Bay of Plenty and Lakes Rheumatic Fever Prevention Plan · Bay of Plenty and Lakes Rheumatic Fever...
-
Upload
duongquynh -
Category
Documents
-
view
214 -
download
0
Transcript of Bay of Plenty and Lakes Rheumatic Fever Prevention Plan · Bay of Plenty and Lakes Rheumatic Fever...
1
Bay of Plenty and Lakes Rheumatic
Fever Prevention Plan:
Bay of Plenty DHB
2013 – 2017 (refreshed as at 20 October 2015)
Summary version
2
Foreword In most of the developed world rheumatic fever is thought of as one of those diseases that people used to get. Here in New Zealand it is still very much a problem. It is a particularly cruel illness, often snatching away a child’s or teenager’s potential, just when they should be gaining their confidence and independence. A complication of a seemingly minor throat infection can lead to heart disease, disability and years of treatment. This scenario plays out month after month; the number of cases still unacceptably high and unequally affecting Māori, Pacific and deprived communities.
From 2009, Bay of Plenty and Lakes DHBs have led and funded a comprehensive approach to reduce rheumatic fever, working closely with affected communities. As national awareness of the issue grew, local initiatives have been absorbed into a national drive to prevent rheumatic fever.
The additional focus and funding that has flowed from the national campaign, has had an impact. Data on cases and their management has never been so complete. There is greater awareness of rheumatic fever and its importance among professionals and communities, established school-based services, a register of cases to make sure secondary cases are prevented, and a core of dedicated staff and community leaders. Television advertising has for the first time alerted the public right across the country to the issue. Efforts to address the underlying determinants of this illness, in particular poor housing conditions, are now benefiting from a clear health service focus, and cross agency approach.
Despite best endeavours, cases of acute rheumatic fever have continued to occur locally and nationally, and rates have remained stubbornly high. There are, however, some encouraging signs of change. The early part of 2015 saw a fall in rates of hospital admissions, and preliminary evaluation of school based services at the national level, showed modest effectiveness in preventing cases. The detailed findings are awaited, as are the results of other research into rheumatic fever that have been commissioned as part of the national programme.
The structure of a comprehensive approach to preventing rheumatic fever has at last been put in place across NZ, and there are now belated, but welcome signs that a difference may be emerging.
Continuing to accept a small but steady number of ill children every year is, as I said in the foreword to the first version of this plan, not an option.
Now is not the time to lose our nerve. Rheumatic fever doesn’t happen in modern, developed countries. It shouldn’t be happening here.
Dr Jim Miller
Medical Officer of Health
Chairperson
Lakes/BOP Rheumatic Fever Steering Group
3
Bay of Plenty DHB Rheumatic Fever Prevention Plan (refreshed version) sign-off
This document has been reviewed and accepted as the refreshed Bay of Plenty DHB Rheumatic
Fever Prevention Plan from 1 January 2016 and beyond 30 June 2017.
Name: Phil Cammish
Chief Executive
Bay of Plenty DHB
___________________ 20/10/2015
Signature
Name: Punohu McCausland
Chairperson, Maori Health Runanga
Bay of Plenty DHB
____________________ 20/10/2015
Signature
4
List of Abbreviations ARF Acute Rheumatic Fever
BAU Business as Usual
BOP Bay of Plenty
BOPDHB Bay of Plenty District Health Board
BPS Better Public Services
CHW Community Health Worker
CME/CNE Continuing Medical Education/Continuing Nursing Education
CoBoP Collaboration Bay of Plenty
DNS District Nursing Service
EECA Energy Efficiency and Conservation Authority
EBOP Eastern Bay of Plenty
EBPHA Eastern Bay Primary Health Alliance
GAS Group A Streptococcus
GP General Practice / Practitioner
HNZ Housing New Zealand
ICD codes International Classification of Disease codes
INR International Normalisation Ratio (for use of warfarin anticoagulant)
MoH Ministry of Health
MOH Medical Officer of Health
NHF National Heart Foundation
NMO Ltd Nga Mataapuna Oranga Primary Health Organisation
PHN Public Health Nurse
PHO Primary Health Organisation
PoPAG Population Health Professional Advisory Group
RAPHS Rotorua Area Primary Health Services
RHD Rheumatic Heart Disease
Toi Te Ora Toi Te Ora – Public Health Service
WBOP Western Bay of Plenty
WBOPPHO Western Bay of Plenty Primary Health Organisation
WISH Whakatohea Iwi Social and Health Services
5
Section 1: Overview of rheumatic fever in Bay Of Plenty and Lakes District Health Boards (DHBs)
1.0 Background Acute rheumatic fever (ARF) has been clearly recognised as a significant problem in New
Zealand which needs to be addressed. Bay of Plenty DHB (BOPDHB) and Lakes DHB
recognised ARF as a priority issue in 2008. In 2009 a joint steering group was established to
lead a range of DHB-funded initiatives to address rheumatic fever which are now operating
largely as business as usual. Ministry of Health (MoH) funded projects were introduced in
2012, with further MoH-funded programmes introduced in 2015.
The approach taken so far has been based firmly on the Heart Foundation rheumatic fever
guidelines, taking into account the local epidemiology and community wishes.
Programmes are now in place in the following areas:
1. raising public awareness that ‘sore throats matter’
2. continuing professional development for health professionals and Community Health
Workers (CHWs)
3. school-based throat swabbing campaigns, with linked activity in reducing skin
diseases
4. improved notification of new cases to the Medical Officer of Health (MOH)
5. implementation of rapid-response clinics in medium-risk areas not covered by school-
based programmes
6. housing improvement and assistance to “live well together” to reduce structural and
functional crowding
7. improving case management, including development of a rheumatic fever register
across Lakes and BOP DHBs
8. enhanced surveillance and root-cause analysis of cases
A range of positive results have been demonstrated to date. These include raised
awareness of rheumatic fever in higher risk communities and the general public; increased
awareness of the sore throat guidelines among GPs; the establishment of a register in
BOPDHB district; school-based throat swabbing programmes in 30 decile 1-3 schools that
are operating to agreed protocols, having gained the support of local communities. To date
though, there is no clear evidence of a sustained trend to reduced rates of ARF in the BOP.
6
1.1 Purpose of the plan The purpose of this refreshed plan is firstly to enable BOPDHB, Lakes DHB and their partner
organisations to co-ordinate services and prioritise initiatives to achieve the national Better
Public Services (BPS) target to reduce the incidence of rheumatic fever by two thirds to 1.3
cases per 100,000 people by June 2017. The plan also signals the level of continuing
preventive services to be provided from 1 July 2017 until June 2022. The BOPDHB
refreshed plan goes beyond the reduction of ARF, by also focusing on minimizing the impact
of rheumatic heart disease (RHD) in the population served by BOP and Lakes DHBs through
coordinated secondary service provision. About 80% of children and young people develop
Rheumatic Heart Disease (RHD) following Acute Rheumatic Fever. A Maori man with RHD
lives 12 years and a Maori woman lives 17 years less than Maori without RHD. Acute
Rheumatic Fever’s long shadow is RHD.
While some limited evidence is emerging nationally and locally on which services are most
likely to achieve the BPS target, it is likely that more evidence will be produced from
evaluations undertaken in the future. This refreshed plan therefore will need to be reviewed
regularly to ensure that practice is aligned to the most recent at hand.
1.2 BOP and Lakes DHBs – a shared approach In order to achieve the Better Public Services target to reduce rheumatic fever, a shared
approach has been taken by BOP and Lakes DHBs, as there is significant regional work that
is common to both. This includes the development of a single rheumatic fever register,
awareness raising, clinical and peer support for the school-based programmes and
continuing professional development for health professionals. There is a shared
commitment to continue to work together to meet this challenging target.
However, it is also recognised that in some areas, different approaches are warranted. This
is reflected in the development of two separate plans, one for Lakes DHB and one for
BOPDHB, which share a common overview but provide DHB-specific interventions.
1.3 Commitment to reducing rheumatic fever in the BOP and Lakes DHBs
1.3.1. Target data Lakes and BOP DHBs are committed to reducing the incidence of rheumatic fever to levels
set by the Better Public Services targets. The specific targets for each DHB are summarised
in Tables 1 and 2 along with the National targets.
7
Table 1: Acute rheumatic fever initial hospitalisation target rates per year for Lakes and BOPDHBs (per 100,000
total population), 2012/13 to 2016/17
District Health Board 2009/10–2011/12 Baseline
rate
(3-year
average
rate)
2012/13 Target: Remain at
baseline level
2013/14 Target: 10%
reduction
from
baseline
level
2014/15 Target: 40%
reduction
from
baseline
level
2015 /16 Target: 55%
reduction
from
baseline
level
2016/17 Target: 2/3
reduction
from
baseline
level
Lakes 7.8 7.8 7.0 4.7 3.5 2.6
Bay of Plenty 3.8 3.8 3.4 2.3 1.7 1.3
New Zealand 4.0 4.0 3.6 2.4 1.8 1.3
Table 2: Acute rheumatic fever initial hospitalisation target numbers per year for Lakes and BOP DHBs (total
population), 2012/13 to 2016/17
District Health Board 2009/10–2011/12
Baseline numbers
(3-year average rate)
2012/13 Target:
Remain at baseline level
2013/14 Target:
10% reduction from baseline level
2014/15 Target:
40% reduction from baseline level
2015 /16 Target:
55% reduction from baseline level
2016/17 Target:
2/3 reduction from baseline level
Lakes 8 8 7 5 4 3
Bay of Plenty 8 8 7 5 4 3
New Zealand 177 177 162 109 83 62
1.3.2 Performance data The actual performance against these targets for the years 2012/13, 2013/14 and 2014/15 is
shown in Table 3: Table 3: Actual acute rheumatic fever hospitalisation rates and numbers per year for Lakes and BOP DHBs (total
population), 2012/13 to 2014/15 (data provided by Ministry of Health)
District Health Board 2012/13 actual 2013/14 actual 2014/15 actual Rates Numbers Rates Numbers Rates Numbers
Lakes 6.8 7 3.9 4 5.8 6
Bay of Plenty 3.3 7 4.6 10 3.2 7
New Zealand Total 4.0 179 3.9 175 3.0 135 New Zealand Maori 12.7 10.6 8.8 New Zealand Pacific 25.9 31.6 22.5
8
A brief summary of the demographics of the 44 cases of first episode AFRF notifications to
the Medical Officer of Health from 1 January 2010 to 30 September 2015 shows that:
• A total of 31 cases were in the eastern BOP and 13 in the western BOP
• A total of 21 cases came from geographical areas where full school-based throat
swabbing programmes are currently in place, 18 resided in areas where there is
reasonable access to current rapid response clinics, and 3 were in areas that are
outside of sore throat management programmes other than routine general practice.
• Of the 44 cases, 39 were Maori, 3 Pacific, one NZE and one Unknown using the
prioritised ethnicity classification system
• A total of 36 cases were aged 5-14, 4 were aged 15-19 and 4 were <5 or >20 years
of age.
1.4 Rheumatic fever champions The BOP and Lakes rheumatic fever champions have been nominated by their respective
DHBs and all are members of the BOP and Lakes rheumatic fever steering group. One of
the key tasks of the champions is to act as the main point of contact for rheumatic fever
issues in each DHB. The Lakes and BOP DHBs Rheumatic Fever Champions will work
within the two DHBs and with equivalent champions across other DHBs, to drive and co-
ordinate actions in each DHB plan to achieve DHB targets.
1.4.1 Lakes DHB Dr Johan Morreau (Community Paediatrician) and Dr Neil Poskitt (General Practitioner and
Clinical Leader of Child Health for RAPHS) are the rheumatic fever champions for Lakes
DHB. One of the key tasks of the champions is to act as the main point of contact for
rheumatic fever issues in Lakes. Dr Poskitt, in conjunction with RAPHS, has been key to the
development of the Rheumatic Fever Register. This provides the capability to audit current
rates, trends, adherence rates and review of patient care.
Elise Pope (rheumatic fever co-ordinator) is the champion for continuous monitoring and
performance of prophylaxis care, interlinking primary and secondary health care services
and assisting in the transition from child to adult care for rheumatic fever patients throughout
Lakes DHB.
1.4.2 BOPDHB Dr John Malcolm (Paediatrician, Whakatane Hospital) and Pamela Barke (Nurse Leader
Regional Community Services) are the rheumatic fever champions for the BOPDHB. John’s
appointment provides paediatric medical oversight for programmes, and draws on his
considerable expertise and interest in rheumatic fever issues over many years.
9
Pamela Barke is the champion for monitoring performance of the delivery of Benzathine
Penicillin prophylaxis. This work is also linked to the steering group priority goals to develop
a regional rheumatic fever register and audit Bi-cillin delivery. The district nurses also
provide education and facilitate follow up care for patients with a diagnosis of acute
rheumatic fever and/or rheumatic heart disease (RHD).
1.4.3 Future Governance provisions To date, the governance of the BOP Rheumatic Fever Prevention Plan has been through the
BOP and Lakes DHBs Rheumatic Fever Steering Group. This Group has included all the key
stakeholders, but at a senior clinical and portfolio manager, Planning and Funding level. This
group will continue to provide immediate oversight for the refreshed BOP Rheumatic Fever
Prevention Plan.
The BOPDHB is currently entering into early discussions on possible new governance
arrangements across the wider central government sector as part of strategic thinking to
better integrate the health and social sectors. This new governance body will include the
Ministries of Education and Social Development, and Te Puni Kokiri as a minimum. The role
of this new Governance Group is to provide strategic oversight of a range of intersectoral
activities, including most likely:
• Social Sector Trial sites in Whakatane and Kawerau;
• Community Response Forum;
• Better Public Service targets, including rheumatic fever prevention;
• BOPDHB’s Child and Youth Strategy, which is jointly signed off by MSD, MoE and
BOPDHB;
• MBIE contract streamlining and accountability/audit processes.
Membership of the Governance Group will be at senior Executive levels in each
organisation.
10
Section 2: Overarching actions to reduce the incidence of rheumatic fever in the BOP and Lakes districts
2.0 Overview of the prevention of ARF and RHD The overarching goal for BOP and Lakes DHBs is to reduce the incidence of rheumatic fever
amongst the total population (but primarily Māori and Pacific peoples) by two thirds by June
2017. In order to achieve this, there are a number of critical prevention stages:
Primordial prevention: Broad social, economic and environmental initiatives undertaken to
prevent or limit the impact of GAS infection in a population. BOP and Lakes DHBs will
undertake interventions aimed at preventing the transmission of Group A streptococcal
throat infections in crowded housing situations through the continuation of the Healthy
Homes Initiative funded by the Ministry until 31 December 2016. DHBs have less direct
influence on child poverty and other social issues, but will work with local government and
other central governments agencies where possible, including through cross sector
programmes such as Children’s Action Team, Social Sector Trials and Whanau Ora, to
improve living standards for vulnerable children and young people.
Primary prevention: Reducing GAS transmission, acquisition, colonisation and carriage or
treating GAS infection effectively to prevent the development of ARF in individuals. BOP and
Lakes interventions will be aimed at school, community and primary health care level
through appropriate detection and management of GAS pharyngitis. Primary prevention also
includes community awareness raising initiatives and continuing professional development
for health professionals.
Secondary prevention: Administering regular prophylactic antibiotics to individuals who
have had an episode of ARF to prevent the development of RHD or to individuals who have
established RHD to prevent the progression of the disease. In the BOP and Lakes,
secondary prevention is closely linked to the implementation of a regional register, with
monitoring and auditing capabilities. Care pathways and Bi-cillin prophylaxis protocols are
also aimed at preventing further recurrence of ARF and RHD.
Tertiary prevention: Intervention in individuals with RHD to reduce symptoms and disability
and prevent premature death. BOP and Lakes DHBs acknowledge the need to ensure
excellent clinical follow up of patients with an existing diagnosis of ARF and RHD. The BOP
and Lakes rheumatic fever register operated by RAPHS will support this work.
11
2.1 BOP and Lakes shared priorities 2013-2017 There is significant regional work that is common to both DHBs to achieve the goal of
reducing rheumatic fever. Since 2009, efforts to address rheumatic fever have been led by
the Lakes/BOP Rheumatic Fever Steering Group. A multifaceted approach was adopted
including the revision of priorities from year to year, with a focus on primary, secondary and
to a lesser extent tertiary prevention. With the adoption of a challenging national target for
the reduction of rheumatic fever rates and confirmation that health is to take the lead across
sectors, primordial prevention will be a new and significant area of work. The steering group
agreed broad priorities for action across both DHBs from 2013 to 2017, these being:
• addressing the determinants of health, in particular poor housing conditions and
crowding;
• establishment of a rheumatic fever register across BOP and Lakes districts;
• community awareness raising;
• continuing professional development for health professionals;
• easier access to primary care;
• ensuring the delivery of high quality school-based programmes in high risk areas to
ensure that children have access to prompt treatment, to ensure that services are
operating safely, and to contribute to national evaluations of effectiveness;
• meaningful monitoring – process and outcome evaluation.
12
2.2 What does this mean for BOPDHB and the BOP school based sore throat swabbing programme? The national interim evaluation has provided some useful insights. While unfortunately not
achieving statistical significance, there is encouragement that the programmes have been
partially successful in reducing the incidence of RF, and may be an important component of
a DHB's programme to achieve the RF target. In regards to BOPDHB, our population, and
our school based programme, there are some aspects which limit direct comparison
between the national evaluation and the potential effectiveness or cost effectiveness of the
service in our region.
The cost of delivering the school based programmes in BOPDHB is considered to be lower
than figures used in the interim evaluation:
• The total school rolls of the 29 schools in the programme is 4,551 as at July 2014.
Based on an approximate 98% consent rate to throat swabbing, then there are 4,460
children able to access the programme.
• The total cost of the school-based throat swabbing programme is $721,667 per
annum, including the agreement prices for all providers, laboratory testing costs, and
the costs of the nursing clinical assurance oversight.
• Therefore the costs per child per annum are $161.81 c.f. Counties-Manukau DHB
costs used in the economic analysis of $200 per child per annum.
Further to the national evaluation, a local audit and evaluation on preliminary data reported a
non-statistically significant decrease in RF rates for Māori children (aged 5-14) in eastern
BOP intervention schools – Opotiki, Kawerau and Tuhoe programmes. In the pre-
intervention period from 2000 to 2010, Maori children aged 5-14 had a ARF rate of
128.7/100,000 (95%CI 60.6-177.4), and in the intervention period from 2011 to 2014, the
rate was 50.7/100,000 (95%CI 16.3-118.3). This data is to be updated for the 2014/15 year
and the inclusion of the Murupara programme. This unpublished audit and evaluation may
provide some broad indication that RF rates may be reducing in the Eastern BOP. However,
because of small numbers, we are unsure how robust this observation is and to what we
should attribute any changes.
The reduced costs of the BOPDHB school-based throat swabbing programme would have
an effect on the cost per QALY gained for the programme. The BOPDHB programme is also
13
not limited to solely the prevention of RF, with linked activities to reduce skin diseases and
highlight the importance of good hygiene practices.
It is appreciated that school based sore throat swabbing programmes are not likely to allow
DHBs to reach RF targets on their own, rather they are seen as a interim approach while
other initiatives increase primary care access. In BOPDHB school based programmes are
one component of the RFPP, with further initiatives detailed elswhere in this Plan.
When school based sore throat swabbing commenced in BOPDHB (in 2009), it was
acknowledged the programme would continue beyond the period funded by MOH.
Stakeholder and community engagement has shown us that the school based programmes
are valued and well received in communities, and act to increase awareness of RF and the
importance of sore throat management in whanau. The interim national evaluation of school
based sore throat programmes does not have a sufficient number of cases to demonstrate a
statistically significant effectiveness in reducing ARF, however it does suggest that the
programme is likely to reduce the number of cases, and act as a useful adjunct to the other
initiatives BOPDHB is employing in order to reach the BPS target of rheumatic fever
incidence reduction. It is interesting to note that an evaluation undertaken by Dr Janine
Stevens of Hawke’s Bay DHBs Say Ahh programme in Flaxmere, also recommended that
the programme should continue. While recognising the challenges in continuing the
programme, such as increasing costs due to increased service utilisation, concens about
over-use of antibiotics, and opportunity costs for other health service priorities, the
recommendation supported continuation of the programme unless conclusive evidence
showed that the programme’s benefits were less than these costs.
2.3 Laboratory data Data supplied by Path Lab for Group A streptococcus swab tests from January 2010 to
September 2015 shows a steady increase in the number of swabs taken in:
• the school-based throat swabbing programme, as additional schools have been
included;
• in general practice, as community awareness increases and health practitioners are
more familiar with accepted best pactice;
• in hospital emergencency departments, as community awareness increases.
Positivity rates have trended downwards in general practice, with positivity rates being lower
in the 2013 to 2015 to date period in comparison with the 2010 to 2011 period. Overall the
percentage of swabs which tested positive taken in A&E was significantly higher than those
14
taken in general practice, which in turn was higher than swabs from the school programme.
That is likely to reflect the severity of symptoms in the people presenting to the different
services.
Table 4 shows the data from the school-based throat swabbing programme, general
practice, and hospital emergency departments.
Table 4: Path Lab data for GAS swab testing – BOPDHB district
Year School-based General practice Hospital Emergency Department
No of swabs
No of +ve swabs
Positivity rate
No of swabs
No of +ve swabs
Positivity rate
No of swabs
No of +ve swabs
Positivity rate
2010 2,040 206 10.1% 7,095 1,336 18.8% 619 116 18.7%
2011 5,954 600 10.1% 9,301 1,800 19.4% 664 138 20.8%
2012 9,659 988 10.2% 6,017 1,732 28.8% 943 193 20.5%
2013 13,734 1,300 9.5% 13,104 1,888 14.4% 1,123 211 18.8%
2014 15,579 1,276 8.2% 16,422 2,031 12.4% 1,285 192 14.9%
2015 to Sept 10,224 987 9.7% 14,283 1,487 15.1% 1,093 169 15.5%
2010 to date 57,190 5,357 9.4% 66,222 10,274 15.5% 5,727 1,019 17.8%
The following graphs present the same data for the general practice swab testing results.
15
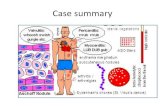
2.4 Root cause analysis data The following flow diagrams showing the outcomes of the national and local system failure
analysis reports disclose that not much more than half of diagnosed cases of rheumatic
fever had any memory of a sore throat throat. Dr S Schulman noted this also as the ARF
programme in Baltimore, USA took effect. Of those that did note a sore throat, about a third
saw a health professional and were prescribed the right antibiotics, although strict adherence
to taking the antibiotics is not known. This supports that:
• reliance cannot be placed on sore throat management as a means to achieve a
target of two-thirds reduction.
• Improvements can be made in the sore throat management pathway, which if
achieved would potentiallly reduce the risk of acute rheumatic fever in children
identified with sore throats.
• echocardiographic screening needs further consideration and the outcome of 2013
Heart Foundation, MOH, Te Puni Kokiri and HRC funded evaluation research may
have a bearing.
16
Analysis of national system failure analysis reports 2014/15
± ⅔ completed course ± ⅓ did not complete course (intervention: improved adherence education)
25 got right antibiotic
31 got antibiotics 6 did not get right antibiotic (Intervention: more health professional education) 42 saw a health professional 11 did not get antibiotics (Intervention: more health professional education) 69 remembered having a sore throat 27 did not see a health professional (Interventions: individual, whanau and community awareness raising/ improved access to primary care including rapid response clinics) 127 systems failure analysis reports completed 58 did not remember having a sore throat (Intervention: improving housing programme, echocardiographic screening?)
17
Analysis of BOP case review forms 2014/15
Unknown if completed course? did not complete course (intervention: improved adherence education)
1 got right antibiotic
1 got antibiotics 0 did not get right antibiotic (Intervention: more health professional education) 1 saw a health professional
(recurrent case) 0 did not get antibiotics (Intervention: more health professional education) 3 remembered having a sore throat (includes recurrent case) 2 did not see a health professional (Interventions: individual, whanau and community awareness raising/ improved access to primary care including rapid response clinics) 7 (6 initial ARF and 1 recurrent) Case review reports completed 4 did not remember having a sore throat (Intervention: improving housing programme, echocardiographic screening?)
18
Section 3: Investment to reduce ARF incidence and RHD
Section 3.0 Introduction N.B. In this publicly available version of the BOP Rheumatic Fever Prevention Plan, funding is shown by general class of activity but not shown at an individual provider contractual level. If more detail is sought, contact the Planning and Funding team at BOPDHB.
This section outlines the service and funding decisions over the next few years. The overall
strategy is to make every effort to achieve the target by 30 June 2017, while keeping DHB
funding levels constant as the Ministry contribution decreases. From 2017/18 onwards, the
DHB funding levels may be able to be reduced, depending on outcomes against the national
and DHB target, and evidence of the most effective and cost-efficient services. The following
summary in Table 5 outlines budgets for the next three years and beyond.
Table 5: Summary of Budgets 2015/16 to 2017/18 and beyond
2015/16 2016/17 2017/18 + out years
DHB funding (contracted) 851,551 825,423 836,520
MoH funding (contracted) 430,375 98,875 0
Additional MoH funding (not contracted) 100,000 331,250 183,743
Total expenditure 1,381,926 1,255,548 1,020,263
3.1 BOPDHB resources committed to reducing rheumatic fever 2015/16 The BOPDHB has planned for the following investment to be made in reducing rheumatic
fever in 2015/16 (GST exclusive). Most of this resource is already committed in provider
agreements – Table 6 refers.
19
Table 6: BOPDHB resources committed to reducing rheumatic fever 2015/16
Initiatives Cost $
School-based throat swabbing programmes
495,731 75,75,71
Community awareness raising
50,475
Rapid response clinics
245,000
Housing improvement initiatives
205,375
Laboratory testing
185,000
Coordination and governance
85,000
Clinical quality assurance of swabbing programmes Funded by DHB through EBPHA to provide quality assurance across all throat swabbing.50
40,936
Register ongoing costs
14,000
District nursing support
60,409
Total 1,381,926 Footnote: The table does not include investment where services are provided in kind. These include: Planning and Funding portfolio manager, contracts management, finance and overhead costs; PHO data analysis and evaluation costs; Paediatrics and Nursing contributions within Rh Fever Steering group. Also Toi Te Ora - Public Health Services Medical Officer of Health time and Communicable Diseases Nurse time in actual case management; costs within general practice, or routine District Nursing Services Bi-cillin management programme. This footnote applies also to Tables 7 and 8.
3.2 BOPDHB investment for 2016/17, including new initiatives The BOPDHB’s strategy for the 2016/17 year is to make every reasonable endeavour to
achieve the target, maintaining services at current levels as much as possible within funding
constraints. The Ministry has reduced its funding from 2015/16 levels by $100,250. The DHB
will also reduce its investment into programmes by $26,128 while maintaining core services.
The intention is to continue funding the following programmes during the 2016/17 year at the
same level as in 2015/16.
20
Opotiki, Kawerau, Murupara, Tuhoe and Tauranga South school-based throat swabbing
programmes, considering any cost efficiencies that are practicable.
The community awareness raising programme delivered by NASH in eastern BOP.
Clinical quality assurance agreement with EBPHA.
Coordination and governance through Toi Te Ora - Public Health Service
Laboratory costs (ensuring that the block amount being paid currently aligns with the
volume of swabs being sent to PathLab, so that the price per swab remains competitive)
Register ongoing costs
District nursing support for a Rheumatic Fever Coordinator
BOPDHB third party funding for all housing projects across the BOP, including those
specifically for rheumatic fever prevention whanau.
The DHB will continue to fund Ministry-initiated projects but with reduced funding and
changes to the service delivery model.
Housing Insulation Initiative scheme, with the pathway, referral criteria and processes be
streamlined from 1 January 2017, and be dependent on subsidy levels and criteria set by
EECA and other third party funding contributions.
A revamped Business as Usual primary and community-based service for rapid
response assessment and treatment of sore throats.
21
Table 7: BOPDHB resources committed to reducing rheumatic fever 2016/17
Initiatives Cost $ Comment School-based throat swabbing programmes
495,731
495,731
No change from 2015/16 other than any cost efficiencies /12/15
Community awareness raising
50,475
No change from 2015/16
Rapid response clinics Revamp of services towards Business as Usual within primary and community care
135,123 Costs reduced from $245,000 in 2015/16
Housing improvement initiatives
188,874 ,6871
Development of new service from 1/01/17 ment of new service from 1/01/1evelopm service from 1/01/17$98,875at $MoH 31 /12/1
Laboratory testing
185,000
No change from 2015/16, although savings will be
sought if swabbing numbers reduce.
Coordination and governance
85,000
No change from 2015/16
Clinical quality assurance of swabbing programmes
.50
40,936 404 No change from 2015/16
Register ongoing costs
14,000
No change from 2015/16
District nursing support
60,409
No change from 2015/16
Total 1,255,548 .175 Footnote: The BOPDHB will consider each funding line separately in this plan when agreements expire, as part of its annual budget planning process from 2016/17 onwards, in light of wider budget drivers and national and local priorities. It will also actively seek additional revenue streams from Ministry of Health and philanthropic trusts which align with this overall plan.
22
3.3 BOPDHB investment for 2017/18 and later out years to 2021/22 The question of when school-based throat swabbing programmes should cease has not yet
been satisfactorily resolved nationally. Continuation of school-based throat swabbing in high
risk communities will largely be determined by their local success and all contributions to the
success in achieving the BPS target, and national evaluations and cost-efficiency analyses.
The BOPDHB’s strategy for the 2017/18 year and later out years to 2021/22 is to shift into a
maintenance mode, retaining a core of specific rheumatic fever prevention services as much
as possible within funding constraints, and building up Business as Usual primary and
community-based services. The shortfall in funding between 2015/16 programme costs, and
funding available from the DHB and MoH is $232,889 in 2017/18 and beyond if all services
delivered in 2016/17 were to continue, and the BOPDHB were to maintain existing
investment levels. Neither proviso is likely, although this will be dependent on whether the
DHB achieves the target by 2016/17. The DHB will therefore reduce the total costs of all
programmes from the 2016/17 figure of $1,255,548 to a maximum of $1,020,263. Of this
$1,020,263, $183,743 will be met by the Ministry of Health, with the balance met by the
BOPDHB. Further savings may occur once national evaluations provide clearer indications
of the effectiveness of different services.
The DHB intends to continue funding the following programmes during the 2017/18 year and
beyond at the same level as in 2015/16.
Opotiki, Kawerau, Murupara, Tuhoe and Tauranga South school-based throat swabbing
programmes, considering national evaluative evidence of effectiveness and cost -
efficiency.
Laboratory costs (ensuring that the block amount being paid currently aligns with the
volume of swabs being sent to PathLab, so that the price per swab remains competitive)
Register ongoing costs
District nursing support for a Rheumatic Fever Coordinator
BOPDHB third party funding for all housing projects across the BOP, including those
specifically for rheumatic fever prevention whanau.
Housing Insulation Initiative scheme, although the pathway, referral criteria and
processes will be streamlined from 1 January 2017, and be dependent on subsidy levels
and criteria set by EECA and other third party funding contributions.
Revamped Business as Usual sore throat management services within primary and
community care.
In 2017/18 and out years, it is intended that the BOPDHB will cease contracting specifically
for the clinical quality assurance agreement with EBPHA, and the coordination and
23
governance through Toi Te Ora - Public Health Service. These activities will be embedded
as Business as Usual into the continuing school-based swabbing programme agreements,
and Toi Te Ora’s core Public Health Services agreement with the Ministry of Health
respectively. This will allow these services two years to plan for this change.
Table 8: BOPDHB resources committed to reducing rheumatic fever 2017/18 and out years
Initiatives Cost $ Comment School-based throat swabbing programmes
495,73175,75,71
No change from 2016/17 other than any cost efficiencies /12/15
Revamped Business as Usual sore throat management services within primary and community care
135,123 No change from 2016/17
Housing improvement initiatives
130,000 501177,6871
No change from 2016/17 Development of new service from 1/01/17 Development of new98,875at $MoH 31 /12/1
Laboratory testing
185,000
No change from 2016/17, although savings will be
sought if swabbing numbers reduce.
Register ongoing costs
14,000
No change from 2015/16
District nursing support
60,409
No change from 2015/16
Total 1,020,263 .175 Footnote: The BOPDHB will consider each funding line separately in this plan when agreements expire, as part of its annual budget planning process from 2017/18 onwards, in light of wider budget drivers and national and local priorities. It will also actively seek additional revenue streams from Ministry of Health and philanthropic trusts which align with this overall plan.
24
3.4 Co-benefits While the focus of this plan remains the prevention of Acute Rheumatic fever and Rheumatic
Heart Disease, there are a number of co-benefits associated with the work undertaken.
These include:
3.4.1 Prevention, early assessment and treatment of skin infections Up until recently, in New Zealand there has not been a demonstrated causal association
between streptococcal skin infections and rheumatic fever. However the same socio-
economic factors that result in skin infections are linked to rheumatic fever e.g. crowded
housing conditions, poverty and barriers to effective early primary health care. Therefore the
preventive actions taken for acute rheumatic fever would be expected to impact on the
incidence of skin infections and vice versa. Indeed, skin infections and cellulitis prevention
are delivered under the same agreement and by the same staff in the Kawerau programme,
with declining throat GAS, ARF and skin infections, and resources have been shared with all
other school-based throat swabbing and community awareness programmes in the BOP.
3.4.2 Respiratory infections in children Similarly to skin infections, the underlying factors causing respiratory infections in young
children are the same as for rheumatic fever i.e. crowded housing conditions, poverty and
barriers to effective early primary health care. Respiratory disease make up three of the top
six ASH conditions for 0-4 year olds (with skin infections a fourth condition). There are on
average 1,100 admissions of BOPDHB children aged 0-14 every year from respiratory
infections, with 89% being bronchiolitis, upper respiratory infections, pneumonia and lower
respiratory infections. In Whakatane 1 in 6 infants are admitted with bronchiolitis. A
childhood respiratory management pathway is being developed under Bay Navigator which
should include information around referral processes for home insulation and other
improvements.
3.4.3 Enrolment and ongoing engagement with primary health care With free primary care and access to prescriptions for all under 13 year olds in the BOP,
some (but not all) of the barriers to accessing primary health care have been removed.
There is still a need to increase engagement with primary health care for adolescents aged
13-19, who traditionally have low utilisation rates, particularly for conditions not associated
with injury or sexual and reproductive health. Needing to access primary care for sore throat
management, including pharmacy for antibiotics, will help to normalise routine primary care
consultations.
The enrolment rate for BOP residents in general practice and PHOs is generally high at
98+%, although those not enrolled will tend to be in those populations at risk of rheumatic
25
fever. Staff working in school-based and community rheumatic fever programmes check the
enrolment of all families they engage with.
These co-benefits illustrate there would be value in taking a more comprehensive approach
to well child health care to encompass a number of common issues as part of an integrated
service within communities. Community Health Workers can contribute local knowledge and
credibility. This wider approach within families could include as appropriate to the age of the
child:
• Housing improvements;
• Immunisation outreach;
• Skin infections and cellulitis;
• Sore throat management;
• Oral health;
• SUDI prevention;
• Breastfeeding promotion;
• Smoking cessation.
3.5 Re-designed Healthy Homes Initiative from January 2017 The BOPDHB has been involved in home insulation and broader home improvement
projects for many years. In conjunction with philanthropic trusts, private home insulation
providers, NGOs and Hauora services, it has developed expertise and experience in this
field, which has been strengthened with the Ministry of Health funded Healthy Homes
Initiative. The current situation in the BOP is as follows:
• There are existing community-based projects in Maketu and surrounding areas, and
Kawerau, with the potential for a new project in Murupara township in 2016.
• Philanthropic trusts e.g. BayTrust are funding home assessments, project
management, DIY workshops and community development as part of a long term
strategic direction.
• The two energy trusts, Tauranga Electricity Community Trust and Eastern Bay
Energy Trust, are acting as third party funders to support government funding
available through EECA. The DHB is contributing an additional $50,000 per annum
for home insulation funding.
• A comprehensive set of interventions alongside home insulation are now available
across most of the BOPDHB district. These include curtains, heaters, firewood,
clothing, bedding and blankets, budget advice, and Work and Income benefit
reviews, and are currently exploring ways to deliver free or low cost home
maintenance services.
26
• The Ministry of Health Healthy Homes Initiative programme ceases at 31 December
2016. Through this programme, effective relationships have been developed with
MSD and HNZ.
The DHB is looking to establish a sustainable service across its district from 1 January 2017.
One of the problems at the moment is that there are a number of eligibility criteria for funding
of home insulations, set by EECA, the Ministry of Health, and third party funders. This has
resulted in a number of referral processes being in place, which leads to confusion amongst
health practitioners who are engaged with families who would benefit from home
improvements.
The intention is to simplify referral processes for all health practitioners by having a common
referral form that would be sent to a single clearing house. Having only one initial referral
form will allow the DHB to widen the sources of referrals to include general practice, public
health nurses and other health professional not currently involved in making referrals. This
organisation would be funded by the DHB to undertake healthy homes assessments; refer
for interventions to reduce crowding and make home improvements; provide home energy
awareness and healthy living together education; and report back to the DHB on
assessment and intervention outcomes. The assessments would be funded by the
philanthropic sector and home insulations would be funded by EECA and local funders
according to their criteria. It is likely that in future the government’s funding will be limited to
rental property, but that is the sector where the most uninsulated homes are.
The BOPDHB in conjunction with Lakes DHB and through Toi Te Ora-Public Health Service
will hold a workshop on healthy housing in about April 2016. This workshop will provide an
opportunity for existing projects to showcase their work, for key stakeholders to outline their
roles, and for discussion on future pathways for home insulation and other home
improvements. There may be opportunities to involve landlord and rental management
groups. The workshop may lead to the development of a permanent cross-agency forum for
health and housing issues, if that is the collective wish of the key stakeholders.
3.6 Revamped Business as Usual sore throat management services in primary and community care Although it is early days yet, the current rapid response clinic service may prove to be cost
ineffective in its current form. The service is more effective in the eastern BOP where it is
reaching into smaller communities that are medium to high risk through schools and general
27
practice. The western BOP service is for a large population and geographical area, and is
still relying on families to access a centralised service in Tauranga city, even if free and out
of normal hours, which is unlikely to overcome the usual barriers to accessing primary health
care. A revamp of the rapid response clinic service is likely to be required, particularly in the
western BOP, based on services that are more accessible to at-risk populations. This could
include greater use of school nurses in primary, intermediate and secondary schools, and
pharmacies. Further work is required with PHOs and others to refine this service. The
intention is to establish this new service no later than 1 July 2016, and earlier if necessary.
28
Section 4: Action plan for 2015/16 and subsequent years
4.0 Introduction This section identifies detailed actions that BOPDHB will undertake to prevent the transmission of Group A streptococcal throat infections in
children and young people. Primordial prevention interventions will address housing conditions, general hygiene and skin infections. These
actions also fit with Toi Te Ora’s Goal 1: To reduce childhood admissions from ARF, respiratory and skin infections, each by 2/3rds in 5 years.
Please refer to the logic model diagram in Appendix 2.
N.B. This section is based on the content that was included in the original RFPP. Through the refresh progress, new or expanded actions
have then been developed for the 2015/16 and 2016/17 years leading up to the target assessment at 30 June 2017, and to 2017/18 and
beyond following that date. A lead person, agency or agencies are identified for each action, and a timeframe set for completion of that action.
This section can then be the basis for action reporting to the Ministry of Health.
Section Action Lead agency Timeframe
4.1 Housing
Housing advocacy plan to be finalised and implemented.
Ongoing implementation of advocacy plan.
Toi Te Ora Public Health
Service
Q3-4 2015/16 and ongoing
Housing report to be published on Toi Te Ora website
Toi Te Ora Public Health
Service
Q3 2015/16
Qualitative housing research report completed. Information
used for advocacy.
Toi Te Ora Public Health Q3 2015/16 and ongoing
29
Service
Housing workshop completed. Scope the potential to establish
a wider BOP housing forum
Toi Te Ora Public Health
Service
Planning and Funding, BOPDHB
Q4 2015/16
Ongoing review and monitoring of Healthy Homes Initiative Planning and Funding, BOPDHB
Sustainability Options Ltd
Tauranga Community Housing
Trust
Q1 2015/16 and ongoing
MoH-funded programme continues until 31 December 2016.
Programme to continue beyond 1 January 2017, but in
modified form.
Planning and Funding, BOPDHB
Q2 2016/17
MoH/HPA ‘Key tips for a warmer, drier home’ toolkit promoted
and distributed to RF sector team and RF housing teams.
Toolkit includes messages for crowded whanau.
Planning and Funding, BOPDHB
Sustainability Options Ltd
Tauranga Community Housing
Trust
Q1 2015/16 and ongoing
30
Toi Te Ora Public Health
Service
Toi Te Ora and Pacific Islands Community (Tauranga)
Trust/EBPHA to promote Pacific resources and information as
part of the wider RF awareness campaigns.
Toi Te Ora Public Health
Service
Q4 2015/16
Toi Te Ora undertaking a revision of the ‘Our Home Our
Responsibility’ calendar.
The MoH/HPA ‘Key tips for a warmer, drier home toolkit’
promoted and utilised.
Toi Te Ora Public Health
Service
Q4 2015/16
New housing referral and assessment system in place from 1
January 2017.
Planning and Funding BOPDHB Q2 2016/17
(Work with philanthropic sector, EECA, iwi Runanga, local
authorities and insulation companies to develop community
healthy housing projects.) Dependent on national government
decisions on continuation of EECA funding from 1 July 2016.
Likely to focus on private rental accommodation only.
Continue to explore opportunities for working with iwi.
Planning and Funding BOPDHB Q1 2015/16 and ongoing
31
4.2 Improving general hygiene in education settings
Hygiene messages promoted by CHWs in the throat swabbing
schools
Throat swabbing project
providers
Q1 2015/16 and ongoing
Hand and general hygiene awareness raising and education in
schools and ECEs.
Toi Te Ora Public Health
Service
Q1 2015/16 and ongoing
4.3 Reducing skin infections in schools, community and home settings
Healthy skin / skin infection information promoted via website,
CHWs, newsletters
Toi Te Ora Public Health
Service
Q1 2015/16 and ongoing
Ongoing awareness raising via the rheumatic fever
programme.
Toi Te Ora Public Health
Service
Throat swabbing project
providers
Q3 2015/16 and ongoing
Finalise and disseminate skin infection report and implement
the recommendations. Implement the recommendations of the
PoPAG and skin infection reports.
Planning and Funding BOPDHB
Toi Te Ora Public Health
Service
Q2 2015/16 and ongoing
Annual trend monitoring of skin infections Toi Te Ora Public Health
Service
Q3 2015/16 and annually in
2017 onwards
32
4.4 Throat swabbing programmes
Ongoing funding of BOPDHB programmes will continue in
(2015/16 and 2016/17.
BOPDHB to pick up funding for Tuhoe programme from 1
January 2016.
Planning and Funding BOPDHB
Planning and Funding BOPDHB
Q1 2015/16
Q1 2016/17
Q3 2015/16
Ongoing funding of all school-based programmes will continue
as long as evaluations and cost efficiency analysis
demonstrates benefit.
Ministry of Health
Planning and Funding BOPDHB
Q1 2017/18
Feed back findings of MoH evaluations and analysis to primary
and secondary care.
Planning and Funding BOPDHB Q2 2015/16 and ongoing
Promote and utilise MoH on-line tools and best practice
outlined in the New Zealand Primary Care Handbook.
Rheumatic fever e-learning course promoted. CHWs to
complete course as part of ongoing training.
Toi Te Ora Public Health
Service
EBPHA Rheumatic Fever Nurse
Coordinator
BOPDHB Rheumatic Fever
Clinical Champion
Q3 2015/16
Support school-based swabbing programmes.
EBPHA Rheumatic Fever Nurse
Coordinator
Q1 2015/16 and ongoing
33
Review of first rapid response clinic initiatives, and seek quality
improvements. Explore further options to make primary care
more accessible and affordable e.g. drop in clinics, primary
care clinics attached to EDs, extended and weekend hours.
Develop a new programme to optimise access to free primary
care for sore throat management.
Planning and Funding BOPDHB
PHOs
Q3 2015/16 and ongoing
4.5 Awareness raising of sore throats, Rheumatic Fever and its presentations, and Rheumatic Heart Disease
Yearly review and re-release (of a Rheumatic Fever
awareness raising communication plan).
The 2015/16 campaign to complement national awareness
campaigns, messages and resources. Campaign to include a
focus on local Pacific Island communities.
Toi Te Ora Public Health
Service
Q2 2015/16
Presentations and discussions with ED, Orthopaedics, adult
medicine, primary care re 2014 NHF Guidelines. BOPDHB Rheumatic Fever
Clinical Champion Q3 2015/16
Incorporate 2014 RHD benchmarks from NHF into Bay
Navigator. BOPDHB Rheumatic Fever
Clinical Champion Q2 2015/16
The 2016/17 campaign to complement national awareness
campaigns (if held), messages and resources. Campaign to
include a focus on local Pacific Island communities.
Dissemination across BOP disciplines.
Toi Te Ora Public Health
Service
Q4 2016/17
34
Development of early arthritis part of pathway to identify Septic
Arthritis Acute Rheumatic Fever.
Dissemination across BOP disciplines
BOPDHB Rheumatic Fever
Clinical Champion Q4 2015/16
4.6 Delivery and monitoring of
prophylactic antibiotics
Register will be utilised by BOP DNS, paediatricians,
cardiologists, physicians, Toi Te Ora.
Register implementation and utilisation for primary Bi-cillin
purposes; note facility supporting cardiac care INR for cardiac
and echo appointments.
Planning and Funding BOPDHB
Rotorua Area Primary Health
Services
BOPDHB Rheumatic Fever
Clinical Champion
Clinical Nurse Manager District
Nursing Services
Q2 2015/16
Handovers for Bi-cillin recipients of both Bi-cillin delivery and
cardiac care when moving between DHBs.
Clinical Nurse Manager District
Nursing Services
Q2 2015/16
More frequent auditing to be undertaken once register is fully
functional.
Clinical Nurse Manager District
Nursing Services
Planning and Funding BOPDHB
Q4 2015/16
35
Introduce analgesia utilisation to help comfort and adherence
in western BOP.
Clinical Nurse Manager District
Nursing Services
BOPDHB Rheumatic Fever
Clinical Champion
Q4 2015/16
Fully functioning RF clinical register across Lakes/ BOP.
Continued funding and use of same.
Register review to support cardiac care INR for cardiac and
echo appointments.
Planning and Funding BOPDHB
Rotorua Area Primary Health
Services
BOPDHB Rheumatic Fever
Clinical Champion
Q1 2015/16
Ongoing quality improvement in DNS services. Ongoing use of
register to improve timeliness of secondary prophylaxis.
Clinical Nurse Manager District
Nursing Services
Q3 2015/16 and ongoing
36
4.7 Notification of ARF cases to the Medical Officer of Health (MOH)
Any exceptions are followed up with notifying doctor
Toi Te Ora analyst to compare hospitalisation figures with
notifications.
Toi Te Ora Public Health
Service
Q1 2015/16 and ongoing
4.8. Review of cases to identify known risk factors and system failure points
Root cause analysis reports completed for all notified ARF
patients. Feedback provided if required.
Toi Te Ora Public Health
Service
Q1 2015/16 and ongoing
4.9 Other actions to facilitate the effective follow-up of identified
RF cases
Review and improvements to pathway.
BOPDHB Rheumatic Fever
Clinical Champion
Toi Te Ora Public Health
Service
Q4 2015/16 and ongoing
Distribution of dental pack to all Bicillin patients and selected
other priority risk groups through throat swabbing schools and
rapid response clinics to be undertaken as funding allows for
replacement packs and packs for new patients.
Toi Te Ora Public Health
Service
Q3 2015/16 and ongoing
37
4.10 Interventions for patients who do not have established RHD
Implementation and review of a treatment plan for patients who
do not have established (or documented) rheumatic heart
disease.
BOPDHB Rheumatic Fever
Clinical Champion
Q4 2015/16 and ongoing
4.11 Interventions for patients who do have established RHD
Incorporation of NHF guideline on follow up to Bay Navigator
pathway development. Register use of this. BOPDHB Rheumatic Fever
Clinical Champion
Q4 2015/16 and ongoing
38
Appendix 1 - Stakeholders
Stakeholders
BOP/ Lakes Rheumatic Fever Steering Group BOPDHB Planning and Funding and paediatrics teams Lakes DHB Planning and Funding and paediatrics teams BOPDHB Māori Health Planning and Funding team Lakes DHB Māori Health team Toi Te Ora - Public Health Service Eastern Bay Primary Health Alliance Korowai Aroha Rotorua Ngati Awa Social and Health Services Rotorua Area Primary Health Services (RAPHS), Te Ika Whenua Hauora Tuhoe Hauora Te Manu Toroa (Nga Mataapuna Oranga PHO) Whakatohea Iwi Social and Health Services BOP/ Lakes Rheumatic Fever Sector Group Eastern Bay PHA Toi Te Ora - Public Health Service Korowai Aroha Rotorua Ngati Awa Social and Health Services Te Ika Whenua Hauora Tuhoe Hauora Te Manu Toroa (Nga Mataapuna Oranga PHO) Whakatohea Iwi Social and Health Services Māori Health Services Lakes DHB Māori Health team BOPDHB Māori Health Planning and Funding team BOPDHB Regional Māori Health Services Te Puni Kokiri Housing Sector Smart Energy Solutions Ltd Sustainability Options Ltd Tauranga Community Housing Trust Eastern Bay Energy Trust Tauranga Electricity Community Trust BayTrust Ministry of Health Ministry of Social Development Housing New Zealand Population Health Professional Advisory Group (PoPAG) BOP Child and Youth Strategic Alliance BOPDHB and Lakes DHB cardiologists and echocardiography services
39
Appendix 2 – Logic model for Toi Te Ora Goal 1: Reduce childhood admissions from ARF, respiratory and skin infections, each by 2/3rds in 5 years
40
Appendix 3 - Schools on Rheumatic Fever Throat Swabbing programme
School Decile Roll Provider
Kawerau South School 1 313 Eastern Bay PHA
Putauaki Primary School 2 189 Eastern Bay PHA
Te Whata Tau o Putauaki 1 97 Eastern Bay PHA
Te Kura o Te Teko 1 156 Eastern Bay PHA
Te Mahoe School 1 39 Eastern Bay PHA
Tarawera High School, Kawerau 1 449 Eastern Bay PHA
Ashbrook School, Opotiki 1 143 Whakatohea iwi Social and Health Services
Kutarere School 1 35 Whakatohea iwi Social and Health Services
Omaramutu School 2 68 Whakatohea iwi Social and Health Services
St Joseph’s Catholic School, Opotiki 3 204 Whakatohea iwi Social and Health Services
Woodlands School, Opotiki 3 114 Whakatohea iwi Social and Health Services
Te Kura o Torere 2 28 Whakatohea iwi Social and Health Services
Te Kura Kaupapa Maori o Waioeka 1 73 Whakatohea iwi Social and Health Services
Waiotahe Valley School 3 100 Whakatohea iwi Social and Health Services
Opotiki Primary 1 262 Whakatohea iwi Social and Health Services
Opotiki College 2 470 Whakatohea iwi Social and Health Services
Murupara Area School 1 311 Te Ika Whenua Hauora
41
Te Kura Kaupapa Motuhake o Tawhiuau, Murupara 1 127 Te Ika Whenua Hauora
Ruatoki School 2 157 Te Kaokao o Takapau, Tuhoe
Taneatua School 1 215 Te Kaokao o Takapau, Tuhoe
Tawera Bilingual School 2 34 Te Kaokao o Takapau, Tuhoe
Te Kura Mana Maori o Matahi 1 32 Te Kaokao o Takapau, Tuhoe
Te Kura Maori-a-Rohe Waiohau 1 33 Te Kaokao o Takapau, Tuhoe
Waimana School 2 38 Te Kaokao o Takapau, Tuhoe
Te Kura Kaupapa Maori o Huiarau, Ruatahuna 1 72 Hinepukohurangi Trust, Tuhoe
Te Kura Toitu o Te Whaiti-nui-a-Toi 1 34 Hinepukohurangi Trust, Tuhoe
Gate Pa School, Tauranga 2 272 Te Manu Toroa
Greerton Village School, Tauranga 2 347 Te Manu Toroa
Merivale School, Tauranga 1 139 Te Manu Toroa
29 Schools in Total 1-3 4,551 6 providers in total
Notes:
1. Roll and decile data accurate as at July 2014. 2. Not all children on the roll are consented to take part in the programme. However consent rates are about 98% overall, with some
schools having 100% enrolment. 3. Consented children with sore throats self-present in classes to the Community Health Workers/Nurses who take the swabs. Children
with positive swabs are then followed up with antibiotic treatment. This work is accompanied by education and awareness raising at community, school, family/whanau and child levels.
4. The Ministry of Health contracts with Te Kaokao o Takapau (shortly to be transferred to Tuhoe Hauora), who subcontract Hinepukohurangi Trust to deliver programmes in two schools. The other providers are contracted by the BOPDHB.
42
5. The earliest programmes began in Opotiki over five years ago. Programmes have been progressively started since in Kawerau, then Murupara, Tuhoe rohe and Tauranga. The initial priority populations of Opotiki, Kawerau and Murupara were identified by Dr Belinda Loring in her report completed in 2008. School-based throat swabbing programmes are recommended under guidelines prepared by the New Zealand Heart Foundation and the Cardiac Society of Australia and New Zealand when the incidence of acute rheumatic fever exceeds 50/100,000 children aged 5-14. Census Area Units covering Opotiki, Murupara and Kawerau exceeded that threshold and programmes were accordingly developed. The threshold was also exceeded in the Whakatane West Census Area Unit, but this community was less discrete and self-contained, so a service was not prioritised at that time. However new services (see below) will address this gap shortly.
6. From Term 2 2015, rapid response clinics were established in further schools in Whakatane (Trident High School, Allandale Primary, James Street Primary and Whakatane Intermediate); and Edgecumbe (Edgecumbe Primary, Edgecumbe College).