3minute Blood Film Evaluations
-
Upload
santhi-swetha -
Category
Documents
-
view
215 -
download
0
Transcript of 3minute Blood Film Evaluations
-
8/3/2019 3minute Blood Film Evaluations
1/16
1
www.vetmedpub.com DECEMBER 200Clinical Solutions for Companion-Animal Practitioners
Idea Exchange Mind Over Miller 2004 Annual Index
EVALUATBLOOD FIL
Take 3 minutes to brinabnormalities to ligh
EVALUATBLOOD FIL
Take 3 minutes to brinabnormalities to ligh
-
8/3/2019 3minute Blood Film Evaluations
2/16
2
Many veterinarians and technicians do not routinely evaluate blood films microscopi-cally, largely because they lack confidence in either preparing a well-made blood
film or in being able to accurately identify important abnormalities. But blood filmsshould be evaluated whenever a complete blood count (CBC) is requested, regardless of whether the CBCis done in the clinic or at a reference laboratory. Blood film evaluation is asessential to a CBCas a microscopic examination of urine sediment is to a complete urinalysisor two views are to proper radiographic interpretation. No single hematology procedure pro-duces more valuable information yet requires so little additional time (we recommend threeminutes) and expense.
Even the most expensive hematology analyzers are not designed to eliminate peripheralblood film evaluation. Morphologic features that instruments cannot identify include left shifts(increased immature neutrophils), neutrophil toxicity, lymphocyte reactivity, white blood cell( WBC) malignancy, red blood cell (RBC) poikilocytosis,RBCinclusions, and platelet abnormali-ties. A quick blood film review will help validate certain numerical data including plateletcounts, WBCcounts, WBCdifferentials, andRBCdensity, since even reference laboratory analyz-
ers prove inaccurate with some of the more abnormal samples.In this symposium, we suggest using a systematic method for evaluating blood films. Thismethodwhich requires veterinarians and technicians to answer basic questions aboutRBC,
WBC, and platelet numbers and morphologymaximizes hematologic information. And wecover the most common and important morphologic findings in the peripheral blood.
We hope this symposium will provide veterinary practitioners and technicians with theskills to properly prepare, stain, and evaluate a peripheral blood film and will encouragethem to use this vital hematology tool in their practices.
Dr. Fred L. Metzger Jr.
P E E R - R E V I E W E D
Symposium on a three-minuteperipheral blood film evaluatio
M Y R I A M
K I R K M A N
- O H
, K O
S T U D I O S
3
8
14
Page 8
Page 3
Three-minute peripheral blood film evaluation: Preparing the filmFred L. Metzger Jr. and Alan RebarNo single hematology procedure produces more valuable information yet requi
time and expense than a peripheral blood film. Proper preparation and staining are critical.
Three-minute peripheral blood film evaluation: The erythron and thrombFred L. Metzger Jr. and Alan RebarWhen examining the red blood cells and platelets in a blood film, ask yourself questions to quickly identify and further characterize conditions such as anemithrombocytopenia.
Three-minute peripheral blood film evaluation: The leukonFred L. Metzger Jr. and Alan RebarTaking a moment to briefly examine white blood cells will help you identify coas inflammation or stress that may indicate serious disease.
All articles have been reviewed by at least two board-certified specialists or recognized experts to ensure accuracy, thoroughness,
Symposium on a three-minuteperipheral blood film evaluation
-
8/3/2019 3minute Blood Film Evaluations
3/16
3
P E E R - R E V I E W E D
Three-minute peripheral blood film evaluatioPreparing the filmNo single hematology procedure produces more valuable information yet requires so little time anperipheral blood film evaluation. Proper preparation and staining of the film are critical.
A PERIPHERAL BLOOD FILMevaluation should bepart of all complete blood counts (CBCs), re-gardless of whether hematology is performedin-house or at a reference laboratory. Propersample collection, slide preparation, andstaining are essential to accurately evaluate ablood film, as is the correct use of a high-quality microscope. This article describes thesteps in preparing a blood film and theequipment youll need.
Important components of aCBCinclude evalu-ating the erythron (hematocrit, total red bloodcell [RBC] count, hemoglobin concentration,
absolute reticulocyte count, andRBC
indices),the leukon (total white blood cell [ WBC] count,five-part differential count including immatureneutrophils), the thrombon (platelet countand platelet indices), and the total proteinconcentration. As mentioned earlier, alwaysinclude a peripheral blood film evaluation inthe CBC.
A CBCshould be included in evaluations of every sick patient, every patient with vaguesigns of disease, and every patient receivinglong-term medications. In addition, aCBCshould be performed as part of every preanes-
thetic workup, for adult wellness and geriatricprofiles, and as a recheck test for patients in which RBC, WBC, or platelet abnormalities werepreviously diagnosed.
Artifacts must be avoided for proper hemato-logic interpretation. Causes of artifacts includepoor blood collection techniques, inadequatesample volumes, prolonged sample storage,and delayed sample analysis.
Proper blood collection is vital to prevent er-
roneous results from sample clotting and celllar lysis. Obtain hematology samples from tlargest blood vessel possible to minimize celllar trauma and to prevent the activation of cloting mechanisms. For accurate results, discaclotted samples and collect fresh samples. Common venipuncture sites in dogs and cats include the jugular, cephalic, and lateral and mdial saphenous veins. Anticoagulants incluEDTA, heparin, and citrate. EDTA is the preferredanticoagulant for blood film preparation bcause it preserves cellular detail better thaother anticoagulants do and does not interfer
with Romanowsky staining of WBCs.Inadequate sample volume is a commo
cause of inaccurate hematologic results. Proerly fill anticoagulated blood collection tubesavoid falsely decreased hematocrits and cecounts and to prevent RBCshrinkage.
Hematologic samples must be analyzed soon as possible to prevent artifacts created bexposure to anticoagulants and cell deteriortion due to storage and shipment. Analyze samples within three hours or refrigerate them 39.2 F (4 C) to avoid an artificially increashematocrit, increased mean corpuscular voume, and decreased mean corpuscular hemoglobin concentration.1 Prepare blood film
within one hour of collection to avoid morphologic artifacts. R BC crenation, neutrophil hypersegmentation, lymphocytic nuclear distortioand general WBC degeneration including vacuolization in neutrophils may occur in agesamples. In addition, monocyte vacuolizatiomonocyte cytoplasmic pseudopod formatioand platelet agglutination can be encounterein stored samples.2 If you use a reference laboratory for primary hematologic analyses, wrecommend submitting freshly prepared bloofilms along with the anticoagulated blood.
Collecting a sample for the blood film
Components of and indications for aCBC
Fred L. Metzger Jr.,DVM, DABVP(canine and feline practice)
Metzger Animal Hospital1044 Benner PikeState College, PA 16801
Alan Rebar,DVM, PhD, DACVPDepartment of Veterinary PathobiologySchool of Veterinary MedicinePurdue UniversityWest Lafayette, IN 47907
-
8/3/2019 3minute Blood Film Evaluations
4/16
4
Producing high-quality blood films begins by using clean, new slides. Used slides fre-quently have imperfections such as scratchesand other physical defects. Slides must befree of fingerprints, dust, alcohol, detergents,and debris. Using a microhematocrit tube,
place a small drop (2 to 3 mm in diameter)of well-mixedEDTAblood about 1 to 1.5 cmfrom the end of the slide. Next, draw aspreader slide back into the blood drop atabout a 30-degree angle until the spreaderslide edge contacts the sample drop and cap-illary action disperses the sample along theedge. Then, using a smooth steady motion,push the spreader slide away from the blooddrop, creating a uniform film that coversnearly the entire length of the slide ( Figure 1). Changing the angle of the spreader slide
will change the length and thickness of theblood film. For blood samples with lowhematocrits (severe anemia), you may needto decrease the angle of the spreader slide tomake a good-quality slide. In contrast, forsamples with high hematocrits (severe dehy-dration and polycythemia due to a variety of conditions), you may need to increase theangle of the spreader slide.
Drying is an important step in the produc-tion of good-quality blood films. Allow theblood film to thoroughly air-dry before apply-ing stain, or use a heat block (at the low set-ting) or a hair dryer to hasten the drying time,thus minimizing refractile markings that candistort erythrocyte morphology. In addition,keep formalin and formalin-containing con-
tainers away from all blood and cytology smears to prevent staining artifacts such as in-creased cytoplasmic granularity and ba-sophilia.
Most veterinary practices use a modified Wrights stain (Romanowsky stain) for bothhematology and cytology. Modified Wrightsstains are available as either three- or two-so-lution kits. We prefer kits with three separatesolutions: an alcohol fixative, an eosinophilic
staining solution, and a dark-blue stainingsolution. Veterinary practices should havetwo separate Coplin stain jar setsone forhematology and cytology samples and onefor contaminated samples such as those col-lected for ear and fecal cytology. For opti-mal results, replace staining solutions regu-larly.
Recommended blood staining protocolincludes dipping the air-dried slide five to10 times in each solution while blotting oneedge briefly in between each solution. Rinse
the slide with distilled water after the finstaining step, and allow the blood film to adry before examination. Good staining tecnique is critical to identifying polychrmatophils on a peripheral blood film. If thstaining is done improperly, many of thquick Romanowsky-type stains will not githe needed tinctorial differences between mture RBCs (orange-red) and polychromatophi(bluish-pink). Typically, poor staining withe various quick stains results in allRBCs having a bluish or muddy tint.
The microscope
A high-quality microscope is essential hematology. We recommend a binocular mcroscope with a minimum of 10 , 20 , and100 (oil-immersion) objectives and widfield 10 oculars. When evaluating the slidmake sure maximum light reaches the bloofilm. This means positioning the substage codenser as close as possible to the stage witthe iris wide open. The light source should bequipped with a variable rheostat to allomaximal control of light intensity. To ensuoptimal focused light for the microscopic evuation, the microscope should be in Khler
Evaluating the blood film
Staining the blood film
1.The steps in preparing a blood film. A small dropof blood is placed near the end of a slide ( top ). Aspreader slide is drawn back into the blood dropat a 30-degree angle ( middle ). Then the spreaderslide is pushed away from the blood drop,creating a uniform film across the slide ( bottom ).
F I G U R E 1
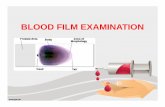
Monolayer
Feathered edge Body of blood film
Application point
LabelMonolayer
F I G U R E
Good staining technique is critical to identifying polychromatophilson a peripheral blood film.
2.The components of the peripheral blood film
-
8/3/2019 3minute Blood Film Evaluations
5/16
5
lumination. Contact your microscope vendor,or review the microscope manual to ensureproper illumination.
The three zones A good-quality blood film has three
zones: the body (near the point of blood ap-plication), the monolayer (the zone betweenthe body and feathered edge), and the feath-ered edge (the area most distant from thepoint of application) ( Figure 2 ). The defini-tion of the monolayer varies from institutionto institution, but the definition used to en-sure consistent semiquantification of variousmorphologic abnormalities is the area whereabout half of the RBCs are touching one an-
other without overlapping. The monolayer isthe area of the blood film where WBCs andplatelet numbers are estimated and cell mor-phology is examined. Although the mono-layer is the only zone where morphologicevaluation of individual cells is performed atoil-immersion magnification, systematicblood film evaluation includes assessing of all three zones.
First, examine the blood film at low mag-nification (10 or 20 ), and scan the entireslide to evaluate overall film thickness, celldistribution, and differentiation of the three
different zones. Evaluate the feathered edge( Figure 3) for microfilariae, phagocytized or-ganisms, atypical cells, and platelet clumping.Next, examine the body of the blood film( Figure 4 ) for rouleau formation orRBCagglu-tination. Then, still using low magnification,evaluate the monolayer ( Figure 5 ), estimatethe total WBCcount ( see the third article in this
symposium), and predict the expected WBCdifferential count. Finally, use the oil-immer-sion objective (100 ) to examine RBC, WBC,and platelet morphology in the monolayer.
EvaluateRBCs for evidence of anisocytosis,poikilocytosis, polychromasia, hemoglobinconcentration, and RBC parasites. ImportantRBCmorphologic abnormalities include sphe-rocytes, schistocytes, acanthocytes, and lepto-cytes ( see the second article in this
symposium).Evaluate neutrophils for toxicity and the
presence or absence of a left shift (increasednumbers of band neutrophils). Evaluate lym-phocytes for reactivity and monocytes forphagocytized organisms ( see the third article in this symposium).
With relatively little practice, you canidentify most important morphologic abnor-malities in theRBCs, WBCs, and platelets with
the 20 objective field of view; these can bequickly validated with the 100 oil-immer-sion view.
Examining a properly prepared peripheralblood film offers invaluable informationabout cellular morphologic changes not pro-
vided by automated instruments and pro- vides a quality assurance confirmation of CBCdata generated by in-clinic or reference labo-ratory hematology analyzers. We recommend
taking about three minutes to view the bloodfilm and, using the questions discussed in thenext two articles of this symposium, to sys-tematically evaluate theRBC, platelet, and WBCcomponents of the peripheral blood film.
ACKNOWLEDGMENTThe authors gratefully acknowledge the technicalassistance and images provided by Dennis DeNi-cola, DVM, PhD, DACVP.
REFERENCES1. Willard, M. et al .: The complete blood countand bone marrow examination. Textbook of Small Animal Clinical Diagnosis by Laboratory
Methods , 3rd Ed. W.B. Saunders, Philadelphia,Pa., 1999; pp 11-30.2. Rebar, A.; Metzger, F.: The Veterinary CE Advi-sor: Interpreting Hemograms in Cats and Dogs.Vet. Med. (suppl.) 96 (12):1-12; 2001.
Summary
F I G U R E 3 F I G U R E 4 F I G U R E 5
P a t
i e n t
I D
P a t
i e n t
I D
P a t
i e n t
I D
3.Look for platelet clumps, microfilariae, andin the feathered edge of the film ( purple section ).
4.Look for rouleau formation and RBC aggluthe body of the film ( purple section ).
5.Estimate platelet and WBC counts and examorphology in the monolayer zone ( purple section ).
-
8/3/2019 3minute Blood Film Evaluations
6/16
-
8/3/2019 3minute Blood Film Evaluations
7/16
-
8/3/2019 3minute Blood Film Evaluations
8/16
8
P E E R - R E V I E W E D
E VALUATING A PERIPHERALblood film validates cellcounts performed by hematology analyzers,plus it offers valuable diagnostic information re-layed by erythrocytes, platelets, and leukocytes.The first article in this symposium describedhow to prepare a peripheral blood film. In thisarticle, we discuss important red blood cell(RBC) and platelet number and morphologicchanges. And in the next article, we discuss
white blood cell ( WBC) alterations.If a patientsRBCmass is reduced, then the
patient is anemic. Once anemia is recognized,the next concern is bone marrow responsive-
ness: Is the anemia regenerative or nonre-generative? If theRBCbone marrow pre-
cursor cells respond with increasedproduction of appropriate magnitude,the anemia is regenerative (responsive). If
RBC production is not effectively increased,the anemia is nonregenerative (nonrespon-sive). Keep in mind that a lag of 48 to 72
hours exists before bone marrow responsive-ness is perceived in the peripheral blood, sobe careful in defining nonresponsiveness.
Evaluating the thrombon by first assessingplatelet numbers is another important part of every complete blood count (CBC). Thrombocy-topenia is more common than thrombocytosis
and can be of great clinical importance. Plateletcounts below 40,000/l can lead to spontaneousbleeding. Platelet clumping, which can be seenin any species but is particularly problematic incats, can give a falsely low platelet count.Platelet clumping frequently interferes with re-sults from impedance cell counters because ag-gregated platelets may be included in theRBCor
WBC counts, resulting in artifactually decreasedplatelet counts.1
Our approach to peripheral blood film eval-uation uses a question-based format. This sys-
tematic approach allows veterinary practitionand technicians to maximize important visuinformation.
Is there evidence of RBCregeneration? (Ipolychromasiaor reticulocytosis present?)In dogs and cats, polychromasia is the princ
pal feature of RBCregeneration on a blood filmprepared with Wrights or modified Wrighstain. Polychromatophils are immatureRBCs thastain bluish because they containRNA( Figure 1)
Polychromatophils on blood smears prepare with Wrights or modified Wrights stain rougcorrespond to reticulocytes on smears prepare
with new methylene blue stain. If regenerationstill questionable after youve evaluated Wrighstained blood films, perform a reticulocyte cou
with new methylene blue stain. When performing reticulocyte counts in ca
it is important to count aggregate reticulocyt(cells containing diffuse accumulations of retilum) since they represent recentRBCproduction
Evaluating theRBCs
Fred L. Metzger Jr.,DVM, DABVP(canine and feline practice)
Metzger Animal Hospital1044 Benner PikeState College, PA 16801
Alan Rebar,DVM, PhD, DACVPDepartment of Veterinary PathobiologySchool of Veterinary MedicinePurdue UniversityWest Lafayette, IN 47907
Three-minute peripheral blood film evaluationThe erythron and thrombonWhen examining the red blood cells and platelets in a blood film, ask yourself these questionsto quickly identify and further characterize conditions such as anemia and thrombocytopenia.
F I G U R E 1
1.Polychromatophils ( arrows ) in a dog (modifiedWrights stain; 100 ).
-
8/3/2019 3minute Blood Film Evaluations
9/169
in response to relatively severe anemia ( Fig-ure 2 ). In cats, aggregate reticulocytes matureinto punctuate reticulocytes within 12 hours,and punctuate reticulocytes mature intoRBCsin about 10 days. Consequently, elevatedpunctuate reticulocytes representRBCregener-ation two weeks earlier, whereas aggregatereticulocytes indicate recent regeneration.2 Indogs and cats, peak reticulocyte counts occurfour to eight days after the onset of anemia.
As a general guideline, a reticulocyte countabove 60,000/l in cats (aggregate only) and80,000/l in dogs indicates a regenerative ane-mia.3 Dogs with regenerative anemias havereticulocyte counts that are frequently 100,000to 300,000/l (dogs with extremely regenera-tive anemia can have counts of 500,000/l orgreater), while cats typically demonstrate aless dramatic response when only the aggre-
gate reticulocyte counts are evaluated.Reference laboratories can provide reticu-
locyte counts, and in some cases, they willautomatically add the reticulocyte count tothe CBC at an additional charge if anemia isidentified. The newer in-clinic, laser-basedhematology analyzers automatically provideabsolute reticulocyte counts with eachCBC.4
Regenerative anemias can be further classi-fied as either blood loss or hemolytic (de-creased RBClifespan) anemias. Whenever yoususpect hemolysis, closely examineRBCmor-phology to detect spherocytes, acanthocytes,schistocytes,RBCinclusions, and parasites ( see below ). Figure 3 is a flow chart for classifyinganemias in dogs and cats.
Are nucleatedRBCs present?Nucleated RBCs, or metarubricytes ( Figure
4 ), are not found in any appreciable numbers
in mammalian peripheral blood samples. Moclinicians consider fewer than 4 nucleatRBCs/100 WBCs to be insignificant when th
WBC count is within the reference range. Ncleated RBCs may be seen in increased numbers with strongly regenerative anemias, bthey should always be less numerous than thpolychromatophils or reticulocytes. This fining has been identified as an appropriate nucleated RBCresponse by some clinicians.
An inappropriate nucleatedRBC responseoccurs when more than 5 nucleatedRBCs/100
WBCs are present in the absence of polychromasia. Conditions associated with an inapprpriate nucleated RBC response include bonmarrow stromal damage, extramedullahematopoiesis, fractures, hyperadrenocorticisfeline leukemia virus infection, chemtherapeutic drug administration, and lead tox
F I G U R E 3
Classifying Anemiasin Dogs and Cats
Blood loss anemia is apossible cause. Look forexternal or internal hem-orrhage orparasites ( e.g. fleas,hookworms). Keep inmind that it takes oneto three days to see thehematocrit decrease.
Hemolytic anemia is apossible cause. Considerimmune-mediatedhemolytic anemia withspherocytosis or Heinzbody hemolytic anemia( e.g. onion ingestion,acetaminophenadministration).
If bone marrow hypopla-sia is present, consideranemia of inflammation,anemia of chronic renaldisease, myelophthisisdue to bone marrow dis-ease, or chemotherapytoxicosis.
If bone marrow hyper-plasia with ineffectiveerythropoiesis is present,consider a nuclear matu-ration defect (FeLV infec-tion, drug toxicosis) or acytoplasmic maturationdefect (lead toxicosis,iron deficiency includingchronic blood loss).
When a patient has a decreased hematocrit, consider itshydration status and perform a reticulocyte count.
The anemia is regenerative if the reticulocyte count is morethan 80,000/l in dogs and more than 60,000/l in cats.
The anemia is nonregenerative if the reticulocyte count is less than80,000/l in dogs and less than 60,000/l in cats. In these cases,perform a serum chemistry profile, urinalysis, and other neededdiagnostic tests to rule out underlying diseases. If no such disease isfound, perform a bone marrow evaluation.
F I G U R E 2
2.Aggregate ( black arrows ) and punctuate ( red arrows )reticulocytes in a cat. Note that aggregatereticulocytes contain greater than or equal to fivebasophilic specks (new methylene blue stain; 100 ).
4.A nucleated RBC ( arrow ) in a dog (modified Wrightsstain; 100 ).
F I G U R E 4
-
8/3/2019 3minute Blood Film Evaluations
10/16
10
cosis, among others.5 Splenic dysfunction (e.g.decreased clearance of circulating nucleatedRBCs) is an important cause of an inappropri-ate release of nucleatedRBCs and may occur inpatients in which the spleen has been re-moved and in patients with splenic neo-plasms, especially hemangiosarcoma.
Is autoagglutination present? Agglutination is unorganized three-
dimensional clumping of RBCs that must bedifferentiated from rouleau formation. It iscommon in dogs with immune-mediated he-molytic anemia. When confirmed, autoagglu-tination suggests an immune-mediatedprocess such as autoimmune-mediated he-molytic anemia or drug-induced hemolyticanemia (e.g. cephalosporins, penicillin) be-cause RBCsurface antibodies cause cell cross-linking and the resulting agglutination.
Rouleau formation is organized linear ar-rays of RBCs caused by decreased zeta poten-tials from plasma proteins (e.g. globular pro-teins, fibrinogen) coatingRBCs. This distinctiveformation is commonly described as stacks of
coins. Unlike agglutination, which is a strongcross-linking between cells, rouleau is a resultof a weak binding between cells because of dissimilar ionic charges on theRBC surface.
Rouleau formation is a common finding whenfibrinogenesis is increased and must be differ-entiated from agglutination. On routine
Wrights-stained or modified-Wrights-stainedblood films, marked rouleau formation andagglutination may be difficult to differentiate.
Whenever you suspect agglutination on ablood film, mix a drop of the well-mixedEDTAanticoagulated blood on a new glass slide
with two or more drops of isotonic saline so-lution. Add a cover slip, and view the mixtureas an unstained wet preparation. Under theseconditions, most rouleaux formations dissipatebut autoagglutination typically persists and isrecognized as clumpedRBCs ( Figure 5 ).
Are poikilocytes present?Normal canineRBCs are shaped like bicon-
cave disks with prominent central pallor. Fe-line RBCs have much less apparent central pal-lor. Abnormally shapedRBCs are called
poikilocytes and include artifactual changes(crenation) as well as true abnormalities (e.g.spherocytes, acanthocytes, schistocytes, lepto-cytes).
Crenation ( Figure 6
) can be confused with importantRBCchanges such as acantho-cytosis. Crenation is a shrinking artifact mostcommonly seen when less than optimal
amounts of blood are collected into theEDTtube and the peripheral blood film is nomade relatively quickly after the anticoagution process.4 Some less common causes ocrenation include electrolyte disturbanceuremia, and rattlesnake envenomation. useful differentiating feature for identifycrenation is that crenation typically affelarge numbers of cells in a particular area the slide, whereas true poikilocytosis typcally affects relatively lower numbers of cethroughout the peripheral blood film. Crention can be minimized by preparing bloofilms immediately after blood samples acollected and properly anticoagulated.
Spherocytes are sphericalRBCs that havelost their normal biconcave shape, resulting more intense staining than normalRBCs. Theyhave no central zone of pallor, and they appear smaller than normalRBCs ( Figure 7 )More than four to six spherocytes per 100field is considered elevated. Spherocytes acommonly seen with many of the immunmediated hemolytic anemias we encounter
veterinary medicine. Be careful when attem
ing to identify spherocytes in felineRBC
s because felineRBCs are much less biconcave thacanine RBCs and, therefore, have much lescentral pallor.
F I G U R E 5
5.A saline wet preparation of canine blood shautoagglutination (20 ).
6.Crenation in a dog (modified Wrights stai ).7.Spherocytes ( black arrows ) and a polychromatoph red
arrow ) in a dog (modified Wrights stain; 10 ).8.Acanthocytes ( arrow ) in a dog (modified Wrigh
100 ).9.Schistocytes ( arrows ) in a dog (modified Wright
100 ).
F I G U R E 6 F I G U R E 7
F I G U R E 8 F I G U RE 9
-
8/3/2019 3minute Blood Film Evaluations
11/16
11
Acanthocytes are abnormally shapedRBCshaving two to 10 blunt, fingerlike surface pro-jections of varying sizes ( Figure 8 ). Thesemorphologic changes are related to abnormalaccumulation of lipids within theRBC mem-brane when there is an abnormal plasmacholesterol:phospholipid ratio. Acanthocytesare seen occasionally in normal animals. Con-ditions most commonly associated with acan-thocyte formation include underlying meta-bolic diseases or diseases affecting normallipid metabolism. Nonneoplastic and neoplas-tic (hemangiosarcoma in particular) diseasesinvolving the liver, spleen, and kidney may have associated acanthocytosis in dogs and,occasionally, in cats.6 Acanthocytosis is mostfrequently associated with liver disease andsplenic hemangiosarcoma.
Schistocytes areRBCfragments formed by mechanical injury ( Figure 9 ). Even in very low numbers (one schistocyte in every threeto five 100 objective fields), schistocytes areclinically relevant. Finding even a few schisto-cytes may help you identify underlying orsubclinical disseminated intravascular coagu-
lation (DIC
). Microvascular mechanical frag-mentation of RBCs associated with diseasessuch as hemangiosarcoma and dirofilariasismay also result in schistocyte formation.7
A leptocyte (codocyte, target cell) is anRBC with excess cell membrane that forms ashape often referred to as having a Mexicanhat appearance ( Figure 10 ). Leptocytes areseen occasionally in normal animals. In-creased numbers of leptocytes (> 3/100oil-immersion field) are expected with poly-chromasia because polychromatophils haveexcess membranes compared with normal
RBCs. Consequently, leptocytosis is common when reticulocytosis is present, so most ref-erence laboratories do not report this mor-phologic finding. However, laboratories willreport leptocytes when they are seen in theabsence of polychromasia since the excesslipid membrane compared with cytoplasmic
volume is an abnormality. The two primary mechanisms causing this abnormal morphol-ogy are either an upset in thecholesterol:phospholipid ratio in plasma re-sulting in lipid loading (as might be seen
with liver disease and other metabolic disor-ders) or a decrease in cytoplasmic contentcompared with normal (as might be seen
with iron deficiency typically due tochronic blood loss).8 With iron deficiency,RBC hemoglobin content decreases, and inaddition to the leptocytosis, hypochromasiais often observed.
AreRBCinclusions present? Accurately characterizing various inclu-
sions is an important aspect of blood filmevaluation. Inclusions may include Heinzbodies, basophilic stippling, Howell-Jolly bodies, and certain infectious agents.
Heinz bodies are localized accumulationsof denatured, oxidized, and precipitated he-moglobin in the RBC. They often affix to theinner RBC membrane and project from theRBC surface. Conditions associated withHeinz body hemolytic anemia include aceta-minophen toxicosis in cats and acute onionand zinc toxicosis in dogs. Diabetes mellitus,hyperthyroidism, and lymphosarcoma in catsand the use of oral benzocaine sprays are
also associated with increased numbers of Heinz bodies; but anemia is not present inthese cases.8 The Heinz bodies observed incats may be small or not project from the cellsurface, making their identification difficult( Figure 11). New methylene blue staining
will help confirm the presence of Heinzbodies; the Heinz bodies stain dark bluecompared with the rest of the erythrocyte( Figure 12 ). In contrast to Heinz bodies indogs, Heinz bodies can be an incidentalfinding in cats, and their relevance must bedetermined by evaluating clinical signs and
other hemogram parameters.Basophilic stippling is seen inRomanowsky-stained films as small, dark-bluepunctate aggregates of residual ribosomes inRBCs ( Figure 13). It has traditionally been as-sociated with lead toxicosis in dogs but may also be associated with highly regenerativeanemias in any species. Further diagnostic in-
vestigation is important when basophilic stip-pling is seen in the absence of reticulocytosis.
Howell-Jolly bodies are small nuclearremnants that may be increased with acceler-
F I G U R E 1 0
F I G U RE 1 2
F I G U RE 1 3
F I G U R E 11
10.Leptocytes ( arrow ) in a dog (modified Wrights 100 ).
11.Heinz bodies, which are noselike RBC proj( arrows ) in a cat (modified Wrights stain; 100 ).
12.A blood film from a cat showing Heinz bodeasier to see with new methylene blue stain ).
13.Basophilic stippling ( black arrow ) and apolychromatophil ( red arrow ) in a dog (modifiedWrights stain; 100 ).
-
8/3/2019 3minute Blood Film Evaluations
12/16
12
ated RBCregeneration. In healthy animals, thelow numbers of RBCs with Howell-Jolly bodiesreleased from the bone marrow are quickly removed from circulation primarily throughthe action of fixed tissue macrophages in thespleen. If Howell-Jolly bodies are easily iden-tified and no reticulocytosis is noted, investi-gate underlying splenic disease. This inclu-sion can be an incidental finding in catsbecause of the open splenic architecture anddecreased erythrophagocytic properties inher-ent to the feline spleen.
Infectious agents including Babesia ( Fig-ure 14 ), Cytauxzoon , and Mycoplasma (previ-ously known as Haemobartonella ) speciesmay be identified inRBCs. Evaluation for My-coplasma species ( Figure 15 ) should be per-formed on freshly collected blood samplesthat have not been refrigerated to improveidentification.
Are platelet numbers normal,decreased, or increased?
Microscopic validation of platelet counts isan important component of blood film evalu-ation. Platelet clumping ( Figure 16 ) inter-feres with accurate enumeration of platelets
with all hematology analyzers and with man-ual counting methods. Clumping occurs inmany samples because of platelet activationduring the collection process. Increasednumbers of large platelets may also result ininaccurate platelet counts when impedance
counting methods are used.On a well-prepared peripheral blood film
in which no marked platelet clumping at thefeathered edge is present, the average num-ber of platelets observed per 100 oil-immersion monolayer field multiplied by 20,000 provides a good estimate of the num-ber of platelets/l. As a general rule, youshould see a minimum of eight to 10 plateletsand a maximum of 35 to 40 platelets per100 oil-immersion monolayer field of
view.9
If the platelet numbers are decreased,can the mechanismbe determined?Thrombocytopenias occur through four
basic mechanisms: sequestration, utilization(consumption), destruction, and decreased orineffective production. While clues as to theunderlying mechanism are found in theCBC,in most cases, bone marrow evaluation isneeded for complete interpretation.
Sequestration thrombocytopenias are un-common in veterinary medicine. They are
usually the result of hypersplenism and,thus, are characterized by an enlargedspleen on physical or radiographic examina-tion.
Utilization, or consumption, thrombocy-topenias are caused by excessive activation of the coagulation cascade. These thrombocy-topenias are associated with inflammatory dis-ease and DIC. Utilization thrombocytopeniasare usually moderate, with platelet numbers
in the 75,000 to 150,000/l range, but valubelow 40,000/l accompanied by petechiare possible.10 Bone marrow evaluation re
veals normal to increased numbers megakaryocytes.
Destruction thrombocytopenias are immune-mediated thrombocytopenias in whicnormal circulating platelets are destroyed circulating antiplatelet antibodies. Destructthrombocytopenias are often extreme, with pripheral platelet counts well below 50,000/Bone marrow examination is characterized normal to increased numbers of megakarocytes.
Decreased or ineffective production is assciated with extremely low platelet countcounts well below 50,000/l are commoBone marrow evaluation will vary greatly most of these cases, although they will shasimilar end results of deceased effective prduction by the bone marrow. With decreaseproduction thrombocytopenias, no identifiabto extremely low numbers of megakaryocytare present. With ineffective production, mobone marrow samples have normal to in
creased numbers of megakaryocytes, and thproduction of platelets is ineffective in macases because of an immune-mediated dstructive process directed at an early stage platelet development or at the megakaryocypopulation itself.
Evaluating the platelets
F I G U RE 1 6
16.A blood film from a cat showing clumped( arrow ) (modified Wrights stain; 20 ).
14.Babesia canis( arrow ) in a dog (modified Wrightsstain; 100 ).
F I G U RE 1 5
15.Mycoplasma haemocanis( arrow ) in a dog (modifiedWrights stain; 100 ).
F I G U R E 1 4
-
8/3/2019 3minute Blood Film Evaluations
13/16
13
If platelet numbers are increased,is the thrombocytosis reactiveor neoplastic?Most thrombocytosis is reactive or neo-
plastic. Reactive thrombocytosis can occursecondary to exercise, hemorrhage,splenectomy, excitement, fractures, high cir-culating glucocorticoid concentrations,myelofibrosis, and iron deficiency anemiaas well as 24 hours or more after bloodloss.11 When the possible causes of reac-tive thrombocytosis have been ruled out,then the possibility of primary plateletleukemia must be considered. When ex-tremely high platelet counts are seen (>1,000,000/l), thrombocytosis due to neo-plasia must be strongly considered.
Are enlarged platelets present?The presence of enlarged platelets ( Figure
17 ), which correlates with increased meanplatelet volume (MPV ), is supportive of an in-creased rate of thrombopoiesis in the bonemarrow in response to a peripheral demand.This interpretation can be used with most
species; however, in cats, enlarged platelets isan equivocal finding.
Determining if an anemia is regenerative ornonregenerative is critical when developing alist of differential diagnoses. In addition, auto-mated platelet counts should be verified by examining blood films because plateletclumping is common, especially in cats,
which results in artifactually decreasedplatelet counts.
ACKNOWLEDGMENTThe authors gratefully acknowledge the technical
assistance and images provided by Dennis DeNi-cola, DVM, PhD, DACVP.
REFERENCES1. Rebar A.H. et al .: Laboratory methods in
hematology. A Guide to Hematology in Dogs and Cats . Teton New Media, Jackson, Wyo., 2002; pp3-36.
2. Duncan, J. et al .: Erythrocytes. Veterinary Laboratory Medicine , 3rd Ed. Iowa State Univer-sity Press, Ames, 1994; pp 3-61.
3. Feldman, B.F. et al .: Reticulocyte response.Schalms Veterinary Hematology , 5th Ed. Lippin-cott Williams & Wilkins, Baltimore, Md., 2000; pp110-116.
4. Rebar A.H. et al .: Erythrocytes. A Guide to Hematology in Dogs and Cats . Teton New Media, Jackson, Wyo., 2002; pp 30-68.
5. Rebar, A.; Metzger, F.: The Veterinary CE Advi-sor: Interpreting Hemograms in Cats and Dogs.Vet. Med. (suppl.) 96 (12):1-12; 2001.6. Feldman, B.F. et al .: Classification and labora-tory evaluation of anemia. Schalms Veterinary
Hematology , 5th Ed. Lippincott Williams & Wilkins, Baltimore, Md., 2000; pp 140-150.7. Rebar A.H. et al .: Platelets. A Guide to Hema-tology in Dogs and Cats . Teton New Media,
Jackson, Wyo., 2002; pp 113-134.8. Thrall, M.A.: Erythrocyte morphology. Veteri-nary Hematology and Clinical Chemistry . Lip-pincott Williams & Wilkins, Philadelphia, Pa.,2004; pp 69-82.9. Duncan, J. et al .: Erythrocytes, leukocytes,hemostasis. Veterinary Laboratory Medicine , 3rdEd. Iowa State University Press, Ames, 1994; pp75-93.10. Harvey, J.W.: Platelets. Atlas of Veterinary
Hematology: Blood and Bone Marrow of Domes-tic Animals . W.B. Saunders, Philadelphia, Pa.,2001; pp 75-80.11. Feldman, B.F. et al .: Acquired platelet dys-function. Schalms Veterinary Hematology , 5th
Ed, Lippincott Williams & Wilkins, Baltimore,Md., 2000; pp 496-500.
Conclusion
F I G U RE 1 7
17.A blood film from a dog with immune-mediatedhemolytic anemia. Note the enlarged platelets ( blackarrows ). Also note the polychromasia, spherocytosis, andHowell-Jolly body ( red arrow ) (modified Wrights stain;100 ).
-
8/3/2019 3minute Blood Film Evaluations
14/16
14
P E E R - R E V I E W E D
Three-minute peripheral blood film evaluatiThe leukonTaking a moment to briefly examine white blood cells will help you identify conditionssuch as inflammation or stress that may indicate serious disease.
IN THE PREVIOUS ARTICLE, we discussed how toexamine the erythron and thrombon compo-nents of peripheral blood films. In this arti-cle, we again use a question-based format toguide you in evaluating the leukon by as-sessing white blood cell ( WBC) numbers andmorphology. All five WBC cell types are as-sessed. Table 1 lists the general patterns of
WBC response under a variety of circum-stances.
Experience is required to accurately estimatecell counts directly from blood films. Subjec-tive analysis of total WBC numbers may beperformed by counting three to five 20 ob-
jective fields; 10 to 20 WBCs/20 field is con-
sidered normal indogs and cats. An-other method in-
volves counting sev-eral 100
oil-immersion monolayerfields and multiplying the av-
erage number of WBCs/100oil-immersion field by 2,000 toobtain a final estimated total
WBCcount.1
A left shift may be the only indicator of activeinflammation in veterinary patients becausetotal WBCand neutrophil counts are frequently
within the reference range. Left shifts are char-acterized by increased numbers of immature
neutrophils (e.g. band cells, metamyelocytein circulation. A left shift is a hallmark of flammation, so accurately identifying bacells is extremely valuable. No hematology aalyzer (in-house or reference laboratory instrmentation) has been documented to accurately identify band neutrophils; consequentthey must be identified microscopically. Oblood films, the nucleus of a band neutrophtypically has parallel sides ( Figure 1), whereathe nucleus of a mature neutrophil is distinctsegmented. One useful approach to differentate band neutrophils is to estimate the degreof nuclear indentation. First, identify the n
rowest and widest portions of the nucleus. the narrowest portion is less than one-third othe widest portion, the cell is classified asband cell.1
The monocyte-macrophage continuum reresents the second major branch of the ciculating phagocyte system (neutrophils athe first). Monocytes ( Figure 2 ), unlike granulocytes (neutrophils, eosinophils, bsophils), are released into the periphera
blood as immature cells and then differenate into phagocytic macrophages ( Figure 3)epithelioid macrophages, or multinucleatgiant cells.
Monocytosis can be another indicator inflammation. It may be seen in both acuand chronic conditions but may also be component of stress leukograms. Conditiofrequently associated with monocytosis iclude systemic fungal diseases (histoplasmsis, blastomycosis, cryptococcosis, coccioidomycosis, aspergillosis
Is there a monocytosis?
Is a left shift present?
Is the totalWBCcount elevated,normal, or decreased?
Fred L. Metzger Jr.,DVM, DABVP(canine and feline practice)
Metzger Animal Hospital1044 Benner PikeState College, PA 16801
Alan Rebar,DVM, PhD, DACVPDepartment of Veterinary PathobiologySchool of Veterinary MedicinePurdue UniversityWest Lafayette, IN 47907
-
8/3/2019 3minute Blood Film Evaluations
15/16
15
immune-mediated hemolytic anemia, bac-terial endocarditis, certain neoplastic dis-eases (particularly when tissue necrosis isnoted), and certain pyogranulomatous dis-eases (e.g. feline infectious peritonitis, tox-oplasmosis, foreign body reactions).2 Thebest interpretation of monocytosis in theabsence of a stress leukogram is tissue de-mand for macrophages.
Persistent eosinophilia indicates a systemichypersensitivity reaction and can be anotherindicator of inflammation. Conditions associ-ated with persistent eosinophilia includeheartworm disease in dogs and cats, felineasthma, canine atopic syndromes, felineeosinophilic granuloma complex (linearplaque form), hypereosinophilic syndrome,mast cell leukemia, and flea allergy dermatitis.3 Parasitic infections confined tothe bowel, such as whipworm infections orascarid and hookworm infections in adult
nonpregnant dogs and cats, do not cause per-sistent peripheral eosinophilia because theparasites do not have a systemic phase.4
The presence of reactive lymphocytes ( Figure 4 ) simply suggests systemic antigenic stimula-tion. This stimulation could be in response to arecent vaccination, an infectious disease, or an-other process stimulating the immune system.
The most commonly identified morphologicchange associated with lymphocyte reactivity isincreased amounts of basophilic cytoplasm.
Atypical lymphocytes ( Figure 5 ) are abnor-mal lymphocytes characterized by increasedsize with indented or cleft nuclei and largeazurophilic cytoplasmic granules. These cellsare not disease-specific and may be present
with infectious and neoplastic condition Atypical lymphocytes require additional vestigation by a clinical pathologist. Bomarrow examination and detailed cytologand possible histologic evaluation of periperal and internal lymphoid tissues may albe recommended.
Are reactive or atypicallymphocytes present?
Is a persistent eosinophilia present?
TABLE 1Common Leukocyte Patterns in Dogs and CatsSegmented
Condition Total WBC Count Neutrophil Count Band Neutrophil Count Lymphocyte Coun
Overwhelming Decreased Decreased or no change Increased or no change Decreasedinflammation
Acute inflammation Increased or no change Increased or no change Increased or no change Decrease
Chronic inflammation Increased or no change Increased or no change Increased or no change Increase
Excitement Increased or no change Increased in dogs; increased No change No changeor no change in cats increased in cats
Stress Increased or no change Increased or no change No change Decreased
F I G U R E 2
F I G U R E 4F I G U R E 3
F I G U R E 1
1.Canine band neutrophils (modified Wrights stain;100 ).
2.A canine monocyte (modified Wrights stain; 100 ).
3.A buffy coat smear from a dog showing a m( arrow ) phagocytizingHistoplasmaspecies (modifie
Wrights stain; 100 ).4.A reactive lymphocyte in a dog (modified Wstain; 100 ).
-
8/3/2019 3minute Blood Film Evaluations
16/16
Toxic neutrophils are a result of an acceler-ated rate of neutrophil production in re-sponse to inflammatory signals received by the bone marrow. Toxic neutrophil changesinclude retention of cytoplasmic features of immaturity and include foamy basophiliccytoplasm ( Figure 6 ) and small basophilicprecipitates known as Dhle bodies ( Figure 7 ). Dhle bodies are often present in lownumbers in normal cats, so, by themselves,they are a relatively equivocal finding; butDhle bodies indicate serious toxicity indogs.5 Other toxic changes include bizarre
nuclear shapes and cellular giantism ( Fig-ure 8 ).Systemic toxemia is often associated with
bacterial endotoxins, but noninfectiouscauses also occur. Infectious diseases com-monly accompanied by severe neutrophiltoxicity include feline pyothorax, pyometra,and severe canine prostatitis. Noninfectiouscauses associated with toxemia include im-mune-mediated hemolytic anemia, acutepancreatitis, tissue necrosis, zinc and leadtoxicosis, and cytotoxic drug therapy.6
Evaluating the five different WBC
types iscritical when you develop a differential di-agnosis list. Increases or decreases in neu-trophils, eosinophils, basophils, lympho-cytes, and monocytes should alert you toinvestigate certain conditions. For example,neutrophilic left shifts, persistenteosinophilia, and monocytosis are indicatorsof inflammation: Left shifts (increased num-bers of immature, or band, neutrophils incirculation) indicate increased turnover andtissue use of neutrophils. Persistent periph-eral eosinophilia indicates a systemic allergic
or hypersensitivity reaction. And monocyto-sis is seen in peripheral blood when a de-mand for phagocytosis is present.
ACKNOWLEDGMENTThe authors gratefully acknowledge the technicalassistance and images provided by Dennis DeNi-
cola, DVM, PhD, DACVP.
REFERENCES1. Rebar, A.; Metzger, F.: The Veterinary CE Advi-sor: Interpreting Hemograms in Cats and Dogs.Vet. Med. (suppl.) 96 (12):1-12; 2001.2. Duncan, J. et al .: Erythrocytes, leukocytes, he-mostasis. Veterinary Laboratory Medicine , 3rd Ed.Iowa State University Press, Ames, 1994; pp 75-93.3. Willard, M. et al .: Leukocyte disorders. Text-book of Small Animal Clinical Diagnosis by Labo-ratory Methods , 3rd Ed. W.B. Saunders, Philadel-phia, Pa., 1999; pp 53-79.4. Rebar, A.H. et al .: Laboratory methods inhematology. A Guide to Hematology in Dogs and Cats . Teton New Media, Jackson, Wyo., 2002; pp10-28.5. Willard, M. et al .: The complete blood countand bone marrow examination. Textbook of Small Animal Clinical Diagnosis by Laboratory
Methods , 3rd Ed. W.B. Saunders, Philadelphia,Pa., 1999; pp 11-30.6. Duncan, J. et al. : Erythrocytes, leukocytes, he-mostasis. Veterinary Laboratory Medicine , 3rd Ed.Iowa State University Press, Ames, 1994; pp 75-93.
ConclusionAre toxic neutrophils present?
5.Atypical lymphocytes in a dog (modified stain; 100 ).
6.Mild neutrophil toxicity in the form of cytbasophilia in a cat (modified Wrights stai ).
7.Moderate neutrophil toxicity in the form obodies ( arrow ) in a cat (modified Wrights sta100 ).
8.Marked neutrophil toxicity in a dog. Notegiantism and basophilic, foamy, vacuolatecytoplasm (modified Wrights stain; 100 ).
F I G U RE 5 F I G U R E 6
F I G U R E 7 F I G U R E 8
R i t d f VETERINARY MEDICINE D b 2004 P i t d i U S A
IDEXX Part # 09-65274-00