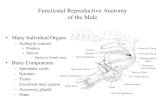
Anatomy & Physiology Unit 12: Urogenital System. Male Anatomy Testicles: 2 per male-located within...
-
Upload
marian-lorin-long -
Category
Documents
-
view
219 -
download
1
Transcript of Anatomy & Physiology Unit 12: Urogenital System. Male Anatomy Testicles: 2 per male-located within...
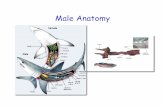
Male Anatomy
Testicles: 2 per male-located within the scrotum for temperature control
Have 2 functions: 1. Endocrine function: making
testosterone Interstitial cells: distinct cells that produce
testosterone 2. Exocrine function: producing sperm
Male Anatomy
Sperm Producing Structures (within testicles)
1. Seminiferous tubules Tubes coiled together to form lobules in
the testes “Sperm-forming factories”
2. Rete testesreceives sperm from seminiferous tubules
Male Anatomy
Sperm Producing Structures (within testicles)
3. Epidydimus Highly coiled, 20 ft. tube Sperm stay here for 20 days to mature Will contract w/ stimulation to expel
sperm
Male Anatomy
Sperm Producing Structures (within testicles)
4. Vas (ductus) Deferens Functions to propel sperm from storage to
urethra Runs from testes to pelvic cavity Enclosed in spermatic cord with blood
vessels—empties into ejaculatory duct Vasectomy: small incision through
scrotum to close off vas deferens
Male Anatomy
5. Urethra Runs from base of bladder to tip of penis Function: transports urine and semen Bladder sphincter closes upon ejaculation
so no urine is expelled and no semen enters the bladder
Male Accessory Organs
All contribute to the contents of semen Semen:
Milky, white and somewhat sticky Provides a transport medium & nutrients;
contains chemicals to protect the sperm Alkaline to protect sperm against acidity of
vagina
**sperm cannot swim in acidic environments
Male Accessory Organs
1. Seminal Vesicles Produces ~ 60% of fluid volume of
semen Full of vitamin C and sugar to nourish
sperm
2. Prostate Gland Gland below the bladder which surrounds
the urethra Adds a milky fluid to semen which helps
activate the sperm
Male Accessory Organs
3. Bulbourethral Gland Pea-sized gland Produces the pre-ejaculate: clear and
thick mucus that flushes through the urethra with stimulation, cleaning away acidic urine; also a lubricant
Male Anatomy: External Genitalia
1. Scrotum: a divided sac hanging outside abdominal cavity Holds testicles Can adjust location to be closer to body
when cold, and further when hot Sperm only produced when at a
temperature 3 degrees cooler than body temperature
Male Anatomy: External Genitalia
2. Penis: designed to deliver sperm into female; consists of: A shaft Glans penis: the tip covered by prepuce
(foreskin) Internally is the urethra and erectile tissue Erectile tissue fills with blood during an
erection
Female Anatomy
Ovaries: 2 small glands located in pelvic cavity Endocrine Functions: produce estrogen
and progesterone Exocrine Functions: make ova (eggs)
Female Anatomy
Ova Producing Structures: within ovaries1. Ovarian Follicles: tiny sacs that hold oocytes
(immature eggs) Surrounded by follicle cells Oocyte will mature here
2. Graafian Follicles: a mature egg which is ready to be ejected from the ovary during ovulation
3. Corpus Luteum: the ruptured follicle after ovulation
Usually degenerates unless fertilized
Female Anatomy
Duct System1. Uterine (Fallopian) Tubes Receives an ovulated oocyte and
provides a site for fertilization Does not actually come in contact with
ovary Fimbrae: finger-like projections which
wave to create a fluid current to direct oocyte to fallopian tubes
Female Anatomy
Duct System
2. Uterus (the womb) Hollow organ that receives, retains and
nourishes a fertilized egg Size of a pear in women who have not
been pregnant Cervix: narrow outlet of uterus
Female Anatomy
Uterus Continued There are 3 layers to the walls of the
uterus Endometrium: the inner mucosa layer of
uterus where fertilized egg burrows into and resides during development (implantation)
Myometrium: the muscular, middle layer which contracts during labor
Epimetrium: the outermost layer of uterus
Female Anatomy
Duct System
3. Vagina (birth canal) Thin walled tube, ~ 3-4 inches long Provides a passageway for the delivery
of an infant and for menstrual flow to leave body
Female Anatomy: External Genitalia1. Mons Pubis: fat pad over pubic bone2. Labia Majora: large folds of skin3. Labia Minora: smaller, more interior folds of
skin4. Clitoris: erectile tissue anterior to labia
minora junction5. Urethra: opening located between clitoris and
vaginal opening6. Perineum: area of skin between vaginal
opening and anus1. Episiotomy: the surgical cutting of perineum
during childbirth
The Menstrual Cycle
On average, takes about 28 days 3 stages
1. Menses (days 1-5) thick endomerial wall detaching from
uterus causes 3-5 days of menstrual flow
(bleeding)
The Menstrual Cycle
2. Proliferative Stage (days 6-14) endometrial wall repaired and blood
supply increased in response to rising estrogen levels
vvulation occurs on day 14 because of spike of blood LH levels
The Menstrual Cycle
3. Secretory Stage (days 15-28) endometrial gland secretion increases
nutrients within uterus progesterone levels high fertilization causes embryo to produce
hormone which maintains endometrial lining
no fertilization causes endometrial blood vessels to end its supply
menses occurs at day 28
Fertilization
The egg: only viable for 12-24 hours post-ovulation
The sperm: can remain fertile in female tract for 12-48 hours (sometimes up to 72 hours) Are attracted to chemical signals from the
egg For fertilization to occur intercourse must
happen 72 hours before ovulation or within 24 hours after
Fertilization
When the sperm reaches the oocyte: acrosomes rupture releasing enzymes to break away surrounding of oocyte First sperm in WINS!
Embryonic and Fetal Development
The zygote: the first cell created from fertilization
Cleavage: early stage of embryonic development Rapid mitotic divisions occur as embryo
moves toward uterus Morula: a solid ball of cells
Enters uterus around days 5-6
Embryonic and Fetal Development
Blastocyst: 100 cell embryo Hollowed out and filled with fluid Free floats in uterus Secrets human chorionic gonadoptropin
(hCG) hCG tells corpus luteum to keep up
hormone production **hCG hormone in urine used to detect
pregnancies
Embryonic and Fetal Development
By Day 7: late blastocyst stage Starts uterine attachment—embeds into
endometrium Cells start re-arranging themselves
1. trophoblast: the fluid filled sphere
2. Inner cell mass: small cluster of cells displace to one side
Embryonic and Fetal Development
Once placenta has formed (functional by third week) the mom’s blood supply is now connected to the babies via the umbilical cord
Nutrients are fed into the amnion (fluid filled sac) where baby develops
Embryonic and Fetal Development
Germ Layers form next (3)
1. Ectoderm: make up the nervous system and skin
2. Endoderm: forms mucosa and glands
3. Mesoderm: forms all else (muscles, bones, etc.)
Embryonic and Fetal Development
Week 3: placenta functions—delivers nutrients, disposes of wastes
Week 8: placenta making progesterone and estrogen to help maintain pregnancy Organ systems groundwork established
Week 9: now a fetus Growth and organ specialization Body proportions develop
Embryonic and Fetal Development
12 weeks: sex is discernable Month 4: looks human
Can suck lips and blink eyes Month 5: limbs near full-size
More muscular activity from baby Months 6 & 7
Weight increase Eyes open
The Mom
Anatomical Changes: Uterus crowds abdominal cavity Center of gravity changes Lumbar lordosis = back pain Relaxin causes pelvis to expand (ligaments
relax) Needs 300 extra calories daily
The Mom
Physiological Changes Morning sickness due to hormonal changes Heartburn because of displacement of esophagus Frequent and urgent urination—incontinence Nasal stuffiness (estrogen) VC increases –dyspnea Blood volume increases 25-40% Varicose veins
Parturition aka childbirth
Occurs ~ 280 days after last menstrual period Labor: series of events that expel infant from
uterus Triggers to induce labor:
High estrogen and low progesterone Braxton Hicks: weak contractions aka false labor False labor becomes actual labor when oxytocin
and prostaglandins are released
Parturition aka childbirth
3 stages of labor: Stage 1: Dilation
From true contractions to full dilation of cervix (10 cm.)
Contractions move in waves from superior uterus inferiorly
Amnion ruptures (water breaks)
Parturition aka childbirth
Stage 2: Expulsion Stage From full dilation to delivery Can take from 20 mins. to 2 hours Baby should exit head first Buttocks first is called breech