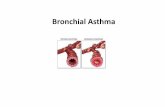
Asthma
description
Transcript of Asthma

AsthmaAsthma

AsthmaAsthma DefinitionDefinition
AsthmaAsthma DefinitionDefinition
Reactive airway disease Chronic inflammatory lung disease
Inflammation causes varying degrees of Inflammation causes varying degrees of obstruction in the airwaysobstruction in the airways
Asthma is reversible in early stages

Triggers of AsthmaTriggers of AsthmaTriggers of AsthmaTriggers of Asthma
AllergensAllergens ExerciseExercise Respiratory InfectionsRespiratory Infections Nose and Sinus problemsNose and Sinus problems Drugs and Food AdditivesDrugs and Food Additives GERDGERD Emotional StressEmotional Stress

Early and Late Phases of Responses of Early and Late Phases of Responses of AsthmaAsthma
Early and Late Phases of Responses of Early and Late Phases of Responses of AsthmaAsthma
Fig. 28--1

AsthmaAsthmaPathophysiologyPathophysiology
AsthmaAsthmaPathophysiologyPathophysiology
Bronchospasm Airway inflammation

AsthmaAsthmaPathophysiologyPathophysiology
AsthmaAsthmaPathophysiologyPathophysiology
Early-Phase ResponseEarly-Phase Response PPeaks 30-60 minutes post exposure, subsides 30-
90 minutes later Characterized primarily by bronchospasm Increased mucous secretion, edema formation,
and increased amounts of tenacious sputum Patient experiences wheezing, cough, chest
tightness, and dyspnea

AsthmaAsthmaPathophysiologyPathophysiology
AsthmaAsthmaPathophysiologyPathophysiology
Late-Phase ResponseLate-Phase Response Characterized primarily by inflammationCharacterized primarily by inflammation Histamine and other mediators set up a self-
sustaining cycle increasing airway reactivity causing hyperresponsiveness to allergens and other stimuli
Increased airway resistance leads to air trapping in alveoli and hyperinflation of the lungs
If airway inflammation is not treated or does not resolve, may lead to irreversible lung damage

Factors Causing Airway Obstruction in Factors Causing Airway Obstruction in AsthmaAsthma
Factors Causing Airway Obstruction in Factors Causing Airway Obstruction in AsthmaAsthma
Fig. 28--3

Summary of Pathophysiologic Summary of Pathophysiologic FeaturesFeatures
Summary of Pathophysiologic Summary of Pathophysiologic FeaturesFeatures
Reduction in airway diameter Increase in airway resistance r/t
Mucosal inflammation Constriction of smooth muscle Excess mucus production

AsthmaAsthmaClinical ManifestationsClinical Manifestations
AsthmaAsthmaClinical ManifestationsClinical Manifestations
Unpredictable and variable
Recurrent episodes of wheezing, breathlessness, cough, and tight chest

AsthmaAsthmaClinical ManifestationsClinical Manifestations
AsthmaAsthmaClinical ManifestationsClinical Manifestations
Expiration may be prolonged from a inspiration-expiration ratio of 1:2 to 1:3 or 1:4
Between attacks may be asymptomatic with normal or near-normal lung function

AsthmaAsthmaClinical ManifestationsClinical Manifestations
AsthmaAsthmaClinical ManifestationsClinical Manifestations
Wheezing is an unreliable sign to gauge severity of attack
Severe attacks can have no audible wheezing due to reduction in airflow
“Silent chest” is ominous sign of impending respiratory failure

AsthmaAsthmaClinical ManifestationsClinical Manifestations
AsthmaAsthmaClinical ManifestationsClinical Manifestations
Difficulty with air movement can create a feeling of suffocation Patient may feel increasingly anxious Mobilizing secretions may become difficult

AsthmaAsthmaClinical ManifestationsClinical Manifestations
AsthmaAsthmaClinical ManifestationsClinical Manifestations
Examination of the patient during an acute attack usually reveals signs of hypoxemia Restlessness Increased anxiety Inappropriate behavior Increased pulse and blood pressure Pulsus paradoxus (drop in systolic BP during
inspiratory cycle >10)

AsthmaAsthmaComplicationsComplications
AsthmaAsthmaComplicationsComplications
Status asthmaticus Severe, life-threatening attack refractory
to usual treatment where patient poses risk for respiratory failure

AsthmaAsthmaDiagnostic StudiesDiagnostic Studies
AsthmaAsthmaDiagnostic StudiesDiagnostic Studies
Detailed history and physical exam Pulmonary function tests Peak flow monitoring Chest x-ray ABGs

AsthmaAsthmaDiagnostic StudiesDiagnostic Studies
AsthmaAsthmaDiagnostic StudiesDiagnostic Studies
Oximetry Allergy testing Blood levels of eosinophils Sputum culture and sensitivity

AsthmaAsthmaCollaborative CareCollaborative Care
AsthmaAsthmaCollaborative CareCollaborative Care
Education Start at time of diagnosis Integrated into every step of clinical care
Self-management Tailored to needs of patient Emphasis on evaluating outcome in terms of
patient’s perceptions of improvement

AsthmaAsthmaCollaborative CareCollaborative Care
AsthmaAsthmaCollaborative CareCollaborative Care
Acute Asthma EpisodeAcute Asthma Episode O2 therapy should be started and monitored
with pulse oximetry or ABGs in severe cases Inhaled -adrenergic agonists by metered
dose using a spacer or nebulizer Corticosteroids indicated if initial response is
insufficient

AsthmaAsthmaCollaborative CareCollaborative Care
AsthmaAsthmaCollaborative CareCollaborative Care
Acute Asthma EpisodeAcute Asthma Episode
Therapy should continue until patient• is breathing comfortably • wheezing has disappeared• pulmonary function study results are
near baseline values

AsthmaAsthmaCollaborative CareCollaborative Care
AsthmaAsthmaCollaborative CareCollaborative Care
Status asthmaticusStatus asthmaticus Most therapeutic measures are the same as
for acute Increased frequency & dose of
bronchodilators Continuous -adrenergic agonist nebulizer
therapy may be given

AsthmaAsthmaCollaborative CareCollaborative Care
AsthmaAsthmaCollaborative CareCollaborative Care
Status asthmaticusStatus asthmaticus IV corticosteroids Continuous monitoring Supplemental O2 to achieve values of 90% IV fluids are given due to insensible loss of
fluids Mechanical ventilation is required if there is
no response to treatment

AsthmaAsthma Drug TherapyDrug Therapy
AsthmaAsthma Drug TherapyDrug Therapy
Long-term control medications Achieve and maintain control of persistent
asthma
Quick-relief medications Treat symptoms of exacerbations

AsthmaAsthmaDrug TherapyDrug Therapy
AsthmaAsthmaDrug TherapyDrug Therapy
BronchodilatorsBronchodilators -adrenergic agonists-adrenergic agonists
(e.g., albuterol, salbutamol[Ventolin])(e.g., albuterol, salbutamol[Ventolin])Acts in minutes, lasts 4 to 8 hoursShort-term relief of bronchoconstriction Treatment of choice in acute exacerbations

AsthmaAsthmaDrug TherapyDrug Therapy
AsthmaAsthmaDrug TherapyDrug Therapy
BronchodilatorsBronchodilatorsUseful in preventing bronchospasm
precipitated by exercise and other stimuliOveruse may cause rebound bronchospasmToo frequent use indicates poor asthma
control and may mask severity

AsthmaAsthmaDrug TherapyDrug Therapy
AsthmaAsthmaDrug TherapyDrug Therapy
Bronchodilators (longer acting)Bronchodilators (longer acting)8 – 12 or 24 hr; useful for nocturnal asthma
Avoid contact with tongue to decrease side effects
Can be used in combination therapy with inhaled corticosteroid

AsthmaAsthmaDrug TherapyDrug Therapy
AsthmaAsthmaDrug TherapyDrug Therapy
Antiinflammatory drugsAntiinflammatory drugs Corticosteroids (e.g., beclomethasone, Corticosteroids (e.g., beclomethasone,
budesonide)budesonide)Suppress inflammatory responseInhaled form is used in long-term controlSystemic form to control exacerbations and
manage persistent asthma

AsthmaAsthmaDrug TherapyDrug Therapy
AsthmaAsthmaDrug TherapyDrug Therapy
Antiinflammatory drugsAntiinflammatory drugs Corticosteroids Corticosteroids
Do not block immediate response to allergens, irritants, or exercise
Do block late-phase response to subsequent bronchial hyperresponsiveness
Inhibit release of mediators from macrophages and eosinophils

AsthmaAsthmaDrug TherapyDrug Therapy
AsthmaAsthmaDrug TherapyDrug Therapy
Anti-inflammatory drugsAnti-inflammatory drugs Mast cell stabilizers (e.g., cromolyn, nedocromil)Mast cell stabilizers (e.g., cromolyn, nedocromil)
Inhibit release of histamineInhibit release of histamineInhibit late-phase responseLong-term administration can prevent and reduce
bronchial hyper-reactivityEffective in exercise-induced asthma when used 10
to 20 minutes before exercise

AsthmaAsthmaDrug TherapyDrug Therapy
AsthmaAsthmaDrug TherapyDrug Therapy
Leukotriene modifiers (e.g. Singulair) Leukotriene – potent bronchco-constrictors
and may cause airway edema and inflammation
Have broncho-dilator and anti-inflammatory effects

AsthmaAsthmaPatient Teaching Related to DrugPatient Teaching Related to Drug
TherapyTherapy
AsthmaAsthmaPatient Teaching Related to DrugPatient Teaching Related to Drug
TherapyTherapy
Correct administration of drugs is a major Correct administration of drugs is a major factor in determining success in asthma factor in determining success in asthma managementmanagement Some persons may have difficulty using an MDI
and therefore should use a spacer or nebulizer DPI (dry powder inhaler) requires less manual
dexterity and coordination

AsthmaAsthmaPatient Teaching Related to DrugPatient Teaching Related to Drug
TherapyTherapy
AsthmaAsthmaPatient Teaching Related to DrugPatient Teaching Related to Drug
TherapyTherapy
Inhalers should be cleaned by removing dust cap and rinsing with warm water
-adrenergic agonists should be taken first if taking in conjunction with corticosteroids

Nursing ManagementNursing ManagementNursing DiagnosesNursing Diagnoses
Nursing ManagementNursing ManagementNursing DiagnosesNursing Diagnoses
Ineffective airway clearance
Anxiety
Ineffective therapeutic regimen management

Nursing ManagementNursing ManagementPlanningPlanning
Nursing ManagementNursing ManagementPlanningPlanning
Normal or near-normal pulmonary function Normal activity levels No recurrent exacerbations of asthma or
decreased incidence of asthma attacks Adequate knowledge to participate in and
carry out management

Nursing ManagementNursing ManagementHealth PromotionHealth Promotion
Nursing ManagementNursing ManagementHealth PromotionHealth Promotion
Teach patient to identify and avoid known triggersUse dust coversUse of scarves or masks for cold airAvoid aspirin or NSAIDs
Desensitization can decrease sensitivity to allergens

Nursing ManagementNursing ManagementHealth PromotionHealth Promotion
Nursing ManagementNursing ManagementHealth PromotionHealth Promotion
Prompt diagnosis and treatment of upper respiratory infections and sinusitis may prevent exacerbation
Fluid intake of 2 to 3L every day

Nursing ManagementNursing ManagementHealth PromotionHealth Promotion
Nursing ManagementNursing ManagementHealth PromotionHealth Promotion
Adequate nutrition Adequate sleep Take -adrenergic agonist 10 to 20
minutes prior to exercising

Nursing ManagementNursing ManagementNursing ImplementationNursing ImplementationNursing ManagementNursing ManagementNursing ImplementationNursing Implementation
Acute Intervention Monitor respiratory and cardiovascular
systemsLung soundsRespiratory ratePulseBP

Nursing ManagementNursing ManagementNursing ImplementationNursing ImplementationNursing ManagementNursing ManagementNursing ImplementationNursing Implementation
ABGsPulse oximetryFEV and PEFRWork of breathing
Response to therapy

Nursing ManagementNursing ManagementNursing ImplementationNursing ImplementationNursing ManagementNursing ManagementNursing ImplementationNursing Implementation
Nursing InterventionsNursing InterventionsAdminister O2
BronchodilatorsChest physiotherapyMedications (as ordered)Ongoing patient monitoring

Nursing ManagementNursing ManagementNursing ImplementationNursing ImplementationNursing ManagementNursing ManagementNursing ImplementationNursing Implementation
An important goal of nursing is to decrease An important goal of nursing is to decrease the patient’s sense of panicthe patient’s sense of panic Stay with patient Encourage slow breathing using pursed lips for
prolonged expiration Position comfortably

Nursing ManagementNursing ManagementNursing ImplementationNursing ImplementationNursing ManagementNursing ManagementNursing ImplementationNursing Implementation
The patient must learn about medications and develop self-management strategies
Patient and health care professional must monitor responsiveness to medication
Patient must understand importance of continuing medication when symptoms are not present

Nursing ManagementNursing ManagementNursing ImplementationNursing ImplementationNursing ManagementNursing ManagementNursing ImplementationNursing Implementation
Important patient teaching: Seek medical attention for bronchospasm or
when severe side effects occur Maintain good nutrition Exercise within limits of tolerance

Nursing ManagementNursing ManagementNursing ImplementationNursing ImplementationNursing ManagementNursing ManagementNursing ImplementationNursing Implementation
Important patient teaching (cont.): Patient must learn to measure their peak flow
at least daily Asthmatics frequently do not perceive changes
in their breathing

Nursing ManagementNursing ManagementNursing ImplementationNursing ImplementationNursing ManagementNursing ManagementNursing ImplementationNursing Implementation
Counseling may be indicated to resolve problems
Relaxation therapies may help relax respiratory muscles and decrease respiratory rate

Nursing ManagementNursing ManagementNursing ImplementationNursing ImplementationNursing ManagementNursing ManagementNursing ImplementationNursing Implementation
Peak Flow ResultsPeak Flow Results GreenGreen zonezone
Usually 80-100% of personal best Remain on medications

Nursing ManagementNursing ManagementNursing ImplementationNursing ImplementationNursing ManagementNursing ManagementNursing ImplementationNursing Implementation
Peak Flow ResultsPeak Flow Results Yellow zoneYellow zone
Usually 50-80% of personal best Indicates caution Something is triggering asthma

Nursing ManagementNursing ManagementNursing ImplementationNursing ImplementationNursing ManagementNursing ManagementNursing ImplementationNursing Implementation
Peak Flow ResultsPeak Flow Results Red zoneRed zone
50% or less of personal best Indicates serious problem Definitive action must be taken with health care
provider