Barrett's Esophagus Icd 9 Code, Barrett's Esophagus Classification, Barrett's Esophagus Reversal
Copyright © 2010 Pearson Education, Inc. Figure 23.1 Alimentary canal and related accessory...
-
Upload
agnes-underwood -
Category
Documents
-
view
236 -
download
1
Transcript of Copyright © 2010 Pearson Education, Inc. Figure 23.1 Alimentary canal and related accessory...

Copyright © 2010 Pearson Education, Inc.
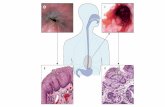
Figure 23.1 Alimentary canal and related accessory digestive organs.
Mouth (oral cavity)Tongue
Esophagus
LiverGallbladder
Anus
DuodenumJejunumIleum
Small intestine
Parotid glandSublingual glandSubmandibulargland
Salivaryglands
Pharynx
StomachPancreas(Spleen)
Transverse colonDescending colonAscending colonCecumSigmoid colonRectumVermiform appendixAnal canal
Largeintestine

Copyright © 2010 Pearson Education, Inc.
Figure 23.2 Gastrointestinal tract activities.
FoodIngestion
PropulsionEsophagus
Stomach
PharynxMechanicaldigestion
Chemicaldigestion
• Chewing (mouth)• Churning (stomach)• Segmentation (small intestine)
Smallintestine Largeintestine
Defecation Anus
Feces
Bloodvessel
Lymphvessel
Absorption
• Swallowing (oropharynx)• Peristalsis (esophagus, stomach, small intestine, large intestine)
Mainly H2O

Copyright © 2010 Pearson Education, Inc.
Figure 23.3 Peristalsis and segmentation.
Frommouth
(b) Segmentation: Nonadjacent segments of alimentary tract organs alternately contract and relax, moving the food forward then backward. Food mixing and slow food propulsion occurs.
(a) Peristalsis: Adjacent segments of alimentary tract organs alternately contract and relax, which moves food along the tract distally.

Copyright © 2010 Pearson Education, Inc.
Figure 23.3a Peristalsis and segmentation.
From mouth
(a) Peristalsis: Adjacent segments of alimentary tract organs alternately contract and relax, which moves food along the tract distally.

Copyright © 2010 Pearson Education, Inc.
Figure 23.3b Peristalsis and segmentation.
(b) Segmentation: Nonadjacent segments of alimentary tract organs alternately contract and relax, moving the food forward then backward. Food mixing and slow food propulsion occurs.

Copyright © 2010 Pearson Education, Inc.
Figure 23.4 Neural reflex pathways initiated by stimuli inside or outside the gastrointestinal tract.
External stimuli(sight, smell, taste,
thought of food)
Central nervous systemand extrinsic autonomic nerves
Afferent impulses Efferent impulses
Long reflexes
Internal(GI tract)stimuli
Chemoreceptors,osmoreceptors, ormechanoreceptors
Local (intrinsic)nerve plexus(“gut brain”)
Effectors:Smooth muscle
or glands
Gastrointestinalwall (site of shortreflexes)
Response:Change in
contractile orsecretory activityLumen of the
alimentary canal
Short reflexes

Copyright © 2010 Pearson Education, Inc.
Figure 23.5 The peritoneum and the peritoneal cavity.
Peritonealcavity
Parietalperitoneum
Visceralperitoneum
Ventralmesentery
Abdominopelviccavity
Mesenteryresorbedand lost
Dorsalmesentery
Vertebra
Alimentarycanal organ
(a) Schematic cross sections of abdominal cavity illustrate the peritoneums and mesenteries.
(b) Some organs lose their mesentery and become retroperitoneal during development.
Alimentarycanal organ
Alimentary canal organ ina retroperitoneal position
Liver

Copyright © 2010 Pearson Education, Inc.
Figure 23.5a The peritoneum and the peritoneal cavity.
Peritonealcavity
Parietalperitoneum
Visceralperitoneum
Ventralmesentery
Abdominopelviccavity
Dorsalmesentery
Vertebra
Alimentarycanal organ
(a) Schematic cross sections of abdominal cavity illustrate the peritoneums and mesenteries.
Liver

Copyright © 2010 Pearson Education, Inc.
Figure 23.5b The peritoneum and the peritoneal cavity.
Abdominopelviccavity
Mesenteryresorbedand lost
(b) Some organs lose their mesentery and become retroperitoneal during development.
Alimentarycanal organ
Alimentary canal organ ina retroperitoneal position

Copyright © 2010 Pearson Education, Inc.
Figure 23.6 Basic structure of the alimentary canal.
Glands in submucosa
Submucosa
LumenMucosa-associatedlymphoid tissue
Duct of gland outsidealimentary canal
Gland in mucosa
NerveArteryVein
Lymphaticvessel Mesentery
Intrinsic nerve plexuses• Myenteric nerve plexus• Submucosal nerve plexus
Mucosa• Epithelium• Lamina propria• Muscularis mucosae
Muscularis externa
• Longitudinal muscle • Circular muscleSerosa• Epithelium• Connective tissue

Copyright © 2010 Pearson Education, Inc.
Figure 23.7 Anatomy of the oral cavity (mouth).
Uvula
Uvula
Soft palate Palatoglossal arch
Palatinetonsil
Palatinetonsil
Sublingualfold withopenings ofsublingual ducts
Hard palate
Oral cavity
Tongue
Tongue
Upper lip
Lower lip
VestibuleGingivae (gums)
Gingivae(gums)
Hard palate
Soft palate
Lingual frenulumOpening ofsubmandibularduct
Palatineraphe
Inferior labialfrenulum
Lingual tonsil
Oropharynx
Posterior wallof oropharynx
Palatopharyngealarch
Superior labialfrenulum
Palatoglossalarch
Epiglottis
Hyoid bone
Laryngopharynx
Esophagus
Trachea
(a) Sagittal section of the oral cavity and pharynx (b) Anterior view

Copyright © 2010 Pearson Education, Inc.
Figure 23.7a Anatomy of the oral cavity (mouth).
UvulaSoft palate Palatoglossal arch
Palatine tonsil
Hard palate
Oral cavity
Tongue
Lingual tonsilOropharynx
EpiglottisHyoid bone
Laryngopharynx
Esophagus
Trachea(a) Sagittal section of the oral cavity and pharynx

Copyright © 2010 Pearson Education, Inc.
Figure 23.7b Anatomy of the oral cavity (mouth).
UvulaPalatine tonsil
Sublingual foldwith openings ofsublingual ducts
Tongue
Upper lip
Lower lip
VestibuleGingivae (gums)
Gingivae (gums)
Hard palate
Soft palate
Lingual frenulum
Opening ofsubmandibular duct
Palatine raphe
Inferior labialfrenulum
Posterior wallof oropharynx
Palatopharyngealarch
Superior labialfrenulum
Palatoglossal arch
(b) Anterior view

Copyright © 2010 Pearson Education, Inc.
Figure 23.8 Dorsal surface of the tongue, and the tonsils.
Epiglottis
PalatopharyngealarchPalatine tonsil
Lingual tonsil
Palatoglossalarch
Foliate papillae
Circumvallatepapilla
Terminal sulcus
Dorsum of tongue
Midline grooveof tongue
Filiform papilla
Fungiform papilla

Copyright © 2010 Pearson Education, Inc.
Figure 23.9 The salivary glands.
Teeth
Ducts ofsublingualgland
Sublingualgland
Submandibularduct
Posterior belly ofdigastric muscle
Parotid ductMasseter muscleBody of mandible (cut)
Parotidgland
Tongue
Submandibulargland
(a)
Lingualfrenulum
Mylohyoidmuscle (cut)Anterior belly ofdigastric muscle
Mucouscells
(b)
Serous cellsforming demilunes

Copyright © 2010 Pearson Education, Inc.
Figure 23.9a The salivary glands.
Teeth
Ducts ofsublingualgland
Sublingualgland
Submandibularduct
Posterior belly ofdigastric muscle
Parotid ductMasseter muscleBody of mandible (cut)
Parotidgland
Tongue
Submandibulargland
(a)
Lingualfrenulum
Mylohyoidmuscle (cut)Anterior belly ofdigastric muscle

Copyright © 2010 Pearson Education, Inc.
Figure 23.9b The salivary glands.
Mucouscells (b)
Serous cellsforming demilunes

Copyright © 2010 Pearson Education, Inc.
Figure 23.10a Human dentition.
IncisorsCentral (6–8 mo)
IncisorsCentral (7 yr)
Canine (eyetooth)(16–20 mo)
Canine (eyetooth)(11 yr)
Premolars(bicuspids)First premolar(11 yr)
MolarsFirst molar(10–15 mo)
MolarsFirst molar (6–7 yr)
Lateral (8–10 mo) Lateral (8 yr)
Second molar(about 2 yr)
Second molar(12–13 yr)Third molar(wisdom tooth)(17–25 yr)(a)
Permanentteeth
Deciduous(milk) teeth Second premolar
(12–13 yr)

Copyright © 2010 Pearson Education, Inc.
Figure 23.10b Human dentition.
Deciduous teeth Permanent teeth(b)

Copyright © 2010 Pearson Education, Inc.
Figure 23.11 Longitudinal section of a canine tooth within its bony alveolus.
Crown
Neck
Root
EnamelDentinDentinal tubulesPulp cavity (containsblood vessels and nerves)Gingiva (gum)
Cementum
Root canalPeriodontalligament
Apical foramen
Bone

Copyright © 2010 Pearson Education, Inc.
Figure 23.12 Microscopic structure of the esophagus.
Mucosa(contains a stratifiedsquamous epithelium)
Submucosa (areolarconnective tissue)
Lumen
Muscularis externa
Adventitia (fibrousconnective tissue)
(a) (b)
• Circular layer • Longitudinal layer

Copyright © 2010 Pearson Education, Inc.
Figure 23.12a Microscopic structure of the esophagus.
Mucosa(contains a stratifiedsquamous epithelium)Submucosa (areolarconnective tissue)
LumenMuscularis externa
Adventitia (fibrousconnective tissue)(a)
• Circular layer • Longitudinal layer

Copyright © 2010 Pearson Education, Inc.
Figure 23.12b Microscopic structure of the esophagus.
Mucosa(contains a stratifiedsquamous epithelium)
(b)

Copyright © 2010 Pearson Education, Inc.
Figure 23.13 Deglutition (swallowing) (1 of 5).
Tongue
Trachea
Pharynx
Epiglottis
Glottis
Bolus of food
1 Upper esophageal sphincter is contracted. Duringthe buccal phase, the tongue presses against the hard palate, forcing the food bolus into the oropharynx where the involuntary phase begins.

Copyright © 2010 Pearson Education, Inc.
Figure 23.13 Deglutition (swallowing) (2 of 5).
Epiglottis
Esophagus
Uvula
Bolus
2 The uvula and larynx rise to prevent food fromentering respiratory passageways. The tongue blocks off the mouth. The upper esophageal sphincter relaxes, allowing food to enter the esophagus.

Copyright © 2010 Pearson Education, Inc.
Figure 23.13 Deglutition (swallowing) (3 of 5).
Bolus
3 The constrictor muscles of the pharynx contract, forcing food into the esophagus inferiorly. The upper esophageal sphincter contracts (closes) after entry.

Copyright © 2010 Pearson Education, Inc.
Figure 23.13 Deglutition (swallowing) (4 of 5).
Relaxed muscles
Circular musclescontract
Bolus of food
Longitudinal musclescontract
Stomach
Gastroesophagealsphincter closed
4 Food is moved throughthe esophagus to the stomach by peristalsis.

Copyright © 2010 Pearson Education, Inc.
Figure 23.13 Deglutition (swallowing) (5 of 5).
Relaxedmuscles
Gastroesophagealsphincter opens
5 The gastroesophageal sphincter opens, and food enters the stomach.

Copyright © 2010 Pearson Education, Inc.
Figure 23.14a Anatomy of the stomach.
Cardia
Esophagus
Pyloric sphincter(valve) at pylorus
Pyloriccanal
Pyloricantrum
Rugae ofmucosa
Body
Lumen
Serosa
Fundus
Lessercurvature
Greatercurvature
Muscularisexterna • Longitudinal layer • Circular layer • Oblique layer
(a)
Duodenum

Copyright © 2010 Pearson Education, Inc.
Figure 23.14b Anatomy of the stomach.
Liver(cut)
Lessercurvature
Body
Fundus
Spleen
Greatercurvature
(b)

Copyright © 2010 Pearson Education, Inc.
Figure 23.15a Microscopic anatomy of the stomach.
Mucosa
Surfaceepithelium
Lamina propria
Muscularismucosae
Oblique layer
Circular layer
Longitudinallayer
Serosa
(a) Layers of the stomach wall (l.s.)Stomach wall
Muscularis externa(contains myentericplexus)
Submucosa(contains submucosalplexus)

Copyright © 2010 Pearson Education, Inc.
Figure 23.15b Microscopic anatomy of the stomach.
(b) Enlarged view of gastric pits and gastric glands
Mucous neck cells
Parietal cell
Surface epithelium(mucous cells)
Gastric pits
Chief cell
Enteroendocrine cell
Gastric pit
Gastric gland

Copyright © 2010 Pearson Education, Inc.
Figure 23.15c Microscopic anatomy of the stomach.
(c) Location of the HCl-producing parietal cells and pepsin-secreting chief cells in a gastric gland
Pepsinogen
Mitochondria
PepsinHCl
Chief cell
Enteroendocrinecell
Parietal cell

Copyright © 2010 Pearson Education, Inc.
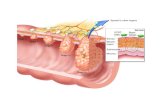
Figure 23.16 Photographs of a gastric ulcer lesion and of the bacteria that most commonly cause it.
Bacteria
Mucosalayer ofstomach
(a) A gastric ulcer lesion (b) H. pylori bacteria

Copyright © 2010 Pearson Education, Inc.
Figure 23.16a Photographs of a gastric ulcer lesion and of the bacteria that most commonly cause it.

Copyright © 2010 Pearson Education, Inc.
Figure 23.16b Photographs of a gastric ulcer lesion and of the bacteria that most commonly cause it.
Bacteria
Mucosalayer ofstomach
(b) H. pylori bacteria

Copyright © 2010 Pearson Education, Inc.
Figure 23.17 Neural and hormonal mechanisms that regulate release of gastric juice.
Presence of lowpH, partially digested foods, fats, or hypertonic solution in duodenum when stomach begins to empty
Distension;presence offatty, acidic,partiallydigested foodin theduodenum
Briefeffect
Intestinal(enteric)gastrinreleaseto blood
Entero-gastricreflex
Release of intestinalhormones (secretin,cholecystokinin, vasoactiveintestinal peptide)
Localreflexes
Vagalnucleiin medulla
Pyloricsphincter
Stimulate
Inhibit
1
1
2
Stomachsecretoryactivity
Sight and thoughtof food
Stomachdistensionactivatesstretchreceptors
Stimulation oftaste and smellreceptors
Food chemicals(especially peptides and caffeine) and rising pHactivate chemoreceptors
Loss ofappetite,depression
Emotionalupset
Lack ofstimulatoryimpulses toparasym-patheticcenter
Cerebralcortex
Cerebral cortexConditioned reflex
Vagovagalreflexes
Localreflexes
Medulla
G cells
Hypothalamusand medullaoblongata
Vagusnerve
Vagusnerve
Gastrinreleaseto blood
Gastrinsecretiondeclines
G cells
Overridesparasym-patheticcontrols
Sympatheticnervoussystemactivation
1
11
1
2
2
2
Stimulatory events Inhibitory events
Cephalicphase
Gastricphase
Intestinalphase
Excessiveacidity (pH <2) in stomach
Distension of duodenum; presence of fatty, acidic, hypertonic chyme, and/or irritants in the duodenum

Copyright © 2010 Pearson Education, Inc.
Figure 23.18 Mechanism of HCl secretion by parietal cells.
Stomach lumenChief cell
Parietal cell
Inter-stitialfluid
Carbonicanhydrase
Alkalinetide
HCO3–
Bloodcapillary
CO2
Cl–
CO2 + H2O
H2CO3
HCO3–- Cl–
antiporter
HCO3–
H+
Cl– Cl–l
K+ K+
H+
H+-K+
ATPase
HCI

Copyright © 2010 Pearson Education, Inc.
Figure 23.19 Peristaltic waves in the stomach.
1 Propulsion: Peristaltic waves move from the fundus toward the pylorus.
2 3 Grinding: The most vigorous peristalsis and mixing action occur close to the pylorus.
Retropulsion: The pyloric end of the stomach acts as a pump that delivers small amounts of chyme into the duodenum, simultaneously forcing most of its contained material backward into the stomach.
Pyloricvalveclosed
Pyloricvalveclosed
Pyloricvalveslightlyopened

Copyright © 2010 Pearson Education, Inc.
Figure 23.20 Neural and hormonal factors inhibiting gastric emptying.
Presence of fatty, hypertonic,acidic chyme in duodenum
Duodenal entero-endocrine cells
Chemoreceptors andstretch receptors
Enterogastrones(secretin, cholecystokinin,vasoactive intestinalpeptide)
Duodenalstimulidecline
Via shortreflexes
Via longreflexes
Entericneurons
Initial stimulus
Physiological response
Result
Contractile force andrate of stomachemptying decline
CNS centers sympathetic activity; parasympathetic activity
Stimulate
Inhibit
Secrete Target

Copyright © 2010 Pearson Education, Inc.
Figure 23.21 The duodenum of the small intestine, and related organs.
Jejunum
Mucosawith folds
Cystic duct
DuodenumHepatopancreaticampulla and sphincter
Gallbladder
Right and lefthepatic ducts of liver
Bile duct and sphincter
Main pancreatic ductand sphincter
PancreasTail of pancreas
Head of pancreas
Common hepatic duct
Major duodenalpapilla
Accessory pancreatic duct

Copyright © 2010 Pearson Education, Inc.
Figure 23.22a Structural modifications of the small intestine that increase its surface area for digestion and absorption.
Vein carrying blood tohepatic portal vessel
MusclelayersCircularfoldsVilli
(a)
Lumen

Copyright © 2010 Pearson Education, Inc.
Figure 23.22b Structural modifications of the small intestine that increase its surface area for digestion and absorption.
(b)
Absorptive cells
Lacteal
Intestinal crypt
Mucosaassociatedlymphoid tissue
MuscularismucosaeDuodenal gland Submucosa
EnteroendocrinecellsVenuleLymphatic vessel
Goblet cellBloodcapillaries
Vilus
Microvilli(brush border)

Copyright © 2010 Pearson Education, Inc.
Figure 23.22c Structural modifications of the small intestine that increase its surface area for digestion and absorption.
(c) Intestinal crypt
Absorptive cells
Villi
Gobletcells

Copyright © 2010 Pearson Education, Inc.
Figure 23.23 Villi and microvilli of the small intestine.
(b)
Microvilli
Absorptivecell
(a)
Desquamatingcells
Villi

Copyright © 2010 Pearson Education, Inc.
Figure 23.23a Villi and microvilli of the small intestine.
(a)
Desquamatingcells
Villi

Copyright © 2010 Pearson Education, Inc.
Figure 23.23b Villi and microvilli of the small intestine.
(b)
Microvilli
Absorptivecell

Copyright © 2010 Pearson Education, Inc.
Figure 23.24a Gross anatomy of the human liver.
SternumNipple
Liver
Right lobeof liver
Gallbladder
(a)
Bare area
Falciformligament
Left lobe of liver
Round ligament(ligamentum teres)

Copyright © 2010 Pearson Education, Inc.
Figure 23.24b Gross anatomy of the human liver.
Lesser omentum(in fissure)
Left lobe of liver
(b)
Porta hepatiscontaining hepaticartery (left) andhepatic portal vein(right)Quadrate lobeof liverLigamentum teres
Gallbladder
Hepatic vein (cut)
Sulcus forinferiorvena cava
Caudate lobeof liver
Bare area
Bile duct (cut)
Right lobe ofliver
Sternum
Nipple
Liver

Copyright © 2010 Pearson Education, Inc.
Figure 23.25a-b Microscopic anatomy of the liver.
(a) (b)Lobule Central vein Connectivetissue septum

Copyright © 2010 Pearson Education, Inc.
Figure 23.25c Microscopic anatomy of the liver.
(c)
Interlobular veins(to hepatic vein) Central vein
Sinusoids
Portal triad
Plates ofhepatocytes
Portal vein
Fenestratedlining (endothelial cells) of sinusoids
Bile duct (receivesbile from bile canaliculi)
Bile duct
Portal arteriolePortal venuleHepatic
macrophagesin sinusoid walls
Bile canaliculi

Copyright © 2010 Pearson Education, Inc.
Figure 23.26 Structure of the enzyme-producing tissue of the pancreas.
Small duct
Acinar cells
Basement membrane
Zymogen granules
Rough endoplasmicreticulum(a)
(b)
Acinar cells

Copyright © 2010 Pearson Education, Inc.
Figure 23.26a Structure of the enzyme-producing tissue of the pancreas.
Smallduct
Acinar cells
Basementmembrane
Zymogengranules
Roughendoplasmicreticulum
(a)

Copyright © 2010 Pearson Education, Inc.
Figure 23.26b Structure of the enzyme-producing tissue of the pancreas.
(b)
Acinarcells

Copyright © 2010 Pearson Education, Inc.
Figure 23.27 Activation of pancreatic proteases in the small intestine.
Stomach
Pancreas
Epithelialcells
Trypsinogen(inactive)Chymotrypsinogen(inactive)Procarboxypeptidase(inactive)
Trypsin
Chymotrypsin
Carboxypeptidase
Membrane-boundenteropeptidase

Copyright © 2010 Pearson Education, Inc.
Figure 23.28 Mechanisms promoting secretion and release of bile and pancreatic juice.
1
2
3
4
5
6
Chyme enter-ing duodenum causes release ofcholecystokinin (CCK) and secretin from duodenal enteroendocrine cells.
CCK (red dots) and secretin (yellow dots) enter the bloodstream.
CCK induces secretion of enzyme-rich pancreatic juice. Secretin causes secretion of HCO3
–-rich pancreatic juice.
Bile salts and, to a lesser extent, secretin transported via bloodstream stimulate liver to produce bile more rapidly.
CCK (via bloodstream) causes gallbladder to contract and hepatopancreatic sphincter to relax; bile enters duodenum.
During cephalic and gastric phases, vagal nerve stimulation causes weak contractions of gallbladder.

Copyright © 2010 Pearson Education, Inc.
Figure 23.29a Gross anatomy of the large intestine.
Left colic(splenic) flexure
Transversemesocolon
Epiploicappendages
Descendingcolon
Teniae coli
Sigmoidcolon
Cut edge ofmesentery
External anal sphincter
Rectum
Anal canal(a)
Right colic(hepatic) flexureTransversecolon SuperiormesentericarteryHaustrum
Ascendingcolon IIeum
IIeocecal valve
Vermiform appendix
Cecum

Copyright © 2010 Pearson Education, Inc.
Figure 23.29b Gross anatomy of the large intestine.
(b)
Rectal valveRectum
Anal canal
Levator animuscle
Anus
Anal sinuses
Anal columns
Internal analsphincter
External analsphincter
Hemorrhoidalveins
Pectinate line

Copyright © 2010 Pearson Education, Inc.
Figure 23.30a Mesenteries of the abdominal digestive organs.
Falciform ligament
Liver
Gallbladder
Spleen
Stomach
Ligamentum teres
Greater omentum
Small intestine
Cecum
(a)

Copyright © 2010 Pearson Education, Inc.
Figure 23.30b Mesenteries of the abdominal digestive organs.
Liver
Lesser omentumGallbladder
StomachDuodenum
Transverse colon
Small intestine
Cecum
Urinary bladder(b)

Copyright © 2010 Pearson Education, Inc.
Figure 23.30c Mesenteries of the abdominal digestive organs.
Transverse colon
Greater omentum
Descending colonJejunumMesentery
Transversemesocolon
Sigmoidmesocolon
Sigmoid colon
Ileum
(c)

Copyright © 2010 Pearson Education, Inc.
Figure 23.30d Mesenteries of the abdominal digestive organs.
(d)
Pancreas
LiverLesser omentum
Stomach
Duodenum
Transversemesocolon
Greater omentumMesentery
Jejunum
Visceral peritoneum
Urinary bladder
Transverse colon
Ileum
Parietal peritoneum
Rectum

Copyright © 2010 Pearson Education, Inc.
Figure 23.31 Defecation reflex.
Impulses fromcerebral cortex(consciouscontrol)
Voluntary motornerve to externalanal sphincter
External analsphincter(skeletal muscle)
Internal anal sphincter(smooth muscle)
Sensorynerve fibers
Involuntary motor nerve(parasympathetic division)
Stretch receptors in wall
Rectum
Sigmoidcolon
3
1
2
Distension, or stretch, of therectal walls due to movement of feces into the rectum stimulates stretch receptors there. The receptors transmit signals along afferent fibers to spinal cord neurons.
A spinal reflex is initiated in which parasympathetic motor (efferent) fibers stimulate contraction of the rectal walls and relaxation of the internal anal sphincter.
If it is convenient to defecate, voluntary motor neurons are inhibited, allowing the external anal sphincter to relax so that feces may pass.

Copyright © 2010 Pearson Education, Inc.
Figure 23.32 Flowchart of chemical digestion and absorption of foodstuffs (1 of 4).
Carbohydrate digestion
• Glucose and galactose are absorbed via cotransport with sodium ions.• Fructose passes via facilitated diffusion.• All monosaccharides leave the epithelial cells via facilitated diffusion, enter the capillary blood in the villi, and are transported to the liver via the hepatic portal vein.
Starch and disaccharides
Oligosaccharidesand disaccharides
Lactose Maltose Sucrose
Glucose Fructose
Salivaryamylase
Mouth
Pancreaticamylase
Brush borderenzymes in small intestine(dextrinase, gluco-amylase, lactase, maltase, and sucrase)
Smallintestine
Smallintestine
Foodstuff
Galactose
Path of absorptionEnzyme(s)and source
Site ofaction

Copyright © 2010 Pearson Education, Inc.
Figure 23.32 Flowchart of chemical digestion and absorption of foodstuffs (2 of 4).
Protein digestion
• Amino acids are absorbed by cotransport with sodium ions.• Some dipeptides and tripeptides are absorbed via cotransport with H+
and hydrolyzed to amino acids within the cells.
+
• Amino acids leave the epithelial cells by facilitated diffusion, enter the capillary blood in the villi, and are transported to the liver via the hepatic portal vein.
Smallintestine
Smallintestine
Stomach
Foodstuff
Protein
Large polypeptides
Pepsin(stomach glands)in presence of HCl
Small polypeptides,small peptides
Pancreaticenzymes (trypsin, chymotrypsin,carboxypeptidase)
Amino acids(some dipeptidesand tripeptides)
Brush border enzymes(aminopeptidase,carboxypeptidase,and dipeptidase)
Path of absorptionEnzyme(s)and source
Site ofaction

Copyright © 2010 Pearson Education, Inc.
Figure 23.32 Flowchart of chemical digestion and absorption of foodstuffs (3 of 4).
Fat digestion
Small intestine
Small intestine
Foodstuff
Unemulsifiedfats
Emulsification by the detergent action of bile salts ductedin from the liver
Pancreatic lipases
Monoglyceridesand fatty acids
Glyceroland
fatty acids
Path of absorptionEnzyme(s)and source
Site ofaction
• Fatty acids and monoglycerides enter the intestinal cells via diffusion. • Fatty acids and monoglycerides are recombined to form triglycerides and then combined with other lipids and proteins within the cells, and the resulting chylomicrons are extruded by exocytosis.
• The chylomicrons enter the lacteals of the villi and are transported to the systemic circulation via the lymph in the thoracic duct.• Some short-chain fatty acids are absorbed, move into the capillary blood in the villi by diffusion, and are transported to the liver via the hepatic portal vein.

Copyright © 2010 Pearson Education, Inc.
Figure 23.32 Flowchart of chemical digestion and absorption of foodstuffs (4 of 4).
Nucleic acid digestion
• Units enter intestinal cells by active transport via membrane carriers.
• Units are absorbed into capillary blood in the villi and transported to the liver via the hepatic portal vein.
Smallintestine
Smallintestine
Foodstuff
Nucleic acids
Pancreatic ribo-nuclease and deoxyribonuclease
Brush borderenzymes(nucleosidasesand phosphatases)
Pentose sugars,N-containing bases,
phosphate ions
Path of absorptionEnzyme(s)and source
Site ofaction

Copyright © 2010 Pearson Education, Inc.
Figure 23.33 Protein digestion and absorption in the small intestine.
Absorptiveepithelialcell
Apical membrane (microvilli)
Aminoacid carrier
Capillary
Lumen of intestine
Pancreaticproteases
Amino acids of protein fragmentsBrush border enzymes
Na+
Na+
1 Proteins and protein fragments are digested to amino acids by pancreatic proteases (trypsin, chymotrypsin, and carboxy- peptidase), and by brush border enzymes (carboxypeptidase, aminopeptidase, and dipeptidase)of mucosal cells.
2 The amino acids are then absorbed by active transport into the absorptive cells, and move to their opposite side (transcytosis).
3 The amino acids leave the villus epithelial cell by facilitated diffusion and enter the capillary via intercellular clefts.
Active transport
Passive transport

Copyright © 2010 Pearson Education, Inc.
Figure 23.34 Emulsification, digestion, and absorption of fats.
Epithelialcells ofsmallintestine
Fat dropletscoated withbile salts
Fat globule
Lacteal
Bile salts
Micelles made up of fatty acids, monoglycerides,and bile salts
1 Large fat globules are emulsified (physically broken up into smaller fat droplets) by bile salts in the duodenum.
2 Digestion of fat by the pancreatic enzyme lipase yields free fatty acids and monoglycerides. These then associate with bile salts to form micelles which “ferry” them to the intestinal mucosa.
3 Fatty acids and monoglycerides leave micelles and diffuse into epithelial cells. There they are recombined and packaged with other lipoid substances and proteins to form chylomicrons.
4 Chylomicrons are extruded from the epithelial cells by exocytosis. The chylomicrons enter lacteals. They are carried away from the intestine by lymph.

Copyright © 2010 Pearson Education, Inc.
Figure 23.35 Embryonic development of the digestive system.
Stomodeum
Foregut
Site ofliverdevelopmentMidgut
Spinal cord
Hindgut
Proctodeum
Endoderm
Brain
Oralmembrane
Heart
Yolk sac
Cloacalmembrane
Bodystalk
(a)
Lung bud
Liver
Gall-bladder
Cystic ductVentral pancreatic bud
Dorsalpancreaticbud
Duodenum
Stomach
(b)
Bileduct

Copyright © 2010 Pearson Education, Inc.
Figure 23.35a Embryonic development of the digestive system.
Stomodeum
Foregut
Site ofliverdevelopmentMidgut
Spinal cord
Hindgut
Proctodeum
Endoderm
Brain
Oralmembrane
Heart
Yolk sac
Cloacalmembrane
Bodystalk (a)

Copyright © 2010 Pearson Education, Inc.
Figure 23.35b Embryonic development of the digestive system.
Stomodeum
Lung bud
Liver
Gall-bladder
Cystic ductVentral pancreatic bud
Dorsalpancreaticbud
Duodenum
Stomach
(b)
Bileduct

Copyright © 2010 Pearson Education, Inc.
Table 23.1 Hormones and Paracrines that Act in Digestion (1 of 2)

Copyright © 2010 Pearson Education, Inc.
Table 23.1 Hormones and Paracrines that Act in Digestion (2 of 2)

Copyright © 2010 Pearson Education, Inc.
Table 23.2 Overview of the Functions of the Gastrointestinal Organs (1 of 2)

Copyright © 2010 Pearson Education, Inc.
Table 23.2 Overview of the Functions of the Gastrointestinal Organs (2 of 2)

Copyright © 2010 Pearson Education, Inc.
Table 23.3 Control of Small Intestinal Motility

Copyright © 2010 Pearson Education, Inc.
Making Connections 23.1 Homeostatic Interrelationships Between the Digestive System and Other Body Systems