, Institute of Toxicology,College of Medicine, 3Angiogenesis Center, and 4Department of Primary Care Medicine,National Taiwan University, Taipei, Taiwan
AbstractCysteine-rich 61 (Cyr61; CCN1) plays an important role
in tumor development and progression in many kinds of
human malignancies. Here, we further show the
enforced expression of the Cyr61 gene or treatment with
recombinant Cyr61 protein enhanced expression of
chemokine receptors CXCR1 and CXCR2 in gastric
cancer AGS cells. Attenuation of Cyr61 levels in MKN-45
cells by transfecting with antisense Cyr61 significantly
reduced the level of CXCR1 and CXCR2. It is suggested
that Cyr61 tightly regulates the downstream genes
CXCR1 and CXCR2 in gastric cancer cells. Supportively,
reverse transcription–PCR and immunohistochemical
analysis of human gastric adenocarcinoma showed
that there was a high correlation between the
expression level of Cyr61 and CXCR1/CXCR2. The
up-regulated functionality of CXCR1 andCXCR2 in
Cyr61-overexpressing AGS cells could facilitate their
chemotactic migration toward interleukin-8, a
physiologic ligand of CXCR1 and CXCR2. In addition,
the Cyr61-mediated up-regulation of CXCR1/CXCR2 also
contributed to transendothelial migration, as well as
intravasation in a chick embryo model. Pharmacologic
and genetic approaches revealed that phosphoinositide
3-kinase (PI3K)/Akt, but not extracellular signal-regulated
kinase 1/2 or p38, signaling pathway is requisite for the
up-regulation of CXCR1/CXCR2 mRNA and protein
induced by Cyr61. Function-neutralizing antibody to
integrin AvB3, but not A2B1, effectively abolished
Cyr61-elicited Src activation and the subsequent PI3K/
Akt pathway. Antagonists toward integrin AvB3, Src
kinase, and PI3K/Akt not only suppressed CXCR1/
CXCR2 elevation but also blocked chemotactic
migration induced by Cyr61. In conclusion, we suggest
that Cyr61 promotes interleukin-8–dependent
chemotaxis, transendothelial migration, and
intravasation by induction of CXCR1/CXCR2 through
integrin AvB3/Src/PI3K/Akt–dependent pathway.
(Mol Cancer Res 2007;5(11):1111–23)
IntroductionGastric cancer is the second most common cause of cancer
mortality in the world behind lung cancer (1). It has been
estimated that there will have been >870,000 deaths from the
disease in the year 2000, accounting for f12% of all cancer
deaths (2). Approximately 65% of patients with gastric
carcinoma have regional or distant metastases at the time of
diagnosis. Despite the aggressiveness of surgical and chemo-
therapeutic treatment, the five-year survival rate in metastatic
and advanced stages is extremely poor, ranging from 5% to
15% (3). We have devoted to surgery and perioperative care for
gastric cancer patients, and have gained good perioperative
results (4, 5). However, a better understanding of the
progression of the disease would provide for relevant
development of therapies designed to prevent tumor invasion
and metastasis. Although a number of molecules have been
implicated in the metastasis of gastric cancer cells, the precise
mechanisms determining the directional migration and invasion
of cancer cells into specific organs remain to be established.
There is emerging evidence demonstrating the contribution of
chemokine receptors to organ-specific metastasis, which
provides important clues about why some cancers metastasize
to specific organs (6-8).
Chemokine receptors are G-protein coupled, seven-
transmembrane receptors (9). Based on the chemokine class
they bind, the receptors have been named CXCR1, 2, 3, 4 and
5 (bind CXC chemokines); CCR1 through CCR9 (bind CC
chemokines); XCR1 (binds the C chemokine, Lptn); and
CX3CR1 (binds the CX3C chemokine, fractalkine or neuro-
tactin). More than 50 chemokines have been discovered thus
far, and there are at least 18 human seven-transmembrane-
domain chemokine receptors (10, 11). Studies of human cancer
biopsy samples and mouse cancer models show that chemokine
Received 9/7/06; revised 7/8/07; accepted 7/13/07.Grant support: National Science Council of Taiwan (NSC 93-2320-B-002-019,93-2323-B-002-007, 95-2314-B-002-175).The costs of publication of this article were defrayed in part by the payment ofpage charges. This article must therefore be hereby marked advertisement inaccordance with 18 U.S.C. Section 1734 solely to indicate this fact.Requests for reprints: Ming-Tsan Lin, Department of Primary Care Medicineand Surgery, National Taiwan University Hospital, No. 7, Chung-Shan S. Road,Taipei 100, Taiwan. Phone: 886-2-23123456-5732; Fax: 886-2-23412969.E-mail: [email protected] D 2007 American Association for Cancer Research.doi:10.1158/1541-7786.MCR-06-0289
Mol Cancer Res 2007;5(11). November 2007 1111on April 8, 2020. © 2007 American Association for Cancer Research. mcr.aacrjournals.org Downloaded from

receptor expression of cancer cells is associated with increased
metastatic capacity. For example, CXCR4 and/or CCR7 are
commonly expressed in a wide variety of cancers and in cancer
cells, including breast (7), prostate (12) and ovarian cancer (13),
neuroblastoma (14), and certain types of leukemia (15). The
function of CXCR4 and CCR7 is required for tumor cell
invasion and metastasis (16). CXCR1 and CXCR2 are also
found to be expressed in prostate cancer (17), melanoma (18),
pancreatic cancer (19) and colorectal cancer (20), and their
expression levels are positively correlated with the more
aggressive and advanced stage of these cancers. Above all,
chemokine receptors might be involved in selective metastasis
of cancer cells to specific body sites with high-level expression
of their ligands.
FIGURE 1. Induction of CXCR1 and CXCR2 chemokine receptors by Cyr61. A. Top, the transcripts of chemokine receptors in wild-type AGS cells andstably transfected with Cyr61-expressing plasmid, including mix population (AGS/Cyr61 mix), single clones (AGS/Cyr61-1, AGS/Cyr61-5, AGS/Cyr61-7), andcontrol vector (AGS/neo) by RT-PCR analysis. h-Actin was used as a loading control of RT-PCR. Bottom: Western blot analysis of total cell lysates probedwith Cyr61, CXCR1, CXCR2, CXCR4, and a-tubulin. a-Tubulin was used as a loading and transferring control. B. Top, Western blot was used to detect theprotein levels of Cyr61, CXCR1, and CXCR2 in different gastric cancer cell lines. a-Tubulin was used as an internal control of protein loading and transferring.Bottom, the protein levels of Cyr61, CXCR1, CXCR2, and CXCR4 in Cyr61 or antisense Cyr61 (Cyr61-AS ) transient transfectants. After transientlyexpressing Cyr61 in various dosages in AGS cells (left ) and antisense Cyr61-expressing plasmids in MKN45 cells (right ) for 48 h, total cell protein wasextracted and Western blotting analysis was done. C. Top, the CXCR1 and CXCR2 mRNA expression by conditioned medium treatment of Cyr61transfectants as detected by RT-PCR analysis. Cyr61 neutralizing antibody (10 Ag/mL) or control IgG was placed with conditioned medium to depleteCyr61 protein existence. Bottom, the protein levels of CXCR1 and CXCR2 were analyzed per sample, and a-tubulin was used as internal control. D. Top,rCyr61 stimulated AGS cells for 12 h, and the CXCR1 and CXCR2 protein expression was detected by Western blot analysis. Bottom, rCyr61 (40 ng/mL)treated AGS cells as indicated time, and total cellular lysates probed with specific CXCR1 and CXCR2 antibodies. a-Tubulin was used as internal control.
Lin et al.
Mol Cancer Res 2007;5(11). November 2007
1112
on April 8, 2020. © 2007 American Association for Cancer Research. mcr.aacrjournals.org Downloaded from

Cysteine-rich 61 (Cyr61) is the first cloned member of
the CCN family (21), which comprises connective tissue
growth factor, Cyr61 (CCN1), nephroblastoma overexpressed
(Nov/CCN3), Wisp-1/elm1 (CCN4), Wisp-2/rCop1 (CCN5),
and Wisp-3 (CCN6). Most members of the CCN family share a
uniform modular structure and exhibit diverse cellular function,
such as regulation of cell division, chemotaxis, apoptosis,
adhesion, motility, and ion transport (22-24). Cyr61 has been
reported to mediate cell adhesion, stimulate chemostasis,
augment growth factor– induced DNA synthesis, foster cell
survival, and enhance angiogenesis (25, 26). Elevated Cyr61
expression is associated with advanced breast adenocarcinoma
pathogenesis, pancreatic cancer, and gliomas (27-29). Our
previous study showed that Cyr61 protein is highly expressed
in more advanced gastric adenocarcinoma specimens, and
overexpressed Cyr61 in human gastric cancer cell lines
significantly increased their invasion abilities (30). In the
present study, we further explored how Cyr61 promotes the up-
regulation of chemokine receptors CXCR1 and CXCR2
through the signaling pathway integrin avh3/Src/phosphoino-
sitide 3-kinase (PI3K)/Akt. Functional dissection showed that
the Cyr61-mediated expression of CXCR1/CXCR2 was
involved in gastric cancer cells, transendothelial migration,
and intravasation in a chick embryo model.
ResultsEnforced Expression of CYR61 Gene in Gastric CancerCells Lead to Up-Regulation of Chemokine ReceptorsCXCR1 and CXCR2
We previously found that CYR61 was highly expressed in
more advanced gastric adenocarcinoma specimens, and over-
expressed Cyr61 in human gastric cancer cell lines significantly
increased their migration and invasion abilities (30). Recently,
inherent chemokine receptors have had an important role in
determining distant organ dissemination of cancer cells (7, 8).
Here, we attempt to explore the hypothesis whether over-
expression of Cyr61 would affect the expression of chemokine
receptors in gastric cancer cells. Initially, we used several Cyr61
stable expression AGS clones, including Cyr61-C1, Cyr61-C5,
Cyr61-C7, and Cyr61-M, which have been established and
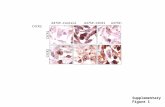
FIGURE 2. CXCR1 and CXCR2 expres-sion correlated with Cyr61 gene in primarygastric carcinomas. A. RNA was isolated from20 cancerous tissues (T1-T20) and fournormal tissues (N1-N4); cDNA was synthe-sized and subjected to RT-PCR for analysis ofCyr61, CXCR1 , and CXCR2 mRNA expres-sion. B. Immunohistochemical staining forCyr61, CXCR1, and CXCR2 of formalin-fixed,paraffin-embedded gastric carcinomas. IgGstaining was used as a negative control.
Cyr61 Promotes Invasiveness of Gastric Cancer
Mol Cancer Res 2007;5(11). October 2007
1113
on April 8, 2020. © 2007 American Association for Cancer Research. mcr.aacrjournals.org Downloaded from

well characterized previously (30, 31). Chemokine receptors,
such as CXCR1, CXCR2, CXCR4, and CCR7 (32, 33), have
been shown to be differentially expressed on gastric cancer
specimens that are associated with tumor aggressiveness.
Reverse transcription–PCR (RT-PCR) analysis was thus used
and showed that both CXCR1 and CXCR2 , but not other
chemokine receptors, mRNA were concomitantly elevated in
the Cyr61-expressing AGS cells compared with the neo control
cells (Fig. 1A, top). Moreover, there was a trend toward a
positive expression pattern for Cyr61 and CXCR1/CXCR2
mRNA in these stable clones (Fig. 1A, top). Consistently,
Western blot analysis revealed that the level of CXCR1 and
CXCR2 protein was significantly increased in the Cyr61-
expressing cells but not in the neo control cells (Fig. 1A,
bottom). Interestingly, the correlated expression of Cyr61 and
CXCR1/CXCR2 also existed in other gastric cancer cells, N87,
TSGH, and MKN45 (Fig. 1B, top). TSGH and MKN45 cells,
which have higher levels of Cyr61 protein, exhibited an
abundant level of CXCR1/CXCR2; in contrast, AGS and N87
cells, which expressed lower levels of Cyr61, displayed a trace
amount of CXCR1/CXCR2. When MKN45 cells were
transiently transfected with increasing amounts of plasmids
carrying the antisense orientation of Cyr61 , the level of CXCR1
and CXCR2 protein was effectively reduced in a dose-
dependent manner (Fig. 1B, bottom).
Because Cyr61 is a secreted protein, we collected 24-h
conditioned medium from Cyr61-overexpressing (AGS/Cyr61-
C7) and neo control cells. When parental AGS cells were
exposed to conditioned medium of AGS/Cyr61-C7, but not
control cells, the levels of CXCR1/CXCR2 mRNA and protein
were significantly elevated (Fig. 1C). The elevation was
strongly diminished if conditioned medium was before
immunodepletion of Cyr61 protein by anti-Cyr61 antibody
(Fig. 1C). In addition, we also used recombinant human Cyr61
protein to test its ability in induction of CXCR1/CXCR2 protein.
It was shown that the expression of CXCR1/CXCR2 protein
increased dose dependently by treatment with 10 to
80 ng/mL of recombinant Cyr61 (rCyr61; Fig. 1D, top). In
general, 40 ng/mL of rCyr61 could induce an evident increase of
CXCR1/CXCR2 protein in AGS cells. In induction kinetics, the
maximal expression of CXCR1/CXCR2 protein was observed at
8 h and sustained for 24 h of rCyr61 exposure (Fig. 1D, bottom).
The above findings strongly suggest that Cyr61 tightly regulates
the expression of the CXCR1/CXCR2 gene in human gastric
cancer cell lines.
To investigate the clinical significance of Cyr61 and
CXCR1/CXCR2 coexpression in gastric cancer, 20 gastric
cancer specimens (T1-T20) and the four adjacent nontumorous
gastric tissues of gastric cancer patients (N1-N4) were analyzed
by using RT-PCR. A total of 13of 20 (65%; samples T1, T2,
T3, T6, T7, T10, T11, T12, T13, T16, T17, T19, T20) of gastric
tumors showed a considerable amount of Cyr61 mRNA
expression. Among them, about 10 of 13 (77%) had coex-
pressed CXCR1 and/or CXCR2 mRNA. In contrast, Cyr61
level in four normal counterparts is lower than that in most
tumor parts (Fig. 2A).
The coexpression of Cyr61 and CXCR1 and/or CXCR2
protein was further shown by using immunohistochemical
analysis. The representative immunohistochemical staining
(T2 tumor; Fig. 2B) patterns of Cyr61 and CXCR1/CXCR2
from consecutive serial sections were near-identical in gastric
tumor tissues implying highly correlated expression. We also
found that CXCR1 and CXCR2 had strong staining at higher
levels in cancer tissue wherein the expression of Cyr61 was
highly localized, and these proteins were not expressed in the
adjacent normal gastric tissues (Fig. 2B). The CXCR1 or
CXCR2 protein seemed to be predominantly localized in the
membrane of tumor epithelial cells and also expressed in the
cytoplasm. Negative staining for gastric tumors was shown
when immunostaining used an IgG control. Taken collec-
tively, the staining data showed that Cyr61 expression was
tightly correlated with CXCR1 and CXCR2 receptors in
gastric carcinomas, implicating that chemokine receptor
induction by the Cyr61 gene plays a role in gastric cancer
progression.
Involvement of CXCR1/CXCR2 in Cyr61-MediatedChemotactic Migration
To clarify whether CXCR1 and CXCR2 receptors expressed
on Cyr61-overexpressing AGS cells are functional, we
stimulated human gastric cancer cells with recombinant
interleukin-8 (IL-8), a physiologic ligand for both CXCR1
and CXCR2. Binding of chemokines to their receptors produces
a characteristic increase in cytosolic calcium. This is one of the
earliest biochemical events that occur in response to chemo-
kines (34). To examine intracellular calcium flux, we labeled
Cyr61-overexpressing (AGS/Cyr61-C7) cells and control
(AGS/neo) cells with Fluo-3AM before adding chemokine
IL-8. Evaluation of the fluorescence of stimulated cells showed
that only AGS/Cyr61-C7 cells mobilized Ca2+ in response to
IL-8 (Fig. 3A). This result indicated that CXCR1 and CXCR2
expressed in Cyr61-expressing cells were the functional
receptors, which readily responded to its ligand.
We next explored if Cyr61-overexpressing gastric cells use
CXCR1 and CXCR2 to migrate in response to IL-8 by Boyden
chamber analysis. AGS/Cyr61-C7, AGS/Cyr61-mixed pool
(AGS/Cyr61-M), and AGS/neo cells were seeded into the
upper chamber of transwells, and their ability to migrate was
evaluated. The results showed that AGS/neo cells were not
responsive to IL-8, even when they are exposed to a high
concentration of the chemokine (Fig. 3B). A concentration of
30 ng/mL IL-8 was able to support the chemotaxis of AGS/
Cyr61-C7 cells as much as 3-fold over unstimulated cells, and
even low concentrations of the chemokine (10 ng/mL) was
sufficient to induce the Cyr61-overexpressing cells to migrate
more rapidly (Fig. 3B). AGS/Cyr61-C7 and AGS/Cyr61-M
cells did not respond to IL-6 ligand stimulation. These results
suggest that Cyr61-overexpressing cells induce CXCR1 and
CXCR2 expression and result in tumor cell chemotactic
migration in response to specific chemokine IL-8 stimulation.
The exact effect of CXCR1 and CXCR2 overexpression by
the Cyr61 gene on chemotactic migration of tumor cells was
further confirmed using neutralizing antibodies. To this end,
AGS/Cyr61-C7 and AGS/Cyr61-M cells were preincubated
with functional blocking antibodies against CXCR1 (15 Ag/mL)
and/or CXCR2 (15 Ag/mL) and then subjected to the upper
chamber of a transwell. The results showed that treatment
with either anti-CXCR1 or anti-CXCR2 antibody attenuated
Lin et al.
Mol Cancer Res 2007;5(11). November 2007
1114
on April 8, 2020. © 2007 American Association for Cancer Research. mcr.aacrjournals.org Downloaded from

IL-8– induced chemotaxis of Cyr61-expressing cells (either
AGS/Cyr61-C7 or AGS/Cyr61-M) by f40% to 50% and
exhibited over 80% inhibition with cotreatment of anti-CXCR1
and anti-CXCR2 (Fig. 3C). This implies that the chemotactic
activity of Cyr61-overexpressing cells toward IL-8 is function-
ally collaborated by CXCR1 and CXCR2.
To confirm a specific interaction between chemokine
receptors and chemokines in Cyr61-expressing cell migration,
rather than an aspecific interference with the Boyden micro-
chamber assay equipment, similar experiments were done in
the agarose assay (35). In this test system, the distance that cells
migrated toward IL-8 source was used as a variable for
chemotactic potency. Initially, cells lined up at the outer edge of
the center well and then flattened out, as they pushed
themselves underneath the agarose to migrate toward the
chemoattractant IL-8 (Fig. 3D, top). Micrographs taken at
higher magnifications showed that more numbers of cells often
migrated toward the source of the IL-8, and the chemotactic
migration of Cyr61-overexpressing cells was in a time-
dependent manner (Fig. 3D, bottom). Cyr61 cells migrated
toward the IL-8 at a rate of 7.8 Am/h during the first 48 h and
then increasing to f13 Am/h between 48 and 96 h. As a
control, AGS/neo cells migrated randomly and slowly. These
results indicate that overexpression of Cyr61 in gastric cancer
cells greatly and directionally enhances cell migration toward
chemoattractant IL-8.
Cyr61 Overexpression Enhanced Gastric Cancer CellTransendothelial Migration and Intravascular Invasion
Endothelial-derived chemokines, including IL-8, have a role
in attracting tumor cells migrating from a site of attachment to
the endothelium across the vessel wall (35). Indeed, consistent
with other findings (36), human umbilical vascular endothelial
cells (HUVEC) express substantial amounts of IL-8 (data not
shown). To explore whether endothelial-derived IL-8 would
also be a chemoattractant for Cyr61-overexpressing cells, we
have cocultured with tumor cells in the upper chamber and
HUVEC in the lower chamber of transwells. Interestingly, the
migratory potency of Cyr61-overexpressing cells was greatly
increased by 3-fold in the presence of HUVEC compared
with none (Fig. 4A). This endothelium-dependent chemotaxis
of Cyr61-expressing cells was effectively abolished by the
FIGURE 3. Effect of recombinant IL-8 on Cyr61-overexpressing gastric cell chemotaxis. A. AGS/neo and AGS/Cyr61-C7 single clone were labeled withFluo-3AM and exposed to rIL-8 (30 ng/mL) assessed intracellular calcium mobilization. B. Chemotactic migration ability of AGS/neo, AGS/Cyr61-C7, andAGS/Cyr61-M cells by stimulation of rIL-8. IL-6 was used as positive control. Phase micrographs showed crystal violet staining of migration of AGStransfectants. Values were compared with the ability of AGS/neo cells upon no stimulation. C. Inhibition of AGS/Cyr61 cells chemotaxis by neutralizingantibodies against CXCR1 and CXCR2. Cells in the upper chamber were pretreated with IgG, CXCR1, or CXCR2 alone or CXCR1 and CXCR2 antibodies,respectively, and recombinant IL-8 (30 ng/mL) was placed in lower chamber. After migrating for 16 h, values were compared with the ability of AGS/Cyr61-C7and AGS/Cyr61-M cells with no treatment. Columns, mean of three independent experiments; bars, SE. P values of <0.05 were considered statisticallysignificant. D. Time course experiment showing the X (the distance of cells moving to IL-8) and Y (the distance of cells moving to PBS control) migrated byCyr61 transfectants in 96 h. The values of X-Y (E, AGS/Cyr61-7; ., AGS/neo) are as chemotaxis distance. Points, mean; bars, SE. All experiments weredone in triplicate on separate occasions with similar results.
Cyr61 Promotes Invasiveness of Gastric Cancer
Mol Cancer Res 2007;5(11). October 2007
1115
on April 8, 2020. © 2007 American Association for Cancer Research. mcr.aacrjournals.org Downloaded from

addition of blocking antibodies to CXCR1, CXCR2, or IL-8
(Fig. 4A). The above results suggest that IL-8 might be the
important endothelial chemokine responsible for the stimulation
of Cyr61-expressing cell chemotaxis.
Transmigrating across the endothelial barrier in the primary
site is an important step for tumor cell invasion and metastasis.
To assess the role of the Cyr61 gene in transendothelial
migration, we used transwell chambers in which the upper and
bottom wells were separated by a HUVEC monolayer,
depositing calcein AM-labeled AGS/Cyr61 cells on top of a
monolayer of HUVEC. The coculture assay was fixed at 8 h,
and calcein-AM–labeled Cyr61 cells, showing a spreading
morphology under the endothelium, were scored as trans-
migrated cells by fluorescent microscopy. As shown in Fig. 4B,
neutralizing antibodies against CXCR1 and CXCR2 abrogated
transendothelial migration of Cyr61-overexpressing cells (either
AGS/Cyr61-C7 or AGS/Cyr61-M) by 40% to 50%. Treatment
with anti– IL-8 antibody seemed more effective (70-80%
inhibition) in inhibiting transmigration of Cyr61-expressing
cells. In contrast, control IgG had no effect on that (Fig. 4B).
The above results thus confirm the role of CXCR1 and CXCR2
in IL-8–dependent transendothelial migration of Cyr61-
expressing cells.
The ability of Cyr61 overexpression promoting tumor cells
across the endothelial barrier prompts us to investigate whether
Cyr61 could enhance the intravasation of tumor cells in vivo .
To address this, we used a chick embryo chorioallantoic
membrane (CAM) model in which the extent of tumor cells’
intravasation can be determined quantitatively by detection of
human Alu sequence. In a time-related experiment, Cyr61
expressing cells were initially detected at 2 days, steadily
increasing during 3 to 6 days of postinoculation (Fig. 5A). In
contrast, neo control cells were barely detected at 4 days, and
only little amounts appeared at 5 to 6 days of postinoculation
(Fig. 5A). The above results strongly suggest that Cyr61
expression effectively promotes gastric cancer cell intravasation
in a CAM model. Cyr61-expressing cells were pretreated with
neutralizing antibodies against CXCR1 or CXCR2, resulting in
significant inhibition to their intravasation ability (Fig. 5B).
This thus confirms the critical role of CXCR1/CXCR2 in
Cyr61-mediated tumor cell intravasation.
Cyr61-Mediated CXCR1/CXCR2 Up-Regulation andChemotaxis through the PI3K/Akt-Dependent Mechanism
We next studied the possible signaling pathway involved in
CYR61-induced CXCR1 and CXCR2 up-regulation and
chemotactic migration observed above. To this end, we exposed
cells to 40 ng/mL of rCyr61 for varying periods of time and
determined the activated signaling pathways by immunoblot-
ting using their specifically phosphorylated antibodies. As
shown in Fig. 6A, the phosphorylated form of both extracellular
signal-regulated kinase 1 (ERK1)/ERK2 and Akt, but not p38
or phosphorylated c-Jun-NH2-kinase, were evidently increased
after 10 min of treatment of rCyr61 and remained at substantial
levels for >2 h after exposure to rCyr61. These findings are
consistent with earlier studies that have shown the ability of
Cyr61 to strongly activate Akt in other cell systems (28, 37).
To determine the involvement of PI3K/Akt or Erk1/Erk2 in
Cyr61-induced up-regulation of CXCR1/CXCR2, their specific
inhibitors LY294002 and PD98059 were used. Western blot
analysis showed that pretreatment with 40 Amol/L LY294002,
a specific inhibitor of the p110 catalytic subunit of PI3K,
markedly decreased phosphorylation on Ser473 of Akt, as well
as the elevation of CXCR1/CXCR2 induced by Cyr61 (Fig. 6B,
top). In contrast, 25 Amol/L PD98059, a specific inhibitor of
ERK, completely abolished Erk1/Erk2 phosphorylation in
the absence of rCyr61, but failed to affect CXCR1/CXCR2
up-regulation in response to rCyr61 (Fig. 6B, bottom). To
further confirm that Akt, the downstream of PI3K, was indeed
involved in the Cyr61-induced elevation of CXCR1 and
CXCR2, we stably transfected a kinase-defective mutant of
Akt (Akt 179A), which can inhibit wild-type Akt in a
dominant-negative fashion (38), followed by stimulation of
40 ng/mL rCyr61. Western blot analysis revealed that stable
expression of dominant-negative Akt in AGS cells resulted in a
FIGURE 4. Effect of IL-8 secreted from the conditioned endothelialmedium on transendothelial migration of Cyr61-overexpressing gastriccell. A. HUVEC cells were cocultured in lower chamber of Boydentranswell, and the conditioned medium was incubated with the absence orpresence of anti – IL-8 (10 Ag/mL) blocking antibody. AGS/Cyr61-7 cells(2.5 � 104) pretreated with CXCR1 (30 Ag/mL) or CXCR2 (30 Ag/mL)antibodies, respectively, were then seeded in the upper chamber allowedto migrate for 16 h. Values were compared with the ability of AGS/Cyr61cells in the upper chamber without HUVEC cocultured condition. B.The inhibitory effects of CXCR1 and CXCR2 neutralizing antibodies onAGS/Cyr61 cell transendothelial migration. Endothelial cells were fullyconfluence preseeded in the upper chamber of transwell overnight; AGS/Cyr61-C7 and AGS/Cyr61-M cells were incubated above the HUVEC layerand allowed to transendothelial migrate with the CXCR1, CXCR2, orIL-8 blocking antibodies for 20 h. IgG treatment was used as control.Values were compared with the ability of AGS/CYR61 cells in the absenceof antibody treatment. Each was placed in triplicate in experiment.Columns, mean; bars, SE. P values of <0.05 were considered statisticallysignificant.
Lin et al.
Mol Cancer Res 2007;5(11). November 2007
1116
on April 8, 2020. © 2007 American Association for Cancer Research. mcr.aacrjournals.org Downloaded from

decrease in the rCyr61-stimulated increased level of CXCR1
and CXCR2 (Fig. 6C). Subsequently, we explored whether
PI3K/Akt pathway is involved in the Cyr61-induced IL-8–
dependent chemotaxis. Figure 6D reveals that 20 to 40 Amol/L
of LY294002 led to a dose-dependent inhibition of the IL-8–
induced chemotactic migration of AGS cells by stimulation of
rCyr61. Furthermore, the Erk inhibitor PD98059 had no
significant effect on Cyr61-induced chemotaxis toward IL-8.
The above results thus suggest that PI3k/Akt signaling pathway
is critically involved in Cyr61-mediated CXCR1/CXCR2 up-
regulation and chemotactic migration.
Integrin and Src Act as Upstream Regulator in the Up-Regulation of CXCR1 and CXCR2
It is well known that Cyr61 protein interacts with various
integrin receptors, such as avh3, avh5, a6h1, to transducer
downstream signaling cascades (39-41). Therefore, we want to
determine whether integrin receptor is necessary for Cyr61–up-
regulated CXCR1/CXCR2 expression. As shown in Fig. 7A,
Cyr61-induced CXCR1 and CXCR2 elevation is strongly
reduced by functional neutralizing antiintegrin avh3 antibody,
but not anti-a2h1 antibody, indicating a vital role of integrin
avh3 in Cyr61-induced expression of IL-8 receptors in human
AGS cells.
Integrins transmit signals directly through Src families (42),
the consequent downstream signals, especially via the mitogen-
activated protein kinase, and PI3K transduction cascades are
critical for regulation of biological activities. To address
whether c-Src is activated by CYR61 gene expression and that
it participates in CXCR1 and CXCR2 induction, we treated
AGS cells with rCYR61 (40 ng/mL) and did Western blot
analysis. The result showed that c-Src phosphorylation at Tyr416
was found at 10 min after rCYR61 stimulation, decreasing at
24 h (Fig. 7B, top). We also observed that c-Src and Akt
kinases phosphorylation decreased by inhibition of integrin
avh3 activity in the presence of rCyr61 (Fig. 7B, bottom),
implicating Cyr61 via binding to the integrin receptor
modulated Src and Akt activity. Moreover, to further examine
whether Src kinase is required for enhanced CXCR1 and
CXCR2 expression in Cyr61-overexpressing cancer cells, we
used a Src-specific inhibitor, PP1, to block c-Src phosphory-
lation. It was found that blockage of Src activity by PP1 led to
inhibition of the Cyr61-induced CXCR1 and CXCR2 expres-
sion, and Akt phosphorylation. We further confirmed the role
of Src in CXCR1 and CXCR2 up-regulation by dominant-
negative Src kinase. As expected, CXCR1 and CXCR2
expression were reduced by transfection with dominant-
negative Src of AGS cells (Fig. 7D). In addition, the chemo-
taxis activity was significantly decreased to a level compared
with that of the negative control untreated cells with treatment
of PP1 (Fig. 7E). Taken together, these results show that
integrin avh3/Src/PI3k/Akt pathway critically contributes to
Cyr61-induced CXCR1 and CXCR2 expression, as well as
IL-8–dependent chemotaxis and intravasation.
DiscussionAccumulating studies have shown that Cyr61 plays a
pleiotropic role and is substantially involved in the develop-
ment and progression of human malignancies, such as
melanomas, gliomas, and carcinomas of the lung, breast,
prostate, and bladder (28, 31, 37, 43-45). Our recent work also
showed that patients with gastric adenocarcinoma displayed
high expression of Cyr61, whose level was positively correlated
with aggressive lymph node metastasis, more advanced tumor
stage, and early recurrence (30), enforcing expression of Cyr61
in AGS gastric cells and directly promoting cell motility and
invasiveness. In this report, we further show that enforced
expression or treatment with Cyr61 increases chemokine
receptors CXCR1 and CXCR2 expression and promotes gastric
cancer cell migration toward CXCR1/CXCR2 native ligand,
IL-8. In addition, Cyr61-expressing cells have greater potency
FIGURE 5. Effects of CXCR1 and CXCR2 on Cyr61-overexpressinggastric cancer cells spontaneously intravasation in the chick embryomodel. A. Detection and quantitation of Cyr61-overexpressing AGS cellsspontaneous metastasis in CAM assay. The 106 cells were suspended inserum-free RPMI medium in upper CAM chamber and allowed tointravasate for 1 to 6 d. Top, PCR amplification of Alu sequences in themixture of human and chicken extracted CAM DNA from lower CAM.Bottom, the quantitation data of upper PCR amplification result. B. AGS/neo and AGS/Cyr61-7 cells were incubated with neutralizing antibodiesagainst CXCR1 (30 Ag/mL), CXCR2 (30 Ag/mL), or control IgG in theupper CAM of the chicken embryo for 4 d. The human and chicken CAMDNAs from lower CAM were extracted and assessed by relative fold ofDNA density compared with AGS/neo cells upon no stimulation. No tumorcells seeded chamber extracted DNA is used as negative control.
Cyr61 Promotes Invasiveness of Gastric Cancer
Mol Cancer Res 2007;5(11). October 2007
1117
on April 8, 2020. © 2007 American Association for Cancer Research. mcr.aacrjournals.org Downloaded from

in transendothelial migration and intravasation in vitro
compared with neo control cells. Blockage of CXCR1/CXCR2
by their specific neutralizing antibodies strongly impairs
Cyr61-mediated chemotaxis, transendothelial migration,
and intravasation. Supportively, immunohistochemical serial
section staining or RT-PCR in gastric tumor specimens revealed
that an evident correlation exists between the level of Cyr61
and CXCR1/CXCR2 receptor expression. Together, our
current data, for the first time, highlights a new function of
Cyr61 involved in promoting IL-8–dependent chemotaxis,
transendothelial migratioin, and intravasation via concomitant
up-regulation of functional CXCR1/CXCR2 in gastric cancer
cells.
CXCR1 and CXCR2 receptors are members of the seven-
transmembrane spanning, G protein–coupled receptor family.
CXCR1 and CXCR2 show a 77% overall sequence identity to
each other (9). Their transmembrane regions and intracellular
loops are highly similar, whereas the amino- and carboxyl-
terminal regions show striking differences. Both receptors are
expressed on polymorphonuclear neutrophil granulocyte
through ligand binding activation to regulate immune cell
migration. However, many clinical studies have revealed that
various carcinomas express both IL-8 receptors CXCR1 and
CXCR2 on the surface of human carcinoma cells by
immunohistochemical analysis, such as breast, colon, gastric,
pancreatic, and head and neck squamous carcinomas (18, 19,
46-48), suggesting an important role in tumor development
or progression. Recent studies reported that high levels of
expression of CXCR1, CXCR2, and CCR7 were found in
gastric cancer cells involved with carcinoma invasion and
metastasis (32, 47, 49). Among these chemokine receptors,
CCR7 played a role in metastasis of lymphoid organs by gastric
cancer cells (49), and the most abundant expression of both
chemokines CCL21/CCL6 and CCL19/ECL had been found in
the lymph nodes (7, 50). In contrast, the actual role of CXCR1/
CXCR2 in gastric cancer invasion and metastasis has yet to
be defined. Tumor-endothelial cell interaction is important for
tumor invasion and metastasis (51, 52), and transendothelial
FIGURE 6. Cyr61 overexpression activates PI3K signaling involved with CXCR1 and CXCR2 up-regulation. A. Phosphorylated Akt and ERK42/ERK44and p38 c-Jun-NH2-kinase (JNK) protein expression levels in rCyr61 treatment (40 ng/mL) for indicated time. Total cell lysates was collected, and 40 Agprotein were subjected to electrophoresis on 10% SDS-PAGE and transferred to polyvinylidene difluoride membranes. Immunoblots with anti –phosphorylated Akt, anti – phosphorylated ERK, anti –phosphorylated c-Jun-NH2-kinase, and anti-p38 show equivalent amounts of the proteins in eachextract. Blots were reprobed with antibodies for Akt and ERK to control for protein loading and transfer. B. Overnight serum-starved cells at 75% to 80%confluence were treated 1 h with vehicle, LY294002 or PD98059, followed by treatment with 40 ng/mL rCyr61 for 1 h. Total protein (40 Ag) was resolved bySDS-PAGE and subjected to immunoblot analysis for phosphorylated Akt (top ), phosphorylated ERK42/ERK44 (bottom ), CXCR1, and CXCR2. Blots werereprobed with antibody for Akt, ERK42/ERK44. a-Tubulin was used to control protein loading and equal transfer. C. AGS cells were transiently transfectedwith dominant-negative Akt (DN-Akt) or control vector pcDNA3 and then treated with 40 ng/mL rCYR61 for 8 h. CXCR1 and CXCR2 protein expression weredetermined by Western blot analysis. Results are representative of three independent experiments. D. AGS cells were incubated with the indicatedconcentrations of LY294002 or PD98059 and treated with IL-8 (30 ng/mL) and then subjected to chemotaxis. The experiments were done in triplicates.Columns, mean; bars, SE. P values of <0.05 were considered statistically significant.
Lin et al.
Mol Cancer Res 2007;5(11). November 2007
1118
on April 8, 2020. © 2007 American Association for Cancer Research. mcr.aacrjournals.org Downloaded from

migration is a key event in cancer hematogenous metastasis
(53). In the present study, we used specific neutralizing anti-
bodies against CXCR1 or CXCR2 that effectively blocked
Cyr61-overexpressing gastric cancer cell chemotactic migration
and intravasation in vitro . Therefore, we suggest that the
expression of chemokine receptors CXCR1 and CXCR2 on
gastric carcinoma cells may facilitate their hematogenous
metastasis. Consistent with our observations and notions,
Ramjeesingh et al. also showed CXCR1-overexpressing mela-
noma cells exhibiting enhanced activity in chemotaxis and
transendothelial migration toward endothelial-derived IL-8 (35).
Our current studies further suggest that organ specificity of
certain tumor metastases might depend on both the types of
chemokines secreted by the host endothelium or organ and the
expression pattern of chemokine receptors on the cancer cell.
Limited studies have focused on the regulatory mechanism
of chemokine receptors in tumor cells. Here, we show that
integrin avh3 acts as an innate receptor for Cyr61 protein to
transduce signaling for up-regulating CXCR1/CXCR2 mRNA
in gastric cancer cells. Actually, most of the Cyr61-promoted
effects, including cell adhesion, migration, and differentiation,
are mediated via its direct binding with the integrin receptor
avh3 (28, 40, 54, 55), which has been implicated in the
pathophysiology of malignant tumors. In addition, the level of
integrin avh3 is generally up-regulated in invasive tumors and
distant metastases in a wide variety of cancers (56). Our
FIGURE 7. Integrin and Src signaling activation involved with Cyr61-induced CXCR1 and CXCR2 expression. A. Cells at 75% to 80% confluence werepretreated with integrin avh3, a2h1 neutralizing antibody or control IgG for 1 h and treated with 40 ng/mL rCyr61. Total protein (40 Ag) was resolved by SDS-PAGE and subjected to immunoblot analysis for CXCR1 and CXCR2. Blots were reprobed with antibody for a-tubulin to control protein loading and equaltransfer. Results are representative of three independent experiments. B. Top, AGS cells were treated with 40 ng/mL of rCyr61 for indicated time.Immunoblots with anti –phosphorylated c-Src show equivalent amounts of the proteins in each extract. Blots were reprobed with an antibody for anti – c-Src tocontrol protein loading and transfer. Bottom, cells were pretreated neutralizing antibody against integrinavh3, a2h1 (10 Ag) and control IgG for 1 h, and thentreated with 40 ng/mL rCyr61. Total protein was resolved by SDS-PAGE and subjected to immunoblot analysis for phosphorylated Akt and phosphorylatedSrc. Blots were reprobed with antibody for Akt and Src to control protein loading and equal transfer. Results are representative of three independentexperiments. C. AGS cells were treated with vehicle PP1 for 1 h after treatment with 40 ng/mL rCyr61. Total protein was resolved by SDS-PAGE andsubjected to immunoblot analysis for phosphorylated c-Src, phosphorylated Akt, CXCR1, and CXCR2. D. AGS cells were transiently transfected withdominant-negative Src (DN-Src) or vector control pcDNA3 and then treated with rCyr61 for 8 h. CXCR1 and CXCR2 expression and Src and Aktphosphorylation were determined by Western blot analysis. Blots were reprobed with antibody for Src, Akt, and a-tubulin to control protein loading and equaltransfer. E. AGS cells were incubated with the indicated concentrations of Src protein inhibitor, PP1, and treated with IL-8 (30 ng/mL). The experiments weredone in triplicates. Columns, mean; bars, SE. P values of <0.05 were considered statistically significant.
Cyr61 Promotes Invasiveness of Gastric Cancer
Mol Cancer Res 2007;5(11). October 2007
1119
on April 8, 2020. © 2007 American Association for Cancer Research. mcr.aacrjournals.org Downloaded from

unpublished data shows that the chemokine receptors CXCR1/
CXCR2 were colocalized with integrin avh3 on the membrane
of Cyr61-overexpressing cells (data not shown). This suggests
that Cyr61-mediated chemotaxis and transendothelial migration
may be through coordination between CXCR1/CXCR2 and
integrin avh3. These findings are clearly relevant to previous
studies published by Babic et al., showing Cyr61 could induce
vascular endothelial cells chemotaxis through avh3-dependentpathway (57). However, how the CXCR1/CXCR2 and integrin
avh3 cooperate with each other to facilitate Cyr61-expressing
cells’ transendothelial migration needs further investigation.
Integrins might transmit signals through the activation of the
ERK42/ERK44 mitogen-activated protein kinase and PI3K/Akt
pathway (42). In the present study, we showed that Cyr61
elicited the activation of PI3k/Akt and Erk1/Erk2, but not p38,
signaling pathways. Indeed, the fact that Cyr61 can activate
both pathways is commonly observed in different kinds of cells
(28, 37). Utilization of pharmacologic inhibitors and genetic
inference shows that the PI3K/Akt, but not Erk1/Erk2, pathway
is required for Cyr61-induced CXCR1/CXCR2 up-regulation
and subsequent chemotaxis. We further found that c-Src was
necessary for Cyr61-induced PI3K/Akt activation and CXCR1/
CXCR2 production. c-Src belongs to the Src family of tyrosine
kinases, which represent important transducers during integrin-
mediated signaling. It has been reported that Src family of
tyrosine kinases are associated with the integrin avh3 and are
activated after integrin ligation in multiple cell types, including
osteoclasts (58), melanoma cells (59), and platelets (60). Src
family of tyrosine kinases are associated with avh3 integrins
through an interaction with the C terminus of the h3 subunit.
The C terminus, including the NITY motif, is unique to the h3
integrin subunit, which may explain the specificity of the
interaction of c-Src with h3 tails, but not h1 or h2 tails (61).
c-Src has been shown to directly phosphorylate many
downstream proteins, including FAK, Cas, paxillin, mitogen-
activated protein kinase, and PI3k-Akt signaling. This was
consistent with our findings that detailed signaling cascade
from integrin avh3 to CXCR1/CXCR2 induction was mediated
by Src kinase and its downstream PI3k-Akt pathway.
In conclusion, we, for the first time, showed that over-
expression of Cyr61 induced functional CXCR1 and CXCR2
receptors that play an important role in chemotactic migration
of human AGS cells toward IL-8. Under such a scenario,
Cyr61-expressing cells exhibited stronger potency in trans-
endothelial migration and intravasation in a CAM model via
a CXCR1/CXCR2-dependent mechanism. Collectively, our
current findings suggest that Cyr61 is possibly involved in
hematogenous invasion and metastasis of human gastric
adenocarcinoma. It also implicates that targeting Cyr61 or
CXCR1/CXCR2 in this disease may be an effective therapeutic
strategy in inhibiting the dissemination of gastric cancer after
local surgical control.
Materials and MethodsAntibodies and Reagents
Anti-CXCR1, CXCR2, and IL-8 monoclonal antibodies
were from R&D Systems; anti-CYR61 polyclonal antibody,
anti–phosphorylated Akt1/Akt2/Akt3 (Ser473)-R antibody,
anti–Akt-1 antibody, anti–phosphorylated ERK1/ERK2 anti-
body, anti-ERK1/ERK2 antibody, anti –phosphorylated Src
antibody, anti-Src antibody, anti–phosphoryalted p38 antibody,
and anti–phosphorylated c-Jun-NH2-kinase antibody were
obtained from Santa Cruz Biotechnology; anti–h-actin anti-
body and anti–a-tubulin antibody, LY294002, and PD98059
were from Sigma. Function-blocking antibody against avh3(LM609); a2h1 was purchased from Chemicon; Cyr61
neutralizing antibodies are a kind gift from Dr. Lester F.
Lau, and they do not cross-react with Fisp12/connective tissue
growth factor (57). Recombinant human IL-8 was purchased
from R&D Systems, and recombinant human Cyr61 was
purchased from Abnova Corporation. [a-32P]dCTP was
obtained from Amersham Biosciences (Amersham International).
Cell Cultures and Tumor SamplesAGS, N87, MKN45, and TSGH human gastric adenocarci-
noma cell lines were obtained from American Type Culture
Collection. All gastric carcinoma cell lines were grown in
RPMI 1640 (Invitrogen Corp.). HUVEC were isolated from
two to five umbilical cord veins, pooled, and established as
primary cultures in M199 containing 20% fetal bovine serum
(62). The surgical samples were obtained from the Department
of Surgery, National Taiwan University Hospital.
Transient Transfection and Established Stable ClonesThe expression vector CYR61 was constructed by placing
human CYR61 cDNA in the pcDNA3.1 eukaryotic expression
vector containing the neomycin gene under the control of the
same promoter. The CYR61-sense expression constructs were
transfected into AGS cells or CYR61-antisense constructs into
MKN45 cells using TransFast liposome (Promega). At 24 h
after transfection, the cells were serum-starved for 16 h and
lysed for analysis for transient transfection. Stable cell popu-
lations were selected by 0.8 mg/mL gentamicin (Invitrogen
Corp.). After G418 selection, we isolated one single clone,
AGS/Cyr61-C7, and a pool mixture, AGS/Cyr61-M.
Collection of Conditioned MediumAt full growth of cell, 90% of the confluence medium were
removed, and cells were washed and then incubated in serum-
free medium for 24 h. Conditioned medium was collected and
centrifuged to remove any cellular contaminants. Immunopre-
cipitation analysis was used to deplete CYR61 protein that
existed in conditioned medium. Goat anti-CYR61 antibody
(10 Ag/mL) was added, the samples were rotated at 4jC over-
night, and then protein A–Sepharose (Amersham Pharmacia;
30 AL of a 50% slurry) was added for 2 h. Followed by
centrifugation for 20 min at 14,000 rpm, the supernatant was
collected as conditioned medium that depleted CYR61.
RNA Isolation and RT-PCRTotal cellular RNA was isolated from gastric carcinoma cell
lines and patient tissue by using RNA TRIzol reagent
(Invitrogen Corp.) using the manufacturer’s directions. cDNA
was synthesized using total RNA (5 Ag) with Moloney murine
leukemia virus reverse transcriptase and random hexamers
(Promega). The reaction mixture was incubated at 37jC for
2 h and was terminated by heating at 95jC for 5 min. The
Lin et al.
Mol Cancer Res 2007;5(11). November 2007
1120
on April 8, 2020. © 2007 American Association for Cancer Research. mcr.aacrjournals.org Downloaded from

primer sequences for PCR are as follows: CYR61, 5¶-CGAGG-TGGAGTTGACGAG AAAC-3¶ (F) and 5¶-AGGACTGGA-TATCATGACGTTCT-3 ¶ (R); CXCR1, 5 ¶-GCCACCT-
GCAGATGAAGATT-3¶ (F) and 5¶-CAGCAGCCAAGA-
CAAACAAA-3¶ (R); CXCR2, 5¶-GTGAACCAGAATCCCTG-GAA-3¶ (F) and 5¶-AGACGCTCCTTCGGAAAAGT-3¶ (R);
CXCR4, 5¶-AATCTTCCTGCCCACCATCT-3¶ (F) and 5-GAC-
GCCAACATAGACCACCT-3¶ (R); CCR7, 5¶-ACATCGGAGACAACACCACA-3 ¶ (F) and 5 ¶-CATGCCACTGAAG
AAGCTCA-3 ¶ (R); CCR10, 5 ¶-GGGTTTCTCCTT-
CCACTCCT-3¶ (F) and 5-TATTCCCCACATCCTCCTTG-3¶(R); h-actin, 5¶-GATGATGATATCGCCGCGCT-3¶ (F) and
5-TGGGTCATCTTCTCGCGGTT-3¶ (R). Primers were used
at a final concentration of 0.5 Amol/L, and the thermal cycling
conditions were as follows: 5 min at 95jC, followed by 32
cycles of 95jC for 60 s, 55jC for 60 s for CYR61 and h-actinor 55jC for 60 s for chemokine receptor genes, and finally
72jC for 60 s. The reactions were done in a Biometra Ther-
maoblock (Biometra, Inc.). PCR products were separated on a
1.2% agarose gel containing ethidium bromide (0.5 Ag/mL),
visualized, and photographed, and relative intensity of the
specific gene expression was determined using the Alpha-
Image Analysis System (Alpha Innotech).
Western Blot AnalysisCells were harvested, lysed in radioimmunoprecipitation
assay buffer [50 mmol/L Tris-HCl (pH 7.4), 150 mmol/L NaCl,
1% Triton X-100, 10% glycerol, 0.25% Na-deoxycholate, 1%
Nonidt P-40, 1 mmol/L EDTA, 1 mmol/L EGTA, 50 mmol/L
Na3VO4, 1 mol/L NaF, 50 mmol/L phenylmethylsulfonyl
fluoride, 1 Ag/mL leupeptin, and 1 Ag/mL aprotinin] for
20 min on ice, and clarified by centrifugation at 14,000 rpm for
20 min at 4jC, and the supernatant was collected. Equal
amounts of protein were loaded onto 10% gradient SDS poly-
acrylamide gel separated and electrotransferred onto polyviny-
lidene difluoride membrane (Immobilon-P membranes;
Millipore Corp.). The protein blot in the membrane was
blocked with 5% skim milk in PBS containing 0.1% Tween 20
(Sigma Chemical Co.), PBS-T, for 1 h at room temperature.
Primary antibodies as indicated were incubated with mem-
branes for 4jC overnight, and the membranes were washed in
PBS-T thrice, probed with horseradish peroxidase–conjugated
secondary antibodies (Santa Cruz Biotechnology) for 1 h
(1:5,000 dilution in PBS-T), and then washed thrice with
PBS-T. The antibody-bound protein bands were detected with
enhanced chemiluminescence reagent (Amersham Pharmacia
Biotech) and photographed with Kodak X-Omat Blue autora-
diography film (Perkin-Elmer Life Sciences).
Under-Agarose Cell Migration AssayA 2% (w/v) agarose solution in RPMI 1640 was mixed with
an equal volume of complete RPMI medium containing 1%
(w/v) bovine serum albumin (Sigma Chemical Co.). An aliquot
of this mixture (900 AL) was placed in six-well tissue culture
plates and allowed to solidify for 1 h at 4jC. Three holes werepunctured at equal distances apart in the agarose sheet by using
a hole puncher. AGS/CYR61-7 and AGS/neo gastric cells were
collected from culture dishes using 4 mmol/L EDTA in HBSS
and resuspended at a concentration of 3.33 � 105 cells per
milliliter. Gastric cells (2 � 103 in 6 AL) were placed in the
middle hole, recombinant IL-8 chemoattractant (30 ng/3 AL)was placed in the left hole, and control buffer (fresh medium)
was placed in the right hole. Solutions in all three holes were
replenished every 12 h. Cells were allowed to migrate under the
agarose sheet for 96 h in an incubator at 37jC and were then
fixed with 4% paraformaldehyde for 1 h. Coverslips were
stained with 0.5% crystal violet (Sigma) for 15 min and then
washed with PBS for visualization under a light microscope
(Leica Microsystems, type 090-135.001). The distance of
chemotactic migration was determined by subtracting migration
toward the chemoattractant (X) and random movement (Y)
toward the fresh medium or control buffer. The value of X-Y
was used as chemotaxis. Each experiment was done in
triplicates.
Transwell Chemotaxis AssayChemotaxis assays were done using modified Boyden
chambers with filter inserts for 24-well dishes containing
8-Am pores (6.5 mm; Corning Costar Corp.). The upper
compartment of the culture insert was coated with 1% gelatin
solution insert. A total of 900 AL of RPMI supplemented with
10% FBS and 10 or 30 ng/mL recombinant IL-8 (R&D
Systems, Inc.) was added to the lower chamber of the transwell
in a 24-well plate or coculture HUVEC grown 100%
confluence in the absence or presence of IL-8 neutralizing
antibody in the lower chamber. AGS/CYR61-C7, AGS/
CYR61-M, or AGS/neo cells (2.5 � 104 in 100 AL medium),
with or without pretreatment with neutralizing antibodies
against CXCR1 or CXCR2, were deposited into the upper
chamber and allowed to migrate for 16 h at 37jC in an
incubator. Cells on the upper side of the filters were removed
with cotton-tipped swabs, and the filters were washed in PBS,
fixed with 4% paraformaldehyde for 15 min, and were then
stained with 0.05% crystal violet for visualization under a light
microscope (type 090-135.001, Lieca Microsystems). The
number of cells in each lower chamber/40� field was
quantitated by counting five random fields.
Transendothelial Migration AssayAGS/CYR61-C7, AGS/CYR61-M, and AGS/neo trans-
fectant cells were labeled with calcein AM (Molecular Probes)
4 Ag/mL at 37jC for 90 min in calcein-labeling buffer. Cells
were then washed twice with HBSS and resuspended. Calcein
AM–labeled cells (2.5 � 104) were added to confluent
HUVEC-coated wells in the upper chamber of the transwell,
incubated with medium alone or medium containing neutral-
izing antibody, and then allowed to migrate for 20 h at 37jC in
an incubator. Nonadherent cells were removed by washing
HBSS thrice, and cells on the upper side of the filters were
removed with cotton-tipped swabs. The fluorescence was
quantitated with Millipore fluorescence plate reader (Millipore
Corp.) using an excitation wavelength of 485 nm and an
emission wavelength of 530 nm.
Chicken Embryo Metastasis AssayThis assay was modified by Zijlstra et al. (63), which was
used to study the intravasation ability of cancer cells. Fertilized
White Leghorn eggs were incubated in a rotary incubator at
Cyr61 Promotes Invasiveness of Gastric Cancer
Mol Cancer Res 2007;5(11). October 2007
1121
on April 8, 2020. © 2007 American Association for Cancer Research. mcr.aacrjournals.org Downloaded from

38jC with 60% humidity for 10 days. At this time, the CAM
was dropped by drilling a small hole through the eggshell into
the air sac and a second hole near the allantoic vein that
penetrates the eggshell membrane but not the CAM. Subse-
quently, a cutoff wheel was used to cut a square window
(1 cm2) encompassing the second hole near the allantoic vein to
expose the underlying CAM. After delivering 1 � 106 cells in
15 AL serum-free RPMI into the CAM windows, an artificial air
sac was subsequently created (‘‘upper CAM’’) then sealed, and
the eggs were returned to a stationary incubator. After 1 to
6 days of incubation, the lower half of the CAM (‘‘lower
CAM’’) was correlated and placed in a sterile 15-mL
polypropylene tube; the tissue was snap-frozen in liquid
nitrogen and stored frozen at �80jC. The frozen tissue was
analyzed for the presence of tumor cells by quantitative alu
PCR as described below. The two sections of the lower CAM
were combined, and genomic DNA was extracted from these
tissues using the Puregene DNA purification system (Gentra
System) according to the manufacturer’s specifications. To
detect human cells in the chick tissues, primers specific for
the human alu repeat sequence [5¶-ACGCCTGTAATCCCAG-CACTT-3¶ (F), 5¶-TCGCCCAGGCTGGAGTGC-3¶ (R)], whichproduced a band of 219 bp, were used to amplify the human alu
repeats present in genomic DNA that was extracted from chick
tissues. The PCR reaction mixture contained 1 Ag of genomic
DNA as template and was done under the following conditions:
polymerase activation at 95jC for 10 min followed by 36
cycles at 95jC for 30 s, 52jC for 30 s, and 72jC for 30 s. A
quantitative measure of amplifiable chick DNA as control was
obtained through amplification of the chick glyceraldehyde-3-
phosphate dehydrogenase genomic DNA sequence with
chGAPDH primers [5’-GAGGAAAGGTCGCCTGGTGGA-
TCG-3¶ (F), 5¶-GGTGAGGACAAGCAGTGAGGAACG-3¶(R)] using the same PCR conditions described for alu .
Ca2+ MobilizationCells were detached from the substratum with 2 mmol/L
EDTA/PBS (minus Ca2+ and Mg2+), washed twice with PBS,
then loaded with Fluo-3AM (Molecular Probes) for 30 min,
and warmed to 37jC before flow cytometry analysis. The
fluorescence intensity was followed kinetically after addition
of IL-8 (30 ng/mL) on a flow cytometer. Fluorescence-
activated cell sorting was done using a FACScan (Becton
Dickinson), and analysis was done using CellQuest 2.0
(Becton Dickinson).
Immunohistochemical AnalysisFormalin-fixed tissue sections were deparaffinized and
treated with proteinase K, whereas tissue sections were treated
with 0.01 mol/L citrate buffer followed by exposure to
microwaves (3 � 5 min). The sections were immersed for
30 min in 0.3% H2O2 in absolute methanol and then treated
with 5% fetal bovine serum for blocking nonspecific binding
sites at room temperature for 1 h. Overnight incubation with the
antihuman CYR61 polyclonal (Santa Cruz), CXCR1 monoclo-
nal (R&D Systems), CXCR2 monoclonal antibodies (R&D
Systems) at 1:100 dilution was followed by incubation with
biotinylated mouse anti-goat IgG or rabbit anti-mouse IgG and
biotin-streptavidin-peroxidase (Super Sensitive Multilink HRP
Detection System, Bio Genex) reaction that used 3,3¶-diaminobenzidine tetrahydrochloride solution as substrate.
Color reaction was developed in diaminobenzidine solution,
and counterstaining was done with Mayer’s hematoxylin
solution.
StatisticsFor statistical analysis, P values were based on two-sided,
parametric Student’s t tests using Excel software from Micro-
soft. A P value of <0.05 on the basis of at least three
independent sets of experiments was considered to be
statistically significant. The significance of the differences in
the CYR61 gene between CXCR1 or CXCR2 was analyzed
using the m2 test. Pearson correlation coefficients were obtained
using SAS software (Release 6.12; SAS Institute, Inc.).
References1. Parkin DM, Bray F, Ferlay J, Pisani P. Estimating the world cancer burden:Globocan 2000. Int J Cancer 2001;94:153–6.
2. Parkin DM, Pisani P, Ferlay J. Estimates of the worldwide incidence of 25major cancers in 1990. Int J Cancer 1999;80:827–41.
3. Oliveira FJ, Ferrao H, Furtado E, et al. Early gastric cancer: report of 58 cases.Gastric Cancer 1998;1:51 – 6.
4. Lin MT, Kung SP, Yeh SL, et al. The effect of glutamine-supplemented totalparenteral nutrition on nitrogen economy depends on severity of diseases insurgical patients. Clin Nutr 2002;21:213–8.
5. Lin MT, Chou TH, Lai PS, et al. A New Surgical Technique: Mini-invasivesurgery for radical subtotal gastrectomy by gasless laparoscopy-assist for earlycancer. Hepatogastroenterology 2006;53:843– 4.
6. Chambers AF, Groom AC, MacDonald IC. Dissemination and growth ofcancer cells in metastatic sites. Nat Rev Cancer 2002;2:563 –72.
7. Muller A, Homey B, Soto H, et al. Involvement of chemokine receptors inbreast cancer metastasis. Nature 2001;410:50–6.
8. Murphy PM. Chemokines and molecular basis of cancer metastasis. N Engl JMed 2001;354:833 –5.
9. Lee J, Horuk R, Rice GC, et al. Characterization of two high affinity humaninterleukin-8 receptors. J Biol Chem 1992;267:16283– 7.
10. Campbell JJ, Butcher EC. Chemokines in tissue-specific and microenviron-ment-specific lymphocyte homing. Curr Opin Immunol 2000;12:336–41.
11. Zlotnik A, Yoshie O. Chemokines: a new classification system and their rolein immunity. Immunity 2000;12:121–7.
12. Sun YX, Wang J, Shelburne CE, et al. Expression of CXCR4 and CXCL12(SDF-1) in human prostate cancers (PCa) in vivo . Cell Biochem 2003;89:462 –73.
13. Scotton CJ, Wilson JL, Milliken D, et. al. Epithelial cancer cell migration: arole for chemokine receptors. Cancer Res 2001;61:4961–5.
14. Geminder H, Sagi-Assif O, Goldberg L, et al. A possible role for CXCR4 andits ligand, the CXC chemokine stromal cell-derived factor-1, in the development ofbone marrow metastases in neuroblastoma. J Immunol 2001;167:4747 –57.
15. Juarez J, Bendall L. SDF-1 and CXCR4 in normal and malignanthematopoiesis. Histol Histopathol 2004;19:299– 309.
16. Balkwill F. Cancer and the chemokine network. Nat Rev Cancer 2004;4:540 –50.
17. Murphy C, McGurk M, Pettigrew J, et al. Nonapical and cytoplasmicexpression of interleukin-8, CXCR1, and CXCR2 correlates with cell proliferationand microvessel density in prostate cancer. Clin Cancer Res 2005;11:4117–27.
18. Varney ML, Li A, Dave BJ, et al. Expression of CXCR1 and CXCR2receptors in malignant melanoma with different metastatic potential and their rolein interleukin-8(CXCL-8)-mediated modulation of metastatic phenotype. ClinExp Metastasis 2003;20:723–31.
19. Kuwada Y, Sasaki T, Morinaka K, et al. Potential involvement of IL-8 andits receptors in the invasiveness of pancreatic cancer cells. Int J Oncol 2003;22:765 –71.
20. Li A, Varney ML, Singh RK. Expression of interleukin 8 and its receptors inhuman colon carcinoma cells with different metastatic potentials. Clin Cancer Res2001;7:3298–304.
Lin et al.
Mol Cancer Res 2007;5(11). November 2007
1122
on April 8, 2020. © 2007 American Association for Cancer Research. mcr.aacrjournals.org Downloaded from

21. Lau LF, Nathans D. Identification of a set of genes expressed during the G0/G1transition of cultured mouse cells. EMBO J 1985;4:3145–51.
22. Brigstock DR. The connective tissue growth factor/cycteine-rich 61/nephroblastoma overexpressed (CCN) family. Endocr Rev 1999;20:189–206.
23. Brigstock DR. The CCN family: a new stimulus package. J Endocrinol 2003;178:169 –75.
24. Lau LF, Lam SC. The CCN family of angiogenic regulators: the integrinconnection. Exp Cell Res 1999;248:44–57.
25. Perbal B. CCN proteins: multifunctional signaling regulators. Lancet 2004;363:62 –4.
26. Kireeva ML, Mo FE, Yang GP, et al. Cyr61, a product of a growth factor-inducible immediate-early gene, promotes cell proliferation, migration, andadhesion. Mol Cell Biol 1996;16:1326– 34.
27. Xie D, Nakachi K, Wang H, et al. Elevated levels of connective tissue growthfactor, WISP-1, and CYR61 in primary breast cancers associated with moreadvanced features. Cancer Res 2001;61:8917–23.
28. Xie D, Yin D, Tong X, et al. Cyr61 is overexpressed in gliomas and involvedin integrin-linked kinase-mediated Akt and h-Catenin-TCF/Lef signaling path-ways. Cancer Res 2004;64:1987– 96.
29. Holloway SE, Beck AW, Girard L, et al. Increased expression of Cyr61(CCN1) identified in peritoneal metastases from human pancreatic cancer. J AmColl Surg 2005;200:371– 7.
30. Lin MT, Zuon CY, Chang CC, et al. Cyr61 induces gastric cancer cellmotility/invasion via activation of the integrin/nuclear factor-kappaB/cyclo-oxygenase-2 signaling pathway. Clin Cancer Res 2005;11:5809–20.
31. Lin MT, Chang CC, Chen ST, et al. Cyr61 expression confers resistance toapoptosis in breast cancer MCF-7 cells by a mechanism of NF-nB-dependentXIAP up-regulation. J Biol Chem 2004;279:24015–23.
32. Eck M, Schmausser B, Scheller K, et al. Pleiotropic effects of CXCchemokines in gastric carcinoma: differences in CXCL8 and CXCL1 expressionbetween diffuse and intestinal types of gastric carcinoma. Clin Exp Immuno 2003;134:508 –15.
33. Kwak MK, Hur K, Park DJ, et al. Expression of chemokine receptors inhuman gastric cancer. Tumour Biol 2005;26:65 –70.
34. Burger JA, Burger M, Kipps TJ. Chronic lymphocytic leukemia B cellsexpress functional CXCR4 chemokine receptors that mediate spontaneousmigration beneath bone marrow stromal cells. Blood 1999;94:3658–67.
35. Ramjeesingh R, Leung R, Siu CH. Interleukin-8 secreted by endothelial cellsinduces chemotaxis of melanoma cells through the chemokine receptor CXCR1.FASEB J 2003;17:1292 –4.
36. Yamaguchi H, Ishii E, Tashiro K, et al. Role of umblical vein endothelialcells in hematopoiesis. Leuk Lymphoma 1998;31:61 –9.
37. Menendez JA, Vellon L, Mehmi I, et al. A novel CYR61-triggered CYR61-avh3 integrin loop’ regulates breast cancer cell survival and chemosensitivitythrough activation of ERK1/ERK2 MAPK signaling pathway. Oncogene 2005;24:761 –79.
38. Kohn AD, Kovacina KS, Roth RA. Insulin stimulates the kinase activity ofRAC-PK, a pleckstrin homology domain containing ser/thr kinase. EMBO J1995;14:4288–295.
39. Kireeva ML, Lam SC, Lau LF. Adhesion of human umbilical veinendothelial cells to the immediate-early gene product Cyr61 is mediated throughintegrin avh3. J Biol Chem 1998;273:3090–6.
40. Leu SJ, Lam SC, Lau LF. Pro-angiogenic activities of CYR61 (CCN1)mediated through integrins avh3 and a6h1 in human umbilical vein endothelialcells. J Biol Chem 2002;277:46248–55.
41. Grzeszkiewicz TM, Kirschling DJ, Chen N, et al. CYR61 stimulates humanskin fibroblast migration through integrin av-h5 and enhances mitogenesisthrough integrin av-h3, independent of its carboxyl-terminal domain. J BiolChem 2001;276:21943 –50.
42. Stupack DG, Cheresh DA. Get a ligand, get a life: integrins, signaling andcell survival. J Cell Sci 2002;115:3729 –38.
43. Tsai MS, Bogart DF, Li P, et al. Expression and function of CYR61, anangiogenic factor, in breast cancer cell lines and tumor biopsies. Cancer Res 2002;60:5603–7.
44. Tong X, Xie D, O’Kelly J, et al. Cyr61, a member of CCN family, is a tumorsuppressor in non-small cell lung cancer. J Biol Chem 2001;276:47709– 14.
45. Sampath D, Winneker RC, Zhang Z. Cyr61, a member of the CCN family, isrequired for MCF-7 cell proliferation: regulation by 17h-estradiol and overexpression in human breast cancer. Endocrinology 2001;142:2540–8.
46. Richards BL, Eisma RJ, Spiro JD, et al. Coexpression of interleukin-8 receptors in head and neck squamous cell carcinoma. Am J Surg 1997;174:507 –12.
47. Kitadai Y, Haruma K, Mukaida N, et al. Regulation of disease-progressiongenes in human gastric carcinoma cells by interleukin 8. Clin Cancer Res 2000;6:2735– 40.
48. Miller LJ, Kurtzman SH, Wang Y, et al. Expression of interleukin-8 receptorson tumor cells and vascular endothelial cells in human breast cancer tissues.Anticancer Res 1998;18:77 –82.
49. Mashino K, Sadanaga N, Yamaguchi H, et al. Expression of chemokinereceptor CCR7 is associated with lymph node metastasis of gastric carcinoma.Cancer Res 2002;62:2937– 41.
50. Gunn MD, Kyuwa S, Tam C, et al. Tobacco, alcohol and the risk of gastriccancer. A population-based case – control study in Sweden. Int J Cancer 1994;57:26 –31.
51. Nicolson GL. Metastatic tumor cell attachment and invasion assayutilizing vascular endothelial cell monolayers. J Histochem Cytochem 1982;30:214–20.
52. Cohen MC, Bereta M, Bereta J. Effect of cytokines on tumor cell-endothelialinteractions. Indian J Biochem Biophys 1997;34:199– 204.
53. Nicolson GL, Irimura T, Nakajima M, et al. Metastatic cell attachment toand invasion of vascular endothelium and its underlying basal lamina usingendothelial cell monolayers. Symp Fundam Cancer Res 1983;36:145–67.
54. Chen N, Leu SJ, Todorovic V, et al. Identification of a novel integrin avh3binding site in CCN1 (CYR61) critical for pro-angiogenic activities in vascularendothelial cells. J Biol Chem 2004;279:44166–76.
55. Schober JM, Chen N, Grzeszkiewicz TM, et al. Identification of integrina(M)h(2) as an adhesion receptor on peripheral blood monocytes for Cyr61(CCN1) and connective tissue growth factor (CCN2): immediate-early geneproducts expressed in atherosclerotic lesions. Blood 2002;99:4457–65.
56. Wang GK, Zhang W. The signaling network of tumor invasion. HistolHistopathol 2005;20:593–602.
57. Babic AM, Kireeva ML, Kolesnikova TV, et al. CYR61, a product of agrowth factor-inducible immediate early gene, promotes angiogenesis and tumorgrowth. Proc Natl Acad Sci U S A 1998;95:6355–60.
58. Hruska KA, Teitelbaum SL. Renal osteodystrophy. N Engl J Med 1995;333:166 –74.
59. Chellaiah M, Fitzgerald C, Filardo EJ, et al. Osteopontin activation of c-src inhuman melanoma cells requires the cytoplasmic domain of the integrin a v-subunit. Endocrinology 1996;137:2432– 40.
60. Obergfell A, Eto K, Mocsai A, et al. Coordinate interactions of Csk, Src, andSyk kinases with [a]IIb[h]3 initiate integrin signaling to the cytoskeleton. J CellBiol 2002;157:265 –75.
61. Arias-Salgado EG, Lizano S, Sarkar S, et al. Src kinase activation by directinteraction with the integrin h cytoplasmic domain. Proc Natl Acad Sci U S A2003;100:13298–302.
62. Luscinskas FW, Brock AF, Arnaout MA, et al. Endothelial-leukocyteadhesion molecule-1-dependent and leukocyte (CD11/CD18)-dependent mecha-nisms contribute to polymorphonuclear leukocyte adhesion to cytokine-activatedhuman vascular endothelium. J Immunol 1989;142:2257– 63.
63. Zijlstra A, Mellor R, Panzarella G, et al. A quantitive analysis of rate-limitingsteps in the metastatic cascade using human-specific real-time polymerase chainreaction. Cancer Res 2002;62:7083–7092.
Cyr61 Promotes Invasiveness of Gastric Cancer
Mol Cancer Res 2007;5(11). October 2007
1123
on April 8, 2020. © 2007 American Association for Cancer Research. mcr.aacrjournals.org Downloaded from

2007;5:1111-1123. Mol Cancer Res Been-Ren Lin, Cheng-Chi Chang, Li-Ro Chen, et al. Concomitantly Up-Regulating Chemokine Receptor 1 and 2Transendothelial Cell Migration, and Intravasation by Cysteine-Rich 61 (CCN1) Enhances Chemotactic Migration,
Updated version
http://mcr.aacrjournals.org/content/5/11/1111
Access the most recent version of this article at:
Cited articles
http://mcr.aacrjournals.org/content/5/11/1111.full#ref-list-1
This article cites 63 articles, 25 of which you can access for free at:
E-mail alerts related to this article or journal.Sign up to receive free email-alerts
Subscriptions
Reprints and
To order reprints of this article or to subscribe to the journal, contact the AACR Publications
Permissions
Rightslink site. (CCC)Click on "Request Permissions" which will take you to the Copyright Clearance Center's
.http://mcr.aacrjournals.org/content/5/11/1111To request permission to re-use all or part of this article, use this link
on April 8, 2020. © 2007 American Association for Cancer Research. mcr.aacrjournals.org Downloaded from