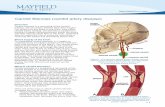
Current indications & therapies for Carotid Artery Stenosis
-
Upload
lpasek -
Category
Health & Medicine
-
view
1.862 -
download
3
description
Transcript of Current indications & therapies for Carotid Artery Stenosis

Carotid Artery Stenosis & Stroke
Current Indications and Therapies

Stroke Facts
Every 45 seconds someone in the USA has a stroke
Annually 46,000 more women than men have a stroke
1 out of every 15 deaths in the USA are because of a stroke
Mean lifetime cost of ischemic stroke is $140,078

What is Carotid Artery Disease?
A type of peripheral arterial disease Narrowing in the carotid artery Atherosclerotic plaque accumulates over
time Most frequently observed at the carotid
bifurcation

A Risk Factor for Stroke
Plaque or clot breaks off from the carotid & blocks a smaller artery in the brain
Narrowing of the carotids due to plaque build-up
A clot becomes wedged in a carotid artery narrowed by plaque

Stroke Symptoms
Sudden weakness of face/arm/leg, especially on one side of the body
Abrupt onset of confusion, trouble speaking or understanding
Sudden double vision or vision problems Abrupt onset of dizziness/loss of balance or
coordination Sudden and severe headache

Carotid Artery Disease Symptoms
Bruit in the affected carotid artery TIA Amarurosis Fugax – temporary blindness in
one eye IMPORTANT: Patients may NOT have any
symptoms

Diagnostic Tools for Carotid Artery Disease
H & P Duplex Ultrasound of the carotids Computed Tomographic Angiography (CTA)
of the neck Magnetic Resonance Angiography (MRA) of
the carotids Carotid Angiography

Duplex Ultrasound Advantages
Non-invasive and painless Widely available Locate and determine degree of lesion
stenosis Post-procedure follow-up tool May give information on the plaque
characteristics

Duplex Ultrasound - Disadvantages
Operator dependent results Tendency for overestimating lesion Calcium may obscure lesion

CTA - Advantages
More precise than a MRA or ultrasound
Safer
Less time consuming
Less invasive that conventional angiography

CTA - Disadvantages
Contrast Nephrotoxicity Allerigc reaction to contrast More complex and expensive than
ultrasound Not widely used compared to ultrasound Patient motion affects image quality

MRA - Advantages
Non-invasive and safer than carotid angiogram
No intra-arterial catheterization
No exposure to x-rays
Procedure and recovery times are shorter that carotid angiography
Allergic reaction to contrast is minimal
Kidney damage from contrast is rare

MRA - Disadvantages
Claustrophobic patients will have to be pre-medicated
Interaction with pacemakers and other metallic implants
Does not image calcium well Very tight stenosis may be difficult to
distinguish from an occulsion

Carotid Angiography - Advantages
Clear & accurate vessel visualization Diagnosis & treatment in a single procedure

Carotid Angiography - Disadvantages
Risk of stroke associated with carotid angiogram
Relatively expensive and invasive Potential for allergic reaction to the dye nephrotoxic

Dr. Anain’s diagnostics
Carotid duplex If the patient is at moderate risk for Carotid
Artery Endarterectomy then a MRA/CTA If the patient is high risk for Carotid Artery
Endarterectomy then: Carotid Angiogram

Treatment Modalities
Medical Therapy Carotid Endarterectomy (CEA) Carotid Artery Stenting (CAS)

Medical Treatment
To reduce the risk of future stroke: Control hypertension, diabetes, and weight Stop smoking Lower cholesterol Increase exercise

Medical Treatment
Serial carotid duplex ultrasounds to monitor the disease
Antiplatelet – Aspirin, Plavix Anticoagulation – coumadin Statin

CEA – Carotid Endarterectomy
To reduce the risk of stroke Surgically remove plaque Arteriotomy at the stenotic section of the
carotid Plaque is manually removed Closure of arteriotomy

CEA Advantages
Proven effective in low surgical risk patients Safe and effective (with an experienced
surgeon) Decreases the risk of stroke

CEA - Disadvantages
Surgery and neck incision therefore longer recovery time
Risk with general anesthesia Potential for emboli and cause stroke Cranial nerve palsy (X and XII) Infection Unproven indication in high surgical risk
candidates

CAS – Carotid Artery Stenting
Endovascular stent placement via stab wound in the groin
For plaque stabilization to reduce the risk of future stroke

CAS
Use of embolic protection placed in carotid artery to reduce the chance of peri-procedure complications (throwing a clot into brain)
Placement of a self-expanding stent to trap or exclude the plaque
Devices (embolic protection) and catheters are removed while the stent remains and the access site (groin) bleeding is managed with a vascular closure device in the wound and a pressure dressing

CAS - Advantages
If patient has contraindication for a CEA (already had a CEA, multiple diseases and a high surgical risk)
Stabilizes the plaque to minimize risk of embolization
Avoids the risk of cranial nerve damage Does not require general anesthesia Option for patients

CAS - Disadvantages
Potential for embolization resulting in stroke Not all patients are suitable for stenting: Severe aortic arch and supra-aortic vessel
tortuosity Thrombus String sign present Patients with very long & severe lesions Heavy all around calcification of the artery

Carotid Endarterectomy-outcomes
Adequate cerebral blood flow Pain controlled Evidence of normal wound healing Know ways to slow the progression of
atherosclerosis Know S&S to report Understand follow-up care

Nursing Diagnoses
Pre-op ineffective cerebral perfusion Post-op potential complications: cerebral
ischemia, respiratory distress, cranial nerve damage (facial VII, hypoglossal XII, glossopharyngeal IX, Vagus X, Accessory XI)
Deficient knowledge, ineffective therapeutic regimen management, or ineffective health maintenance

Nursing DX: Ineffective Tissue Perfusion Cerebral
Partial or complete occulsion of the carotid artery by atherosclerotic plaque and/or thrombus
A cerebral embolus associated with dislodgment of atherosclerotic plaque or a thrombus from the carotid artery

Nursing DX: Ineffective Tissue Perfusion Cerebral – Desired Outcome
Maintain adequate cerebral tissue perfusion as evidenced by:
Mentally alert and orientates Absence of dizziness, visual disturbances,
and speech impairments Normal motor and sensory function

Report Symptoms of Carotid Artery Occlusion and/or cerebral embolization
Agitation Lethargy Confusion Dizziness Slurred speech Expressive aphasia Paresthesias

Measures to maintain adequate cerebral tissue perfusion
Administer antiplatelet agents to prevent new or extended thrombus formation and further occulsion of the carotid artery
Avoid activities that create a Valsalva response (strain with BM, holding breath while moving up in bed)
Prevent HTN to reduce risk of cerebral embolism by reduce stress, give antihypertensives

If Symptoms of decreased cerebral perfusion occur
Maintain of bed rest Head of bed flat unless contraindicated Anticoagulants (IV Heparin, Lovenox,
warfarin Provide emotional support to patient and
family Symptoms usually necessitates postponement of planned surgery

Potential Complications of Carotid Endarterectomy – Cerebral Ischemia
Prolonged artery clamp time during surgery and/or vasospasm associated w/clamping and manipulation of cerebral vessels
Hypotension associated w/hypovolemia from blood loss and IV Dextran commonly used
Embolization during or after surgery and/or formation of a thrombus at surgical site

Potential Complications of Carotid Endarterectomy – Respiratory Distress
Airway obstruction associated w/tracheal compression which can occur as a result of inflammation,
edema, and/or hematoma formation in the surgical
area of the neck

Potential Complications of Carotid Endarterectomy – Cranial Nerve Damage
Facial VII, hypoglossal XII, glossopharyngeal IX, Vagus X, and/or accessory nerves XI
Related to surgical trauma and/or compression of the nerves as a result of inflammation, edema, and/or hematoma formation
Observe for TIA or stroke symptoms

Nursing Actions to maintain adequate cerebral blood flow – post op
Report S&S of excessive site bleeding (new or expanding hematoma, continued bright red bleeding from incision and wound drain
Report decreasing Hgb levels Report S&S of hypovolemic shock Report S&S cerebral ischemia TIA/stroke
symptoms

Implement measures to prevent cerebral ischemia – reduce pressure on carotid vessels
Reduce operative site inflammation and/or edema: HOB up, ice pack to incision as ordered
Maintain patency of wound drain: free of kinks and emptied as often as necessary
Instruct pt to avoid turning head abruptly or hyperextending neck to reduce stress on suture line and prevent a hematoma

Implement measures to prevent cerebral ischemia – reduce pressure on carotid vessels
Caution pt to avoid activities that create a Valsalva response to prevent dislodgment of exisitng thrombi and reduce stress and bleeding from suture line
Maintain blood pressure within a safe range w/ antihypertensives
HTN may occur as a result of underlying disease processes or damage to the carotid sinus baroreceptors during surgery

Implement measures to prevent cerebral ischemia – reduce pressure on carotid vessels
Control HTN to prevent rupture of the operative vessel or reduce risk of dislodgment of any existing thrombus
To treat hypotension consider sympathomimetics (dopamine) and transfer to ICU if on drip

Patient will not experience respiratory distress – assess for & report
Increased edema or expanding hematoma in surgical area
Deviation of trachea from midline New or increased difficulty swallowing S&S of respiratory distress: restlessness, agitation,
rapid and/or labored breathing, stridor, sternocleidomastoid muscle retraction
Significant decrease in pulse oximetry results

Thank You
For your kind attention From: Bridget Foster,RN Christina Palmeri, RN,
Tonya Salter, RN, Lana Pasek, NP, the staff of 3 North of Sister’s of Charity Hospital and Paul Anain, MD of the Endovascular and Vascular Center of Western New York












![COMPUTATIONAL COMPARISON OF FLUID-DYNAMICS IN …€¦ · the Carotid Artery Stenosis Consensus conference [20] for grading carotid stenoses. In particular, stenosis estimate (% diameter](https://static.fdocuments.in/doc/165x107/5f070b947e708231d41b06ac/computational-comparison-of-fluid-dynamics-in-the-carotid-artery-stenosis-consensus.jpg)