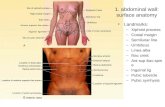
Board review abdomen 9.4.13
-
Upload
nikita-joshi -
Category
Health & Medicine
-
view
326 -
download
2
description
Transcript of Board review abdomen 9.4.13

Board ReviewAbdominal Pathology
Nikita Joshi, MD9/4/13
References:Peer 8Rivers

Moment for a selfish plug for myself.. On behalf of your education!
@njoshi8#EMConf#EMBoardReview#FOAM#FOAMED

15 yo boy presents with abdominal pain. He has been ill for 10 days with malaise, fever, and sore throat. Vitals signs are BP 110/80, pulse 76, respirations 16, and temp 38.3 (100.9F). Physical examination is notable for exudative pharyngitis and an enlarged spleen. Which of the following statements regarding his signs and symptoms is most accurate?
A)Fatigue resolves with pharyngitis symptomsB)Petechiae of the palate is pathognomonicC)Rash is often seen associated with these symptomsD)Splenomegaly is common

15 yo boy presents with abdominal pain. He has been ill for 10 days with malaise, fever, and sore throat. Vitals signs are BP 110/80, pulse 76, respirations 16, and temp 38.3 (100.9F). Physical examination is notable for exudative pharyngitis and an enlarged spleen. Which of the following statements regarding his signs and symptoms is most accurate?
A)Fatigue resolves with pharyngitis symptomsB)Petechiae of the palate is pathognomonicC)Rash is often seen associated with these symptomsD)Splenomegaly is common

What’s the diagnosis?
Infectious mononucleosis
Disease Characteristics?
• Malaise• Exudative pharyngitis• Fever• Lymphadenopathy –
posterior aspect of neck
A – malaise / fatigue can persist for months; pharyngitis resolves after 2-4 wks
B – Petechiae can be seen on soft palate in many types of pharyngitis
C – Rash is seen only occasionally; maculopapular rash develops if pt with EBV is treated with ampicillin or amoxicillin

Exudative Pharyngitis Peritonsillar Abscess
Roberts: Roberts and Hedges' Clinical Procedures in Emergency Medicine,6th ed.Copyright © 2013 Saunders, An Imprint of Elsevier
Acute exudative pharyngitis (A) is characterized by bilateral tonsillar edema, erythema, and exudate. Edema is symmetric, uvula lies midline. A Peritonsillar abscess (B, arrow) is characterized by asymmetric tonsillar bulging, uvula deviated away from the side of the abscess.

A mother brings in her 5 day old daughter for evaluation of sudden-onset, forceful, green colored vomiting. The baby was born at term and at home by spontaneous vaginal delivery; she has no respiratory symptoms. Examination reveals a distended abdomen. Which of the following is the most likely diagnosis?
A)Duodenal atresiaB)Malrotation with midgut volvulusC)Necrotizing enterocolitisD)Tracheoesophageal fistula

A mother brings in her 5 day old daughter for evaluation of sudden-onset, forceful, green colored vomiting. The baby was born at term and at home by spontaneous vaginal delivery; she has no respiratory symptoms. Examination reveals a distended abdomen. Which of the following is the most likely diagnosis?
A)Duodenal atresiaB)Malrotation with midgut volvulusC)Necrotizing enterocolitisD)Tracheoesophageal fistula

What is malrotation with midgut volvulus?
• Infants younger than 1 mon + bilious vomiting• Acute symptoms• Rapidly go into shock
Congenitally malrotated bowel twists on mesentary, near duodenum = obstruction
Compression of superior mesentary artery, vascular compromise

Age Clinical Associations
Key Associations
Malrotation with midgut volvulus
Less than 1 month
• Bilious vomiting (obstruction)
• Shock
• Paucity of small bowel air
• Or normal!
NEC Preterm • Abd distention• Nonbilious
vomiting (ileus)
• Diffuse dilated loops of small bowel
Duodenal Atresia Less than 24 hrs of birth
• Vomiting (bilious or non depedent on atresia location)
• Trisomy 21 (Down synd)
Tracheoesophageal Fistula
Early infancy • Choking, coughing, cyanosis WITH FEEDS
• Rare

Necrotizing Enterocolitis
Kliegman: Nelson Textbook of Pediatrics, 19th ed.Copyright © 2011 Saunders, An Imprint of Elsevier
• Abdominal distention, hepatic portal venous gas (arrow)
• Bubbly appearance of pneumatosis intestinalis (arrowhead). pathognomonic for neonatal necrotizing enterocolitis

Increasing emesis 2-6 week old neonate? Pyloric Stenosis
• Nonbilious projectile vomiting after feeds• Dehyration• Failure to thrive• Olive shaped mass (hypertrophied pylorus)
Hypochloremic, hypokalemic metabolic acidosis

A 64 yo man with history of HTN, diverticulosis, remote abdominal aortic aneurysm repair presents with a 2-day history of black stools, abdominal discomfort, and low grade fever. He is diaphoretic. Vital signs include BP 72/46, pulse 138, and respiratory rate 24. Physical exam reveals a midline abdominal scar, diffuse abdominal tenderness, and bright red blood in his rectum. Two large bore intravenous lines are placed, and fluid resuscitation is begun. What is the appropriate next step in management?
A)Obtain vascular surgery consultationB)Order abdominal and pelvic CT scans and start intravenous antibioticsC)Start nasogastric lavage and obtain endoscopy consultationD)Start proton-pump inhibitor and octreotide infusion

A 64 yo man with history of HTN, diverticulosis, remote abdominal aortic aneurysm repair presents with a 2-day history of black stools, abdominal discomfort, and low grade fever. He is diaphoretic. Vital signs include BP 72/46, pulse 138, and respiratory rate 24. Physical exam reveals a midline abdominal scar, diffuse abdominal tenderness, and bright red blood in his rectum. Two large bore intravenous lines are placed, and fluid resuscitation is begun. What is the appropriate next step in management?
A)Obtain vascular surgery consultationB)Order abdominal and pelvic CT scans and start intravenous antibioticsC)Start nasogastric lavage and obtain endoscopy consultationD)Start proton-pump inhibitor and octreotide infusion

What is the concerning pathophysiology?
• Aortoenteric fistula (AEF) – primary complication of AAA, can occur anytime after repair
• Bowel gets eroded by the aneurysm– Local infection– Abscess– Sentinel bleed from local vessel in bowel
wall

Other answers• Order abdominal and pelvic CT scans and
start intravenous antibioticsConsider scan if pt is STABLE, can show if there
is local infection from fistula• Start nasogastric lavage and obtain
endoscopy consultationHelpful in locating source of bleed?Endoscopy if UGIB• Start proton-pump inhibitor and octreotide
infusionUsed for suspected variceal bleeding

Several people present with facial flushing and throbbing headache 25 minutes after eating tune at a sushi restaurant. What is the most likely diagnosis?
A)Allergic reactionB)Ciguatera poisoningC)Scombroid poisoningD)Tetrodotoxin poisoning

Several people present with facial flushing and throbbing headache 25 minutes after eating tune at a sushi restaurant. What is the most likely diagnosis?
A)Allergic reactionB)Ciguatera poisoningC)Scombroid poisoningD)Tetrodotoxin poisoning

Classic symptoms of scombroid – facial flushing, throbbing headache
Source? Histidine rich dark meat fish, bacteria converts histidine to histamine like substances
Symptoms 20-30 mins post ingestion•Diarrhea, abdominal cramping, hypotension (rarely)•Fish has sharp, metalic, peppery taste
Treatment•Antihistamines•IVF

• Ciguatera (neurotoxin)– 15 mins – 24 hrs– Na channels– Symptoms: GI,
cardiac, neuro– Bradycardia,
paresthesia (hot and cold reversal)
• Tetrodotoxin– Na channel block– Paresthesias – rarely
respiratory paralysis

A 60 yo man with history of cirrhosis presents with abdominal pain and tense ascites. Paracentesis is performed, and the ascitic fluid granulocyte count is 275 cells/mm3. What is the appropriate next step?
A)Discharge with a prescription for pain medicationsB)Obtain surgery consultationC)Start ceftriaxoneD)Wait for culture results

A 60 yo man with history of cirrhosis presents with abdominal pain and tense ascites. Paracentesis is performed, and the ascitic fluid granulocyte count is 275 cells/mm3. What is the appropriate next step?
A)Discharge with a prescription for pain medicationsB)Obtain surgery consultationC)Start ceftriaxoneD)Wait for culture results

???Diagnosis??? How to make the diagnosis???
• Spontaneous Bacterial Peritonitis– Paracentesis– Ascitic fluid analysis, cell count, culture– PMN > 250 = high incidence of SBP– Definitive diagnosis with culture

Spontaneous Bacterial Peritonitis
• IV Ceftriaxone for empiric antibiotic coverage
• Portal hypertension from cirrhosis creates bowel edema, facilitates transmural migration of enteric flora into immunocompromise peritoneal cavity
• Flora: gram negative enterobactera (E.Coli, Salmonella, Klebsiella); Strep Pneumo

Goldman: Goldman's Cecil Medicine, 24th ed.Copyright © 2011 Saunders, An Imprint of Elsevier

50 yo woman presents complaining of a funny feeling in the back of her throat when she swallows; she thinks she has fish bone stuck in her throat. She has no respiratory distress or stridor, and her voice is normal. What is the next step in management?
A)Barium swallowB)BronchoscopyC)Discharge homeD)Plain radiographs

50 yo woman presents complaining of a funny feeling in the back of her throat when she swallows; she thinks she has fish bone stuck in her throat. She has no respiratory distress or stridor, and her voice is normal. What is the next step in management?
A)Barium swallowB)BronchoscopyC)Discharge homeD)Plain radiographs

• Radiographs are indicated in every pt with history suggestive of foreign body ingestion
• Good for radiopaque objects– Directly see object– Indirectly see signs such as soft tissue swelling
• Bronchoscopy useful for visualization and removal
• CT – useful if xrays not diagnostic• Barium swallow – contraindicated if
esophageal perforation suspected• Discharge only after thorough work up

FB in esophagus tend to lodge at area of esophageal narrowing:•Most common site of esophageal foreign body in children?
•Most common site in adults?
- C6 (children less than 4 yrs)- Lower esophageal sphincter / diaphragmatic hiatus (T10-11)

Kliegman: Nelson Textbook of Pediatrics, 19th ed.Copyright © 2011 Saunders, An Imprint of Elsevier
Esophagus-PA view will show flat surface of coin-Lat view will show sagittal plane
Trachea-Lat view will show flat surface of coin-PA view will show sagittal plane
Figure 319-1 Radiographs of a coin in the esophagus. When foreign bodies lodge in the esophagus, the flat surface of the object is seen in the anteroposterior view (A) and the edge is seen in the lateral view (B). The reverse is true for objects in the trachea.

Alkaline Disc Button Battery Ingestion•90% will pass through esophagus•Corrosive•Esophageal strictures, burns, necrosis, perforation
• Double density circular appearance at border• Similar in size to coins

Your heart should skip a beat!
J Paediatr Child Health. 2013 Apr;49(4):330-2. doi: 10.1111/j.1440-1754.2012.02511.x. Epub 2012 Jul 31.Oesophageal complication from button battery ingestion in an infant.
Liao AY, McDonald D.

60 yo man with history of alcohol abuse presents with epigastric pain. Initial laboratory test results are as follows: WBCs 20,000; blood glucose 450; AST 375, lipase 400. What is the appropriate disposition?
A)General medical floorB)ICUC)Observation unitD)Surgical floor

60 yo man with history of alcohol abuse presents with epigastric pain. Initial laboratory test results are as follows: WBCs 20,000; blood glucose 450; AST 375, lipase 400. What is the appropriate disposition?
A)General medical floorB)ICUC)Observation unitD)Surgical floor

NON-GALLSTONE PANCREATITIS (1974)
GALLSTONE PANCREATITIS (1982)
At Admission
Age >55 yr Age >70 yr
White blood cells >16,000/mm3 >18,000/mm3
Blood glucose >200 mg/dL >220 mg/dL
Serum lactate dehydrogenase >350 IU
>400 IU/L
Serum aspartate aminotransferase >250 IU/L
>250 IU/L
During Initial 48 hr
Hematocrit decrease of >10 % >10%
Blood urea nitrogen increase of >5 mg
>2 mg/dL
Serum calcium <8 mg/dL <8 mg/dL
Arterial po2 <60 mm Hg NA
Serum base deficit >4 mEq/L >5 mEq/L
Fluid sequestration >6 L >4 L

Causes of pancreatitis
• Gallstone obstruction• Alcohol abuse• Leads to pancreatic autodigestion

58 yo woman with history of cholelithiasis presents with epigastric abdominal pain, nausea, vomiting, and shortness of breath. She is obese and diaphoretic with diffuse inspiratory crackles. Her current vitals signs are blood pressure 80/40, pulse 135, respirations 45, temperature 99, o2 on room air 70%. Lipase level is 3,000. What is the next appropriate step?
A)Abdominal ultrasonographyB)CTC)Emergent cholecystectomyD)Intubation

58 yo woman with history of cholelithiasis presents with epigastric abdominal pain, nausea, vomiting, and shortness of breath. She is obese and diaphoretic with diffuse inspiratory crackles. Her current vitals signs are blood pressure 80/40, pulse 135, respirations 45, temperature 99, o2 on room air 70%. Lipase level is 3,000. What is the next appropriate step?
A)Abdominal ultrasonographyB)CTC)Emergent cholecystectomyD)Intubation

Severe pancreatitis with Resp Failure (ARDS)
• Pancreatitis leads to release of inflammatory mediators that sets up systemic inflammatory response and multiorgan failure
• Image when making diagnosis on stable pt
• Ultrasound useful if considering gallstones• Treatment: aggressive fluid resuscitation,
pain control• Early cholecystectomy can be dangerous
in pancreatitis – consider ERCP to relieve pancreatic duct obstruction

Adam: Grainger & Allison's Diagnostic Radiology, 5th ed.Copyright © 2008 Churchill Livingstone, An Imprint of Elsevier
Acute respiratory distress syndrome:•Noncardiogenic pulmonary edema•Acute damage to alveoli•Diffuse infiltrative lung lesions with interstitial/alveolar edema•Severe hypoxemia•Respiratory failure•Refractory hypoxemia after damage to alveolar-capillar barrier

Which of the following is the defining triad of hemolytic uremic syndrome?
A)Abdominal distention, headache, hypertensionB)Abdominal pain, purpura, swollen jointsC)Anemia, high creatinine, low plateletsD)Cyanosis, low back pain, vomiting

Which of the following is the defining triad of hemolytic uremic syndrome?
A)Abdominal distention, headache, hypertensionB)Abdominal pain, purpura, swollen jointsC)Anemia, high creatinine, low plateletsD)Cyanosis, low back pain, vomiting

HUS
• Microangiopathic hemolytic anemia• Nephropathy• Thrombocytopenia
• Young children, after minor resp illness or gastroenteritis
• E.Coli O157:H7• Associated symptoms: HTN, irritability,
seizures, abdominal pain, bloody diarrhea, toxic megacolon, intussusception, coma

Abdominal pain, purpura, swollen jointsHenoch-Schonlein purpura
Abdominal distention, headache, hypertensionNephrotic Syndrome
Cyanosis, low back pain, vomitingNothing in particular

3 yo boy is brought in by his mother for evaluation of facial swelling. She says he has been progressively more tired over the past few days, has eaten less than usual, and has had a stomache ache. Vital signs are blood pressure 100/56, pulse 110, resp 20, temp 98.6, and o2 sat 98%. On physical examination, he is awake and alert with very mild tachycardia. He has appreciable swelling of the face, hands, and feet. Lab eval reveals Hgb 15.5, BUN 9, Cr 0.5, albumin 1.8. UA reveals elevated protein but is otherwise normal. Which of the following is the best management strategy for this patient?
A)Admission to a basic pediatric unit for initiation of corticosteroid therapy. B)Admission to an ICU for invasive blood pressure monitoring.C)Diuresis with furosemide in the ED followed by discharge home.D)Emergent hemodialysis in the ED followed by admission.

3 yo boy is brought in by his mother for evaluation of facial swelling. She says he has been progressively more tired over the past few days, has eaten less than usual, and has had a stomache ache. Vital signs are blood pressure 100/56, pulse 110, resp 20, temp 98.6, and o2 sat 98%. On physical examination, he is awake and alert with very mild tachycardia. He has appreciable swelling of the face, hands, and feet. Lab eval reveals Hgb 15.5, BUN 9, Cr 0.5, albumin 1.8. UA reveals elevated protein but is otherwise normal. Which of the following is the best management strategy for this patient?
A)Admission to a basic pediatric unit for initiation of corticosteroid therapy. B)Admission to an ICU for invasive blood pressure monitoring.C)Diuresis with furosemide in the ED followed by discharge home.D)Emergent hemodialysis in the ED followed by admission.

Nephrotic Syndrome - Proteinuria, Hypoalbuminemia, Edema
• Admission to peds floor for nephro eval
• ICU not needed – pt not in shock• Renal failure rare with nephrotic synd• Diuresis not indicated because no
signs of fluid overload

Pediatr Nephrol. 2013 Aug 30. [Epub ahead of print]The nephrotic syndrome: pathogenesis and treatment of edema formation and secondary complications.Cadnapaphornchai MA, Tkachenko O, Shchekochikhin D, Schrier RW.

3 week girl brought in for evaluation of sudden onset explosive bloody diarrhea. She has history of poor weight gain and infrequent stool production. On physical examination, she is not jaundiced but has fever, abdominal distention, and signs of dehydration. She cries weakly when the abdomen is palpated. Rectal examination reveals an empty vault, but at the end of the examination, she has another episode of explosive diarrhea. Which of the following should be included in the management of her condition?
A)Abdominal ultrasonographyB)EsophagogastroduodenoscopyC)Exchange transfusionD)Rectal decompression

3 week girl brought in for evaluation of sudden onset explosive bloody diarrhea. She has history of poor weight gain and infrequent stool production. On physical examination, she is not jaundiced but has fever, abdominal distention, and signs of dehydration. She cries weakly when the abdomen is palpated. Rectal examination reveals an empty vault, but at the end of the examination, she has another episode of explosive diarrhea. Which of the following should be included in the management of her condition?
A)Abdominal ultrasonographyB)EsophagogastroduodenoscopyC)Exchange transfusionD)Rectal decompression

Hirschsprung Disease
• Congenital megacolong• Congenital aganglionosis of colon• Absence of ganglions starts distally at
anus and present for variable distance proximally
• Definitive therapy: surgical resection of aganglionic segment
• ED Management: gastric and rectal decompression, broad spectrum abx, fluid/electrolyte replacement

Clinical Features
• Neonates: failure to pass meconium• Infants brought to the ED: – constipation and obstipation– Vomiting, irritability, and abdominal
distention
• Children who appear ill with fever should be evaluated for enterocolitis and toxic megacolon

• Ultrasound will not be helpful• EGD can assess for UGIB, but minimal
role in LGIB• Exchange transfusion for severe
neonatal jaundice

FIGURE 67-15 Contrast enema demonstrating transition point (arrow) in Hirschsprung's disease.
Townsend: Sabiston Textbook of Surgery, 19th ed.Copyright © 2012 Saunders, An Imprint of Elsevier

55
Good work!

Type Onset Source Characteristics
Treatment Other
Traveler’s DiarrheaE.Coli enterotoxigenic
Abrupt onset
• Fecally contaminated food/water
• Watery diarrhea
• Abdominal cramps
• Oral hydration
• 3-5 days quinolones
Enterohemorrhagic E Coli O157:H7
4-9 days incubation
• Contaminated, undercooked beef
• Shigella-like toxins
• Diarrhea, abd crampy pain, vomiting
• Watery then becomes bloody
• NOT abx due to risk of Hemolytic Uremic Synd (HUS)
• Complications of HUS, TTP
Shigella (dysentery)
1-2 days • Fecal - oral • Fever, crampy abd pain, diarrhea
• Watery / green diarrhea, then bloody mucoid stool
• quinolones • Dehydration
• Reiter’s synd
• HUS• Febrile
seizures• Pneumoniti
s

Type Onset Source Characteristics
Treatment Other
Salmonella Contaminated food / water – eggs, meat
Gastroenteritis, sepsis, typhoid fever, asymptomatic carrier