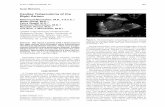
Cases of TBM / Tuberculoma in Pregnancy
Transcript of Cases of TBM / Tuberculoma in Pregnancy

Cases of TBM / Tuberculomain Pregnancy
Presentor : Dr. Hemamalini
Designation : Consultant Physician
Hospital : Fernandez Hospital, Hyderabad
Date of Presentation : 16.09.2014

Case 1- Tuberculoma
Mrs. S.P.,32 yr old, primi
Admitted on 28.05.14 early hours at 38wks GA
Seizures; GTCS at home&twice after admission
BP- 150/90mmHg, pedal oedema 2+, urine albumin
trace
Preeclampsia profile normal ( CBC with platelets,
CUE, s.bilirubin, SGPT, SGOT, s. Cr, LDH, urine C/S)

Peripartum Management
MgSO4 loading 4gm followed by maintenance 1g/hr
Tab Depin SR 10mg tid
Labour induced for antepartum eclampsia
Vaginal delivery of 2.75 kg boy same day
Postpartum enoxaparin 40mg scly for 5days,
nifedepin SR 10mg bd for 2weeks

Postpartum Period
Headache and left upper limb numbness from 7th pnd
Advised MRI/MRV brain by physician on opd basis
Admitted at another hospital following brain imaging
in view of the findings
3weeks and 6weeks after ATT was started, she came
for follow up with our physician

Brain Imaging was Suggestive of Tuberculoma in Rt.Parietal area



Summary
Primi, normotensive through out pregnancy
presenting at term with GTCS; rightly managed as
eclampsia;
later investigated in view of focal neurological
deficit, found to have intracranial lesion.
Presently on ATT and antiepileptics, doing well

Why we are Presenting this case?
Suspect other differential diagnosis in all cases of
eclampsia if
– focal neurological deficits
– persistent headache/ other neurological
symptoms
– Recurrent seizures despite MgSO4
– Prolonged unconsciousness following seizure

Why we are Presenting this case?
– No features of eclampsia like raised BP/ urine protein
– Late onset seizure ( beyond 1week postpartum)
– Fever with seizures ( not explained by other site
infection)
– Partial seizures with or without secondary
generalisation
– Past history suggestive of recurrent headaches +/-
other neurological symptoms

CASE 2 - TBM

History
Mrs. G., 27yr old, G3A2, 22wks gestation
Previous 2 first trimester losses
Evaluated by rheumatologist 2012- ACL IgG low +ve,
IgM –ve, LAC 1.3, ? APLA- repeated after 3months-
same result
HCQs 200mg, prednisolone 5mg started interval
period

Present Pregnancy
Spontaneous conception
Enoxaparin 40mg scly od since conception inview of APLA;
continued HCQs and prednisolone
Dry cough since two months ( from 4/10 gestation) with low
grade fever in evenings (temperature not documented)
Prednisolone stopped after 2weeks after cough started;
received 2 courses of antibiotcs
Seen by two pulmonologists outside in the previous 1 month
before admission with us. CXR not done
Prescribed inhalers/nebulisations- partial relief

Continued..
Thrombocytopenia 50,000 on routine CBC at
5months gestation
Stopped LMWH
Seen by rheumatologist for low platelets, at this
point as she changed the obstetrician
Platelets dropped to 38,000 but no bleeding
manifestations
Restarted prednisolone at 20mg/day

Continued..
Referred to us 3days later with c/o altered behaviour
since 2days- ? Steroid induced psychosis,? Depressive
illness/other psychiatric problem
History reviewed-Headache since 1week; no vomiting
Cough decreased since one week with cough
suppressants, but drowsy
Lethargic, not speaking, not eating since two days.
Ambulating to toilet
Wt. loss 7kg in pregnancy

At FH
Admitted on 4.08.14 in ICU
Normal built and nourished
Drowsy, lethargic, not willing to ambulate; not talking except
occasional muttering
Other general examination unremarkable
PR: 100/min, BP-90/60mmHg, RR: 20/min, temp 99F
No focal neurological deficit, pupils NSRL, mild neck stiffness,
uncooperative for complete neurological examination, fundus
normal
Lungs clear; other systemic examination normal

Investigations
CBC- 10.5G Hb, 5,000/cmm WBC, 46,000 Plt
CUE- protein 2+, pus cells nil; C/S sterile
TSH- 0.09
Na-127, K-4.3, Cl-92
HIV, HBs Ag –ve
LFT, RFT normal. aPTT- 47.9/28.2
PT- 15.9/13.9

CXR- Miliary TB

MRI Brain- Meningeal EnhancementCSF analysis-
Sugar: 18mg/dl
Protein: 199mg/dl
Total cell count- WBC- 36. RBC 18
Polymorphs 65. lymphocytes 35
ADA- 13 (>10, suspect 10-11)
Grams stain- few pus cells, occasional lymphocytes, no microorg
AFB stain: -ve
Fungal stain- no fungal elements
MTB DNA PCR-ve
Cryptococcal antigen –ve
AFB culture positive ( reported after 6weeks)

At FH
Diagnosis of miliary TB with meningoencephalitis was made
Neurophysician input
ATT started + inj Decadron 8mg IV tid given within 24hrs of
admission, IV ceftriaxone 2G bd, enteral nutrition, inj
optineuron infusion daily
Next 24hrs- pt. deteriorated with worsening level of
consciousness ( E2M2V2), pupils NS, sluggishly reacting,
fundus normal;
Platelets 23,000/cmm, WBC 36,000/cmm

At FH
Fetal scan- intraplacental clot, AEDF
Planned for termination of pregnancy after
repeating brain imaging ( CECT), in view of
worsening maternal condition and poor fetal
prognosis
After multidisciplinary counseling , family wanted
patient to be transferred to a neuro centre, hence
discharged

At the other Hospital
MRI repeated- features s/o TBM with communicating
hydrocephalous and secondary ischemic changes; MRA
normal
EVD ( External Ventricular Drain)was placed on the 2nd
day after transfer in view of acute hydrocephalous
Ventilatory support
ATT, steroids, levetiracetam,supportive care continued
Found to have IUFD;SERPC done. Received RDPs

Outside Hospital
Cardiac arrest- revived- brain dead ( EEG)
CT brain
– mild hydrocephalous
– Intraventricular shunt in situ
– Features s/o cerebal edema also seen ( paucity of CSF
sulcal spaces
– No e/o intracranial herniation
Left against medical advise in view of poor prognosis (
later communication- pt. died on the way home)

Summary
Young lady with 2 previous miscarriages, with
probable APLA syndrome ( though 2 first trimester
miscarriages -not an indication for testing for APLA)
On low dose steroids (? not indicated) for a long
duration
Prolonged cough labeled as allergic bronchitis
without CXR
Low grade fever ignored as not documented

Summary
Steroids hiked in view of thrombocytopenia without
taking into consideration her previous history of fever,
cough and wt.loss
Diagnosed as miliary TB with meningoencephalitis at
22wks gestation after altered level of consciousness
Low sodium secondary to SIADH- indicate severe
disease
Rapid neurological deterioration and later cardiac
arrest and brain death

Lessons to be Learnt APLA investigations and diagnosis according to
guidelines only
Asymptomatic APLA in interval period- no need of
treatment
In pregnancy if APLA confirmed: LDA +/- LMWH only (
no indication for steroids unless secondary APLA)
Evaluate cough beyond 3 weeks with CXR- don’t
hesitate as radiation exposure is very minimal- use
abdominal lead shield

Lessons to be learnt
High degree of suspicion for Koch’s in pregnancy if they
are on steroids
Evaluate for other symptoms before increasing steroid
dose in pregnancy
Evaluate for organic causes of brain disorder before
assuming psychiatric problems
Manage in a centre with
neuroimaging/neurophysician/neurosurgeon support if
TBM is diagnosed

Lessons to be learnt
Thrombocytopenia and neurological symptoms-
always brain imaging is indicated
Do not ignore weight loss in pregnancy – has to be
evaluated; need to consider bone TB too as many of
them may be having low backache or other bone
pains
Evaluation for hyperthyroid, secondary APLA in this
case?

Discussion- Miliary TB
Widespread dissemination of Mycobacterium
tuberculosis via hematogenous spread
Classic miliary TB is defined as milletlike (mean, 2 mm;
range, 1-5 mm) seeding of TB bacilli in the lung, as
evidenced on chest radiography. This pattern is seen in
1-3% of all TB cases
Miliary TB may occur in an individual organ (very rare, <
5%), in several organs, or throughout the entire body
(>90%), including the brain

Characterized by a large amount of TB bacilli
May easily be missed; fatal if left untreated
25% of miliary TB - Meningeal involvement
Miliary TB may mimic many diseases
50% of cases are undiagnosed antemortem;
Therefore, a high index of clinical suspicion is
important to obtain an early diagnosis

Risk Factors for Miliary Tuberculosis
Cancer
Transplantation
HIV infection
Malnutrition
Diabetes
Immunosuppression including, but are not limited to, the following:
Silicosis
End-stage renal disease
Major surgical
procedures -
Occasionally may
trigger dissemination

Progressive Symptoms over days to weeks or occasionally over several months
Weakness, fatigue (90%)
Weight loss (80%)
Headache (10%)
Signs of miliary TB include
the following:
Subtle signs, such as low-
grade fever (20%)
Fever (80%)
Cough (60%)
Generalized
lymphadenopathy (40%)
Hepatomegaly (40%)
Splenomegaly (15%)
Pancreatitis (< 5%)
Multiorgan dysfunction,
adrenal insufficiency

Investigations
High-resolution computed tomography (HRCT) is relatively more
sensitive and shows randomly distributed miliary nodules
In extrapulmonary locations, ultrasonography, CT, and magnetic
resonance imaging are useful
Positron-emission tomographic CT has been investigated as a
promising tool for evaluation of suspected TB.
Fundus examination for choroid tubercles, histopathological
examination of tissue biopsy specimens, and rapid culture
methods for isolation of M. tuberculosis in sputum, body fluids,
and other body tissues aid in confirming the diagnosis

Choroidal Tubercles


Coronal plain computed tomography (A) positron-emission tomography (B) images
showing diffuse increased 18F fluorodeoxyglucose uptake in spleen,multifocal
uptake in liver, mediastinal node (black arrow).

Labs Low sodium levels may correlate with disease severity, and the
syndrome of inappropriate secretion of antidiuretic hormone
(SIADH) or hypoadrenalism
30% of cases, alkaline phosphatase levels are elevated
Elevated levels of transaminases suggest liver involvement or, if
treatment has been initiated, drug toxicity
Leukopenia/leukocytosis may be present; Leukemoid reactions
may occur; patients may have anemia; and thrombocytopenia or,
rarely, thrombocytosis may be present.
ESR elevated in approximately 50%

Cultures for Mycobacteria
Include those of the sputum, blood, urine, or cerebral spinal
fluid.
Sensitivity testing is essential for all positive isolates, and
consider investigation for multidrug-resistant TB (MDR-TB)
in all cases.
Negative sputum smear results (even 3 negatives) do not
exclude the possibility of TB.
Blood cultures are positive in approximately 5% of patients
who do not have HIV infection. 85% positivity rate, if HIV +ve

Lumbar Puncture
Strongly considered, even with normal brain MRI
Leukocytes: Approximately 65% of patients have WBC
counts with 100-500 mononuclear cells/μL.
Lymphocytic predominance (70%)
CSF lactic acid levels are mildly elevated
Elevated protein levels (90%)
Low glucose levels (90%)
RBCs are common
Acid-fast bacilli (≥40% with serial spinal taps)

Nucleic Acid Probes / Other Tests Specificity for smear-negative and culture-negative specimens is
lower than 100% (false-negative results).
False-positive TB cultures are of concern (5%). This may be due to
laboratory contamination
Sputum induction has low sensitivity, and findings are smear-
negative and culture-negative in 80% of patients because of
hematogenous spread
Fiberoptic bronchoscopy is the most effective procedure for obtaining
cultures (bronchoalveolar lavage)
The culture yield for transbronchial biopsies is 90%
Bone marrow biopsy yield is approximately 50%, without serious
adverse effect

Treatment
Miliary TB with meningeal involvement may require
prolonged treatment (up to 12 mo).
Early treatment of patients with suspected miliary
tuberculosis decreases the likelihood of mortality
and improves outcome.
Surgical treatment is rarely necessary. Occasionally,
a ventriculoatrial shunt is indicated for
hydrocephalus

Empirical Treatment
Early empirical therapy for suspected miliary
tuberculosis is prudent
Delay of even 1-8 days contributes to a high
mortality rate
Steroids are warranted for hypotension due to
presumed adrenal insufficiency after an
adrenocorticotropic hormone (ACTH) stimulation
test

For MDR-TB, use a minimum of 1 susceptible
injectable and at least 3 additional susceptible
drugs to prevent the development of additional
resistance
Placenta examination by the pathologist is
imperative.
In a newborn, 3 gastric aspirates of the newborn are
helpful;lumbar puncture is indicated if the newborn
does not thrive

Isolation
Usually removed from isolation when 3 consecutive
sputum smear results are negative and clinical
improvement is shown
Must not be confined with immunosuppressed
patients prior to the establishment of negative
sputum cultures
Negative pressure room or in adequate respiratory
isolation is needed

Prognosis of Miliary TB
If left untreated, the mortality associated is assumed
to be close to 100%
With early and appropriate treatment, mortality is
reduced to less than 10%
The earlier the diagnosis, the better the likelihood of
a positive outcome

Prognosis of Miliary TB
Most deaths occur within the first 2 weeks of
admission to the hospital; may be related to
delayed onset of treatment
Relapse rate is 0-4% with adequate therapy and
directly observed therapy; most relapses occur
during the first 24 months after completion of
therapy

Mortality is strongly associated with
Age
Mycobacterial burden
Delay in initiation of chemotherapy
Laboratory markers such as lymphopenia,
thrombocytopenia, hypoalbuminemia, and elevated
hepatic transaminases

Healing in TB following “successful” treatment
results in fibrosis and consequent anatomical and
physiological alterations of the involved organs
Persistence of physiological, immunological, and
radiological defects in miliary TB in spite of
treatment and the observation of sequelae in
treated cases of pulmonary TB patients point out
that these patients will not regain optimal health
despite achieving a microbiological cure


![8 printable Extrapulmonary TB-10.2nid]/8_printable... · •LP: WBC 149, t prot 152, glucose 14 • M ... • Less clear role in tuberculoma or spinal TBM • Dexamethasone 0.4mg/kg/d](https://static.fdocuments.in/doc/165x107/5d3f0c1b88c9937e518c8187/8-printable-extrapulmonary-tb-102-nid8printable-lp-wbc-149-t-prot.jpg)