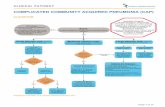
Community Acquired Pneumonia
description
Transcript of Community Acquired Pneumonia

Community Acquired Pneumonia
Lisa Bennett RN, BSNMSN 621, FridayMarch 1, 2012
(Background:Microsoft Images)

Community Acquired Pneumonia
Community Acquired Pneumonia (CAP) is an acute infection of lung tissue that develops outside of the hospital setting. CAP is the leading cause of death from infection in the United States. The most common bacterial cause of CAP is streptococcus pneumoniae which will be the focus of this tutorial.
(Cochrane 2009)

At the completion of this tutorial you will be able to :
• Describe the pathophysiology of CAP• Identify the populations at risk for CAP• Recognize the common signs and symptoms
of CAP• Determine which tests will help to diagnose
CAP• Report the current guidelines for the
management of CAP

Mr. Congestion
Mr. C is a 70 year old male that presents to the primary care clinic where you work. He is accompanied by his daughter. Mr. C’s daughter states that Mr. C has a bad cold with a cough and that he has been confused. He fell as he was getting dressed this morning.

To understand CAP a review of the Inflammatory Response is needed:
(Bowne 2012)

Four Stages of Pathologic Process of Pneumococcal Pneumonia
Edema: Build up of fluid containing protein and bacteria accumulates in the air sacs of the lungs
Red Hepatization: An excess of fluid in the capillaries of the air sacs causes an influx of many white and red blood cells
Gray Hepatization: Macrophages come to the rescue engulfing the white blood cells, red blood cells and other cellular debris
Resolution: Alveolar exudate is then removed and the lung gradually returns to normal
(Porth 2009)

Bacteria commonly enter the respiratory tract, but do not normally cause pneumonia. When pneumonia does occur, it is the result of:
1.A very virulent microbe2.A large “dose” of bacteria3.An impaired host defense mechanism
(Waterer et al 2010)

Factors that Interfere with Respiratory Defense Mechanisms
Mechanisms Function Factors That Impair Nose and throat defenses • IgA protects again the multiplying
of bacteria• Sneezing removes bacteria from
respiratory tract
• Decreased IgA • Nasal inflammation caused by
allergies• Common cold• Trauma to the nose
Cough reflexes Protect against aspiration Reduced cough reflex r/t•Stroke•neuromuscular diseases•sedation•anesthesia
Muociliary clearance system Cilia remove bacteria from respiratory passages
• Smoking• Viruses • Cold, dry air
Alveolar macrophage Removes bacteria from alveoli • Cold, dry air• Alcohol use• Smoking• Obstruction
IgG and IgM Help to remove bacteria from the blood
• IgG deficiency• IgM deficiency
(Porth 2009)

Back to Mr. C
Past Medical History:•20 year smoking history•Coronary Artery Disease•Recovering alcoholic•History of asthma (currently tapering off corticosteroids for recent exacerbation)

Quick Review: Why is Mr. C at increased risk for developing CAP?
History of Smoking
Yes, smoking reduces the ability to remove
bacteria
Corticosteroids
Yes, immune system is compromised with steroid use
History of Alcoholism
Yes, decreases ability to remove
bacteria from alveoli

(Wikipedia 2012)

Common Signs & Symptoms Indicative of CAP Caused by Streptococcus Pneumoniae
• Sudden onset• High fever• Shaking chills• Productive cough – watery at first and then
becomes blood tinged• Pleuritic pain
(Porth 2009)

Mr C’s Physical Assessment
Low grade fever
Yes! Trick question: Fever is less likely to
be elevated in elderly
Productive cough
Yes! WBCs, RBCs and exudate are coughed
up
Pain with Breathing
Yes! Inflammation in lung tissue can lead to pain with inspiration
Mr. C has an oral temperature of 100 degrees. His blood pressure is 138/70, heart rate is 90 and respiratory rate is 34. You notice that he is using accessory muscles to breath. He reports pain on inspiration when you auscultate his lungs. You are able to hear crackles in the left lower lobe. Mr C begins to cough and grabs a tissue to spit out blood tinged sputum. You obtain his pulse ox and find that it is 90%.

Clinical Assessment FindingsIndicative of CAP
• High Fever • Rapid, shallow breathing• Tachycardia• Decreased breath sounds• Adventitious breath sounds• Leukocytosis

Diagnostic Testing
• Chest Radiograph • Pulse Oximetry (Pulse Ox)• White Blood Cell Count (WBC)• Blood Urea Nitrogen (BUN)• Sputum culture

Normal Pneumonia
(Wikipedia 2012)
Chest RadiographMay show hyper-expansion, atelectasis or infiltrates

(Wikipedia 2012)
Pulse Ox
Evaluate for HypoxemiaInflammation, edema and infection decreases perfusion

(Microsoft Images)
Laboratory Tests• WBC-(leukocyte count) increases with the presence
of infection• BUN-measures the level of nitrogen in the blood
derived from urea. An elevated BUN can indicate dehydration or impaired kidney function
• Sputum Culture-identifies causative bacteria to determine antibiotic therapy required to treat CAP

CURB-65Prediction Rule to Assist in Determining Site of Care
• Confusion (disorientation to person, place or time)
• Urea (BUN > 7 mmol/L)
• Respiratory Rate (RR > 30 breaths/minute)
• Blood Pressure (systolic< 90 mmHg-diastolic< 60 mm Hg)
• 65 (years of age or greater)
One point for each prognostic variable 0-1 treat as outpatient, 2 general inpatient admission,
3-5 intensive care admission
(Uptodate 2012)

Use the CURB-65 Scale to determine where Mr. C’s pneumonia will be managed
Outpatient
Sorry! Mr. C has 3 out of 5 predictive
indicators which means that he should
be admitted to the intensive care unit
Hospitalize on General Inpatient Floor
Almost Correct! Yes, Mr. C should be admitted.
3/5 predictive indicators shows that intensive care observation is
needed
Hospitalize in the Intensive Care Unit
Yes! Mr. C has 3 out of 5 predictive indicators
which would guide us to admit him for care in the
intensive care unit

Medical Management
• You decide to admit Mr. C to the hospital for IV antibiotics, oxygen therapy and monitoring
• You repeat his lab work upon admission because the sample drawn in the clinic has hemolyzed
• Empiric treatment is based on presumptive diagnosis of pneumococcal pneumonia– Combination therapy of Beta-lactam and macrolide
• Oxygen is administered via nasal cannula to maintain pulse ox > 93%
(Mandell et al 2007)

In less than 72 hours Mr. C is off his oxygen, on a general care inpatient unit and is changed to oral
antibiotics. His discharge planning will include:
• Smoking cessation • Yearly influenza vaccination• Pneumococcal vaccination with booster in 5
years• Importance of fluid intake

Let’s Review• Community Acquired Pneumonia CAP is the
leading cause of infectious death in the U.S.• Streptococcus Pneumoniae is the most common
cause of CAP• Compromised defense mechanisms put
individuals at risk for developing CAP• Empiric therapy is based on presumptive cause of
CAP• Age and co-morbid disease increase risk and
morbidity of infection from pneumonia• Prevention education should be included in
anticipatory guidance during clinic visits

References• Alcon, A., Fabregas, N., & Torres, A. (2005). Pathophysiology of
pneumonia. Clinics in Chest Medicine, 26, 39-46. doi:10.1016/j.ccm.2004.10.013
• Boldt, M. D., & Kiresuk, T. (2001). Community-acquired pneumonia in adults. The Nurse Practitioner, 26(11), 11-23. Retrieved from www.tnpj.com
• File, T. (2011, October 4). Treatment of community-acquired pneumonia in adults in the outpatient setting. Retrieved February 23, 2012 from UpToDate online textbook: http://www.uptodate.com
• File, T. (2011, October 15). Treatment of community-acquired pneumonia in adults who require hospitalization. Retrieved February 23, 2012 from UpToDate online textbook: http//www.uptodate.com
• Fung, H. B., & Monteagudo-Chu, M. O. (2010). Community-acquired pneumonia in the elderly. The American Journal of Geriatric Pharmacoltherapy, 8(1), 47-62. doi:10.1016/j.amjopharm.2010.01.003

References
• Haessler, S., & Schimmel, J. J. (2012). Managing community-acquired pneumonia during flu season. Cleveland Clinic Journal of Medicine, 79, 67-78. doi:10.3949/ccjm.79a.11108
• LM, B., TJM, V., & MM, K. (2009). Antibiotics for community acquired pneumonia in adult outpatients. The Cochrane Library, i-31. Retrieved from www.thecochranelibrary.com
• Mandell, L. A., Wunderink, R. G., Anzueto, A., Bartlett, J. G., Campbell, G. D., Dean, N. C.,...Whitney, C. G. (2007). Infectious diesease society of american/american thoracic society consensus guidelines on the management of community-acquired pneumonia in adults. Clinical Infectious Diseases, 44, S27-S72. doi:10.1086/511159
• Niederman, M. S. (2004). Review of treatment guidelines for community-acquired pneumonia. The American Journal of Medicine, 117, 51S-57S. doi:10.1016/j.amjmed.2004.07.008

References• Porth, C. M., & Matfin, G. (2009). Pathophysiology: Concepts of altered
health states (8th ed.). Philadelphia, PA: Lippincott Williams & Wilkins.• Waterer, G. W., Rello, J., & Wunderlink, R. G. (2010). Management of
community-acquired pneumonia in adults. American Journal of Respiratory Critical Care Medicine, 183(), 157-164. Doi: 10.1164/rccm.201002-0272CI
• http://faculty.alverno.edu/bowneps/inflammation/inflammprint.htm retrieved February 23, 2012 with permission
• http://en.wikipedia.org/wiki/Pneumonia retrieved February 23, 2012 with permission