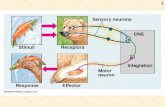
Brain Spinal cord Central nervous system (CNS) Peripheral nervous system (PNS) Figure 22.1 The human...
-
Upload
ada-edith-farmer -
Category
Documents
-
view
337 -
download
4
Transcript of Brain Spinal cord Central nervous system (CNS) Peripheral nervous system (PNS) Figure 22.1 The human...

Brain
Spinal cord
Central nervous system (CNS)
Peripheral nervous system (PNS)
Figure 22.1 The human nervous system.

The Nervous System
Meninges protect brain and spinal cord Dura mater: outermost layer Arachnoid mater: middle layer
Subarachnoid space contains cerebrospinal fluid (CSF)
Pia mater: innermost layer
Blood–brain barrier

Figure 22.2 The meninges and cerebrospinal fluid.
Skull bone
Cerebrum
Cerebellum
Spinal cord
Subarachnoid space of spinal cord
Subarachnoid space (contains cerebrospinal fluid)
Skull bone
Dura mater
Arachnoid mater
Pia mater
Blood vessel
Cerebrum
Cranial meninges
Dura mater
Arachnoid mater
Pia mater
Spinalmeninges
Subarachnoid space (contains cerebrospinal fluid)
Central canal

The Nervous System
Meningitis: inflammation of meninges Encephalitis: inflammation of the brain Meningoencephalitis: inflammation of both

Bacterial Meningitis
Initial symptoms of fever, headache, and stiff neck Followed by nausea and vomiting May progress to convulsions and coma Diagnosis by Gram stain and latex agglutination of
CSF

Figure 22.4 Spinal tap (lumbar puncture).
Spinal cord
Spinal needle is inserted, usually between the fourth and fifth lumbar vertebrae
Fourth lumbar vertebra
Cauda equina
Sample of cerebrospinal fluid
Fifth lumbar vertebra
L4
L5
Cerebrospinal fluid
Longitudinal section of the spine

Haemophilus influenzae Meningitis
Occurs mostly in children (6 months to 4 years) Gram-negative aerobic bacteria, normal throat
microbiota Capsule antigen type b Prevented by Hib vaccine

Neisseria Meningitis
Also called meningococcal meningitis Caused by N. meningitidis
Gram-negative, aerobic cocci with a capsule
10% of people are healthy nasopharyngeal carriers Begins as throat infection, rash Serotypes B, C, Y, W-135 Serotype B & C in United States Serotype A in Africa Vaccination (A, C, Y, W-135 capsule) recommended
for college students

Figure 22.3 Neisseria meningitis.
Cilia
N. meningitidis
N. meningitidis

Streptococcus pneumoniae Meningitis
Also called pneumococcal meningitis Caused by S. pneumoniae (a gram-positive
diplococcus) 70% of people are healthy nasopharyngeal carriers Most common in children (1 month to 4 years) Mortality: 30% in children, 80% in elderly Prevented by vaccination

Listeriosis
Caused by Listeria monocytogenes Gram-negative aerobic rod Usually foodborne; it can be transmitted to
fetus Reproduce in phagocytes Spread phagocyte-to-phagocyte

Figure 22.5 Cell-to-cell spread of Listeria monocytogenes, the cause of listeriosis.
Listeria monocytogenes
Macrophage
Pseudopod
Macrophage

Diseases in Focus: Meningitis and Encephalitis.
Gram stain of cerebrospinal fluid.

Tetanus
Caused by Clostridium tetani Gram-positive, endospore-forming, obligate
anaerobe Grows in deep wounds Tetanospasmin released from dead cells blocks
relaxation pathway in muscles Prevention by vaccination with tetanus toxoid
(DTaP) and booster (Td) Treatment with tetanus immune globulin (TIG)

Advance case of tetanus

Botulism
Caused by Clostridium botulinum Gram-positive, endospore-forming, obligate
anaerobe Intoxication comes from ingesting botulinal toxin Botulinal toxin blocks release of neurotransmitter,
causing flaccid paralysis Prevention
Proper canning Nitrites prevent endospore germination in sausages

Botulism
Treatment: supportive care and antitoxin Infant botulism results from C. botulinum
growing in intestines Wound botulism results from growth of
C. botulinum in wounds

Botulinal Types
Type A toxin 60–70% fatality Found in CA, WA, CO, OR, NM
Type B toxin 25% fatality Europe and eastern United States
Type E toxin Found in marine and lake sediments Pacific Northwest, Alaska, Great Lakes area

Leprosy
Also called Hansen’s disease Caused by Mycobacterium leprae Acid-fast rod that grows best at 30°C Grows in peripheral nerves and skin cells Transmission requires prolonged contact with an
infected person

Leprosy
Tuberculoid (neural) form: loss of sensation in skin areas; positive lepromin test
Lepromatous (progressive) form: disfiguring nodules over body; negative lepromin test

Figure 22.9 Leprosy lesions.
Tuberculoid (neural) leprosy Lepromatous (progressive) leprosy

Poliomyelitis (Polio)
Poliovirus Transmitted by ingestion Initial symptoms: sore throat and nausea Viremia may occur; if persistent, virus can enter the
CNS Destruction of motor cells and paralysis occurs in
<1% of cases Prevention: vaccination (enhanced-inactivated polio
vaccine)

Figure 22.11 Worldwide annual incidence of poliomyelitis.N
um
be
r o
f c
on
firm
ed
po
lio
ca
se
s
1999 2000 2001
Year
2002 2003 2004 2005 2006 2007 2008 2009 2010
2008 2009 2010
0
1,000
2,000
3,000
4,000
5,000
6,000
7,000
0
1,000
2,000

Rabies
Caused by the rabies virus Transmitted by animal bite Furious rabies: animals are restless, then highly
excitable Paralytic rabies: animals seem unaware of
surroundings

Figure 22.12 Pathology of rabies infection.
Virus enters tissue from saliva of biting animal.
Virus replicates in muscle near bite and enters neuron of peripheral nervous system.
Virus moves up peripheral nervous system to CNS.
Virus ascends spinal cord.
Virus reaches brain and causes fatal encephalitis.
Virus enters salivary glands and other organs of victim.

Figure 22.13 Reported cases of rabies in animals.
Skunk
Fox
Raccoon
Fox and skunk
KEY
Areas of the United States in which rabies predominates in certain wildlife species. Rabies-infected bats were reported in 47 of the 48 contiguous states. In eastern states in which raccoons are the predominant rabies-infected animal, many cases were also reported in foxes and skunks.

Figure 22.13 Reported cases of rabies in animals.
KEY
Rabies cases in various wild and domestic animals in the United States. Rabies in domestic animals such as dogs and cats is uncommon because of high vaccination rates. Raccoons, skunks, and bats are the animals most likely to be infected with rabies. Most human cases are caused by bites of bats. Worldwide, most human cases are caused by bites of dogs.
Raccoons
Bats
Skunks
Foxes
Cats
Dogs
Cattle
Horses/mules
Wild
Domestic
35.5%
24.8%
24.5%
7.7%
4.6%
1.2%
1.1%
0.6%
0 10 20 30 40 50

Clinical Focus: A Neurological Disease, Figure B.
Silver-haired bat.

Rabies Virus
Virus multiplies in skeletal muscles and then brain cells, causing encephalitis
Initial symptoms may include muscle spasms of the mouth and pharynx and hydrophobia

Prevention of Rabies
Preexposure prophylaxis: injection of human diploid cells vaccine (HDCV)
Postexposure treatment: vaccine plus rabies immune globulin (RIG)

Cryptococcus neoformans Meningitis
Also called cryptococcosis Soil fungus associated with pigeon and chicken
droppings Transmitted by the respiratory route; spreads
through blood to the CNS Mortality up to 30% Treatment: amphotericin B and flucytosine

Figure 22.15 Cryptococcus neoformans.
Capsule

Chronic Fatigue Syndrome
Also called myalgic encephalomyelitis (ME) Unexplained fatigue that lasts at least 6 months,
plus four of these symptoms: Sore throat Tender lymph nodes Muscle pain Pain in multiple joints Headaches Unrefreshing sleep Malaise after exercise Impaired short-term memory or concentration

Chronic Fatigue Syndrome
Experimental treatment promotes antiviral interferons