Acls update class 2015
-
Upload
kandice-chandler -
Category
Healthcare
-
view
3.913 -
download
0
Transcript of Acls update class 2015
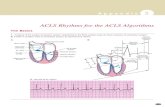
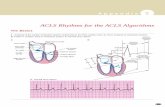
CPR REVIEW
ACLS UPDATEAHA 2010 GUIDELINES
CPR REVIEW
In a NutshellDefibrillation should take a maximum period of five seconds, with charging during chest compressions.
For tracheal intubation, ten seconds hands-off time for the passage of the tube is the only point at which compressions are paused.
Pulse checks are only undertaken where there are signs suggestive of ROSC.
In BLS, compression depth has been increased to between 5 & 6 cm. Studies have shown that a depth of 4-5 cm, as recommended before, was inadequate to achieve ROSC.
The use of feedback technology( separate units or integrated into defibrillators) promoted, to assist in the delivery of high-quality compressions.
AirwayAll healthcare providers should be able to provide ventilation with a bag-mask device during CPR or when the patient demonstrates cardiorespiratory compromise.
Airway control with an advanced airway, which may include an ETT or a supraglottic airway device, is a fundamental ACLS skill.
Prolonged interruptions in chest compressions should be avoided during advanced airway placement.
All providers should be able to confirm and monitor correct placement of advanced airways.
Training, frequency of use, and monitoring of success and complications are more important than the choice of a specific advanced airway device for use during CPR.
During CPR, oxygen delivery to the heart and brain is limited by blood flow rather than by arterial oxygen content.
Rescue breaths are less important than chest compressions during the first few minutes of resuscitation and could lead to interruption in chest compressions.
Increase in intra-thoracic pressure that accompanies positive pressure ventilation decreases CPR efficacy.
Advanced airway placement in cardiac arrest should not delay initial CPR and defibrillation for VF cardiac arrest
Oxygen Administration During CPRIt is unknown whether 100% inspired oxygen is beneficial or whether titrated oxygen is better.
Prolonged exposure to 100% inspired oxygen has potential toxicity.
Passive oxygen delivery via mask with an opened airway during the first 6 minutes of CPR provided by (EMS) resulted in improved survival.
In theory, as ventilation requirements are lower during cardiac arrest, oxygen supplied by passive delivery is likely to be sufficient for several minutes after onset of cardiac arrest with a patent upper airway.
ACLS PRINCIPLE:
IF ITS TOO FAST.SLOW IT DOWN
IF ITS TOO SLOW.SPEED IT UP
IF ITS NOT BEATING.BEAT THE PATIENT
TOO FASTELECTRICALDRUGS
TOO SLOWELECTRICALPACING: CALL FOR ORDERSA/P PAD PLACEMENT4 LEADSRATE AT 70 BPMSTART AT 0 mA AND INCREASE UNTIL CAPTUREDRUGS
NOT BEATINGELECTRICALDRUGS
Sodium BicarbonateUsed for METABOLIC acidosis AND hyperkalemiaAirway and ventilation have to be functional!
IV Dose:1 mEq/kg
Side effects:Metabolic alkalosisIncreased CO2 production
DopamineUsed for hypotension (not due to hypovolemia)Has alpha, beta, and dopaminergic propertiesDopaminergic dilates renal and mesenteric arteries
Second choice for bradycardia (after Atropine)
IV Dose:1-20 micrograms/kg
Side effects:Ectopic beatsN & V
Vasopressin (ADH)Similar effects to Epinephrine without as much cardiovascular side effects!
IV dose = 40 IU
Can be given down ET tube
May be better for asystole
EpinephrineBecause of alpha, beta-1, and beta-2 stimulation, it increases heart rate, stroke volume and blood pressureHelps convert fine Vfib to coarse VfibMay help in asystoleAlso PEA and symptomatic bradycardia
IV Dose:1 mg every 3-5 minutesCan be given down the ET tubeMay increase ischemia because of increased O2 demand by the heart
MagnesiumUsed for refractory VF or VT caused by hypomagnesemia and Torsades de Pointes
Dose:1-2 grams over 2 minutes
Side EffectsHypotensionAsystole!
AtropineIndications:Symptomatic sinus bradycardiaSecond Degree Heart Block Mobitz I Organophosphate poisoning
IV Dose:.5 1 mg every 3-5 minutesMax dose is 3 mgCan be given down ET tube
Side Effects:May worsen ischemia
AdenosineIndication: PSVT
IV Dose:6 mg bolus followed by 12 mg in 1-2 minutes if neededFAST PUSH!!!!MUST FLUSH W/ 10 CC NS IMMEDIATELY
Side Effects:FlushingDyspneaChest PainSinus BradyPVCs
AmiodaroneIndications:TACHYCARDIA
IV Dose:300 mg in 20-30 ml of N/S or D5WSupplemental dose of 150 mg in 20-30 ml of N/S or D5W
Contraindications:Cardiogenic shock, profound Sinus Bradycardia, and 2nd and 3rd degree blocks that do not have a pacemaker
LidocaineIndications: PVCs, VT, VTCan be toxic so no longer given prophylactically
IV dose :1-1.5 mg/kg bolus then continuous infusion of 2-4 mg/minCan be given down ET tube
Signs of toxicity: slurred speech, seizures, altered consciousness
SCENARIOA 62 year old female is admitted to the ER with chest pain, dyspnea, and moist, gurgling crackles. She appears in acute distress and is cyanotic. Vital signs are: P =110, R = 20, BP = 80/40.
Cardiac monitoring is initiated and the following EKG is observed:
What is the patients arrhythmia and probable medical problem?What therapies should be done? Explain each one.
The EKG began to show:
What is occurring in the heart to cause this arrhythmia?How is this treated?What other arrhythmias may occur now?
The patient suddenly becomes lifeless and the EKG shows:
Uh oh! What now?
38
The treatment(s) are unsuccessful and the following EKG appears:
What should be done now and why?
Finally, the following EKG is obtained. However, BP is 40/0
What needs to be done now?