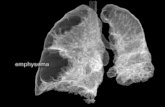
COPD - what is it? C = Chronic O = Obstruction of the airways P = Pulmonary D = Disease Emphysema,...
-
Upload
alberta-rich -
Category
Documents
-
view
213 -
download
1
Transcript of COPD - what is it? C = Chronic O = Obstruction of the airways P = Pulmonary D = Disease Emphysema,...

COPD - what is it?
C = Chronic
O = Obstruction of the airways
P = Pulmonary
D = Disease
Emphysema, Chronic bronchitis, smokers lung, ‘Asthma’
BREATHLESSNESS
cough

Why does COPD matter….to clinicians, commissioners and
patients? Common and increasing in prevalence
1 in 8 acute medical admissions Significant cause of death
1 in 20 deaths 1 in 7 patients admitted with COPD die within 3 months
Significant cause of morbidity 1 in 3 patients with COPD readmitted within 3 months One million bed-days
Preventable and treatable Caused by smoking Patients live with COPD for many years Disabling and frightening breathlessness

Thinking strategically, implementing locally
A joint British Thoracic Society (BTS)
and General Practice Airways Group
(GPIAG) initiative providing the clinical
leadership required to drive high
quality patient-centred care across the
traditional boundaries of secondary and
primary care to integrate and improve
the services for people with respiratory
disease

Who’s who
Anthony Davison, Clinical Director, Southend (BTS Co Chair)
Stephen Holmes, GP, Taunton (GPIAG Co Chair)
Steph Austin, Project Manager, End of Life and Deprivation of Liberties Derby City PCT
Dermot Ryan, GP, Loughbourgh
Stephen Gaduzo, GPwSI, Stockport
Kevin Gruffydd-Jones, GP, Bath
Louise Restrick, consultant respiratory physician, London
Jane Scullion, consultant respiratory nurse, Leicester
Steve Connellan, retired consultant respiratory physician, and coding expert!
Sharon Haggerty, Head of Adult Services, County Durham
Steve Catling, lay representative
Supported by:
Siân Williams (Project Manager ex NHS Manager)
BTS & GPIAG Chairs and CEs
BTS 2600 doctors, doctors in training, nurses, stop smoking professionals, specialist nurses, respiratory physios, technical and physiological measurement
GPIAG: 2400 primary care professionals with respiratory interest
INTEGRATION across professions, across primary and secondary care

Practice basedCommissioning
Money followingpatients
(payment by results)
The context from which we evolved
All Trustsable to apply for
FT status
More choicefor patients
Stronger PCTswith fair funding Regulation for
safety and quality
Independent Sector addingcapacity and
innovation
Better CareBetter patient
experienceBetter value-for-
money
Better information
New providers
e.g. social enterprise

How it felt
F R A G M E N T A T I O N
isolation over reliance on data
Job cuts
People asked to work outside competence
Anxiety

Why IMPRESS is relevant
Primary and community care strategy Leading local change Support PCTs and clinicians to make local decisions on
integrated primary and community care services
World Class Commissioning Lead meaningful engagement with clinicians
Manage knowledge and assess needs
Prioritise for improved outcomes
Influence and shape the market
Support and manage providers

How we can add value
Make it simpler to commission the right thing
Where clear evidence of best practice Eg Pulmonary Rehab, hospital at home
Where uncertain evidence but certain need Eg end of life care COPD
Communicate in language meaningful to clinicians and commissioners
BTS / GPIAG leadership
Make tensions energising not draining

What we are achieving
Role model for integration Primary and secondary care Doctors, nurses, managers Lay representation
Improved understanding Processes Policy Standards
Produced “things” for commissioners and clinicians

Role model: network which “does”
Clinical strategy for COPD will require networks Communication face-to-face
Increased respect Sharing beliefs
Sharing resources, knowledge, opinion eg primary care innovation
Learning: gain from different attitudes eg to risk Positive relationship with pharma industry Include providers and commissioners, clinicians and
managers: start here Project manager: have one Work out positions on 3rd sector, patients, social care Challenges about primary care competence and
secondary care responsiveness: find ways to demonstrate competence

For you to use: Website: www.impressresp.com Jargon Buster Skill mix and competence framework Vision letter to Darzi team Submission to PbR team on unbundling tariff +
guide to coding Criteria for Hospital Referral, Admission,
Discharge and follow up Conference: Royal College of Physicians (6
March 08) Service specification paper: how to guide and
sample COPD spec Delivering care closer to home: outpatient shift
paper Guide to respiratory coding

For you to use (2) Educational package ready by February 2009 Effective Care - Effective
Communication: Living and Dying with COPD
Advised on Clinical Strategy and communications strategy End of life care quality markers - detailed response to consultation Stories
Somerset PCT tender Kings Fund scenario planning Wigan, Hammersmith community consultants Needs assessment, Salford

Commissioning to meet the needs of patients with
COPD

What next?
Education and training across the system: explore roles Develop clinical leaders and networks Launch and implement ‘Living and Dying with COPD’
communication skills education programme Shared evidence bases (service development and clinical) How to procure improvement and integration PROMs Audit patient journey experience Evaluation criteria for evaluating impact of new services Sleep services Asthma Extending our reach and evaluating our impact Use Clinical Strategy to raise profile of respiratory care Managing Long Term conditions meeting 7 April 28 April, London first IMPRESS conference,

Respiratory specifications
Networks Needs assessment: JSNA,
East Region PHO model Vision Clinical leadership What do you want - the matrix,
human capital, research How much do you want to
spend - programme budgeting Who’s accountable for what? Training and education Governance Procurement rules Contracting currency

Care Closer to Home Integration Substitution
Location Skills Technology Model from medical model to
supported self care/co-creation/co-production model
Organisational (eg by private or voluntary sector)
Segmentation Simplification “Decisions about location
and level of specialism should be kept separate”
“ right care at the right time, reliably, by the professional(s) most competent to provide their care. “Patients…more flexible access: timing and mode of consultation
with a HCP of their choice…[that] suits them at that point in their lives

Dos and don'ts of procurement
Commissioners (1)
Support or establish a clinical network for needs assessment, service specification and care pathways
Beware IP exploitation when develop specifications Involve local patients actively and continuously What’s sustainable and cost-effective: competitive
procurement or a continuous improvement What’s readiness of the local NHS to enter a fair
competition: how will you help? What’s impact on integration and on NHS sustainability if
the contract is won by a non-NHS provider Who will be your expert primary and secondary care
advisors to adjudicate bidders?

Dos and don'ts of procurement
Commissioners (2)
Is responsibility for keeping the service up-to-date with best practice built into the specification?
Consider NHS human and intellectual capital: should spec include provision of audit, research, education and training of primary and community care professionals?
Consider inclusion of incentives to reward best practice Have benchmark data for evaluation and some manageable but
important evaluation criteria e.g. continuity of care for patients, equity of access across practices and localities, hospital utilisation, unscheduled care.
Clarify for clinicians who the commissioners are - names, contacts Consider unintended consequences e.g. residual costs of providing
an acute medicine service and therefore the total costs of the system if investment is removed from a local trust.
25 June 2008

Dos and don'ts of procurement
NHS clinicians
Get involved in any local clinical network across primary and secondary care Actively work together to consider improvements Use IMPRESS resources e.g. BTS referral criteria to assist in these conversations Plan for how you and your colleagues will listen to patients and engage them in not just self-
management but also in service design, information provision and service evaluation Campaign for investment in respiratory care: demonstrate how it can meet commissioners’
aims: reduction in avoidable hospital admissions care closer to patients’ homes prevention (“upstream” eg system-wide leadership for smoking cessation)
Maintain relationships with colleagues but be sure you know what their role is now, and who the decision-makers:
who is a PCT commissioner? who is in the PCT provider organisation? who is a practice-based commissioner? who is a GP with an interest in providing services?
25 June 2008

Dos and don'ts of procurement
Bidders: it needs one knowledgeable person full-time for several weeks + expert help
Familiarise yourselves with process: scoring system, timelines and adjudication Get help early from people who have the appropriate skills in
budgeting and scenario planning data analysis social marketing presentations
Make connections with key stakeholders directly Having read the specification, is it appropriate to bid – does it fit organisation’s
strategy? Do you have the resources to bid? What are the risks of not bidding, or not winning? Do you have the resources to deliver the service? If you bid, respond to the specification as it is written in the final documents; seek
clarification using the formal processes Start thinking “out of the box”, without being restricted by knowing how things are
done now or the implications for the use of NHS assets. Think about not just the written submission but any other adjudication processes
such as an interview. Who should attend? For what reason? Imagine what your competitors might do





![Acute or chronic pulmonary emphysema? Or both?—A ......emphysema or acute alveolar dilation, respectively [3 , 5]. In some cases, an interstitial emphysema is described [, 636].](https://static.fdocuments.in/doc/165x107/6138f505a4cdb41a985b64ce/acute-or-chronic-pulmonary-emphysema-or-bothaa-emphysema-or-acute-alveolar.jpg)