© 2009 The McGraw-Hill Companies, Inc. All rights reserved Electrocardiography and Pulmonary...
-
Upload
marianna-short -
Category
Documents
-
view
214 -
download
1
Transcript of © 2009 The McGraw-Hill Companies, Inc. All rights reserved Electrocardiography and Pulmonary...

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
Electrocardiography and Electrocardiography and Pulmonary Function TestingPulmonary Function Testing
PowerPoint® presentation to accompany:
Medical AssistingThird Edition
Booth, Whicker, Wyman, Pugh, Thompson

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-2
Learning Outcomes
52.1 Explain the conduction system of the heart.
52.2 Describe the basic patterns of an electrocardiogram (ECG).
52.3 Identify the components of an electrocardiograph and what each does.

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-3
Learning Outcomes (cont.)
52.4 Explain how to position the limb and precordial electrodes correctly.
52.5 Describe in detail how to obtain an ECG.
52.6 Identify the various types of artifacts and potential equipment problems and how to correct them.

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-4
Learning Outcomes (cont.)
52.7 Discuss how the ECG is interpreted.
52.8 Identify common arrhythmias.
52.9 Define exercise electrocardiography.
52.10 Explain the procedure of Holter monitoring.
52.11 Describe forced vital capacity.

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-5
Learning Outcomes (cont.)
52.12 Describe the procedure of performing spirometry.
52.13 Describe the procedure for obtaining a performing peak expiratory flow rate.
52.14 Describe the procedure for performing pulse oximetry testing.

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-6
Introduction Patients often have cardiovascular
or respiratory problems
Medical assistant Perform screening and/or diagnostic testing Understand the anatomy and physiology of the
heart and respiratory system

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-7
The Medical Assistant’s Role Electrocardiography
Graphic recording of the electrical impulses of the heart
Uses Evaluate symptoms of heart
disease Check effectiveness or side
effects of medications General examination

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-8
The Medical Assistant’s Role (cont.) Pulmonary function tests
Measure and evaluate a patient’s lung capacity and volume
Uses Help detect and diagnose
pulmonary problems Monitor respiratory
disorders Evaluate effectiveness of
treatments

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-9
Conduction System of the Heart Cardiac cycle
Controlled by specialized tissues in the heart wall that transmit electrical impulses
Impulses cause muscle to contract and relax

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-10
Bundle Branches
Bundle of HisSA Node
Purkinje Fibers
AV Node
Pacemaker of the heart
Sets rhythm of contractions
Bottom of right atrium
Impulse delayed slightly
Located in septum between ventricles
Relay impulse to Purkinje fibers
Located in ventricle walls
Contraction of ventricles
Conduction System of the Heart (cont.)

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-11
Electrocardiography Transmission, magnitude,
and duration of electrical impulses of the heart
Polarity Having a positive and
negative pole Resting cell
Positive outside Negative inside
Depolarization Impulse that initiates a
contraction
Repolarization Period of electrical recovery
following depolarization Prior to polarized (resting)
state
Conduction System of the Heart (cont.)

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-12
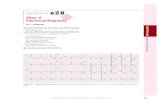
Basic pattern of the ECG Waves (deflections) are labeled P, Q, R, S, T, U
Conduction System of the Heart (cont.)

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-13
Apply Your KnowledgeTrue or False
___ The AV node is the heart’s pacemaker.
___ The medical assistant does not perform ECGs or PFTs.
___ The bundle branches relay impulses to the Purkinje fibers in the ventricles.
___ The heart is resting in the polarized state.
___ Depolarization initiates contractions of atria and ventricles.
___ Repolarization occurs before depolarization. F
ANSWER:
T
T
T
F
F
following
may
SA

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-14
The Electrocardiograph Electrical impulses are
detected through the skin Measures Amplifies – signal is
increased Records using the stylus

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-15
Types of electrocardiographs Standard machine –
12-lead, which records 12 different views at once
Single channel – one lead and records only one view
The Electrocardiograph (cont.)

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-16
Electrodes and electrolyte products Electrolyte – enhances
transmissions of electric current
Electrodes Ten areas of the body
Right and left arms Right and left legs Six locations on the chest
Enables physician to pinpoint origin of problems
The Electrocardiograph (cont.)

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-17
Leads Provide different images of electrical activity
Marked automatically on the ECG
Limb leads Three standard – I, II, III Three augmented – AVF, AVR, AVL
Precordial leads – V1 through V6
The Electrocardiograph (cont.)

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-18
ECG paper Single or multichannel available
Heat- and pressure-sensitive
Standardized to permit uniform
interpretation
Vertical axis – strength
of impulse (millivolt)
Horizontal axis – time
0.04 sec
5 mm(0.5 mV)
1 mm(0.1 mV)
1 mm5 mm
0.2 sec
The Electrocardiograph (cont.)

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-19
Controls Standardization control
Speed selector – 25mm/sec standard
Sensitivity control – adjusts height of tracing
Lead selector – enables selection of a single lead
Centering control – adjusts position of stylus
Stylus temperature control – adjusts darkness of line
Marker control – on older machines
On/Off switch
The Electrocardiograph (cont.)

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-20
Apply Your KnowledgeMatching:
___ Adjusts position of stylus A. Vertical axis
___ Adjusts height of tracing B. Sensitivity control
___ Adjusts darkness of tracing C. Precordial leads
___ Measures strength of impulse D. Horizontal axis
___ Measures time E. Limb leads
___ AVF, AVR, AVL F. Amplification
___ V1 through V6 G. Centering control
___ Increases signal H. Stylus temperature control
ANSWER:
H
G
F
E
D
C
B
A
Superbly Matched!

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-21
Preparing to Administer an ECG Proper technique essential
Preparing the room and equipment Other electrical equipment turned off Quiet room, comfortable temperature Check machine
Warm up Adequate paper

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-22
Preparing the patient
Introduce yourself
Explain the procedure
Answer questions
Ensure patient comfort
Perform ECG procedure
Preparing to Administer an ECG (cont.)

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-23
Applying the Electrodes and the Connecting Wires Electrodes – disposable
are most common
Positioning electrodes Use consistent technique Limb electrodes – place at
same level Precordial electrodes –
specific intercostal spaces Precordial Lead Placement

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-24
Attaching wires Numbers and letters
correspond to those for electrodes
Connect limb wires first Precordial in same sequence
as electrodes Avoid tension on wires
Applying the Electrodes and the Connecting Wires (cont.)

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-25
Operating the Electrocardiograph Standardize
Run the ECG Automatic Manual Multiple-channel
Check the tracing Clear / free from
artifact

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-26
Apply Your Knowledge1. In addition to making sure the room is comfortable for the
patient and the ECG machine is ready, what else should you do to prepare for performing an ECG?
ANSWER: All other electrical equipment in the room should be turned off.
2. Electrodes are placed at how many positions on the body?
ANSWER: Ten: four limb and six chest positions.

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-27
Apply Your Knowledge
3. What should you do just prior to running the ECG to see if the machine needs adjusting? What should you do upon completion of the test?
ANSWER: Standardize the electrocardiograph prior to running the tracing. Upon completion of the ECG, you should check the tracing to be sure is it clear and free from artifact.

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-28
Troubleshooting Artifacts
Causes Improper technique Poor conduction
Outside interference Improper handling

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-29
Wandering baseline – somatic interference or mechanical problems
Flat line – loose or disconnected wire
Extraneous marks – careless handling
Troubleshooting: Artifacts

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-30
Causes AC interference –
machine picks up current from other electrical equipment
Somatic interference – muscle movement
Identifying source of interference Check tracings for leads
I, II, and III
If unable to identify source, stop and notify supervisor of problem
Leave patient connected
Troubleshooting: Artifacts (cont.)

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-31
Completing the Procedure Acceptable tracing
Label properly Disconnect wires from
electrodes Remove electrodes / wipe off
electrolyte Assist patient up Prepare room appropriately
Mount tracing if necessary

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-32
Apply Your Knowledge1. What are four general causes of artifacts?
ANSWER: They are improper technique, poor conduction, outside interference, and improper handling of the tracing.
2. What should you after running an ECG?
ANSWER: After making sure the tracing is acceptable, you should label it properly, disconnect wires from electrodes, remove electrodes and wipe off electrolyte, assist patient up, and prepare the room appropriately for the next patient.
Bravo!

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-33
Interpreting the ECG Not a medical assistant
responsibility
Knowing how they are interpreted will enable you to recognize a problem requiring immediate attention
Heart rate If regular – count QRS
complexes in a 6-second strip and multiply by 10
Irregularities Conduction
abnormalities Reaction to medication

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-34
Intervals and segments Variations in length and position
Conduction disturbances Myocardial infarctions Electrolyte disturbances
Wave changes – normally similar in each lead
Interpreting the ECG (cont.)

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-35
Heart rhythm Regularity of the heartbeat
Distances between complexes and waves is normally consistent
Rhythm strip obtainedfrom lead II
Interpreting the ECG (cont.)

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-36
Abnormal cardiac arrhythmias Irregularities in heart rhythm Ventricular fibrillation – life-threatening with no cardiac
output Premature ventricular contractions – heartbeats that
originate from the ventricles Bundle branch blocks – impulse through the heart is
slowed or blocked Atrial fibrillation – electrical disturbance in the atria and/or
AV node
Interpreting the ECG (cont.)

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-37
Apply Your KnowledgeMatching (may be used more than once):
___ Number of QRS complexes in 6 sec x 10 A. V-fib
___ Cannot identify “P” waves B. Heart rhythm
___ Produces no cardiac output C. Bundle branch block
___ Originates in ventricles D. Atrial fibrillation
___ Slows or stops impulse E. Heart beat
___ Multiple impulses from sites outside SA node F. PVC
___ “Saw-tooth” image
___ Regularity of heart beat
___ Due to irritable of ventricular heart muscleF
F
E
D
A
A
D
C
B
ANSWER:

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-38
Exercise Electrocardiography Stress test – measures the
heart’s response to a constant or increasing workload
Uses Determine how
a diseased heart is functioning Screen a patient for heart
disease Determine patient’s ability to
start an exercise program

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-39
Ambulatory Electrocardiography Resting ECG may not show abnormalities
Holter monitoring Monitors heart over a
24-hour period of normal activity
Uses Diagnosis Evaluate status post-MI
Patient education Record activities What to avoid How to check monitor

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-40
Ambulatory Electrocardiography (cont.)
Connecting the patient 3 or 5 electrodes
Prep skin prior to placing
Tape in place to eliminate tension and ensure that electrodes stay in place for entire time of testing
Put fresh battery in the machine
Check tape
Ensure that machine is turned on

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-41
Apply Your KnowledgeWhat is the purpose for stress testing and Holter monitor testing?
ANSWER: Stress testing is used to measure the heart’s response to a constant or increasing workload. A Holter monitor is used to obtain a tracing over a period of time when a resting ECG shows no abnormalities. Both are used for diagnosing cardiac conditions or for monitoring current treatments and medications.
Correct!

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-42
Pulmonary Function Testing Evaluates lung volume
and capacity Uses
Evaluate of shortness of breath
Detect and classify of pulmonary disorders
Evaluate of effectiveness of treatments

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-43
Spirometry Measures air taken in by and
expelled by the lungs
Forced vital capacity (FVC) – greatest volume of air that can be expelled with a rapid, forced expiration
Types of spirometers: Computerized Mechanical

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-44
Performing Spirometry Technique similar for all types – be consistent
Patient preparation Inform the patient about conditions and activities that
could affect the test accuracy Explain procedure and its purpose Explain the need for a nose clip Be sure patient forms a tight seal around the mouthpiece Position the patient properly Demonstrate correct procedure

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-45
Performing the maneuver
Urge patient to blow hard and to continue
blowing
Provide feedback on performance
Obtain three acceptable maneuvers
Observe the patient’s symptoms
Notify physician immediately if symptoms occur
Performing Spirometry (cont.)

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-46
Determining effectiveness of medications
Perform test before patient takes medication for day
Repeat after patient takes the medication
Special considerations
Uncooperative patients
Patients who do not understand
Patients who cannot follow directions
Patients who cannot perform the procedure
Performing Spirometry (cont.)

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-47
Calibration Daily – keep logbook Calibration syringe –
standardized measuring instrument
Detect leaks – check time/volume graph
Results Evaluate ventilatory function Screening for pulmonary disorders Severity of problems Response to therapy or medication
Infection control Clean equipment after each
patient Discard disposable supplies
appropriately Wash hands before and after
each use
Performing Spirometry (cont.)

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-48
Peak Expiratory Flow Rate Determines amount of
air that can be quickly forced from the lungs
Peak flow meter
Reveals narrowing of airways before an asthma attack
Peak flow zones Different for each
patient Green zone – good
control of asthma Yellow zone – large
airways are beginning to narrow
Red zone – medical emergency

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-49
Pulse Oximetry Testing Non-invasive measurement of the oxygen saturation
in arterial blood Hemoglobin absorbs infrared light Measures amount of light absorbed Hypoxemia – less than 95%
Uses Pulmonary and cardiac conditions Post-operatively Sleep apnea

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-50
Apply Your Knowledge
1. What is the purpose of PFTs?
ANSWER: To evaluate lung volume and capacity.
2. What is FVC?
ANSWER: It is forced vital capacity: the greatest volume of air that can be expelled with a rapid, forced expiration. It is the measurement of the volume of air expelled and amount of time taken to expel it.

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-51
Apply Your Knowledge3. Joey Jackson called to ask about taking his asthma medicine. He said he
as been using his peak flow meter and the readings have been in his yellow zone. What do you tell him?
ANSWER: This means that his large airways are beginning to narrow and that he should take his medication as prescribed.
4. Joey decided to come to the office and you check his oxygen saturation with the pulse oximeter. The reading was 93%. What does this mean and what should you do?
ANSWER: Joey is hypoxemic. You need to notify the physician and document findings.
YIPPEE!4 for 4

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-52
In Summary ECG and PFTs – vital to diagnosis and
treatment of cardiac and pulmonary disease
Medical assistant Understanding of anatomy and physiology of both
systems Accurate performance of procedures Recognition of abnormalities Patient education

© 2009 The McGraw-Hill Companies, Inc. All rights reserved
52-53
End of Chapter
As the arteries grow hard, the
heart grows soft.
~ H. L. Mencken