13573588 Case Study for Peri Appendiceal Abcess
-
Upload
licservernoida -
Category
Documents
-
view
9 -
download
0
description
Transcript of 13573588 Case Study for Peri Appendiceal Abcess

I. Patient’s Data
I. General Data
Patient’s. Name: Mrs Kliyente
Sex: female
Age: 53 y/o
Date of Birth: May 20, 1955
Civil status: Married
Citizenship: Filipino
Current Address: Magsaysay Area, Brgy. Sto. Cristo Tala Caloocan City
Religion: Catholic
Occupation: Employer (Carinderia owner)
Room and Bed number:
Hospital number: 52-56-34
Chief Complaint: Abdominal pain
Admitting Diagnosis: t/c Periappendical Abscess
Admission Date and Time: January 27, 2009- 5: 00 pm
Final Diagnosis: Periappendical abscess s/p Exploratory Laparotomy
II Chief Complaint: Abdominal pain
III History of Present illness:
4 weeks prior to admission patient experienced abdominal pain at RLQ of the
abdomen with a pain scale of “10” accompanied by recurrent fever at night and resolved
by paracetamol affording temporary relief of fever. Patient also experienced nausea,
anorexia. Constipation was managed by taking suppository 3x a week. Pt. also took two
tablets of Buscupan in the morning and afternoon for abdominal pain once but didn’t take
effect. Persistence of the condition pt. consulted St. Peter hospital but no diagnosis and
medication given.
1

3 weeks prior to admission patient experienced consistent Right Lower Quadrant
abdominal pain, recurrent fever, nausea constipation, and anorexia. With continuous pain
pt seek consultation at FEU Fairview but no clear diagnosis has been given but given
Cefuroxime and Metronidazole for UTI. Still with persistent abdominal pain pt still used
suppository for temporary relief.
2 weeks prior to admission persistence of above condition, as advised by
personnel’s from FEU Fairview, patient undergone CT scan and Health scan. Still patient
used suppository for temporary relief of constipation and abdominal pain.
A week prior to admission with unfailing occurrence of above condition, patient
prompted to seek consultation of EAMC OPD with the CT scan result. No diagnosis and
medication has been given. Patient still used suppository and stopped using UTI
medications.
Few hours prior to admission patient came back at EAMC still with the CT scan
result and above condition; patient is diagnosed with a leaked abcess from the appendix
T/C “periappendecal abscess” based on the CT scan result. Patient was given Cefuroxime
for abdominal pain w/c took effect and subsequently admitted. CBC laboratory procedure
done and no other exams was done.
IV Past Medical History
Patient has no previous hospitalization, no history of HPN, DM, BA, no known allergies.
V Family Medical History
(+) DM – brother
(+) Appendicitis – daughter
VI Personal and Social Data
Non smoker nor alcoholic drinker
No specific sleeping pattern. The Client prefers vegetables and Fluid Intake one
glass per meal approximately 3-4 times a day.
Own a Carinderia
2

VII Review of System
General/Constitutional
• (-)Weight loss or gain• (-)Fatigue• (-)Headache• (+)Weakness• (+)Restlessness• (-)Trouble sleeping• (+) Activity Intolerance
Skin • (-)Rash, • (-)Itching, • (-)Pigmentation• (+)Dryness• (-)Nail changes
Eyes/Ears/Nose/Mouth/Throat • (+) Headaches• (-) Vertigo• (-) Lightheadedness• (-) Injury • (-) Double vision• (-) Tearing• (-) Pain • (-) Nose bleeding• (-) Colds• (-) Obstruction• (-) Discharge • (+)Dental difficulties• (-) Gingival bleeding• (-) Dentures • (+) Difficulty chewing• (-) Neck stiffness • (-) Tenderness
Cardiovascular • (-)Chest pain• (-) Substernal distress• (-) Palpitations• (-) SyncopeRespiratory • (-) Pain
3

• (-) Cough • (-) Hemoptysis• (-) Dyspnea on exertion, • (-) Orthopnea• (+) Tachynea
Gastrointestinal • (+)Anorexia• (-) Dysphagia,• (-) Food idiosyncrasy• (-) Abdominal pain• (-) Heartburn• (-) Eructation• (-) Nausea• (-) Vomiting• (-) Hematemesis,• (+) Constipation• (-) Flatulence• (-) Hemorrhoids
Genitourinary • (-) Urgency• (-) Frequency• (-) Dysuria• (-) Nocturia• (-) Polyuria• (-) Oliguria
Musculoskeletal • (-) Pain• (-) Swelling• (-) Redness or heat of muscles and joints• (+) Muscular weakness• (-) Cramps
Neurologic:
• (-) Dizziness• (-) Lightheadedness• (-) Numbness• (-) Tremor
Psychiatric:• (+) Nervousness• (+) Stress• (+) Restlessness
4

VIII Physical Examination
Date of Assessment: January 29, 2009
Vital Signs:
Blood Pressure: 110/80 mmHg
Pulse Rate: 110 bpm
Respiratory Rate: 24 bpm
Temperature: 37.7 degrees Celsius (Febrile)
Stool: once a week
General Appearance:
Medium frame built, stooped posture, smooth rhythmic gait, appropriate
dressed, no body and breath odor and obvious physical deformity.
Mental Status/ Neurologic:
Conscious, oriented, anxious, uses simple words for communication.
Integument:
Flushed, warm and dry skin, no edema in extremities,
no lesions, decreased skin turgor, concave nail plate shape,
smooth pink nail bed color and capillary refill within 3 seconds.
Head and Face:
Skull is proportionate to body size, white scalp; partly black to gray shinny
evenly distributed hair. Face is symmetrically and easy facial movement.
Eyes:
Thin eyebrows, effective closure of eyelids and lashes,
bilateral blink response, eyeballs are symmetrical, pinkish bulbar
conjunctiva, white sclera, equal pupils and moist lacrimal apparatus.
Ears:
Auricle color is normal racial, symmetrical and elastic, pinna recoils when
folded, some cerumen in external canal, no aural discharge & responds to
normal voice.
5

Nose:
Normal external racial tone, midline septum, pink mucosa, moist nasal
cavity, with non tender sinuses.
Mouth:
Pallor in the lips & mucosa, midline tongue, smooth and movable,
teeth incomplete.
Pharynx:
Pallor in mucosa, none inflamed tonsil, gag reflex present.
Neck:
ROM neck muscle; palpable non tender lymph nodes, midline trachea,
palpable thyroid gland.
Breast and Axilla:
Sagging, smooth & palpable non tender lymph nodes.
Chest and Lungs:
Symmetrical fremitus, shallow breathing, resonant percussion, heart rate at
110 cpm, pulmonic, aortic, tricuspid and apical heart sounds present.
Abdomen:
Normal racial tone of the skin, flat contour and symmetry, symmetrical
movement, hypoactive bowel sounds, negative in rovsing’s sign and Mc
Burney’s sign.(direct maneuver)
6

X Course in the Ward
January 29, 2009 Received patient lying in bed, very anxious looking, waiting
for the impending surgery. On DAT diet and will progress
to NPO diet post midnight, with no contraptions attached.
Vital Signs taken and recorded. Patient was febrile (37.7 C)
January 30, 2009 The patient was scheduled for surgery (Exploratory
laprotomy), very anxious yet conscious and coherent
However the surgery was cancelled because she has no CP
clearance so the surgery was rescheduled on Tuesday (Feb.
02). V/S has been taken & recorded. Patient was febrile
(37.8 C)
February 05, 2009Received patient. on bed on its second day post-OP,
conscious and coherent. Tense and weak in appearance,
facial grimacing when surgery incision border is palpated,
and verbally reported pain at both sides of abdominal area
with the score of 6. With on going IVF of D5LR at 300cc
level infusing at KVO rate and heplock at the right arm kept
intact. With abdominal elastic bandage dressing then
changed to abdominal sterile gauze dressing kept dry and
clean. On NPO diet and progressed to sips of water.
February 06, 2009At 8:00 am the pt. was febrile (37.6*c) done TSB. The pt.
was on IVF of D5LR at 800cc level infusing at KVO rate
and instructed on moderate high back rest. Still on sips of
water diet, vital signs taken & recorded.
XI Final Diagnosis: Periappendical abscess s/p Explore Laparotomy
7

II Review of Related Literature
What is Appendicitis?
The appendix is a closed-ended, narrow tube up to several inches in length that attaches
to the cecum (the first part of the colon) like a worm. (The anatomical name for the
appendix, vermiform appendix, means worm-like appendage.) The inner lining of the
appendix produces a small amount of mucus that flows through the open center of the
appendix and into the cecum. The wall of the appendix contains lymphatic tissue that is
part of the immune system for making antibodies. Like the rest of the colon, the wall of
the appendix also contains a layer of muscle, but the muscle is poorly developed.
What is appendicitis and what causes appendicitis?
Appendicitis means inflammation of the appendix. It is thought that appendicitis begins
when the opening from the appendix into the cecum becomes blocked. The blockage may
be due to a build-up of thick mucus within the appendix or to stool that enters the
appendix from the cecum. The mucus or stool hardens, becomes rock-like, and blocks the
opening. This rock is called a fecalith (literally, a rock of stool). At other times, the
lymphatic tissue in the appendix may swell and block the appendix. After the blockage
occurs, bacteria which normally are found within the appendix begin to invade (infect)
the wall of the appendix. The body responds to the invasion by mounting an attack on the
bacteria, an attack called inflammation. An alternative theory for the cause of
appendicitis is an initial rupture of the appendix followed by spread of bacteria outside
the appendix.. The cause of such a rupture is unclear, but it may relate to changes that
occur in the lymphatic tissue, for example, inflammation, that line the wall of the
appendix.)
If the inflammation and infection spread through the wall of the appendix, the appendix
can rupture. After rupture, infection can spread throughout the abdomen; however, it
usually is confined to a small area surrounding the appendix (forming a peri-appendiceal
abscess).
8

Sometimes, the body is successful in containing ("healing") the appendicitis without
surgical treatment if the infection and accompanying inflammation do not spread
throughout the abdomen. The inflammation, pain and symptoms may disappear. This is
particularly true in elderly patients and when antibiotics are used. The patients then may
come to the doctor long after the episode of appendicitis with a lump or a mass in the
right lower abdomen that is due to the scarring that occurs during healing. This lump
might raise the suspicion of cancer.
9

What are the complications of appendicitis?
The most frequent complication of appendicitis is perforation. Perforation of the
appendix can lead to a Periappendiceal abscess (a collection of infected pus) or diffuse
peritonitis (infection of the entire lining of the abdomen and the pelvis). The major reason
for appendiceal perforation is delay in diagnosis and treatment. In general, the longer the
delay between diagnosis and surgery, the more likely is perforation. The risk of
perforation 36 hours after the onset of symptoms is at least 15%. Therefore, once
appendicitis is diagnosed, surgery should be done without unnecessary delay.
A less common complication of appendicitis is blockage of the intestine. Blockage occurs
when the inflammation surrounding the appendix causes the intestinal muscle to stop
working, and this prevents the intestinal contents from passing. If the intestine above the
blockage begins to fill with liquid and gas, the abdomen distends and nausea and
vomiting may occur. It then may be necessary to drain the contents of the intestine
through a tube passed through the nose and esophagus and into the stomach and intestine.
10

A feared complication of appendicitis is sepsis, a condition in which infecting bacteria
enter the blood and travel to other parts of the body. This is a very serious, even life-
threatening complication. Fortunately, it occurs infrequently.
What are the symptoms of appendicitis?
The main symptom of appendicitis is abdominal pain. The pain is at first diffuse and
poorly localized, that is, not confined to one spot. (Poorly localized pain is typical
whenever a problem is confined to the small intestine or colon, including the appendix.)
The pain is so difficult to pinpoint that when asked to point to the area of the pain, most
people indicate the location of the pain with a circular motion of their hand around the
central part of their abdomen. A second, common, early symptom of appendicitis is loss
of appetite which may progress to nausea and even vomiting. Nausea and vomiting also
may occur later due to intestinal obstruction.
As appendiceal inflammation increases, it extends through the appendix to its outer
covering and then to the lining of the abdomen, a thin membrane called the peritoneum.
Once the peritoneum becomes inflamed, the pain changes and then can be localized
clearly to one small area. Generally, this area is between the front of the right hip bone
and the belly button. The exact point is named after Dr. Charles McBurney--McBurney's
point. If the appendix ruptures and infection spreads throughout the abdomen, the pain
becomes diffuse again as the entire lining of the abdomen becomes inflamed.
Rovsing's sign
Deep palpation of the left iliac fossa may cause pain in the right iliac fossa. This is the
Rovsing's sign, also known as the Rovsing's symptom. It is used in the diagnosis of acute
appendicitis. Pressure over the descending colon causes pain in the right lower quadrant
of the abdomen.
11

McBurney’s Sign
McBurney's sign, is a sign of acute appendicitis.[2] The clinical sign of rebound pain
when pressure is applied is also known as Aaron's sign.
Specific localization of tenderness to McBurney's point indicates that inflammation is no
longer limited to the lumen of the bowel (which localizes pain poorly), and is irritating
the lining of the peritoneum at the place where the peritoneum comes into contact with
the appendix. Tenderness at McBurney's point suggests the evolution of acute
appendicitis to a later stage, and thus, the increased likelihood of rupture. Because the
location of the appendix is often different in different people, and can migrate within the
abdomen, many cases of appendicitis do not cause point tenderness at McBurney's point.
Other abdominal processes can also sometimes cause tenderness at McBurney's point.
Thus, this sign is highly useful but neither necessary nor sufficient to make a diagnosis of
acute appendicitis. Also, the anatomical position of the appendix is highly variable (for
example in retrocaecal appendix, an appendix behind the caecum), which also limits the
use of this sign.
Psoas sign
Occasionally, an inflamed appendix lies on the psoas muscle and the patient will lie with
the right hip flexed for pain relief.
Obturator sign
If an inflamed appendix is in contact with the obturator internus, spasm of the muscle can
be demonstrated by flexing and internally rotating the hip. This maneuver will cause pain
in the hypogastrium.
12

If the appendix curls around behind the cecum, pain and tenderness may be felt in the
lumbar region. If its tip is in the pelvis, these signs may be elicited only on rectal
examination. Pain on defecation suggests that the tip of the appendix is resting against the
rectum; pain on urination suggests that the tip is near the bladder or impinges on the
ureter.
How is appendicitis diagnosed?
The diagnosis of appendicitis begins with a thorough history and physical examination.
Patients often have an elevated temperature, and there usually will be moderate to severe
tenderness in the right lower abdomen when the doctor pushes there. If inflammation has
spread to the peritoneum, there is frequently rebound tenderness. Rebound tenderness is
pain that is worse when the doctor quickly releases his hand after gently pressing on the
abdomen over the area of tenderness.
13

White Blood Cell Count
The white blood cell count in the blood usually becomes elevated with infection. In early
appendicitis, before infection sets in, it can be normal, but most often there is at least a
mild elevation even early. Unfortunately, appendicitis is not the only condition that
causes elevated white blood cell counts. Almost any infection or inflammation can cause
this count to be abnormally high. Therefore, an elevated white blood cell count alone
cannot be used as a sign of appendicitis.
Urinalysis
Urinalysis is a microscopic examination of the urine that detects red blood cells, white
blood cells and bacteria in the urine. Urinalysis usually is abnormal when there is
inflammation or stones in the kidneys or bladder. The urinalysis also may be abnormal
with appendicitis because the appendix lies near the ureter and bladder. If the
inflammation of appendicitis is great enough, it can spread to the ureter and bladder
leading to an abnormal urinalysis. Most patients with appendicitis, however, have a
normal urinalysis. Therefore, a normal urinalysis suggests appendicitis more than a
urinary tract problem.
Abdominal X-Ray
An abdominal x-ray may detect the fecalith (the hardened and calcified, pea-sized piece
of stool that blocks the appendiceal opening) that may be the cause of appendicitis. This
is especially true in children.
14

Ultrasound
An ultrasound is a painless procedure that uses sound waves to identify organs within the
body. Ultrasound can identify an enlarged appendix or an abscess. Nevertheless, during
appendicitis, the appendix can be seen in only 50% of patients. Therefore, not seeing the
appendix during an ultrasound does not exclude appendicitis. Ultrasound also is helpful
in women because it can exclude the presence of conditions involving the ovaries,
fallopian tubes and uterus that can mimic appendicitis.
Barium Enema
A barium enema is an x-ray test where liquid barium is inserted into the colon from the
anus to fill the colon. This test can, at times, show an impression on the colon in the area
of the appendix where the inflammation from the adjacent inflammation impinges on the
colon. Barium enema also can exclude other intestinal problems that mimic appendicitis,
for example Crohn's disease.
Computerized tomography (CT) Scan
In patients who are not pregnant, a CT Scan of the area of the appendix is useful in
diagnosing appendicitis and peri-appendiceal abscesses as well as in excluding other
diseases inside the abdomen and pelvis that can mimic appendicitis.
Laparoscopy
Laparoscopy is a surgical procedure in which a small fiberoptic tube with a camera is
inserted into the abdomen through a small puncture made on the abdominal wall.
Laparoscopy allows a direct view of the appendix as well as other abdominal and pelvic
organs. If appendicitis is found, the inflamed appendix can be removed with the
laparascope. The disadvantage of laparoscopy compared to ultrasound and CT is that it
requires a general anesthetic.4
15

There is no one test that will diagnose appendicitis with certainty. Therefore, the
approach to suspected appendicitis may include a period of observation, tests as
previously discussed, or surgery.
Why can it be difficult to diagnose appendicitis?
It can be difficult to diagnose appendicitis. The position of the appendix in the abdomen
may vary. Most of the time the appendix is in the right lower abdomen, but the appendix,
like other parts of the intestine, has a mesentery. This mesentery is a sheet-like membrane
that attaches the appendix to other structures within the abdomen. If the mesentery is
large, it allows the appendix to move around. In addition, the appendix may be longer
than normal. The combination of a large mesentery and a long appendix allows the
appendix to dip down into the pelvis (among the pelvic organs in women). It also may
allow the appendix to move behind the colon (called a retro-colic appendix). In either
case, inflammation of the appendix may act more like the inflammation of other organs,
for example, a woman's pelvic organs.
The diagnosis of appendicitis also can be difficult because other inflammatory problems
may mimic appendicitis. Therefore, it is common to observe patients with suspected
appendicitis for a p
eriod of time to see if the problem will resolve on its own or develop characteristics that
more strongly suggest appendicitis or, perhaps, another condition.
What other conditions can mimic appendicitis?
The surgeon faced with a patient suspected of having appendicitis always must consider
and look for other conditions that can mimic appendicitis. Among the conditions that
mimic appendicitis are:
16

* Meckel's diverticulitis. A Meckel's diverticulum is a small outpouching of the small
intestine which usually is located in the right lower abdomen near the appendix. The
diverticulum may become inflamed or even perforate (break open or rupture). If inflamed
and/or perforated, it usually is removed surgically.
* Pelvic inflammatory disease. The right fallopian tube and ovary lie near the
appendix. Sexually active women may contract infectious diseases that involve the tube
and ovary. Usually, antibiotic therapy is sufficient treatment, and surgical removal of the
tube and ovary are not necessary.
* Inflammatory diseases of the right upper abdomen. Fluids from the right upper
abdomen may drain into the lower abdomen where they stimulate inflammation and
mimic appendicitis. Such fluids may come from a perforated duodenal ulcer, gallbladder
disease, or inflammatory diseases of the liver, e.g., a liver abscess.
* Right-sided diverticulitis. Although most diverticuli are located on the left side of the
colon, they occasionally occur on the right side. When a right-sided diverticulum ruptures
it can provoke inflammation they mimics appendicitis.
* Kidney diseases. The right kidney is close enough to the appendix that inflammatory
problems in the kidney-for example, an abscess-can mimic appendicitis
How is appendicitis treated?
Once a diagnosis of appendicitis is made, an appendectomy usually is performed.
Antibiotics almost always are begun prior to surgery and as soon as appendicitis is
suspected.
There is a small group of patients in whom the inflammation and infection of appendicitis
remain mild and localized to a small area. The body is able not only to contain the
inflammation and infection but to resolve it as well. These patients usually are not very ill
17

and improve during several days of observation. This type of appendicitis is referred to as
"confined appendicitis" and may be treated with antibiotics alone. The appendix may or
may not be removed at a later time.
On occasion, a person may not see their doctor until appendicitis with rupture has been
present for many days or even weeks. In this situation, an abscess usually has formed,
and the appendiceal perforation may have closed over. If the abscess is small, it initially
can be treated with antibiotics; however, the abscess usually requires drainage. A drain (a
small plastic or rubber tube) usually is inserted through the skin and into the abscess with
the aid of an ultrasound or CT scan that can determine the exact location of the abscess.
The drain allows pus to flow from the abscess out of the body. The appendix may be
removed several weeks or months after the abscess has resolved. This is called an interval
appendectomy and is done to prevent a second attack of appendicitis.
How is an appendectomy done?
During an appendectomy, an incision two to three inches in length is made through the
skin and the layers of the abdominal wall over the area of the appendix. The surgeon
enters the abdomen and looks for the appendix which usually is in the right lower
abdomen. After examining the area around the appendix to be certain that no additional
problem is present, the appendix is removed. This is done by freeing the appendix from
its mesenteric attachment to the abdomen and colon, cutting the appendix from the colon,
and sewing over the hole in the colon. If an abscess is present, the pus can be drained
with drains that pass from the abscess and out through the skin. The abdominal incision
then is closed.
Newer techniques for removing the appendix involve the use of the laparoscope. The
laparoscope is a thin telescope attached to a video camera that allows the surgeon to
inspect the inside of the abdomen through a small puncture wound (instead of a larger
incision). If appendicitis is found, the appendix can be removed with special instruments
that can be passed into the abdomen, just like the laparoscope, through small puncture
wounds. The benefits of the laparoscopic technique include less post-operative pain
18

(since much of the post-surgery pain comes from incisions) and a speedier return to
normal activities. An additional advantage of laparoscopy is that it allows the surgeon to
look inside the abdomen to make a clear diagnosis in cases in which the diagnosis of
appendicitis is in doubt. For example, laparoscopy is especially helpful in menstruating
women in whom a rupture of an ovarian cysts may mimic appendicitis.
If the appendix is not ruptured (perforated) at the time of surgery, the patient generally is
sent home from the hospital after surgery in one or two days. Patients whose appendix
has perforated are sicker than patients without perforation, and their hospital stay often
is prolonged (four to seven days), particularly if peritonitis has occurred. Intravenous
antibiotics are given in the hospital to fight infection and assist in resolving any abscess.
Occasionally, the surgeon may find a normal-appearing appendix and no other cause for
the patient's problem. In this situation, the surgeon may remove the appendix. The
reasoning in these cases is that it is better to remove a normal-appearing appendix than to
miss and not treat appropriately an early or mild case of appendicitis.
19

20

21

22

23

What are the complications of appendectomy?
The most common complication of appendectomy is infection of the wound, that is, of
the surgical incision. Such infections vary in severity from mild, with only redness and
perhaps some tenderness over the incision, to moderate, requiring only antibiotics, to
severe, requiring antibiotics and surgical treatment. Occasionally, the inflammation and
infection of appendicitis are so severe that the surgeon will not close the incision at the
end of the surgery because of concern that the wound is already infected. Instead, the
surgical closing is postponed for several days to allow the infection to subside with
antibiotic therapy and make it less likely for infection to occur within the incision.
Wound infections are less common with laparoscopic surgery.
Another complication of appendectomy is an abscess, a collection of pus in the area of
the appendix. Although abscesses can be drained of their pus surgically, there are also
non-surgical techniques, as previously discussed.
24

Are there long-term consequences of appendectomy?
It is not clear if the appendix has an important role in the body in older children and
adults. There are no major, long-term health problems resulting from removing the
appendix although a slight increase in some diseases has been noted, for example,
Crohn's disease.
Gerontologic Considerations
Acute appendicitis does not occur frequently in the elderly population. Classic signs
and symptoms are altered and may vary greatly. Pain may be absent or minimal.
Symptoms may be vague, suggesting bowel obstruction or another process. Fever
and leukocytosis may not be present. As a result, diagnosis and prompt treatment
may be delayed, causing potential complications and mortality. The patient may
have no symptoms until the appendix ruptures. The incidence of perforated
appendix is higher in the elderly population because many of these patients do not
seek health care as quickly as younger patients.
PHARMACOLOGIC ASPECTS OF AGING
Older people use more medications than does any other age group: although they
comprise only 12.6% of the total population, they use 30% of all prescribed medications
and 40% of all over-the-counter medications. Medications have improved the
health and well-being of older people by alleviating symptoms of discomfort, treating
chronic illnesses, and curing infectious processes. Problems commonly occur, however,
because of medicationinteractions, multiple medication effects, multiple medication
use (polypharmacy), and noncompliance. Combinations of prescription medications and
some over-the-counter medications further complicate the problem.
Any medication is capable of altering nutritional status, which, in the elderly, may
already be compromised by a marginal diet or by chronic disease and its treatment.
25

Medications can depress the appetite, cause nausea and vomiting, irritate the stomach,
cause constipation or diarrhea, and decrease absorption of nutrients. In addition, they can
alter electrolyte balance and carbohydrate and fat metabolism. A few examples of
medications capable of altering the nutritional status are antacids, which produce
thiamine
deficiency; cathartics, which diminish absorption; antibiotics and phenytoin, which
reduce utilization of folic acid; and phenothiazines, estrogens, and corticosteroids, which
increase food intake and cause weight gain.
Age
Age has long been the focus of research on pain perception and pain tolerance, and again
the results have been inconsistent. For example, although some researchers have found
that older adults require a higher intensity of noxious stimuli than do younger adults
before they report pain (Washington, Gibson & Helme, 2000), others have found no
differences in responses of younger and older adults (Edwards & Filligim, 2000). Other
researchers have found that elderly patients (older than 50 years of age) reported
significantly less pain than younger patients (Li, Greenwald, Gennis et al., 2001).
Experts in the field of pain management have concluded that if pain perception is
diminished in the elderly person, it is most likely secondary to a disease process (eg,
diabetes) rather than to aging (American Geriatrics Society, 1998). More research is
needed in the area of aging and its effects on pain perception to understand what the
elderly are experiencing. Although many elderly people seek health care because of pain,
others are reluctant to seek help even when in severe pain because they consider pain to
be part of normal aging. Assessment of pain in older adults may be difficult because
of the physiologic, psychosocial, and cognitive changes that often accompany aging.
In one study, as many as 93% of nursing home residents reported being in pain daily for
the past 6 months (Weiner, Peterson, Ladd et al., 1999). Unrelieved pain contributes to
the problems of depression, sleep disturbances, delayed rehabilitation, malnutrition, and
cognitive dysfunction (Miaskowski, 2000). The way an older person responds to pain
may differ from the way a younger person responds.
26

Because elderly people have a slower metabolism and a greater ratio of body fat to
muscle mass than younger people, small doses of analgesic agents may be sufficient
to relieve pain, and these doses may be effective longer (Buffum & Buffum, 2000).
Elderly patients deal with pain according to their lifestyle, personality, and cultural
background, as do younger adults. Many elderly people are fearful of addiction and,
as a result, will not report that they are in pain or ask for pain medication. Others
fail to seek care because they fear that the pain may indicate serious illness or they fear
loss of independence. Elderly patients must receive adequate pain relief after surgery or
trauma. When an elderly person becomes confused after surgery or trauma, the confusion
is often attributed to medications, which are then discontinued. However, confusion in
the elderly may be a result of untreated and unrelieved pain. In some cases postoperative
confusion clears once the pain is relieved. Judgments about pain and the adequacy of
treatment should be based on the patient’s report of pain and pain relief rather than on
age.
27

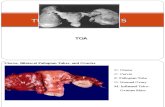
Peri-appendiceal abscess
(Appendix, cut section, showing that pus fills the appendix lumen and spills out into the
fat, forming a peri-appendiceal abscess. This is a surgical emergency.)
If the inflammation and infection spread through the wall of the appendix, the
appendix can rupture. After rupture, infection can spread throughout the abdomen;
however, it usually is confined to a small area surrounding the appendix (forming a peri-
appendiceal abscess).
Treatment
A laparotomy is a large incision made into the abdomen. Exploratory laparotomy is used
to visualize and examine the structures inside of the abdominal cavity.
Purpose:
Exploratory laparotomy is a method of abdominal exploration, a diagnostic tool that
allows physicians to examine the abdominal organs. The procedure may be recommended
for a patient who has abdominal pain of unknown origin or who has sustained an injury to
the abdomen. Because of the nature of the abdominal organs, there is a high risk of
28

infection if organs rupture or are perforated. In addition, bleeding into the abdominal
cavity is considered a medical emergency. Exploratory laparotomy is used to determine
the source of pain or the extent of injury and perform repairs if needed.
Laparotomy may be performed to determine the cause of a patient's symptoms or to
establish the extent of a disease.
Some other conditions that may be discovered or investigated during exploratory
laparotomy include:
cancer of the abdominal organs
peritonitis (inflammation of the peritoneum, the lining of the abdominal cavity)
appendicitis (inflammation of the appendix)
pancreatitis (inflammation of the pancreas)
abscesses (a localized area of infection)
adhesions (bands of scar tissue that form after trauma or surgery)
diverticulitis (inflammation of sac-like structures in the walls of the intestines)
intestinal perforation
ectopic pregnancy (pregnancy occurring outside of the uterus)
foreign bodies (e.g., a bullet in a gunshot victim)
internal bleeding
Demographics
Because laparotomy may be performed under a number of circumstances to diagnose or
treat numerous conditions, no data exists as to the overall incidence of the procedure.
Description
The patient is usually placed under general anesthesia for the duration of surgery. The
advantages to general anesthesia are that the patient remains unconscious during the
29

procedure, no pain will be experienced nor will the patient have any memory of the
procedure, and the patient's muscles remain completely relaxed, allowing safer surgery.
Incision
Once an adequate level of anesthesia has been reached, the initial incision into the skin
may be made. A scalpel is first used to cut into the superficial layers of the skin. The
incision may be median (vertical down the patient's midline), paramedian (vertical
elsewhere on the abdomen), transverse (horizontal), T-shaped, or curved, according to the
needs of the surgery. The incision is then continued through the subcutaneous fat, the
abdominal muscles, and finally, the peritoneum. Electrocautery is often used to cut
through the subcutaneous tissue as it has the ability to stop bleeding as it cuts.
Instruments called retractors may be used to hold the incision open once the abdominal
cavity has been exposed.
Abdominal Exploration
The surgeon may then explore the abdominal cavity for disease or trauma. The abdominal
organs in question will be examined for evidence of infection, inflammation, perforation,
26
abnormal growths, or other conditions. Any fluid surrounding the abdominal organs will
be inspected; the presence of blood, bile, or other fluids may indicate specific diseases or
injuries. In some cases, an abnormal smell encountered upon entering the abdominal
cavity may be evidence of infection or a perforated gastrointestinal organ.
If an abnormality is found, the surgeon has the option of treating the patient before
closing the wound or initiating treatment after exploratory surgery. Alternatively, samples
of various tissues and/or fluids may be removed for further analysis. For example, if
cancer is suspected, biopsies may be obtained so that the tissues can be examined
microscopically for evidence of abnormal cells. If no abnormality is found, or if
immediate treatment is not needed, the incision may be closed without performing any
further surgical procedures.
During exploratory laparotomy for cancer, a pelvic washing may be performed; sterile
fluid is instilled into the abdominal cavity and washed around the abdominal organs, then
30

withdrawn and analyzed for the presence of abnormal cells. This may indicate that a
cancer has begun to spread (metastasize).
Closure
Upon completion of any exploration or procedures, the organs and related structures are
returned to their normal anatomical position. The incision may then be sutured (stitched
closed). The layers of the abdominal wall are sutured in reverse order, and the skin
incision closed with sutures or staples.
Diagnosis/Preparation
Various diagnostic tests may be performed to determine if exploratory laparotomy is
necessary. Blood tests or imaging techniques such as x ray, computed tomography (CT)
scan, and magnetic resonance imaging (MRI) are examples. The presence of
intraperitoneal fluid (IF) may be an indication that exploratory laparotomy is necessary;
one study indicated that IF was present in nearly three-quarters of patients with intra-
abdominal injuries.
Directly preceding the surgical procedure, an intravenous (IV) line will be placed so that
fluids and/or medications may be administered to the patient during and after surgery. A
Foley catheter will be inserted into the bladder to drain urine. The patient will also meet
with the anesthesiologist to go over details of the method of anesthesia to be used.
Aftercare
The patient will remain in the postoperative recovery room for several hours where his or
her recovery can be closely monitored. Discharge from the hospital may occur in as little
as one to two days after the procedure, but may be later if additional procedures were
performed or complications were encountered. The patient will be instructed to watch for
symptoms that may indicate infection, such as fever, redness or swelling around the
incision, drainage, and worsening pain.
31

Risks
Risks inherent to the use of general anesthesia include nausea, vomiting, sore throat,
fatigue, headache, and muscle soreness; more rarely, blood pressure problems, allergic
reaction, heart attack, or stroke may occur. Additional risks include bleeding, infection,
injury to the abdominal organs or structures, or formation of adhesions (bands of scar
tissue between organs).
Morbidity and Mortality Rates
The operative and postoperative complication rates associated with exploratory
laparotomy vary according to the patient's condition and any additional procedures
performed.
Alternatives
Laparoscopy is a relatively recent alternative to laparotomy that has many advantages.
Also called minimally invasive surgery, laparoscopy is a surgical procedure in which a
laparoscope (a thin, lighted tube) and other instruments are inserted into the abdomen
through small incisions.
The internal operating field may then be visualized on a video monitor that is connected
to the scope. In some patients, the technique may be used for abdominal exploration in
place of a laparotomy. Laparoscopy is associated with faster recovery times, shorter
hospital stays, and smaller surgical scars.
32

During a laparotomy, and an incision is made into the patient's abdomen (A). Skin and
connective tissue called fascia is divided (B). The lining of the abdominal cavity, the peritoneum, is cut, and any exploratory procedures are undertaken (C). To close the incision, the peritoneum, fascia, and skin are stitched (E). (Illustration by GGS Inc.)
33

III Anatomy and Physiology
Large Intestine:.
Its primary purpose is to extract water from feces. About 1.5 M (5 feet) long, it
extends from the ileocecal valve to the anus.
Major functions are to dry out the indigestible food residue by absorbing water &
to eliminate these residues from the body as feces.
It frames the small intestine on these sides & has the following subdivisions:
cecum, appendix, colon, rectum & anal canal.
Cecum
The cecum (also spelled caecum), the first portion of the large bowel, situated in
the lower right quadrant of the abdomen.
The cecum receives fecal material from the small bowel (ileum) which opens into
it. The appendix is attached to the cecum.
The bottom of the cecum is a blind pouch (a cul de sac) leading nowhere.A pouch
connected to the ascending colon of the large intestine and the ileum. It is separated from
the ileum by the ileocecal valve (ICV) or Bauhin's valve, and is considered to be the
beginning of the large
34

Appendix
The appendix is a branch of the cecum, like the appendix, the cecum was once
believed to have no function.
The appendix is a small, finger-like appendage about 10 cm (4 in) long that is
attached to the cecum just below the ileocecal valve. The appendix fills with food and
empties regularly into the cecum. Because it empties inefficiently and its lumen is small,
the appendix is prone to obstruction and is particularly vulnerable to infection.
Ascending colon
Smaller in caliber than the cecum, with which it is continuous.It passes upward,
from its commencement at the cecum, opposite the colic valve, to the under surface of the
right lobe of the liver, on the right of the gall-bladderyeo, where it is lodged in a shallow
depression, the colic impression; here it bends abruptly forward and to the left, forming
the right colic flexure (hepatic).
Transverse Colon
Longest and most movable part of the colon, passes with a downward convexity
from the right hypochondrium region across the abdomen, opposite the confines of the
epigastric and umbilical zones, into the left hypochondrium region, where it curves
sharply on itself beneath the lower end of the spleen, forming the splenic or left colic
flexure. The right colic flexure is adjacent to the liver.
.
Rectum
The last 6 to 8 inches of the large intestine. The rectum stores solid waste until it
leaves the body through the anus.
Anus
Termination of Rectum formed of spichnter which relaxes to allow fecal matter to
pass through.
35

IV Pathophyisiology
A. Written Report:
The following case introduces a fifty three year old female patient who was
brought to the hospital because of the persistent conditions such as abdominal pain,
recurrent fever, nausea, anorexia. After further tests and surgery performed, the patient
was diagnosed with Periappendical abscess s/p Exploratomy Laparotomy.
This study focuses on one of the complications of Appendicitis which is the Peri-
appendicial abscess that is cause of untreated inflammation of appendix. The patient
obstruction of the lumen was believed to arise spontaneously on an obscure or unknown
cause. Impediment of the lumen causes the mucous secretion to increase and its
accumulation causes luminal pressure to increase. Condition appears to favor resident
bacterial growth. Inflammation develops resulting to mucosal damage. With continued
swelling, the appendix presses against the adjacent abdominal wall and its sensitive
parietal peritoneum causing to deteriorate and perforate. Contents of appendical abscess
leaked to the peritoneum surfaces. Contents are confined to a small area of appendix.
Spillage of the contents causes the inflammation of parietal peritoneum leading to the
manifestation of fever.
36

Obstruction of the lumen
↑ mucosal secretion
↑ intraluminal pressure
Bacterial Invasion( resident Bacteria from intestine)
Mucosal damage
Spillage of infected appendical contents
outside appendix
Confined to a small area surrounding appendix
( peri-appendiceal abscess)
37
Inflammation of parietal peritoneum
FEVER
Anticipatory for Surgery (Exploratory
Laparotomy)
anxiety Activity Intolerance
Acute painHyperthermia
Idiopathic(Constipation/Fecalith)
Inflammation

B. Diagram
V Problem List
Pre-operative:
1. Fever – Hyperthermia
2. Anxiety
Post-operative:
1. Acute Pain
2. Activity Intolerance
3. Anxiety
38

VI Laboratory and Diagnostic Procedures
January 27. 2009
LABORATORY PROCEDURE: Complete Blood Count
Hemoglobin
Red pigments in red blood cell that carries oxygen all through out the body.
A. Test and ResultTest Result Reference Value
Hemoglobin (Hgb) 123 Male: 140-170/L Female: 120-150/L
B. InterpretationHemoglobin count was within the normal range
C. SignificanceIncrease in normal range
Polycythemia, Chronic Obstructive Pulmonary Disease Congestive Heart Failure
Decrease in normal range Anemia Hemorrhage
Hematocrit
The Percentage of Red Blood Cell of the total blood volume.
A, Test and Result
Test Result Reference Value
Hematocrit (Hct) 37% Male:42-51%Female:37-47%
B. Interpretation
Hematocrit count was within the normal range
39

C. Significance
Increase in normal range Erythrocytosis Dehydration
Decrease in normal range Hemorrhage Anemia Pregnancy
RBC Count
It is the count of the actual number of red blood cells per volume of blood.
A. Test and ResultTest Result Reference Value
RBC count 4.3 Male:4.5-5.9 x 106g/LFemale:4.5-5.1 x 106g/L
B. InterpretationRBC count was .2 lower that the normal range which may indicate dietary
deficiency because the client was anorexic.
C. SignificanceIncrease in normal range
Dehydration Pulmonary Fibrosis Erythrocytosis Polycythemia Congenital Heart Disease Chronic Obstructive Pulmonary Disease
Decrease in normal range Hemorrhage Anemia Pregnancy Dietary Deficiency
40

WBC CountIt is the count of the actual number of white blood cells per volume of blood.
A. Test and ResultTest Result Reference Value
WBC Count 6.1 5.0-10.0x103/L
B. InterpretationWBC count was within the normal range
C. SignificanceIncrease in normal range
Infection Steroid use
Decrease in normal range Bone Marrow failure Iron Deficiency
Platelet Count
A. Test and ResultTest Result Reference Value
Platelet Count Adequate 150-400x106/L
B. SignificanceIncrease in normal range
Rheumatoid arthritis Malignant Disorder Polycythemia Iron Deficiency Anemia
Decrease in normal range Thrombocytopenic Purpura, Acute leukemia, Aplastic anemia, Cancer chemotherapy.
41

Differential Count
NeutrophilsMake up 50% to 60% of leukocytes in the blood and are responsible for
phagocytosis of bacteria and cellular debris.
LymphocytesMake up 20% to 30% of the total white blood cells and are responsible in
producing antibody
MonocytesAre phagocytic cell.It can be produced rapidly and make up about 5% of the total
white blood cell count.
EosinophilsMake up 1%-4% of the total leukocytes. Increases in number during allergic
states and infestation with worms.
BasophilsIncreased in numbers in such pathological conditions and make up approximately
0.5%-1.0% of leukocytes.A. Test and Result
Test Result Reference Value
Neutrophils 0.63 0.45-0.65
Lymphocytes 0.37 0.25-0.35
Monocytes -- 0.03-0.06
Stabs -- 0.02-0.04
Eosinophils -- 0.02-0.04
Basophils-- 00-0.05
Blasts-- 0.0
ABO/RH Typing B+
42

B. Interpretations
The result for Neutrophils count was within the normal range. Lymphocytes count
was .0.02 more than the normal range which may indicate chronic bacterial infection or
viral infection. The patient blood type appeared to be B+.
C. SignificanceIncrease in normal range
Neutrophils
Acute infections
Trauma or surgery
Leukemia,
Malignant disease
Necrosis
Stress
Lymphocytes
Chronic Infection
Viral Infection
Mononecleosis
Monocytes
Chronic Inflammatory Disorder
Tuberculosis
Parasitic disease
Eosinophils
Parasitic Infections
Allergic reactions
Leukemia
Basophils
Leukemia
Decrease in normal range
Neutrophils
43

Aplastic Anemia
Dietary Deficiency
Radiation Therapy
Bone marrow suppression
Lymphocytes
Leukemia
Sepsis
Immunodeficiency disease
SLE
Immunodeficiency including AIDS
Monocytes
Drug therapy: Prednisone
Eosinophils
Stress
Use of some medications (ACTH, epinephrine, thyroxine)
Basophils
Allergic reactions
Stress
Nursing Considerations
1. Make sure that the vital signs are stable.
2. Choose non-dominant hand for the site when getting the specimen
3. Clean the site
4. Apply tourniquet to the site but not more than two minutes
5. Apply light pressure to make sure that the site is correct
6. If failed to the first attempt, change the site from distal to proximal
7. Release the tourniquet once there is blood in the hub
44

8. Transfer immediately the collected blood to the specimen container with purple
cap and deliver to the laboratory not more that 30 minutes.
9. To prevent coagulation turn the container upside down.
Diagnostic Procedures
A. Test and Result
CT Scan
Painless diagnostic procedure for examining soft tissue. It allows
visualization of grey matter, necrotic tissue, and tumors.
EXAM: CT SCAN of the whole abdomenDate: January 15, 2009
CT SCAN Report
History: 1 Month. History of Intermittent right Quadrant pain. Multiple axial tomograpic
sections of the whole abdomen with oral contrast and intravenous contrast were obtained.
A peripherally enhancing complex predominantly cystic mass is seen in the Right Lower
abdomen, adjacent to the ileo-cecal junction, most likely extra-luminal. It measures 5 cm
x 7cm x 5 cm. Surrounding fat stranding is seen. The visualized small and large bowels
appear unremarkable. The liver, gall bladder, pancreas, adrenal glands and spleen show
no unusual findings. The kidney and its collecting structures including the urinary
bladder are intact. The uterus is normal in size with no focal lesions noted. No adrenal
masses seen. The abdominal aorta shows no dilatation. Minimal curvilinear are seen in
the included lung bases. The rest of the soft tissues, vascular and osseous structures are
unremarkable.
Impression:Complex mass at the right lower abdomen; consider a Periappendiceal periceal
abscess- Minimal fibrotic changes, bilateral lower lungs.
B. Nursing Considerations
45

1. Secure Consent of the client.
2. Inform client that the procedure will take 30 minutes to 1 hour.
3. Explain test purpose and procedure. Provide written instructions. Reinforce
knowledge regarding possible adverse effects such as radiation.
4. Inform the client that there will be clicking and whirring noise and that he/she
may use earplugs.
5. Provide medications as ordered.
6. Reassure the patient that scanning procedures no greater radiation than
conventional x-ray studies
7. Check for patient allergies such as nausea, vomiting, warmth, and flushing of the
face may signal possible allergy for iodine.
8. Check for signs of claustrophobia
9. Be aware that abdominal cramping and diarrhea may occur; therefore medication
may be given as ordered to decrease these side effects.
10. Inform the patient that solid foods are usually withheld on the day of examination.
Clear liquids may be taken up to 2 hours before examination.
11. For CT of the abdomen, the patient usually can take nothing by mouth.
12. Notify physician immediately if allergic reaction occurs.
13. Secure Consent of the client.
14. Inform client that the procedure will take 30 minutes to 1 hour.
15. Inform the client that there will be clicking and whirring noise and that he/she
may use earplug.
A. Test and Result
46

Roentegnographic
Roentenographic Report
Date: January 10, 2009
Abdomen:
Shows gas in the visualize bowel loops. Minimal feces are seen in the rectum. Gas
pattern is non obstructive. Osseous structures & soft tissue outline are intact.
Impression:
Unremarkable abdomen
B. Nursing Considerations
1. The patient should be given a brief explanation of the purpose of and procedure
for the test and assured that there will be no discomfort.
2. Remove all jewelry and other ornamentation in the abdomen area before the X-
ray
3. Remind the patient of need to remain motionless during the procedure.
47

VII Drug Study
Name of Drug Action Indication Route and Dosage
Availability Contraindications Adverse Effects
Nursing Indications
Hyoscine N-
Butykbromide
Inhibits
acetycholine
at receptor
sites in
autonomic
nervous
system, which
controls
secretions,
free acids in
stomach;
blocks central
muscarinic
receptors,
which
decreases
involuntary
Used in the
management of
various
gastrointestinal
disorders.
Tablet:
adult and
children >6
yrs: 10-
20mg 3-5
times daily.
Injection: 0.3
mg/ml and 1
mg/ml in 1-
ml vials, 0.4
mg/ml in 0.5-
ml ampules
and 1-ml
vials, 0.86
mg/ml in 0.5-
ml ampules
Tablets: 0.4 mg
Transdermal
system
Myasthenia gravi,
megacolon,
hypersensitivity.
Xerostomia,
tachycardia,
urinary
retention..
-Tell patient
to avoid
hazardous
activities
requiring
alertness;
dizziness
may occur.
-Advice
patient to
avoid use of
alcohol or
other CNS
depressants
while taking
medication.
48

movements..(Transderm-
Scop): 1.5
mg/patch
(releases 0.5
mg
scopolamine
over 3 days)
-Explain that
rinsing the
mouth, good
oral hygiene,
and sugarless
gum or candy
will help to
counteract
dryness.
Started: December 28, 2008
Discontinued: December 28, 2008
49

Name of Drug Action Indication Route and
Dosage
Availability Contraindications Adverse Effects Nursing Indications
Acetaminophen May cause
analgesia by
inhibiting
CNS
prostaglandin
synthesis.
Relief mild-
to-moderate
pain:
treatment of
fever.
25 to 650
mg P.O. q
4 to 6
hours, or
1,000 mg
three or
four times
daily.
Caplets,
capsules: 160
mg, 500 mg,
650 mg
(Drops: 100
mg/ml
Elixir: 80
mg/2.5 ml, 80
mg/5 ml, 120
mg/5 ml, 160
mg/5 ml
Gelcaps: 500
mg
Liquid: 160
mg/5 ml, 500
mg/15 ml
Solution: 80
mg/1.66 ml,
Hypersensitivity:
Intolerance to
tartrazine, alcohol,
table sugar,
saccharin.
Stimulation,
drowiness,
nausea,vomiting,
abdominal pain,
heapatotoxicity,
hepatic seizure,
renal failure,
thrombocytopenia,
pancytopenia,
rash, uticaria and
hypersensitivity,
cyanosis, anemia,
neutropenia,
jaundice, CNS
stimulation,
delirium followed
by vascular
collapse,
-Tell the
patient to
read label on
the other
OTC.
-Advised the
client to
avoid
alcohol.
-Inform
patient to
recognized
signs of
chronic
overdose,
bleeding,
50

100 mg/1 ml,
120 mg/2.5
ml, 160 mg/5
ml, 167 mg/5
ml
Suppositories:
80 mg, 120
mg, 125 mg,
300 mg, 325
mg, 650 mg
Suspension:
32 mg/ml, 160
mg/5 ml
Syrup: 160
mg/5 ml
Tablets
(chewable): 80
mg, 160 mg
Tablets
(extended-
release): 160
convulsion,
trauma, death.
.
bruising,
malaise,
fever.
-Tell patient
to notify
physician for
pain or fever
lasting for 3
days.
51

mg, 325 mg,
500 mg, 650
mg
Tablets (film-
coated): 160
mg, 325 mg,
500 mg.
Started: December 29, 2008
Discontinued: January 12, 2009
Name of Drug
Action Indication Route and Dosage
Availability Contraindications Adverse Effects
Nursing Indications
Metronidazole Direct-acting
amebicide or
trichomobacide.
It binds to
Infections in
the intra-
abdominal
skin and skin
750 mg P.O.
q 8 hours for
5 to 10 days
Tabs:
250, 375
500mg
Blood dyscrasias,
active CNS
diseases,
hypersebsitivity to
Convulsive
seizures,
peripheral
neuropathy,
-Obtain C&S
before
beginning
drug therapy
52

bacterial and
protozoan DNA
to cause loss of
helical
structurem
strand
breakage,
inhibition if
nucleic acid
synthesis and
cell death.
structure. Ext Rel tabs:
750mg
Injection
500mg/100ml:
Powder for
Injection:
500mg single
dose
imidazole,
tuberculosis if
mucous
membranes and
certain viral
conditions and first
trimester if
pregnancy.
rash,
pruritus, GI
comfort,
anorexia,
nausea,
furred
tongue, dry
mouth and
unpleasant
metallic
taste,
headache,
less
frequently
vomiting,
diarrhea,
weakness,
dizziness
and
darkening
of the
to identify if
correct
treatment has
been initiated.
-Assess for
allergic
reactions:
rash, urticaria
and pruritus.
-Monitor for
possible drug
induced
adverse
reactions.
-Monitor
renal
function:
urine output,
53

urine. input and
output ratio.
Started: January 13, 2008
Discontinued: January 20, 2008
Name of Drug
Action Indication Route and Dosage
Availability Contraindications Adverse Effects Nursing Indications
Cefuroxime Inhibits
bacterial
cell wall
synthesis,
rendering
cell wall
osmotically
Uncomplicated
UTI due to
E.coli or K.
pneumoniae.
Preoperative
prophylaxis in
clients
Tablets:
250 mg
Standing
Order:
750 mg
IV q8
Oral
suspension:
125 mg/5 ml
Powder for
injection:
750 mg, 1.5
g, 7.5 g
Diarrhea/loose
stool, nausea and
vomiting,
abdominal pain.
Adverse reactions
CNS: headache,
hyperactivity,
hypertonia, seizures
GI: nausea,
- Give in even
doses around
the clock; If
GI upset
occurs, give
with food;
drug must be
54

unstable,
leading to
cell death
by binding
to cell wall
membrane
undergoing
surgical
procedures
classified as
clean-
contaminated
or potentially
contaminated.
.
(ANST) Premixed
containers:
750 mg/50
ml, 1.5 g/50
ml
Tablets: 125
mg, 250 mg,
500 mg
vomiting, diarrhea,
abdominal pain,
dyspepsia,
pseudomembranous
colitis
GU: hematuria,
vaginal candidiasis,
renal dysfunction,
acute renal failure
Hematologic:
hemolytic anemia,
aplastic anemia,
hemorrhage
Hepatic: hepatic
dysfunction
Metabolic:
given for 10-
14 days to
ensure
organism
death and
prevent
superinfection
55

hyperglycemia
Skin: toxic
epidermal
necrolysis,
erythema
multiforme,
Stevens-Johnson
syndrome
Other: allergic
reaction, drug
fever,
superinfection,
anaphylaxis
Interactions
Drug-drug.
Antacids
containing
aluminum or
56

magnesium,
histamine2-receptor
antagonists:
increased
cefuroxime
absorption
Probenecid:
decreased excretion
and increased blood
level of cefuroxime
Drug-diagnostic
tests. Blood
glucose, Coombs'
test, urine glucose
tests using
Benedict's solution:
false-positive
results
57

Glucose,
hematocrit:
decreased levels
White blood cells
in urine: increased
level
Drug-food.
Moderate- or high-
fat meal: increased
drug
bioavailability
Name of Drug
Action Indication Route and Dosage
Availability Contraindications Adverse Effects Nursing Indications
58

Ranitidine Inhibits
histamine at
H2 receptor
site in the
gastric
parietal
cells, which
inhibits
gastric acid
secretion.
Used in the
management
of various
gastrointestinal
disorders such
as dyspepsia
gastrointestinal
reflux disease
[GERD],
peptic ulcer
and zolunger-
ellisou
syndrome.
Prophylaxis
of GI
hemorrhage
from the
stress
ulceration
and in
Standing
Order : 50
mg IV q8
Capsules
(liquid-filled):
150 mg, 300
mg
Solution for
injection: 25
mg/ml in 2-,
6-, and 40-ml
vials
Solution for
injection (pre-
mixed): 50
mg/50 ml in
0.45% sodium
chloride
Syrup: 15
mg/ml
Tablets: 150
mg, 300 mg
Tablets
Hypersensitivity to
drug or its
components
• Alcohol
intolerance (with
some oral
products)
• History of acute
porphyria.
Cardiac
arrythmias,
bradycardia,
headache,
somnolence,
fatigue, dizziness,
hallucinations,
depression,
insomnia,
alopecia, rash,
erythema
multiforme,
nausea and
vomiting,
abdominal
discomfort,
diarrhea,
constipation,
pancreatitis,
agranulocytosis,
-Monitor ASL,
ALT and serum
creatinine when
used to prevent
stress-related
GI tract
bleeding.
-Evaluate
results of
laboratory tests,
therapeutic
effectiveness
and adverse
reactions
(bradycardia,
PVC’s,
tachycardia,
CNS changes,
rash,
59

patients at
risk of
developing
acid
aspiration
during
general
anesthesia
prophylaxis
of mendelson
syndrome.
.
(effervescent):
150 mg
autoimmune
hemolytic or
aplastic anemia,
thrombocytopenia
granulocytopenia,
cholestatic or
hepatocellular
effects,
hypersensitivity
reactions.
gynecomasticia,
GI disturbance
and hepatic
failure.)
- Assess
knowledge and
teach patient
appropriate use,
possible side
effects or
appropriate
interventions
and adverse
symptoms to
report.
Started: February 3, 2009
Standing Order : 50 mg IV q8
60

Name of Drug
Action Indication Route and Dosage
Availability Contraindications Adverse Effects
Nursing Indications
61

Keterolac
(tromethamine)
Possesses anti-
inflammatory,
analgesics and
antipyretic
effects
Management
of severe,
acute pain in
adults that
requires
analgesia and
the opiate
level, usually
in a
postoperative
setting
Standing
Order: 30 mg
IV q6
Tablets: Each
white, round,
film-coated
tablet, with one
side printed in
black ink with
KET10 on one
side, contains:
ketorolac
tromethamine
10 mg.
Nonmedicinal
ingredients:
hydroxypropyl-
methylcellulose,
lactose,
magnesium
stearate,
microcrystalline
cellulose,
-Hypersensitivity
to the drug or
allergic symptoms
to aspirin or other
NSAID’s.
-Active peptic
ulcer , recent GI
bleeding or
perforation, history
of peptic ulcer or
GI beeding.
-Advanced renal
impairement
-High risk of
bleeding.
Systemic
use:
headache,
dizziness,
drowsiness,
diarrhea,
nausea,
dyspepsia/
indigestion,
epigastric/
GI pain and
edema,
Purpura,
asthma,
abnormal
visio,
abnormal
liver
function.
-Use as part
of a regular
analgesic
schedule
rather than on
as needed
basis.
-If pain
returns within
3-5 hours, the
next dose can
be increased
by up to 50 %
-Do not mix
IV/IM
ketorolac in a
small volume
with morpine
sulfate,
62

polyethylene
glycol and
titanium
dioxide. Bottles
of 100 and 500.
Store at room
temperature
with protection
from light.
Parenteral:
10 mg/mL:
Each mL of
clear, slightly
yellow, sterile
solution
contains:
ketorolac
tromethamine
10 mg.
Nonmedicinal
. meperinide
HCL,
promethazine
HCL, or
hydroxyzine
HCL, will
precipitate
from solution.
-the IV bolus
must be given
over no less
than 15 sec.
give IM
slowly and
deeply into
the muscle.
63

ingredients:
alcohol 10%
w/v and sodium
chloride in
sterile water.
The pH is
adjusted with
sodium
hydroxide or
hydrochloric
acid. Ampuls of
1 mL, trays of
5. Store at room
temperature
with protection
from light.
30 mg/mL:
Each mL of
clear, slightly
yellow, sterile
64

solution
contains:
ketorolac
tromethamine
30 mg.
Nonmedicinal
ingredients:
alcohol 10%
w/v and sodium
chloride in
sterile water.
The pH is
adjusted with
sodium
hydroxide or
hydrochloric
acid. Ampuls of
1 mL, trays of
5. Store at room
temperature
with protection
65

from light.
Started: Feb 3, 2009
Discontinued: Feb 4, 2009
Standing Order: 30 mg IV q6
66

VIII NCP
67

PRE-OPERATIVE NURSING CARE PLAN
Assessment Diagnosis Planning Nursing Interventions
Rationale Evaluation
Subjective:
“ Masakit ang ulo
ko at mainit ang
pakiramdam ko” as
verbalized by the
patient.
Objective:
> Increased in body
surface temperature
above normal range
of 36.5-37.4 C
(37.7 C)
>warm to touch
>Flushed skin
Hyperthermia
related to
inflammatory
response as
evidenced by
increased body
temperature ( 37. 7
C)
Rationale:
Fever is caused by
secretion of cytokines
by cells that appear in
the inflammatory
reaction (e.g.
macrophages). Two
common cytokines
are interleukin-1 (Il-1)
Short term
Planning:
Within one hour of
nursing
interventions the
patient will reduce
the body
temperature from
37.6 C to 37. 4 C
Diagnostic
Underlying cause of
excessive heat
production
Identified
Surface
Temperature
Monitored
Therapeutic
Surface cooling by
means of doing
TSB, heat loss by
evaporation and
conduction
>To assess
causative or
contributing factors
>To evaluate effects
or degree of
hyperthermia
>To reduce heat
Within one hour of
nursing
interventions the
patient’s body
temperature of 37.7
C reduced to 37. 4C
>Goal is met
68

and tumor necrosis
factor (TNF). Given
that these factors
cause fever and are
produced by
inflammatory cells, it
follows that a large
number of cells
produce large
amounts of cytokines
resulting in higher
fever. There is, then, a
direct relationship
between the severity
of the inflammatory
response and fever.
Promoted.
Educative
Instructed to
Maintain bed rest.
Advised to increase
Fluid intake.
.
>This will help in
reducing metabolic
demands and
oxygen
Consumption.
>Increase in oral
fluids will prevent
dehydration.
69

Assessment Nursing
Diagnosis
Goal Nursing
Interventions
Rationale Evaluation
Subjective:
“Natatakot ako sa
gagawing
operasyon sa akin”
as verbalized by the
patient.
Objective:
> poor eye contact
>Extraneous
movement (rocking
movements)
>Restlessness
Anxiety related to
impending surgery
as evidenced by
restlessness
Rationale:
Disturbed behavior
is due to
apprehension of the
outcome of the
surgery and
imagined threat to
one’s health.
Short term
Planning
After 8 hours of
rendering nursing
care and
interventions the
client will be able
to Verbalize
awareness of
feelings of anxiety.
Long Term
Planning
The patient will
appear relax and
will reduce anxiety
Diagnostic:
Vital Signs
Monitored
Therapeutic
Established a
therapeutic
relationship to the
client.
To identify physical
responses
associated with
both medical and
emotional
conditions.
To gain client’s
trust.
After 8 hours of
rendering nursing
care and
interventions the
client was able to
verbalize awareness
of feelings of
anxiety.
Goal is met
70

>Difficulty of
concentrating
>Confusion
V/S:
BP: 110/80 mmHg
RR: 24 bpm
PR: 110 cpm
Temp: 37.7 C
to a manageable
level. Encouraged the client
for participation in
relaxation exercise
(Deep breathing
exercise, progressive
muscle
relaxation,meditation)
and provide comfort
measures.g
environmental
factors).
Educative:
Encourage client to
acknowledge and to
express feelings
about the procedure/
operation that will be
done.
These are effective
non-chemical ways
to reduce anxiety
and client’s ability
to deal with
excessive stimuli is
impaired.
To determine her
feelings towards the
procedure or
conditions
71

Encourage client to
have an exercise/
activity program such
as reading books
To divert patients
attention and reduce
level of anxiety
about the surgery
POST-OPERATIVE NURSING CARE PLAN
72

Assessment Diagnosis Planning Intervention Rationale Evaluation
Subjective:”Masakit ang tahi
ko”as verbalized by
the client
Objective:>Facial Grimace
>Guarding behavior
>Cannot ambulate
>Pain score of 6
>Incision site in the
abdomen (7 inches)
is erythematous.
Acute pain related
to tissue injury
secondary to
surgical intervention
as evidenced by
report of 6 pain
scale.
Rationale:Acute Pain is
common to the
client who
undergone
surgery procedure
because there is a
break in the skin.
Short Term GoalAfter 1 hour of
Nursing Care, client
will be able to
verbalize reduction
of pain from 6 to 4.
and will be able to
ambulate
Long Term Goal:The Client will be
able to demonstrate
nonpharmacological
technique for
relaxation.
Diagnostic:Duration, frequency,
intensity
and precipitating
factors Assessed.
Therapeutic:
The Client
positioned to Semi-
Fowler’s and Deep
breathing exercise
Instructed with a
pillow to support the
inscision wound
Educative:
>This is a base to
plan the intervention
>DBE can make the
client feel relaxed; it
helps in coping up
with pain. In semi-
fowlers position
pressure in the
abdomen is reduced.
After 8 hours of
Nursing Care, the
client verbalized
reduction of pain
from 6 to 4. and
able to ambulate
Goal is Met
73

Advised the client to
apply
nonpharmacological
technique such as
relaxation technique
before,during and
after pain occur
> It helps to reduce
pain by increasing
the release of
endorphins
74

IX Discharge Plan
MEDICATION:
The Patient and the relatives are provided information about the time of
medication to be taken as ordered by her doctor.
ENVIRONMENT
Provide information to patient and significant others that the environment must be
clean and use clean materials because the surrounding may contribute to the client of risk
of infection.
EXERCISE:
Instruct the client to do leg exercise to promote blood circulation,Moderate
exercise in the morning within the patient’s limit and with rest.Inform client that the
normal activity can be resumed after 3-4 weeks.
HEALTH TEACHING:
Instruct the patient and significant others of proper way to clean the incision
wound,from incision site to the surrounding area of wound with cottons and betadine
or alcohol,one cotton each stroke and use sterile dressings.Inform client that the
Semi-fowler’s position may help to reduce tension to the incision site
Inform client and Instruct Deep Breathing Exercise and that she may use a pillow
to support abdomen because Deep Breathing Exercise promotes heeling.
DIET
Inform the patient to increased her intake of water a day(8-12glasses) and intake
of fiber must be increased too to treat her constipation.
OUT-PATIENT FOLLOW-UP:
Inform patient to make an appointment to have the surgeon remove the sutures
between 5th and 4th days.
SPIRITUAL
The Patient and the significant others are advised to have a deep Faith to Devine
God for Guidance.
75

X Bibliography
1. Brunner and Suddarth's Textbook of Medical-Surgical Nursing
i. by Suzanne C. Smeltzer and Brenda G. Brade
2. Fundamentals of Nursing by Kozier
3. Nurses’s Drug Handbook by George R. Spratto and Adrienne L. Woods
4. Essentials of Human Anatomy And Physiology by Elaine N. Marieb
5. Blackwell’s Nursing Dictionary
6. Nurse’s Pocket Guide by Marilyn E. Doenges
7. Pathophysiology by Thomas J. Nowak
8. (http://www.radiology.rsnajnls.org
)http://radiology.rsnajnls.org/cgi/content-nw/full/215/2/337/
9. http://www.aafp.org/afp/991101ap/2027.html
10. www.medicinenet.com
76

Homework Help https://www.homeworkping.com/
77