Anterior Uveitis
-
Upload
hossein-mirzaie -
Category
Health & Medicine
-
view
17.153 -
download
5
Transcript of Anterior Uveitis

Anterior Uveitis

Anterior Uveitis
• Prevalence
• Symptoms
• Diagnostic techniques and signs
• Pathophysiology
• Associated conditions
• Management

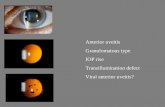
Anterior Uveitis - Introduction
• Unilateral• Asymmetrical• Inflammation of the uvea anterior to the middle of
the vitreous cavity• One of the serious “red eye” conditions• Associated with trauma• Associated with systemic disease• Has vision threatening complications

Anterior Uveitis - Prevalence
• The most common form of intraocular inflammatory disease
• We must consider incidence, not prevalence• 8-12 per 100,000 population per year• Highest in age range 20-50 (20-30 is peak)• Risk factors
– Associated systemic conditions– Blunt trauma– Previous history

Anterior Uveitis – History & Symptoms
• History of blunt trauma• History of associated systemic condition• If acute:
– Painful eye– Watery eye– Photophobia– Mild to moderate reduction in vision
• If chronic:– No symptoms

Anterior Uveitis – Diagnostic Techniques & Signs
• Monocular Visual Acuity measurement
• Slit lamp biomicroscopy
• Tonometry
• Gonioscopy?

Anterior Uveitis – Diagnostic Techniques & Signs
• Monocular Visual Acuity measurement– Reduced to 6/6-6/9 in mild disease
– Reduced to 6/9-6/30 in moderate disease
– Reduced to <6/30 in severe disease
• Visual Acuity reduced due to:– Corneal oedema
– Aqueous flare
– Aqueous cells
– Cystoid macular oedema (CME)

Anterior Uveitis – Diagnostic Techniques & Signs
• Slit lamp biomicroscopy– Circumlimbal injection– AC flare and cells– Keratic precipitates (KP)– Pupil miosis– Hypopyon– Band Keratopathy

Anterior Uveitis – Diagnostic Techniques & Signs
• Slit lamp biomicroscopy– Fibrin in the AC– Cells in the anterior vitreous– Peripheral Anterior Synechiae (PAS)– Posterior synechiae– Rubeosis iridis– Mutton fat KP (granulomatous disease)– Iris nodules (granulomatous disease)

Anterior Uveitis – Diagnostic Techniques & Signs
• Tonometry– IOP reduced– IOP unaffected– IOP elevated (corneal oedema)
• Gonioscopy– PAS

Anterior Uveitis – Diagnostic Techniques & Signs
Circumlimbal injection

Anterior Uveitis – Diagnostic Techniques & Signs
Circumlimbal injection

Anterior Uveitis – Diagnostic Techniques & Signs
Aqueous Flare

Anterior Uveitis – Diagnostic Techniques & Signs
Cells in aqueous

Anterior Uveitis – Diagnostic Techniques & Signs
Grading of cells and flare
Grade Flare Cells0 Complete absence No cells
1+ Faint flare (barely detectable)
5 to 10 cells in view
2+ Moderate flare (iris and lens still clear)
10 to 20 cells in view
3+ Marked flare (iris and lens hazy)
20 to 50 cells in view
4+ Intense flare (coagulated aqueous, no circulation, fibrin visible)
50+ cells in view

Anterior Uveitis – Diagnostic Techniques & Signs
Keratic Precipitates

Anterior Uveitis – Diagnostic Techniques & Signs
Hypopyon vs Hyphaema

Anterior Uveitis – Diagnostic Techniques & Signs
Hypopyon vs Hyphaema

Anterior Uveitis – Diagnostic Techniques & Signs
Band Keratopathy

Anterior Uveitis – Diagnostic Techniques & Signs
Fibrin in aqueous

Anterior Uveitis – Diagnostic Techniques & Signs
Fibrin in aqueous

Anterior Uveitis – Diagnostic Techniques & Signs
Posterior Synechiae





Anterior Uveitis – Diagnostic Techniques & Signs
Rubeosis Iridis

Anterior Uveitis – Diagnostic Techniques & Signs
Mutton Fat Keratic Precipitates

Anterior Uveitis – Diagnostic Techniques & Signs
Iris Nodules

Anterior Uveitis – Diagnostic Techniques & Signs
Severe Acute Anterior Uveitis

Anterior Uveitis – Diagnostic Techniques & Signs
Gonioscope view of Peripheral Anterior Synechiae (PAS)

Anterior Uveitis – Classification
• Uveitis by location:– Anterior Uveitis
• Iritis• Iridocyclitis• Cyclitis
– Intermediate Uveitis• Pars planitis
– Posterior Uveitis• Choroiditis• Chorioretinities• Retinochoroiditis• Retinitis
– Panuveitis

Anterior Uveitis – Classification
• Uveitis by time course:– Acute
• < 6 weeks duration• May be recurrent
– Chronic• > 6 weeks duration• White eye• Mild signs of inflammation• Mild or no symptoms

Anterior Uveitis – Classification
• Chronic Anterior Uveitis associated with:– Juvenile chronic arthritis– Posterior Uveitis due to:
• Sarcoidosis• Toxoplasmosis• Syphilis• Tuberculosis• Herpes Zoster• Cytomegalovirus• AIDS
– Fuch’s Heterochromic Iridocyclitis• Asymptomatic• 2% of uveitis patients• Progressive loss of iris stromal pigment -> heterochromia• Mild inflammation resistant to treatment

Anterior Uveitis – Classification
• Source:– Endogenous– Exogenous
• trauma• surgery
• Inflammatory process:– Granulomatous– Non-granulomatous
• Unable to find cause?– “idiopathic anterior uveitis” – 30% of all cases

Anterior Uveitis – Classification of Severity
Clinical Degree of Anterior Uveitis
Mild Moderate SevereMild to moderate Symptoms
VA 6/6 to 6/9
Superficial circumcorneal flush
No KPs
0-1+ cells and flare
Moderate to severe symptoms
AV 6/9 to 6/30
Deep circumcorneal flush
KPs
1-3+ cells and flare
Moderate to severe symptoms
VA <6/30
Deep circumcorneal flush
KPs
3-4+ cells and flare

Anterior Uveitis – Classification of Severity
Clinical Degree of Anterior Uveitis
Mild Moderate SevereNormal pupil .
No posterior synechiae
No iris swelling
IOP reduced <4mmHg
Miotic, sluggish pupil
Mild posterior synechiae
Mild iris swelling
IOP reduced 3-6 mmHg
Anterior vitreous cells
Sluggish or fixed pupil
Fibrous posterior synechiae
Boggy iris (crypts)
IOP increased
Moderate to severe anterior vitreous cells

Anterior Uveitis – Pathophysiology
• Non-granulomatous– No pathogen– Responsive to topical treatment
• Granulomatous– Pathogen induced– Less responsive to topical treatment

Anterior Uveitis – Pathophysiology
• Inflammatory response causes breakdown of the blood-aqueous barrier
• Plasma protein -> Flare• Cells are WBC• Fibrin derives from clotting factors• Deposition of cells and proteins
– KP– Hypopyon

Anterior Uveitis – Pathophysiology
• Deposition of calcium salts in cornea– Band keratopathy– Only after recurrent attacks
• Inflammation causes iris tissue to become sticky– PAS -> reduced aqueous outflow -> IOP+– Posterior synechiae -> pupil block -> IOP+++
• Deposition of Macrophages– Mutton Fat KP– Iris nodules

Anterior Uveitis – Pathophysiology
• Circumlimbal injection– Due to common blood supply with uveal vessels
• Lack of normal oxygen supply to iris– Vessel growth factors released
– Leaky new vessel growth on iris
– Rubeosis Iridis
– Extension of vessels into AC angle
– ACG

Anterior Uveitis – Management
• Chronic - Early referral to GP if not being managed currently
• Recurrent acute episode – Urgent referral to GP for prescription of treatment regimen and monitoring
• Acute episode, previously undiagnosed – Urgent referral to hospital eye casualty department
• All patients – check IOP. If raised refer to GP or casualty depending on level
• Counsel patients on importance of condition

Anterior Uveitis – Management
• Goals of management– Preserve visual acuity– Relieve ocular pain– Eliminate ocular inflammation– Identify the source of inflammation– Prevent formation of synechiae– Control the IOP

Anterior Uveitis – Management
• Treatment regimen– Topical Corticosteroid therapy
• Reduce inflammation• Reduce exudate leakage• Increase cell wall stability• Inhibit lysozyme release by granulocytes• Inhibit circulation of lymphocytes
– Cycloplegia• Relieve pain• Prevent posterior synechiae• Stabilize the blood-aqueous barrier
– Systemic steroid therapy– Systemic NSAID therapy (aspirin, ibuprofen)

Anterior Uveitis – Associated Conditions
• Blunt Trauma• Ocular Surgery• Juvenile Chronic Arthritis• Ankylosing Spondylitis• Reiter’s syndrome• Sarcoidosis• Tuberculosis• Herpes Zoster• Herpes Simplex• Syphilis• Hypermature Cataract• Lens Rupture• Sympathetic ophthalmitis• Fuch’s heterochromic iridocyclitis

Anterior Uveitis – Clinical Pearls
• Four major complications exist– Cataract– Secondary glaucoma– Band keratopathy– Cystoid macular oedema
• Easy to spot acute by signs & symptoms• Check patients with associated systemic conditions for chronic
condition, which may be asymptomatic• Acute condition is most commonly caused by blunt trauma.
Recurrence in such cases is rare• Any three recurrent acute episodes, with no other explanations,
indicates a systemic cause