Acute Glomerulonephritis
description
Transcript of Acute Glomerulonephritis

Nephrology DivisionKing Khalid University
Tutorial Med Course 441
1

14 year old Saudi Malec/o fever-headache for 10 daysGeneral malaiseDark urine x 3 days
2

HPIFever
intermittentMuscular joint
painUrine character Edema No skin rash
3

PH & Med◦Antibiotic and NSAID
Social HxS. reviewFH
4

Examination BP : 160/90 mmHg and pulse rate: 120/minTemperature : 39 ºC Respiration: 25/min. paleLook SickPuffiness in faceHead and neckJVP
5

Chest ExaminationNormal percussionNormal TVFNormal breath soundVesicular breathingS1 increaseS2 NS3 positivePansystolic murmur
◦Radiation to axilla◦Grade IIII 6

Abd◦Tend epigastic◦Tend loins◦BS +ve
CNS◦Normal
M.S. /Normal
7

Initial Diagnosis
Fever? Infection vs autoimmune Disease
Murmur ; M R vs VSD
HEAMATURIA
Urine Sample with hematuria 8

Initial Diagnosis
Hematuria Systemic
◦ Hemolytic Anemia◦ Embolization ◦ Anti-coagulant
Surgical◦ Stone ◦ Tumor◦ Papillary◦ APKD
Medical◦ Acute kidney injury◦ Glomerulonephritis◦ Rapid pogressive glomerulonephrtis◦ IgA Nephropathy
9

Differential Diagnosis of Hematuria ARF-AKI-ATN
◦ Acute glomerulonephritis (post-infection)
◦ RPGN◦ IgA◦ Hemolytic uremic syndrome◦ NSAID
Hemolytic Anemia
IgA Nephropathy Hemolytic uremic 10

InvestigationWBC 15,000 cells/microliter
◦ Hb – 100 g/L◦ Plat – 150 g/L◦ ESR 90
PT normal◦ PPT normal Sec◦ BI normal Sec
11

U&E Scr - 210µmol/LUrea – 20mmol/LK – 6mmol/LNa – 125 mmol/LCa – 1.9 mmol/LAlbumin – 28 g/L
12

Urine Analysis
Many RBCRed cell cast
abscentProtein – 1.2 g/24
hr
13

14

U/S : kid size ENLARGE 12.2 cm
15

16

17

Treatment Patient receive ceftriaxone IV and
IV fluidTREAT HYPERKALEMIA
18

19

Follow – up:S Cr – 300 µmmol/LJVPOliguriaEdema
20

Investigations for Glomerulonephritis
Regular follow-up and U&EAntistreptolysin O (ASO)ANA, Anti-DNAC3-C4ANCA (p,c)HCV Antibody (HBsAg)HIVRFCryoglobulinAnti-basement membrane anti-body
(with lung hemorrhage 21

Management IV LasixRepeat urine analysis
◦RBC castKidney biopsy : RPGNSerology tesy : all negativeRF: -negativeFinal diagnosisAnti-glomerular basement
membrane anti-bodies22

Glomerular Disease – Acute Glomerulonephritis
Post infectious glomerulonephritis
Group A Strep Infection Infective endcarditis
Membranoproliferative glomerulonephritis:
Systemic lupus erythematosus
Hepatitis C virus
IgA Nephropathy (Buerger’s Disease)
Rapidly progressive glomerulonephritis
Type I RPGN (direct antibody) Good Posture syndrome
Type II RPGN (immune complex)
Post infectious Systematic lupus erythematosus Henoch – Schonlein pupura (IgA)
Type III RPGN (pauci-immune) Vasculitis (, Wegener
granulomatosis; poiyarteritis nodosa-microscopic polyangitis)
23

Complications of acute glomerulonephritis
HypertensionPulmonary edemaHyperkalemiaEncephalopathy convulsionElectrolyte disturbancePericaditisGastroentritisPeptic ulcer
24

Management of Glomerulonephritis
Treat the causeConservative managementDialysis
25

Acute post-infection glomerulonephritis
Often associated with group AB-hemolytic streptococcal type 12
infectionAlso staphylococcus or viruses
26

Acute Glomerulonephritis
Symptoms occur 10-21 days after infection◦Hematuria◦Proteinuria (<1gm/24 hr)◦Decreased GFR, oliguria◦Hypertension◦Edema around eyes, feet and ankles◦Ascites or pleural effusion
Antistreptolysin O (ASO), Low C3, normal C4
◦Kidney biopsy immune complexes and proliferation 27

28

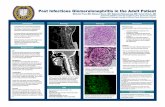
Proliferative GN-post streptococcal
This glomerulus is hypercellular and capillary loops are poorly defined This is a type of proloferative glomerulonephritis known as post-streptococcal
glomerulonephritis 29

Post-streptococcal GN
Post-streptococcal glomerulonephritis is immunologically mediated, and the immune deposits are distributed in the capillary loops in a granular, bumpy pattern because of the focal nature of the deposition process
30

31

Post-streptococcal glomerunephritis
Conservative Treatment (acute kidney injury
Improves 1 – 4 weeks, C3 normalizes in 1 – 3 months, hypertension improves 1 – 3 months, intermittent hematuria x 3 years
99% complete recovery in children and 85% in adult
32

IgA nephropathy (Buerger’s Disease) Most common acute
glomerulonephritis in US, South East Asia
Associated with H.S. Purpura Upper respiratory (50%) in 1 – 2
days (synpharyngitic hematuria) Primary versus secondary (IBD,
Liver disease, SLE, vasculitis) 50% risk of CRF Proteinuria, hypertension, renal
insufficiency predict worse prognosis
50% increase IgA, normal compliments
TREATMENT OF CONSERVATIVE ACEi
HIGH RISK: patient prednisone and alkylating agent
Cyclophosphamide-azothroprim & ASA & ACEi & tosilectomy 33

Rapid Progressive GNType I RPGN (direct antibody)
◦Good pasture syndromeType II RPGN(immune complex)
◦Post infectious◦Systematic lupus erythematosus◦Henoch-schonlein purpura (IgA)◦ cryoglobulinemia
Type II (pauci-immune)◦Vasculitis (, Wegener
granulomatosis, microscopic polyangitis,poplyarteries nodosa)
34

Rapidly progressive GN
Develops over a period of days and weeks
Primarily adults in 50’s and 60’sProgresses to renal failure in a few
weeks or monthsHematuria is common, may see
proteinuria, edema or hypertension
35

Rapidly progressive (Crescentic) GlomerulonephritisMorphology
◦Crescent formation◦Crescents are formed by
proliferation of parietal cells◦Infiltrates of WBC’s & fibrin
deposition in Bowman’s space◦EM reveals focal ruptures in the
GBM
36

37

38

39

40

Goodpasture Syndrome
Antibody formation against pulmonary and glomerular capillary basement membranes
Damage glomerular basement membrane
Men – 20 to 30 years of agePulmonary hemorrhage and renal
failure
TREATMENT Early treatment is essential Pulse steroid (10 mg/kg/day for 3 – 5
days)CyclophosphamidePlasmapheresis
41

Goodpasture’s syndrome
This immunoflourescence micrograph shows positivity with antibody to IgG has a smooth, diffuse, linear pattern that is characteristic for glomerular basement antibody with Goodpasture’s syndrome 42

Microscopic PolyangitisNecrotizing vasculitis of small – and
medium – sized vessels in both the arterial and venous circulations
Frequently involves the lung and the kidney with typical complications of hemorrhage and glomerulonephritis
Usually positive p-ANCA (anti-myeloperoxidase)
Usually positive c-ANCA (ant-proteinase 3)
43

44

45

Treatment Initial Therapy
Combination cyclophosphamide-corticosteroid therapy
Pulse methyl prednisone (10 mg/kg/day for 3-5 days)
A slow steroid taper, with the goal of reaching 20 mg of prednisone per day by the end of two months and an overall glucocorticoid course of between 6 and 9 months
Either daily oral or monthly intravenous cyclophosphamide
46

Treatment PlasmapheresisSevere manifestations of pumonary
hemorrhage on presentationDialysis – dependent renal failure
upon presentationConcurrent anti-GBM antibodies
47

48

49

50

Glomerular Disease – Acute Glomerulonephritis
Post infectious glomerulonephritis
Group A Strep Infection Infective endcarditis
Membranoproliferative glomerulonephritis:
Systemic lupus erythematosus
Hepatitis C virus
IgA Nephropathy (Buerger’s Disease)
Rapidly progressive glomerulonephritis
Type I RPGN (direct antibody) Good Posture syndrome
Type II RPGN (immune complex)
Post infectious Systematic lupus erythematosus Henoch – Schonlein pupura (IgA)
Type III RPGN (pauci-immune) Vasculitis (cryoglobulinemia,
Wegener granulomatosis; popular arteritis nodosa)
51

Hemolytic Anemia IgA Nephropathy hemolytic uremic 52

HPIFever
intermittentMuscular joint
pain No skin rashUrine character edema
53

Rapidly progressive glomerulonephritis
Immune Complex◦ Anti-pathogen Antibody – Post Infectious GN◦ IgA Nephropathy◦ Anti-nuclear antibodies – SLE◦ C3 Nephritis – MPGN ◦ Cryoglobulin – HCV and HBsAg
Anti-glomerular basement antibodies◦ GMB antibodies
Antineutrophil cytoplasmic antibodies (ANCA)◦ Wegener's granulomatosis◦ Microscopic polyangitis
54