Chapter 39 Urinary System. Anatomy and Physiology Review Urinary system consists of two kidneys, two...
Transcript of Chapter 39 Urinary System. Anatomy and Physiology Review Urinary system consists of two kidneys, two...

Chapter 39
Urinary System

Anatomy and Physiology Review
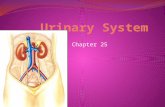
• Urinary system consists of two kidneys, two ureters, bladder, and urethra
• Functions:– Manufacture urine– Expulse waste products

Anatomy and Physiology Review

Anatomy and Physiology Review


Anatomy and Physiology Review

Assessment
• Pain on urination
• Pattern of urination
• Strength of urine stream
• Urgency, frequency, incontinence, hematuria, and nocturia
• Intake and output
• Urine color, clarity, and odor

Urinary Terms
• Anuria– Cessation of urine production
• Dysuria– Difficult urination
• Hematuria– Blood in urine
(continued)

Urinary Terms
• Nocturia– Excessive urination at night
• Oliguria– Decreased urine production
(continued)

Urinary Terms
• Polyuria– Excess urination
• Urgency– Need to urinate immediately

Changes with Aging
• Nephrons decrease
• Glomerular filtration rate decreases
• Blood urea nitrogen increases
• Sodium-conserving ability diminishes
• Bladder capacity decreases
• Renal function increases when lying down
(continued)

Changes with Aging
• Bladder and perineal muscles weaken
• Incidence of stress incontinence increases in females
• Prostate may enlarge in males

Common Diagnostic Tests
• Urine tests
• Blood tests
• Radiographic tests
• Urodynamic tests
• Endoscopic exam
• Biopsy

Common Diagnostic Tests

Common Diagnostic Tests

Urinary Retention
• Person unable to void when an urge– Stasis may lead to infection– May result in distended bladder– Urine overflow may cause incontinence
• Caused by stress, calculus obstruction, stones, tumor, infection, medications, or trauma
(continued)

Urinary Retention
• Symptoms:– Frequency, voiding small amounts, and
distended bladder
• Treatment:– Urinary analgesics, antispasmodics,
catheter, and surgery

Urinary Incontinence
• Involuntary loss of urine from bladder
• Types:– Stress
• Leakage of urine on straining
– Urge• Sudden need to urinate
(continued)

Urinary Incontinence
• Types:– Overflow
• Full bladder leads to leakage
– Total• No control of voiding
– Nocturnal enuresis• Nighttime incontinence
(continued)

Urinary Incontinence
• Goal of treatment:– Keep perineum clean, dry, and intact
(continued)

Urinary Incontinence
• Potential treatment:– Medications– Pelvic floor exercises– Bladder retraining– Catheter insertion– Surgery

Cystitis
• Inflammation of urinary bladder
• Caused by escherichia coli, candida albicans, coitus, prostatitis, and diabetes mellitus
• Treatment:– Culture/sensitivity testing, antimicrobial
medication, and urinary tract analgesic
(continued)

Cystitis
• Increase fluid intake, acidic foods, and intake and output

Pyelonephritis
• Bacterial infection of renal pelvis, tubules, and interstitial tissue of one or both kidneys
• Also known as pyelitis or nephropyelitis
• Treat to prevent from becoming chronic
(continued)

Pyelonephritis
• Treatment:– Urine culture/sensitivity testing, antimicrobials,
antipyretics, analgesics, increase fluids, intake and output, and daily weight

Acute Glomerulonephritis
• Glomerulus within nephron unit becomes inflamed
• May be bacterial or viral
• Treat to prevent renal complications, cardiac complications, and complications to cerebral functioning
(continued)

Acute Glomerulonephritis
• Treatment:– Drug therapy, fluid restriction, monitor labs,
I&O, bed rest, and VS

Chronic Glomerulonephritis
• Slowly progressive, destructive process affecting glomeruli
• Causes loss of kidney function
• Treat to prevent further renal damage and cardiac or cerebral complications
(continued)

Chronic Glomerulonephritis
• Treatment:– Medications, protein and fluid restriction, bed
rest, intake and output, VS, and monitor labs, daily weight, and lung sounds

Urinary Calculi
• Calculus, or stone, formed in urinary tract
• Very small calculi may be flushed out by peristalsis and fluids
• All urine must be strained, stones collected, and sent to lab for composition
(continued)

Urinary Calculi

Urinary Calculi

Urinary Calculi
• Treatment:– Lithotripsy, surgery, analgesics, medications,
and dietary changes

Urinary Bladder Tumors
• May be cancerous or benign papillomas
• Surgery may remove tumor, part of bladder, or entire bladder– Makes urinary diversion necessary
• Other treatment:– Chemotherapy, analgesics, and sometimes
low-residue diet

Urinary Bladder Tumors

Urinary Bladder Tumors

Renal Tumors
• Cancer in kidneys
• Radical nephrectomy may be performed if other kidney healthy and disease localized
• Treatment:– Immunotherapy, targeted therapy, analgesics,
antiemetics, chemotherapy, and radiation• Chemotherapy and radiation provide minimal
benefit

Polycystic Kidney
• Multiple grape-like clusters of fluid-filled cysts develop in and greatly enlarge both kidneys
• Treat to preserve kidney function, prevent infections, and relieve pain
(continued)

Polycystic Kidney
• Control hypertension
• Eventually, may need dialysis or renal transplantation

Renal Failure
• Any acute or chronic loss of kidney function when some kidney function remains
• End-stage renal disease (ESRD)– Total, or nearly total, permanent kidney
failure

Acute Renal Failure (ARF)
• Postrenal– Disrupted urine flow
• Prerenal– Disrupted blood flow to kidney
• Intrarenal– Renal tissue damage
• Often reversible if diagnosed early
(continued)

ARF
• Treat to stabilize kidney function, return to normal using surgery, medications, and dietary restrictions
• Treatment:– Medication, dietary changes, fluid restrictions,
and dialysis (peritoneal or hemodialysis)

Chronic Renal Failure/ESRD
• Slow, progressive condition
• Kidney’s ability to function ultimately deteriorates
• Not reversible
• Multisystem disease process
(continued)

Chronic Renal Failure/ESRD
• Goal:– Preserve remaining kidney function and
prevent complications

Dialysis
• Mechanical means of removing waste from blood
• Hemodialysis– Machine with artificial membrane used to
filter blood
• Peritoneal dialysis– Uses peritoneal lining of abdominal cavity
as membrane through which diffusion and osmosis occur

Dialysis

Kidney Transplantation
• Client must be tissue- and blood-typed to determine compatible donor
• After transplant surgery, immunosuppressive drug therapy to decrease chance of organ rejection
• Greatest complication:– Infection

Chapter 60
Infants with Special Needs:Birth to 12 Months

Hypospadias
• Urethral opening on ventral surface of penis
• Surgically corrected during first year of life

Vesicoureteral Reflux
• Backflow of urine from bladder into ureters and possibly kidneys
• Primary symptom:– Recurrent urinary tract infections
• Treatment:– Preventing urinary tract infections and surgery

Wilms’ Tumor
• Nephroblastoma– One of the most common early childhood
cancers
• Symptoms:– Abdominal mass to side of midline, abdominal
pain, malaise, anemia, and fever
(continued)

Wilms’ Tumor
• Avoid palpating tumor
• Surgery is treatment of choice– Also use chemotherapy and radiation

Chapter 61
Common Problems: 1–18 Years

Urinary System
• Acute poststreptococcal glomerulonephritis
• Nephrotic syndrome
• Enuresis