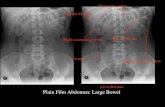
Colon disease Dr.mohammadzadeh. Arterial blood supply to the colon.
-
Upload
lee-lambert -
Category
Documents
-
view
215 -
download
1
Transcript of Colon disease Dr.mohammadzadeh. Arterial blood supply to the colon.

Colon diseaseDr.mohammadzadeh

Arterial blood supply to the colon

Venous drainage of the colon

The lining of the anal canal.

The distal rectum and anal canal

Arterial supply to the rectum and anal canal

Inflammatory Bowel Disease• Inflammatory bowel disease includes ulcerative colitis, Crohn's
disease, and indeterminate colitis. • Ulcerative colitis occurs in eight to 15 people per 100,000 in the
United States and Northern Europe. • The incidence is considerably lower in Asia, Africa, and South
America.• Ulcerative colitis incidence peaks during the third decade of life and
again in the seventh decade of life. • The incidence of Crohn's disease is slightly lower, one to five people
per 100000. • In 15% of patients with inflammatory bowel disease, differentiation
between ulcerative colitis and Crohn's colitis is impossible; these patients are classified as having indeterminate colitis

Principles of Nonoperative Management
: SalicylatesSulfasalazine (Azulfidine), 5-ASA, and related compounds• Antibiotics• Corticosteroids• Immunosuppressive Agents

Indications for surgery in ulcerative colitis
• Emergency surgery : massive life-threatening hemorrhage, toxic megacolon, or fulminant colitis who fail to respond
rapidly to medical therapy

Con…
• Indications for elective surgery : intractability despite maximal medical
therapy high-risk development of major complications
of medical therapy, such as aseptic necrosis of joints secondary to chronic steroid use.
In patients at significant risk of developing colorectal carcinoma.

• Risk of malignancy increases with pancolonic disease and the duration of symptoms is approximately 2% after 10 years, 8% after 20 years, and 18% after 30 years

Indications for Surgery in Crohn
• In Crohn's disease, it is impossible to remove all of the at-risk intestine; therefore, surgical therapy is reserved for complications of the disease.
• fistulas and/or intra-abdominal abscesses.• strictures

Crohn's Colitis
• fulminant colitis or toxic megacolon.
• In this setting, treatment is identical to treatment of fulminant colitis and toxic megacolon secondary to ulcerative colitis.

Anal and Perianal Crohn's Disease
• Anal and perianal manifestations of Crohn's disease are very common.
• Anal or perianal disease occurs in 35% of all patients with Crohn's disease.
• Isolated anal Crohn's disease is uncommon, affecting only 3 to 4% of patients.

• The most common perianal lesions in Crohn's disease are skin tags that are minimally symptomatic.
• Fissures also are common. Typically, a fissure from Crohn's disease is particularly deep or broad and perhaps better described as an anal ulcer. They often are multiple and located in a lateral position rather than anterior or posterior midline as seen in an idiopathic fissure in ano.
• Perianal abscess and fistulas are common and can be particularly challenging. Fistulas tend to be complex and often have multiple tracts .
• Hemorrhoids are not more common in patients with Crohn's disease than in the general population, although many patients tend to attribute any anal or perianal symptom to "hemorrhoids."

Nomenclature
•Diverticulum = sac-like protrusion of the colonic wall
•Diverticulosis = describes the presence of diverticuli
•Diverticulitis = inflammation of diverticuli

Epidemiology
•Before the 20th century, diverticular disease was rare
•Prevalence has increased over time–1907 First reported resection of complicated
diverticulitis by Mayo–19255-10%–196935-50%

Epidemiology
•Increases with age
–Age 40<5%
–Age 6030%
–Age 8565%

Epidemiology
•Gender prevalence depends on age
–M>>FAge less than 40
–M > FAge 40-50
–F > MAges 50-70
–F>>MAges > 70

Anatomic location of diverticuli varies with the geographic location
•“Westernized” nations (North America, Europe, Australia) have predominantly left
sided diverticulosis
–95% diverticuli are in sigmoid colon
–35% can also have proximal diverticuli
–4% have only right sided diverticuli

Anatomic location of diverticuli varies with the geographic location
•Asia and Africa diverticulosis in general is rare and usually right sided
–Prevalence < 0.2%
–70% diverticuli in right colon in Japan

What exactly is a diverticulum?
–True diverticulum contains all layers of the GI wall (mucosa to serosa)
–Colonic pseudo-diverticulum more like a local hernia
•Mucosa-submucosa herniates through the muscle layer (muscularis propria) and then is only covered by serosa


Pathophysiology
•Diverticuli develop in ‘weak’ regions of the colon. Specifically, local hernias develop
where the vasa recta penetrate the bowel wall

Mucosa
Submucosa
Muscularis
Serosa
Vasa recta

Pathophysiology
•Law of Laplace: P = kT / R
•Pressure = K x Tension / Radius
•Sigmoid colon has small diameter resulting in highest pressure zone

Pathophysiology
•Segmentation = motility process in which the segmental muscular contractions separate the lumen into chambers
•Segmentation increased intraluminal pressure mucosal herniation Diverticulosis
–May explain why high fiber prevents diverticuli by creating a larger diameter colon and less vigorous segmentation


Uncomplicated diverticulosis
•Usually an incidental finding at time of colonoscopy



Uncomplicated diverticulosis
•Considered ‘asymptomatic ’
•However, a significant minority of patients will complain of cramping, bloating, irregular
BMs, narrow caliber stools–IBS?–Recent studies demonstrate motility abnormalities
in pts with ‘symptomatic’ uncomplicated diverticulosis

Uncomplicated diverticulosis
•Treatment: Fiber–Bulk content reduces colonic pressure preventing
underlying pathophysiology that lead to diverticulosis
–20 to 30 g fiber per day is needed; difficult to get with diet alone

Pathophysiology of Diverticulitis
•Erosion of diverticular wall from increased intraluminal pressure inflammation focal
necrosis perforation
•Usually inflammation is mild and microperforation is walled off by pericolonic
fat and mesentery

Diagnosis of Diverticulitis
•Classic history: increasing, constant, LLQ abdominal pain over several days prior to
presentation with fever–Crescendo quality – each day is worse–Constant – not colicky–Fever occurs in 57-100% of cases
•In one study, less than 17% of pts with diverticulitis had symptoms for less than 24 hours

Diagnosis of Diverticulitis
Right sided diverticulitis tends to cause RLQ abdominal pain; can be difficult to distinguish
from appendicitis

Diagnosis of Diverticulitis
•Clinically, diagnosis can be made with typical history and examination
•Radiographic confirmation is often performed –Rules out other causes of an acute abdomen–Determines severity of the diverticulitis




Uncomplicated diverticulitis
•Bowel rest or restriction–Clear liquids or NPO for 2-3 days –Then advance diet
•Antibiotics

Uncomplicated diverticulitis
•Antibiotics–Coverage of fecal flora
•Gram negative rods, anaerobes
–Common regimens•Cipro + Flagyl x 10 days

Uncomplicated diverticulitis
•After resolution of attack high fiber diet with supplemental fiber

Uncomplicated diverticulitis
•Follow-up: Colonoscopy in 4-6 weeks
•Flexible sigmoidoscopy and BE reasonable alternative
•Purpose–Exclude neoplasm–Evaluate extent of the diverticulosis

Prognosis after resolution
•30-40% of patients will remain asymptomatic
•30-40% of pts will have episodic abdominal cramps without frank diverticulitis
•20-30% of pts will have a second attack

Prognosis after resolution
•Second attack–Risk of recurrent attacks is high (>50%)
–Some studies suggest a higher rate (60%) of complications (abscess, fistulas, etc) in a second
attack and a higher mortality rate (2x compared to initial attack)
•After a second attack elective surgery

Prognosis after resolution
•Some argue in the elderly recurrent attacks can be managed with medications
•Some argue elective surgery should be considered after a first attack in
–Young patients under 40-50 years of age–Immunosuppressed

Complicated Diverticulitis
•Peritonitis–Resuscitation–Antibiotics
•Ampicillin + Gentamycin + Metronidazole•Imipenem/cilastin
–Emergency exploration–Mortality 6% purulent peritonitis and 35% fecal
peritonitis

Complicated Diverticulitis: Abscess
•Occurs in 16% of patients with acute diverticulitis
•Percutaneous drainage followed by single stage surgery in 60-80% of patients

Complicated Diverticulitis: Abscess
•CT guided drain–Leave in until drain output less than 10 mL in 24
hours
–May take up to 30 days
–Catheter sinograms helpful to show persistent communication between abcess and bowel

Complicated Diverticulitis: Fistulas

Complicated Diverticulitis: Fistulas
•Major types–Colovesical fistula65%–Colovaginal25%–Coloenteric, colouterine10%

Complicated Diverticulitis: Fistulas - Symptoms
•Passage of gas and stool from the affected organ
•Colovesical fistula :–pneumaturia, dysuria, fecaluria
–50% of patients can have diarrhea and passage of urine per rectum

Complicated Diverticulitis: Fistulas
•Diagnosis–CT: thickened bladder with associated colonic
diverticuli adjacent and air in the bladder–BE: direct visualization of fistula track only occurs
in 20-26% of cases–Flexible sigmoidoscopy is low yield (0-3%)–Some argue cystoscopy helpful

Complicated Diverticulitis: Treatment of Fistulas
•Surgery–Resection of affected colon (origin of the fistula)–Fistula tract can be “pinched off” most of the time –Suture closure for larger defects–Foley left in 7-10 days

Diverticular bleeding
•Most common cause of brisk hematochezia (30-50% of cases)
•15% of patients with diverticulosis will bleed
•75% of diverticular bleeding stops without need for intervention

Diverticular bleeding
Patients requiring less than 4 units of PRBC/ day 99% will stop bleeding
Risk of rebleeding 14-38%
After second episode of bleeding, risk of rebleeding 21-50%

Diverticular bleeding: Pathophysiology
•Diverticulum herniates at site of vasa recta•Over time, the vessel becomes draped over
the dome of the diverticulum separated only by mucosa
•Over time, there is segmental weakening of the artery ruptures and bleeds

Diverticular bleeding: Pathophysiology

Diverticular bleeding: Pathophysiology

Diverticular bleeding: Symptoms
•Most only have symptoms of bloating and diarrhea but no significant abdominal pain
–Painless hematochezia–Start – stop pattern; “water faucet”
•Diverticulitis rarely causes bleeding

Diverticular bleeding: Localization
•Right colon is the source of diverticular bleeding in 50-90% of patients
•Possible reasons–Right colon diverticuli have wider necks and
domes exposing vasa recta over a great length of injury
–Thinner wall of the right colon

bleeding:Diverticular Localization
Colonoscopy after rapid prep–Can localize site of bleeding
–Offers possible therapeutic intervention (cautery, clip, etc)
–Often limited by either brisk bleeding obscuring lumen OR no active bleeding with clots in every
diverticuli

Diverticular bleeding:Management

Diverticular bleeding: Localization
•Angiography–Accurate localization
•30-47% sensitive•100% specific
–Need brisk active bleeding: 0.5-1 mL/min
–Offers therapy: embolization, vasopressin•20% risk of intestinal infarction

Diverticular bleeding: Surgery
•Surgery–Segmental resection
•If site can be localized•Rebleeding rate of 0-14%
–Subtotal colectomy•Rebleeding rate is 0%•High morbidity (37%) •High mortality (11-33%)

Hemorrhoids
• Hemorrhoids are cushions of submucosal tissue containing venules, arterioles, and smooth-muscle fibers that are located in the anal canal.
• hemorrhoidal cushions are found in the left lateral, right anterior, and right posterior positions

The distal rectum and anal canal

• Excessive straining, increased abdominal pressure, and hard stools increase venous engorgement of the hemorrhoidal plexus and cause prolapse of hemorrhoidal tissue.

External hemorrhoids• located distal to the dentate line and are covered with anoderm.
• Because the anoderm is richly innervated, thrombosis of an external hemorrhoid may cause significant pain.
• A skin tag is redundant fibrotic skin at the anal verge, often persisting as the residua of a thrombosed external hemorrhoid. Skin tags are often confused with symptomatic hemorrhoids.
• External hemorrhoids and skin tags may cause itching and difficulty with hygiene if they are large.
• Treatment of external hemorrhoids and skin tags are only indicated for symptomatic relief

Internal hemorrhoids
• located proximal to the dentate line and covered by insensate anorectal mucosa.
• Internal hemorrhoids may prolapse or bleed, but rarely become painful unless they develop thrombosis and necrosis (usually related to severe prolapse, incarceration, and/or strangulation).

• Internal hemorrhoids are graded according to the extent of prolapse :
• First-degree hemorrhoids bulge into the anal canal and may prolapse beyond the dentate line on straining.
• Second-degree hemorrhoids prolapse through the anus but reduce spontaneously.
• Third-degree hemorrhoids prolapse through the anal canal and require manual reduction.
• Fourth-degree hemorrhoids prolapse but cannot be reduced and are at risk for strangulation

• Combined internal and external hemorrhoids
• Postpartum hemorrhoids
• Portal hypertension and Rectal varices

Treatment
• Medical Therapy• Rubber Band Ligation• Infrared Photocoagulation• Sclerotherapy• Excision of Thrombosed External Hemorrhoids• Closed Submucosal Hemorrhoidectomy• Open Hemorrhoidectomy• Whitehead's Hemorrhoidectomy

Rubber band ligation of internal hemorrhoids.

Technique of closed submucosal hemorrhoidectomy

Complications of Hemorrhoidectomy
• Postoperative pain• Urinary retention• fecal impaction • Bleeding• Infection• incontinence• anal stenosis • ectropion (Whitehead's deformity).

Anal Fissure• A fissure in ano is a tear in the anoderm distal to the dentate line.
• The pathophysiology of anal fissure is thought to be related to trauma from either the passage of hard stool or prolonged diarrhea.
• The vast majority of anal fissures occur in the posterior midline.
• Ten to 15% occur in the anterior midline.
• Less than 1% of fissures occur off midline

• Anal fissure is extremely common.88,89
• Characteristic symptoms include tearing pain with defecation and hematochezia (usually described as blood on the toilet paper).

• An acute fissure is a superficial tear of the distal anoderm and almost always heals with medical management.
• Chronic fissures develop ulceration and heaped-up edges with the white fibers of the internal anal sphincter visible at the base of the ulcer.
• There often is an associated external skin tag and/or a hypertrophied anal papilla internally

Open lateral internal sphincterotomy for fissure in ano

Closed lateral internal sphincterotomy for fissure in ano

Anorectal Sepsis and Cryptoglandular Abscess

Anatomy of perianorectal spaces. Anterior view

lateral view

Pathways of anorectal infection in perianal spaces

Technique of drainage of perianal abscess

Drainage of horseshoe abscess

Fistula in Ano

Goodsall's rule

Intersphincteric fistula with simple low tract

Uncomplicated transsphincteric fistula

Uncomplicated suprasphincteric fistula

Extrasphincteric fistula secondary to anal fistula

Rectal Prolapse
• Rectal prolapse• Procidentia• Internal prolapse• internal intussusception• Mucosal prolapse

• A thorough preoperative evaluation, including colonic transit studies, anorectal manometry, tests of pudendal nerve terminal motor latency, electromyography (EMG), and cinedefecography, may be useful.
• The colon should be evaluated by colonoscopy or air-contrast barium enema to exclude neoplasms or diverticular disease.
• Cardiopulmonary condition should be thoroughly evaluated because comorbidities may influence the choice of surgical procedure

• The primary therapy for rectal prolapse is surgery, and more than 100 different procedures have been described to treat this condition.
• Operations can be categorized as either abdominal or perineal

Transabdominal proctopexy

Perineal rectosigmoidectomy

Volvulus
• Volvulus occurs when an air-filled segment of the colon twists about its mesentery.
• The sigmoid colon is involved in up to 90% of cases, but volvulus can involve the cecum (<20%) or transverse colon

• The symptoms of volvulus are those of acute bowel obstruction.
• Patients present with abdominal distention, nausea, and vomiting.
• Symptoms rapidly progress to generalized abdominal pain and tenderness.
• Fever and leukocytosis are heralds of gangrene and/or perforation

Sigmoid volvulus