Congestive Heart Failure & Rheumatic Fever
description
Transcript of Congestive Heart Failure & Rheumatic Fever


Define congestive heart failure. Discus Pathophysiology of CHF. Explain clinical manifestations of CHF. Identify therapeutic management of
CHF. Discus nursing considerations of CHF. Explain clinical manifestations of
rheumatic fever. Identify therapeutic management of
rheumatic fever. Discus nursing considerations of
rheumatic fever.

Is inability of the heart to pump an adequate amount of
blood to the systemic circulation at normal filling
pressures to meet the metabolic demands of the
body.



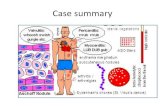
Right sided failure The right ventricle is unable to pump blood effectively into the pulmonary artery Resulting in
Increased pressure in the right atrium and systemic venous
circulation
Hypertension Causes
Hepatosplenomegaly and edema

In left sided failure The left ventricle is unable to pump blood
into the systematic circulation Resulting in
Increased pressure in the left atrium and pulmonary veins
Lungs become congested with blood Causing
Pulmonary pressure and pulmonary edema

Impaired myocardial
function
Pulmonary congestion
Systemic venous
congestion• Tachycardia • Sweating • urine output• Fatigue • Weakness,
restlessness• Anorexia • Pale, cool
extremities• Weak
peripheral pulse
• Tachypnea• Dyspnea,
cyanosis • Exercise
intolerance • Orthopnea • Cough,
hoarseness , wheezing
• Weight gain• Hepatomegaly• Peripheral
edema• Ascites• Neck vein
distention (children).

1. Clinical symptoms Tachypnea and tachycardia at rest Dyspnea, activity intolerance
(during feeding in infants). Weight gain.2. A chest X ray
(Cardiomegaly).3. E C G

1. Improve cardiac function ( increase contractility).
Through administration of digitalis glycosides
The beneficial effects of digitalis are: Increase cardiac output. Decrease heart size. Decrease venous pressure. Relief of edema.

2. Remove accumulated fluid and sodium.
Administration of diuretics Fluid and sodium restriction3. Decrease cardiac workload Limiting physical activity (bed rest). Treating any infections Reducing the effort of breathing
( semi fowler position). Using medication to sedate an
irritable child. 4. Improve tissue oxygenation

Hospitalized Positioning Monitored cardiac and respiratory
function Pulse oximeter Urine output and serum
electrolytes are evaluated.

1. Assist in measures to improve cardiac function
Calculating and administrating the correct dosage of digoxin.
The child’s apical pulse is always checked before administering digoxin.
Not given if the pulse is below 90 b/m in infants and young children.
Or below 70b/m in older children.

Observing for signs of digoxin toxicity
Nausea Vomiting Anorexia Bradycardia

Give digoxin at regular intervals. Do not mix it with other foods or
fluids (inaccurate intake of drug). If a dose is missed more than 4 hours
has , withhold the dose and give the next dose at the regular time, if less than 4 hours give the missed dose.
If the child vomits do not give a second dose.
Do not increase or double the dose for missed dose.
In case of accidental overdose of digoxin call the nearest poison center immediately.

2. Decrease cardiac demands (workload) Uninterrupted period of sleep. Minimize disturbing the infant
(changing bed linen, bathing). The child is fed when hungry. Because infants with CHF tire easily
and may sleep through feeding, smaller feedings every 3 hours may helpful.
Avoid crying

Temperature carefully monitored ( hypothermia or hyperthermia increase the need of oxygen).
Skin breakdown from edema is prevented with change of position every 2 hours ( from side to side within semi fowler position).

3. Reduce respiratory distress Careful assessment. Positioning and oxygen
administration. Respirations are counted for full
minute. Protected from infections. Good hand washing.

4. Maintain nutritional status
Infant do not have the energy to do extra work even feeding.
The nurse seeks measures to enable the infant to feed easily without excess fatigue and to increase the caloric density of the formula.
The infant should be rest before feeding .
A 3-hour feeding schedule works.

Infants should be feed in a semi upright position.
Gavage feeding for infant with feeding difficulties.
A large nipple opening, decreases the energy expenditure of the infant while sucking.

5. Assist in measures to promote fluid loss.
Record fluid intake and output and monitors body weight.
Diuretics should be given early in the day.
If potassium losing diuretics are given, the nurse encourage foods high in potassium.
Fluid restriction. 6. Support child and family.

Is an inflammatory disease that occurs after infection with group AB hemolytic streptococcal Pharyngitis.
It is involves the joints, skin, brain, serous surfaces and heart.
The most significant complication of
RF is Rheumatic heart diseases.

Previous infection with group A- streptococcal
infection.
Prevention or treatment of
group A streptococcal
infection prevents RF.

Major manifestations: fever and arthralgia recent streptococcal infections.
Tested for streptococcal antibodies ( elevated of antistreptolysin-O (ASLO) .

Major manifestations. 1. Carditis Tachycardia out of proportion of
fever. Cardiomegaly. Chest pain.
2. Polyarthritis Swollen, hot , red, painful joints. Favors large joints (knees, elbows,
hips, shoulders, wrists).

3. Erythema marginatum Nonpruritic Affects trunk and extremities (inner
surfaces).
4. Chorea Sudden aimless, irregular
movements of extremities. Involuntary facial grimaces. Speech disturbances.


5. Subcutaneous nodes Nontender swelling. Located over bony prominences.
6. Supporting evidence Positive throat culture

Goals Eradication of hemolytic
streptococci. Prevention of permanent cardiac
damage. Palliation of the other symptoms. Prevention of recurrences of RF.

Penicillin is the drug of choice. Erythromycin
Salicylattotes control inflammatory process especially in the ( joints and reduce fever).
Prophylactic treatment against recurrence of RF (monthly IM injections of benzathine penicillin G).
Followed medically for at least 5 years.

Encourage adherence to the therapeutic plan.
Providing rest and adequate nutrition.
If Carditis is present, activity restrictions.
Prevention, primarily in screening school age children for sore throats caused by group A streptococci.
Throat culture screening programs.